How We Chose The Best Diabetic Supply Companies
Choosing the best diabetic supply company depends mostly on what type of insurance you have. Because there are so many insurance policies out there, we decided the most effective way to scout the best diabetic supply companies was to go directly to the source the people who use them. We interviewed people living with diabetes, as well as clinicians who work in the field: Certified diabetes care and education specialists, nurses, doctors, and dietitians. We asked them who is the most reliable, courteous, trustworthy, on-the-cutting edge of technology, and knowledgeable.
We also learned that before deciding on a specific company, that its important to find out who your insurance has contracts with, which supplies you need, and how you can get them all conveniently to your home with little fuss. People living with diabetes who use insulin pumps told us that it is often easier to get their pump supplies delivered directly from the pump supplier. They also told us that if you need more general supplies, such as test strips, a glucose meter, lancets, and others, then a larger company such as Byramhealth or Edgepark may be right for you. Shop costs and discuss with your medical team which option is right for you or your loved one.
What About Cgm Remote Monitoring And App Communication For Medicare Users
At this time, app communication and remote monitoring are not allowed for therapeutic CGMs. Dexcom has had to turn off this function in its G5 Medicare system, a tremendous frustration for users due to the current Medicare reimbursement codes. We know that Dexcom is working to fix this, along with a number of patient and organizational advocates. Unfortunately, there is no timing to report, but we hope to see this policy overturned as soon as possible remote monitoring of CGM data can save lives!
Abbotts FreeStyle Libre does not have an approved smartphone reader app in the US right now. Its LibreLink and LibreLinkUp apps are available outside the US, though were not sure when theyll come to the US.
Does Medicare Pay For Dexcom G6
Dexcom G6® CGM System will be covered for Medicare beneficiaries, having met the category requirements for therapeutic CGM systems by the U.S. Centers for Medicare& Medicaid Services .
How much does Medicare cover for dexcom?
A: According to Dexcoms Medicare FAQ page, those covered by Medicare can expect to pay 20% of the costs of their G5 CGM, which is roughly $50 per month. Medicare will cover the remaining 80%.
Don’t Miss: Does Aarp Medicare Supplement Plan Cover Silver Sneakers
How Often Does Medicare Pay For Replacement Bg Meter
Yes, Medicare generally pays 80% of the cost of CGM accessories and supplies. Under the guidelines, Medicare Part B covers: Patch refills based on the recommended replacement schedule. For example, if you use a CGM that requires a new patch every 14 days, Medicare will pay for two patches every 28 days.
Donât Miss: Where To Send Medicare Payments
Freestyle Libre 14 Day Sensor Kit
The photos shown are samples onlyNot all photos of the drug may be displayed. Your medication may look different. If you have questions, ask your pharmacist.close popup
Consult your pharmacist.
In the US –
In Canada – Call your doctor for medical advice about side effects. You may report side effects to Health Canada at 1-866-234-2345.
Consult your pharmacist.
Keep a list of all your medications with you, and share the list with your doctor and pharmacist.
If someone has overdosed and has serious symptoms such as passing out or trouble breathing, call 911. Otherwise, call a poison control center right away. US residents can call their local poison control center at 1-800-222-1222. Canada residents can call a provincial poison control center.
Consult your pharmacist.
Do not flush medications down the toilet or pour them into a drain unless instructed to do so. Properly discard this product when it is expired or no longer needed. Consult your pharmacist or local waste disposal company for more details about how to safely discard your product.
Information last revised July 2016.
Copyright 2022 First Databank, Inc.
Selected from NATIONAL DRUG DATA FILE data included with permission and copyrighted by First Databank, Inc., 2019. This copyrighted material has been downloaded from a licensed data provider.
You May Like: Does Medicare Part B Pay For Hearing Aids
What Is Part B For Diabetes
In addition to diabetes self-management training, Part B covers medical nutrition therapy services if you have diabetes or renal disease. To be eligible for these services, your fasting blood sugar has to meet certain criteria. Also, your doctor or other health care provider must prescribe these services for you.
Are Glucose Monitors Covered By Medicare
Medicare Part B covers Glucose monitors as durable medical equipment that your doctor has prescribed for your use at home.
You will need to get your monitor from a Medicare-approved supplier. Medicare will determine if your monitor must be rented or purchased. In some instances, you may be able to choose between those options.
As part of a CGM system, glucose monitors connect wirelessly with insulin pumps. They provide all-day readings of your blood sugar levels without the need for most finger pricks.
Don’t Miss: How Much Does Medicare Pay For Assisted Living Facility
Medicare Coverage For The Freestyle Libre Glucose Monitor
Medically reviewed by Deborah Weatherspoon, Ph.D., MSN Written by Rachael Zimlich, RN, BSN onJanuary 14, 2021
- Continuous glucose monitors can help people with diabetes manage their blood sugar levels.
- Medicare began covering these devices within the last decade.
- Abbotts Freestyle Libre is a continuous glucose monitor that Medicare began covering shortly after its FDA approval in 2017.
A diabetes diagnosis can come with many difficult lifestyle changes, including frequent blood sugar checks.
To check blood glucose levels, people with diabetes must pierce their skin often several times per day and feed blood into a monitor for analysis.
Newer machines called continuous glucose monitors can help make this process easier, letting you keep track of your blood sugar levels in a less invasive way. One type of CGM is Abbotts Freestyle Libre.
Medicare took some time to get on board with covering these devices. However, for the last few years, some people with diabetes have qualified.
Find out when these devices are covered and what you need to do to qualify.
Does Medicare Cover Continuous Glucose Monitors
Original Medicare covers continuous glucose monitors through Part B of Medicare. In most cases, Medicare covers the monthly supplies for a monitor, which is a combination of sensors, transmitters and batteries depending on the brand. Although devices are covered, beneficiaries may have to pay copays or deductibles.
As Medicare Advantage must provide the same level of coverage as Original Medicare, these devices are also available to people on Medicare Advantage Plans. However, individual Medicare Advantage Plans may have different rules around costs, brands and the choice of where you can get services.
In the past, continuous glucose monitors were considered precautionary instead of medically necessary, which limited the number of people who could gain access to the technology. However, rules changed in 2021, allowing more enrollees to benefit from the devices.
You May Like: How Do I Contact Medicare Part B
How Does Freestyle Libre Medicare Part B Coverage Work
Medicare Part B is medical insurance, and it helps pay for outpatient doctors appointments, preventive care such as diabetes screenings, and durable medical equipment . In order for Medicare to approve your DME, your doctor must prescribe it, and it must be a device that will last for three years or more.
You may be responsible for 20 percent of approved Medicare costs for FreeStyle Libre including the equipment itself and your doctors supervision.
Jeemin Kwon
The CGM Discount Access program provides discounted rates on the Guardian Sensor 3 continuous glucose monitoring system for people without insurance coverage for Medtronic CGMs.
Medtronic recently launched its CGM Discount Access program which provides the Guardian Sensor 3 continuous glucose monitor at a discounted price to people who meet the eligibility criteria. Specifically, the program provides a Guardian Link 3 transmitter with a 12-month warranty for $180 and a monthly supply of five Guardian Sensor 3 sensors for $60 per month.
To be eligible for the program, people must:
-
Use multiple daily injections of insulin or be on insulin pump therapy
-
Have a valid CGM prescription from a healthcare professional
-
Not have insurance coverage for a Medtronic CGM
These programs have become increasingly important, especially since people with diabetes face more severe financial hardship during the pandemic. Read more about how COVID-19 has affected the diabetes community here.
Criteria For Cgm Coverage
However, you have to meet certain conditions in order to qualify for coverage. Those conditions are:
- You have to visit the doctor who prescribes the CGM in the 6 months before you order the device
- A follow up visit with your doctor every 6 months after you get your prescription
- A diagnosis of diabetes mellitus
- You already use a blood glucose monitor
- Each day, you need 3+ insulin injections or you need to use a continuous insulin infusion pump
- You need to have blood sugar level tests four or more times a day
- A healthcare provider that is Medicare-approved
- A DME supplier that is Medicare-approved
- Your insulin treatment routine needs frequent adjustments
- Certification from your doctor that you meet the criteria for the CGM and that you follow the treatment plan
Medicare Part Bs coverage for FreeStyle Libre 14 Day includes:
- The patch with a thin sensor that goes under your skin to measure your blood sugar level
- The reader that collects data from the patch
These patches are good for 10-14 days and Medicare Part B will cover the cost of refillable patches.
Medicare Advantage plans also provide coverage for a FreeStyle Libre 14 Day. They cover everything Original Medicare covers as well as some additional benefits. However, exactly what a plan covers and what the out-of-pocket costs are will vary depending on the specifics of your plan.
Read Also: What Is Monthly Premium For Medicare
Abbott’s Freestyle Libre 2 Cgm Picks Up Medicare Coverage
Abbott announced yesterday that its recently cleared FreeStyle Libre 2 integrated continuous glucose monitoring system is now covered by the Centers for Medicare and Medicaid Services , and available to Medicare beneficiaries with diabetes who meet eligibility criteria.
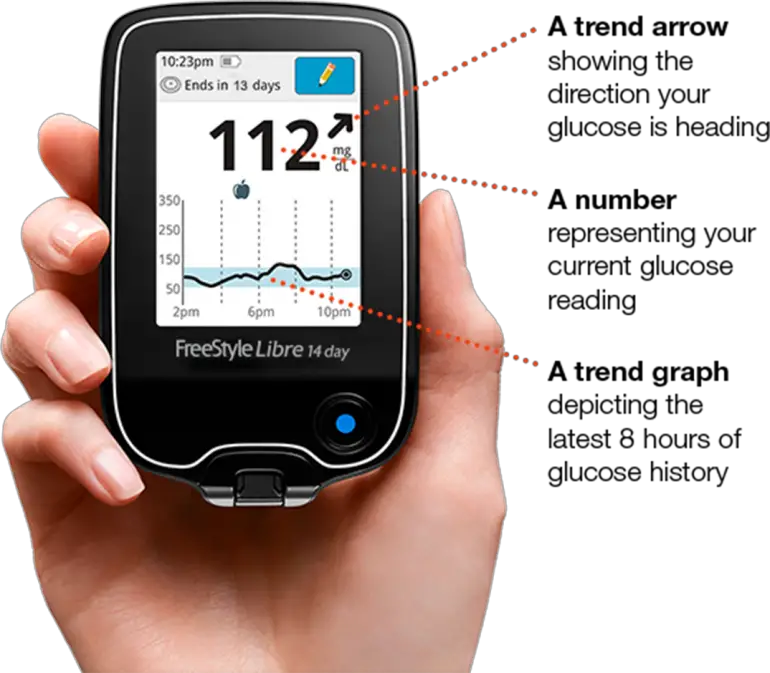
Indicated for diabetes management in patients aged four years or older, the updated version of Abbott’s system can sound the alarm when a user’s glucose is out of range. Data from a 14-day upper-arm sensor is transmitted to a handheld device, which the wearer can use to view their current readings and recent trends.
“Abbott designed the FreeStyle Libre portfolio for performance, access and affordability to make it broadly available to people with diabetes who need it,” Jared Watkin, SVP of diabetes care at Abbott, said in a statement. “By securing reimbursement, Abbott is making sure our latest life-changing technology can get to everyone who needs it, whether they’re children, adults or seniors eligible for Medicare.”
WHAT’S THE IMPACT?
According to the CDC and CMS, diabetes affects roughly 25% of U.S. adults aged 65 years or older.
While prior devices in the FreeStyle Libre family have already been available to this population, access to the Libre 2’s automated alert features could simplify the challenges of glucose management for these older adults.
THE LARGER TREND
Does Medicare Cover Glucose Meter And Supplies
Glucose meters are portable devices that measure blood sugar. They are also known as glucometers.
You must meet the following requirements for Medicare to cover your glucose meter:
- You have been diagnosed with diabetes
- Your doctor has stated that a professional can train you to use this device
- If you cant operate the device, another person will be available to do it for you
- The monitor is for use in your home, rather than clinical use
Medicare Part B covers 80% of the Medicare-approved cost of glucose meters and the supplies needed to operate them after you meet the Part B deductible. These supplies include:
- blood sugar testing strips
- glucose control solutions that check the accuracy of your at-home equipment
Medicare will cover these costs whether or not you use insulin. If you use insulin, you may be eligible for a larger quantity of test strips and other supplies than you would be if you dont use insulin.
Typically, a person who uses insulin will have Medicare coverage for 300 test strips and 300 lancets every three months. If you dont use insulin, youll have coverage for 100 test strips and 100 lancets every three months.
If your physician can prove that its medically necessary for you to receive more supplies than your eligibility indicates, you may be able to get them.
For coverage to take place, your physician and medical supplies provider must both accept Medicare assignment.
Don’t Miss: How Do I Join Medicare
Does Medicare Cover The Freestyle Libre
- Get the facts about Medicare coverage for the FreeStyle Libre. Learn about the cost of the continuous glucose monitor and when it is covered for diabetes treatment.
The U.S. Centers for Disease Control and Prevention estimates that one out of every 10 adults in the United States suffers from diabetes and that approximately 90% to 95% have type 2 diabetes. If you’re one of the more than 34 million Americans living with the disease, blood sugar monitoring is likely a part of your daily routine. Although essential to managing diabetes, traditional blood glucose monitors come with hassles and pain of frequent finger sticks. The FreeStyle Libre simplifies monitoring and is often covered by Medicare.
Does Medicare Cover Freestyle Libre 14 Day
FreeStyle Libre is one of the better known brands of continuous glucose monitors . This monitor, and others like it, have changed the game for many with diabetes.
Not too long ago if you wanted to check your blood glucose levels, you would need to need to pierce your skin several times a day. Then youd have to feed the blood into a monitor to get a reading.
Now, thanks to this fairly new technology of continuous glucose monitors , thats not the case anymore. CGMs let you keep track of your blood sugar level in a less painful and invasive way. And, not only that, but CGMs are more accurate than the traditional way of checking your blood sugar level.
Abbotts FreeStyle Libre is a popular option. And this leads many people to ask the question, does Medicare cover FreeStyle Libre 14 Day?
In this article, we answer that question in clear, plain English. You will also find the average costs of a FreeStyle Libre 14 Day.
Don’t Miss: Is Rollator Walker Covered By Medicare
How Do I Get Medicare To Cover A Cgm
For Medicare to cover the cost of FreeStyle Libre, you must:
- Continue to pay your Part B premium
- Have already paid your Part B deductible
- Receive a prescription for the device from a physician who accepts Medicare
- Buy the CGM from a supplier who accepts Medicare
- Cover whatever portion of the costs that Medicare doesn’t
Medicare Coverage For Therapeutic Cgm
Medicare Part B covers therapeutic continuous glucose monitors such as the Freestyle Libre 2 and the Dexcom G6 for people with diabetes.
Medicare covers therapeutic continuous glucose monitors as durable medical equipment . You will be responsible for your Medicare Part B deductible and 20 percent of the Medicare-approved cost. Medicare will cover the other 80 percent after you meet your deductible.
A Medigap policy also called Medicare Supplement insurance can cover some of your out-of-pocket costs for the Medicare Part B deductible and coinsurance. Additionally, Medicare Advantage plans are required to cover everything included in Medicare Part A and B coverage but may offer additional benefits.
Both Medigap and Medicare Advantage plans are sold by private insurers. Your plans administrator can verify your policys coverage of therapeutic CGM.
Also Check: How Much Is Medicare Part B Now
Medicare Eligibility For A Therapeutic Cgm
A therapeutic CGM is a medical device approved by the U.S. Food and Drug Administration as a replacement for home blood sugar monitors. It provides you and your doctor with the medically necessary information to make diabetes treatment decisions, such as changes in diet and your insulin dosage.
To qualify for a therapeutic CGM, you must be undergoing treatment for diabetes and meet certain other criteria.
To be eligible for a therapeutic CGM under Medicare, you must meet the following requirements.
- You are using insulin to treat Type 1 or Type 2 diabetes.
- You need to check your blood sugar four or more times per day.
- You must use an insulin pump or receive three or more insulin injections per day.
- You must make routine, in-person visits to your doctor.
- Your doctor has determined that you meet all Medicare eligibility requirements.
The decision between a therapeutic CGM or a traditional monitor is one you should make after talking to your doctor. A therapeutic CGM may be a better option if you use insulin and frequently change your dosage.
How Much Does It Cost To Get An Insulin Pump
Medicare covers 80% of the Medicare-approved cost of insulin pumps. You are responsible for the other 20%, plus the Part B deductible and monthly premiums.
Your pump must be prescribed by a Medicare-approved physician and purchased or rented from a Medicare-approved medical supplier for Medicare to cover it.
Also Check: Can You Have Medicare And Medical At The Same Time
What Are The Qualifications For Medicare Coverage For Cgms
Under the guidelines established by Medicare, the following statements must apply to you to qualify for coverage for a CGM:
- You have an established diagnosis of diabetes.
- You are currently using a blood glucose monitor.
- Your doctor recommends that you check your blood sugar four or more times every day.
- You use insulin to control diabetes, and your regimen needs to be adjusted regularly.
- You have been seeing the doctor who will prescribe the CGM for at least 6 months.
- Your doctor has taught you how to properly use the device.
For coverage to continue, you will need to see the prescribing doctor for checkups every 6 months. In addition, you must use the receiver to display your glucose readings. You may use the smartphone app in addition to the receiver to review data or send readings to your medical provider however, you can’t only use your smartphone. This rule exists because a smartphone is not classified as durable medical equipment.