What Does Medicare Cover
Federally managed Medicare has four parts, which include Part A and Part B , together known as original Medicare. The two other parts of Medicare are Part C, also known as Medicare Advantage, and Part D .
A person with a diagnosis of obstructive sleep apnea generally gets Medicare coverage for a 3-month trial of CPAP therapy. Medicare may extend coverage for CPAP if a persons doctor reports that the therapy is helping alleviate the condition.
Medicare Advantage plans may cover CPAP therapy, as the plans must offer at least the same coverage as original Medicare.
In addition, a Part D plan may offer coverage for doctor-prescribed nasal decongestants, although a person would need to check the list of drugs, called a formulary, that their plan includes.
Does Medicare Cover Sleep Apnea Treatment With A Cpap Machine
In most cases, Medicare generally covers 80% of the allowable charges related to a sleep apnea machine.
Medicare initially may pay for a three-month trial with a CPAP machine. After that time, Medicare may cover a longer period of treatment if you meet with your doctor and he or she determines the device or helping you. Once that information is recorded in your medical record, Medicare will generally cover an additional ten months of sleep apnea machine rental, for a total of 13 months, at which time, you will own the equipment outright. Tubing and other supplies for your sleep apnea machine are generally also covered at 80%.
You generally need to meet your Medicare Part B deductible before Medicare pays its share, and you must rent your device from a supplier enrolled in Medicare. The doctor who orders your CPAP machine must also participate with Medicare.
Option : Use Medicares Website
If you have a Medicarehealthcare plan, you can also find in-network durable medical equipment providers by using Medicares Supplier Directory. After you click the link, enter your zipcode and select the corresponding product category. For CPAP machines and related supplies, select . After you click the search button, the website will provide you with a list of vendors in your area that provides CPAP equipment and accepts Medicare insurance.
For the lucky few of you, you may be able to find a MedicareDME provider that is relatively close to you however, for others, the drive from your home could be long and inconvenient. Luckily, Health Sqyre will ship your desired CPAP products right to your door!
Don’t Miss: Does Medicare Part C Cover Dentures
Will Medicare Supplement Plans Pay For My Cpap Machine
Between five and 20 percent of the adult population has sleep apnea, though the National Sleep Foundation suggests that the numbers may be underreported. People of all ages can develop sleep apnea, and as you get older, you might need a CPAP machine. But will Medicare Supplement plans pay for your durable medical equipment?
Lets look at some of the factors that you should take into account when choosing and deciding how to handle your sleep apnea treatment.
Will Medicare Cover A Cpap Machine
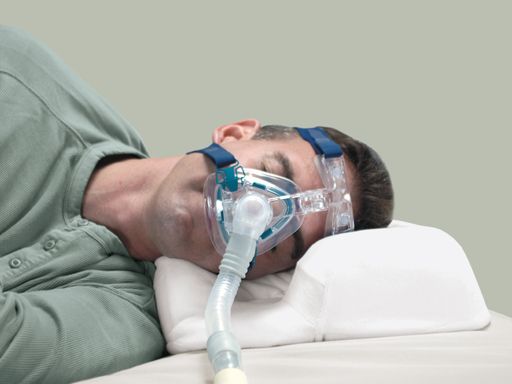
Medicare covers CPAP machines used to treat sleep apnea under the durable medical equipment benefit. To qualify for CPAP coverage, you must meet the following requirements:
- Complete a sleep test in a laboratory setting or by using an approved at-home test
- Be diagnosed with obstructive sleep apnea based on sleep test results
- Have a prescription for a CPAP machine from your doctor
- Get the CPAP machine from a participating Medicare supplier
Since CPAP treatment doesnt work for everyone, Medicare first covers the machine for a three-month trial period. After three months, your doctor will check how the treatment is working for you. Medicare may cover CPAP therapy long term if your doctor verifies in your medical record that you are using the machine and that its helping you.
Recommended Reading: Do I Need Medicare If I Have Tricare
Sleep Apnea And Medicare
Navigating coverage for sleep apnea can be tricky, but luckily, Medicare often picks up a majority of the cost. If youre diagnosed with obstructive sleep apnea, you may qualify for CPAP therapy, including routine accessories for your CPAP machine.
If you already have sleep apnea and are considering a backup oxygen concentrator, there are plenty of affordable oxygen concentrators to consider. While there may be certain restrictions and requirements for Medicare coverage of your CPAP machine, it will definitely offer some form of assistance.
To learn more about Medicare coverage, check out our helpful guides:
How Much Do Positive Airway Pressure Machines Cost
The cost of a positive airway pressure machine depends on the unit’s quality and features, and prices for standard CPAP machines typically range between $250 and $1,000. Bilevel positive airway pressure machines, which provide distinct pressure levels for inhalation and exhalation, are more expensive and can cost as much as $6,000 for advanced models. Automatic CPAP machines , which can adjust the airflow pressure if it detects an airway collapse, typically range in cost from $450 to $1,800.
You May Like: How Old To Be Eligible For Medicare
Medigap And Cpap Machines
Medigap, also known as Medicare Supplemental Insurance, covers the gaps of Original Medicare and can provide additional coverage related to CPAP therapy. For instance, certain Medigap plans in tandem with Medicare coverage might be able to cover the full cost of CPAP machine rentals or accessories needed for the machine for your sleep apnea, as long as your physician certifies that it is medically necessary and is improving your health.
Pro Tip: There are currently 10 different types of Medigap plans offered by private insurers. To help you get started, read my list of affordable medicare supplement plans.
How Much Does Medicare Cover For A Cpap Machine
Whether you have Part B through Original Medicare or enrolled in Medicare Advantage, Medicare will cover your CPAP machine similarly to other benefits. First, youll pay your deductible. Then, Medicare will pay its portion. Youll pay the remainder or coinsurance.
- How much does Medicare pay for CPAP machines? 80% of the Medicare-approved amount.
- How much will you have to pay for a CPAP machine? The remaining 20%.
In most cases, Medicare will help pay to rent your CPAP machine for 13 continuous months if you use it without interruption. After this period, you own the CPAP machine. You will still be responsible for paying the coinsurance on the rental costs.
If you have Original Medicare, you may be able to sign up for Medicare Supplement Insurance . Many states offer Medigap plans that can help cover your CPAP coinsurance during your rental period.
You May Like: How Long Does It Take For Medicare To Become Effective
How Often Can You Get A New Cpap Machine Under Medicare
CPAP machines are used to deliver constant, steady air pressure to patients with obstructive sleep apnea while they are sleeping. Sleep apnea is a medical condition that causes pauses in breathing during sleep.
Medicare does cover CPAP machines if you are diagnosed with sleep apnea. Medicare Part B may cover a 3-month trial of CPAP therapy.
If the CPAP therapy is successful, your doctor may be able to extend the treatment and Medicare will cover it. If you rent a CPAP machine for 13 months, you own it.
Medicare Part B is usually responsible for covering durable medical equipment like CPAP machines.
What Are Medicare Guidelines For Cpap
You have a three-month trial period covered by Medicare. After three months, your doctor will check how the treatment is working for you. Medicare may cover CPAP therapy long-term if your doctor verifies in your medical record that:
- You are using the machine
- The therapy is helping you.
Remember, getting a prescription for a CPAP machine depends on a sleep studys results to determine if you have obstructive sleep apnea. Does Medicare cover sleep study testing and equipment? Yes, Medicare Part B covers the tests youll need to see if youre eligible for CPAP coverage.
Read Also: What Is The Cost Of Medicare Supplement Plan F
Will Medicare Cover Replacement Supplies
The short answer is yes Medicare will cover replacement supplies within reason. A recommended replacement schedule has been created by Medicare outlining what they have deemed necessary. For example, humidifier water chambers should be replaced every 6 months according to the determination of the Medicare program while nasal pillows can be replaced twice per month. It just depends on the piece of equipment. We highly recommend that you take advantage of the replacement schedule, as this will help you maintain healthy CPAP therapy.
What Is A Cpap Machine
If you have OSA, continuous positive airway pressure machines, opens new window are one of the most common treatments. A CPAP machine is a device with a face or nose mask attached to a small pump. The pump pushes pressurized air through a hose, into the mask and into your airway. The steady flow of air keeps the airway open to improve breathing and sleep quality. Some people may require extra CPAP supplies like humidifiers and heating tubes for effective treatment.3
Read Also: How To Avoid Medicare Part D Penalty
How Much Does Medicare Pay For Cpap Machines
Even if Medicare covers your CPAP machine, there are some out-of-pocket costs you should expect to pay, which may include:
- Part B deductibleThe Medicare Part B deductible is $185 per year in 2019. You must meet your deductible before your Part B coverage will kick in.
- Part B coinsurance or copaymentYou are typically responsible for 20 percent of the Medicare-approved amount for the CPAP machine cost, including filters, hoses and other parts.
There is no annual limit on how much you could pay for the Part B coinsurance in a given year.
If you get your CPAP machine from a medical equipment supplier who doesnt accept Medicare assignment , theres no limit to how much they can charge you for the machine.
Speak with your doctor and your DME supplier for specific cost and coverage information.
License For Use Of Current Dental Terminology
End User License Agreement:These materials contain Current Dental Terminology , copyright © 2020 American Dental Association . All rights reserved. CDT is a trademark of the ADA.
The license granted herein is expressly conditioned upon your acceptance of all terms and conditions contained in this agreement. By clicking below on the button labeled I accept, you hereby acknowledge that you have read, understood and agreed to all terms and conditions set forth in this agreement.
If you do not agree with all terms and conditions set forth herein, click below on the button labeled I do not accept and exit from this computer screen.
If you are acting on behalf of an organization, you represent that you are authorized to act on behalf of such organization and that your acceptance of the terms of this agreement creates a legally enforceable obligation of the organization. As used herein, you and your refer to you and any organization on behalf of which you are acting.
Don’t Miss: How To Apply For Medicare Card Replacement
What Is Required In The Initial Face
History
- Signs and symptoms of sleep disordered breathing including snoring, daytime sleepiness, observed apneas, choking or gasping during sleep, morning headaches
- Duration of symptom
- Validated sleep hygiene inventory such as the Epworth Sleepiness Scale
Exam
Our service request form meets the requirements for ordering services for Medicare patients. You can download it here:
Medicare Advantage And Cpap Machines
If youre enrolled in a Medicare Advantage plan, you might receive additional support and coverage for CPAP machines and accessories. Contact your plan to learn more about this potential coverage.
Pro Tip: If youre looking for extra support and the chance to resume some of your daily activities, a durable and lightweight portable oxygen concentrator might be a good option. Check out my list of the best portable oxygen concentrators to learn more.
Don’t Miss: Can You Get Medicare If You Retire At 62
Choosing The Right Cpap Mask
CPAP masks come in a variety of different types, shapes, and styles. You cant assume that a particular size in one brand will fit exactly the same as that size from another brand, so its a good idea to try on masks in person to make sure they fit. Its very important to find a sleep apnea mask that fits well for your particular face. A mask that is too loose may leak air, while a mask that is too tight may increase discomfort and make it harder for you to get used to the machine. Some sleep apnea masks are padded, which you may find more comfortable. Remember to use your CPAP mask as your doctor prescribes.
You can work with your doctor to find a sleep apnea mask that meets your needs. There are several different types of CPAP masks:
Nasal pillow: A nasal pillow sleep apnea mask fits at the bottom of the nostrils and is connected directly into the nose. Covering only the nose, this could be a good choice for people who want to leave their vision totally unblocked to read or watch TV before sleeping. They also work well with people who wear glasses or men with beards or facial hair.
Does My Deductible Apply To Cpap Equipment
Typically, your deductible applies to essential CPAP equipment, not including optional accessories. Most providers have replacement schedules for components such as tubes, masks, and filters that indicate how often replacements are covered. If you require more frequent replacements of certain components, those costs may be out of pocket.
You May Like: Should I Get Medicare Supplemental Insurance
How Often Does Insurance Cover Cpap Machines
Most insurance plans offer partial coverage for CPAP machines once you meet your deductible. Medicare participants are responsible for paying their deductible, plus 20% of the machine rental. If you have a high deductible under your health insurance policy, you may inadvertently end up covering the full cost of your CPAP machine.
Does Insurance Cover Vasectomy Reversals
Category: Insurance 1. Insurance Coverage Vasectomy Reversal Center of America In some cases, medical insurance covers the costs of a vasectomy reversal. In the majority of cases, however, the procedure is not covered by insurance. Discusses vasovasostomy, a procedure to reconnect the vas deferens tubes that were cut during
Recommended Reading: What Is A Medicare Special Needs Plan
How Does Equipment Rental Work
When you qualify for oxygen therapy, Medicare doesnt exactly buy the equipment for you. Instead, it covers the rental of an oxygen system for 36 months.
During that period, youre responsible for paying 20 percent of the rental fee. The rental fee covers the oxygen unit, tubing, masks and nasal cannula, gas or liquid oxygen, and the costs of service and maintenance.
Once the initial 36-month rental period ends, your supplier is required to continue supplying and maintaining the equipment for up to 5 years, as long as you still have a medical need for it. The supplier still owns the equipment, but the monthly rental fee ends after 36 months.
Even after the rental payments have ended, Medicare will continue paying its share of the supplies needed to use the equipment, such as the delivery of gas or liquid oxygen. As with the equipment rental costs, Medicare will pay 80 percent of these ongoing supply costs. You will pay your Medicare Part B deductible, monthly premium, and 20 percent of the remaining costs.
If you still need oxygen therapy after 5 years, a new 36-month rental period and 5-year time line will begin.
What Other Sleep Apnea Treatment Does Medicare Cover
Medicare generally covers certain types of sleep tests your doctor orders to diagnose sleep apnea. It may also cover other types of sleep apnea machines, such as the BPAP machine. Medicare also covers certain types of oral appliance therapy with sleep apnea devices, as long as the supplier is approved with Medicare.
If you need other types of sleep apnea treatment such as surgery to remove obstructing tissue, Part A and Part B typically cover allowable charges for medically necessary care.
If you are a smoker and you need help to quit smoking, Medicare Part B covers smoking cessation sessions with a qualified provider. If your doctor suggests weight loss as part of your sleep apnea treatment, Medicare covers weight loss counseling. In some cases, if you are morbidly obese and your obesity is contributing to your sleep apnea, Medicare may cover certain types of weight loss surgery.
Nasal congestion from allergies may also contribute to sleep apnea. If you have a Medicare Part D Prescription Drug Plan, your plan should cover any prescription allergy medications and nasal sprays your doctor orders for sleep apnea treatment, but you should check your plan formulary to be sure.
To find a Medicare Advantage or Medicare Supplement plan that may cover sleep apnea equipment, enter your zip code on this page.
Don’t Miss: What Is Medicare Ffs Program
Does Original Medicare Cover Cpap Supplies
Yes. Original Medicare helps pay 80% of the cost of the following equipment after youve met your Part B deductible:6
- CPAP machine rental for a 3-month trial if youre newly diagnosed
- CPAP rental for 13 months if youve been using it consistently
- Masks or nose pieces you wear when using the machine
- Tubing to connect the mask or nose piece to the machine
Original Medicare has certain rules for replacing CPAP machine supplies. Contact your doctor or device supplier for more information.
Note: Part B also helps pay up to 80% of the costs of your sleep study if you have clinical signs and symptoms of sleep apnea. Costs covered include Type I, II, III, and IV sleep studies and devices.7
Even Medicare Requires You To Pay At Least 20% Of The Cost And Still Rent Your Cpap Machine For Up To 13 Months
Does humana insurance cover cpap machines. Does medicare cover cpap supplies? One of the most critical parts of the process is documentation and testing. However, coverage varies from plan to plan and so do authorization requirements.
Medicare does cover cpap machines if you are diagnosed with sleep apnea. Youll need a prescription from your doctor to access coverage to rent or buy eligible equipment. We’ll answer the basic questions, like what w
Cover rental or a replacement cpap machine and/or cpap accessories if you. 2 there are several types of sleep apnea, but the most common is obstructive sleep apnea . Insurance plans will cover a continuous positive airway pressure or other pap device if it is medically necessary.
A widespread cause of poor sleep. In addition to cpap machines, medicare part bs durable medical equipment benefit also covers cpap supplies, such as face masks, tubing and filters. Click here to check your humana coverage for sleep apnea products.
Medicare may cover continuous positive airway pressure therapy if youve been diagnosed with obstructive sleep apnea. Medicare will cover the cpap machine and other accessories in the same way that it covers other qualified durable medical equipment . Read more about insurance coverage below.
Most plans include the cpap machine, masks, tubing, headgear, and filters. If you rent a cpap machine for 13 months, you own it. Besides the cpap machine, you might be wondering what other items your insurance covers.
Recommended Reading: Can You Get Medicare At Age 60