What Types Of In
If your situation meets Medicare criteria, Medicare may cover in-home health care such as:
- Skilled nursing care
- Part-time home health aides
- Medical social services
Medicare benefits might also cover:
- Durable medical equipment
- Medical supplies
- Injectable osteoporosis drugs
If you qualify for home health care under Medicare, you generally dont have to pay any coinsurance or copayment. If you need durable medical equipment, youll typically pay 20% of the Medicare-approved amount as coinsurance. Read more about Medicare and durable medical equipment.
Whats The Difference Between Nursing Home Care Long
Its important to understand the different types or nursing care Medicare may cover, as well as the ones it doesnt, so you arent unexpectedly stuck paying your nursing home costs.
Nursing home care can be either skilled or custodial. Skilled nursing home care covered by Medicare is short-term and expected to help improve your condition. If you have hip replacement, for example, your doctor may recommend a couple of weeks in a skilled nursing facility for physical therapy to help you learn to walk with your new hip and recover your mobility more quickly.
Long-term care, on the other hand, is generally custodial carehelp with things such as eating, bathing, toileting, and dressing. As the name suggests, it may last a period of weeks, months, or years. It is usually not covered by Medicare.
Home care nursing is generally home health care provided by a credentialed medical professional. It can be short-term while you recover from an illness or injury, or long-term if you have a serious chronic condition or have chosen hospice care. Medicare may cover home care nursing under certain situations.
Medicare’s Limited Nursing Home Coverage
Many people believe that Medicare covers nursing home stays. In fact Medicare’s coverage of nursing home care is quite limited. Medicare covers up to 100 days of “skilled nursing care” per illness, but there are a number of requirements that must be met before the nursing home stay will be covered. The result of these requirements is that Medicare recipients are often discharged from a nursing home before they are ready.
Local Elder Law Attorneys in Your City
City, State
In order for a nursing home stay to be covered by Medicare, you have to meet the following requirements:
Note that if you need skilled nursing care to maintain your status , then the care should be provided and is covered by Medicare. In addition, patients often receive an array of treatments that don’t need to be carried out by a skilled nurse but which may, in combination, require skilled supervision. For example, the potential for adverse interactions among multiple treatments may require that a skilled nurse monitor the patient’s care and status. In such cases, Medicare should continue to provide coverage.
You cannot rely on Medicare to pay for your long-term care. Contact your attorney to create a long-term care plan. To find a qualified elder law attorney, .
For more information on Medicare, .
Related Articles
Also Check: Can You Cancel Medicare Part B
When Does Medicare Not Cover In
In most cases, Medicare doesnt cover these types of in-home health care.
- Home health aides, when the only care you need is custodial. That means you need help bathing, dressing, and/or using the bathroom.
- In-home meals
- Round-the-clock care
- Homemaker services, like cleaning, laundry, and shopping. If these services arent in your care plan, and theyre the only care you need, theyre generally not covered.
Its important to know that just because your doctor might recommend home health care, Medicare doesnt automatically cover it. It depends on your situation.
Medicare Covers Medically Necessary Home Health Services
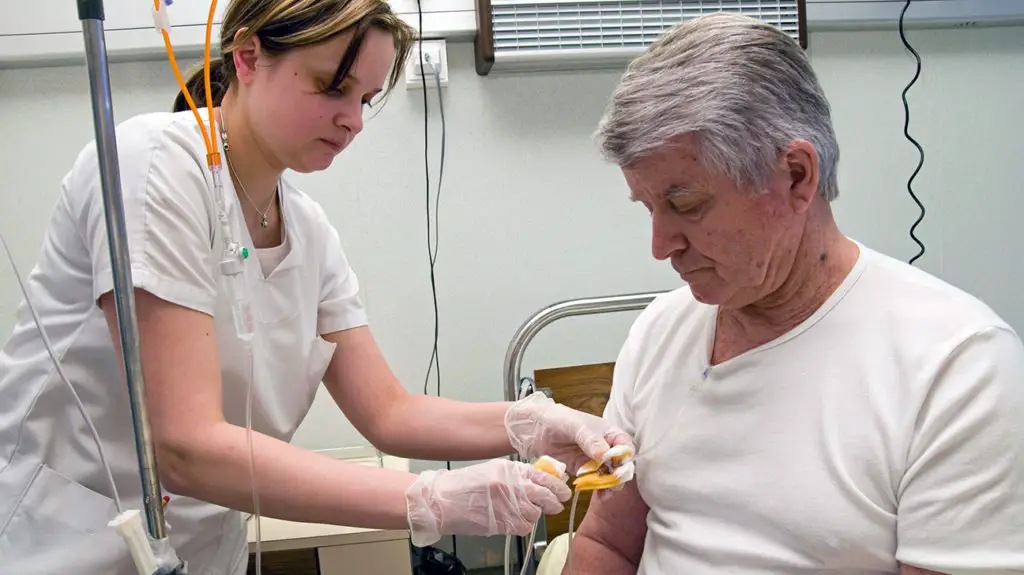
Medicare does not usually cover the cost of non-medical home care aides if that is the only type of assistance that a senior needs. However, a senior who is homebound or requires physiotherapy, occupational health support or other medical assistance in the home may receive assistance with the cost of home health care on a part-time basis via Medicare.
Medicare will cover 100% of the costs for part-time home health services. Part-time means no more than 28 hours a week and no more than eight hours per day. To qualify for home health benefits under original Medicare, a person must have a diagnosis and a relevant prescription from a qualified medical professional. Any home health services must be prescribed by a doctor and reasonably priced, so its important to check the costs of home health services in your area before choosing a provider.
You May Like: What Is A Good Secondary Insurance To Medicare
What Parts Of In
In-home care can cover a wide range of services, but theyre not all covered by Medicare. According to the Medicare site, the in-home care services covered by parts A and B include:
- Part-time or occasional skilled nursing care
- Part-time or occasional health aide care
- Physical therapy
- Occupational therapy
- Speech-language therapy
- Medical social services, such as workers who help make sure youre being billed for the right things and not being abused or taken advantage of by other people on your case
- Durable medical equipment needed to treat your condition
All of these services are covered under parts A and B of Medicare. The prescriptions you receive as part of your treatment are covered by Medicare, too, whether its under parts A and B or under your Part D prescription plan.
The services themselves will cost you zero dollars out of pocket . The only extra cost youll have for home health services is 20 percent of whatever durable medical equipment is needed for your services. Medicare covers the other 80 percent of the costs under your Part B plan.
Skilled Nursing Facility Care Costs
The costs for a rehab stay in a skilled nursing facility are as follows:
- You usually pay nothing for days 120 in one benefit period, after the Part A deductible is met.
- You pay a per-day charge set by Medicare for days 21100 in a benefit period.
- You pay 100 percent of the cost for day 101 and beyond in a benefit period.
Medicare covers inpatient rehab in a skilled nursing facility after a qualifying hospital stay that meets the 3-day rule. The 3-day rule for Medicare requires that you are admitted to the hospital as an inpatient for at least 3 days for rehab in a skilled nursing facility to be covered. You must be officially admitted to the hospital by a doctors order to even be considered an inpatient, so watch out for this rule. In cases where the 3-day rule is not met, Medicare may cover outpatient rehab.
Recommended Reading: Does Medicare Pay For Tdap Shot
How Much Does Knee Replacement Cost With Medicare
Knee replacements are considered a common surgery in the United States, with more than 660,000 procedures done annually as of 2016 according to The New York Times. Because it’s difficult to know exactly what services you’ll need to have a successful surgery until it’s happening, there is no way of knowing exactly how much it will cost beforehand.
Do Medicare Supplement Insurance Plans Cover Nursing Home Costs
Some Medicare Supplement insurance plans include increased coverage in skilled nursing facilities . Medicare Supplement insurance plans may cover your out-of-pocket costs for doctor visits and other medical services covered under Part A and Part B while you are a nursing home resident.
You can start comparing Medicare Advantage plans right away just enter your zip code in the box on this page.
New To Medicare?
Becoming eligible for Medicare can be daunting. But don’t worry, we’re here to help you understand Medicare in 15 minutes or less.
You May Like: Are Medicare Advantage Premiums Deducted From Social Security
Medicare Doesn’t Cover Medical Care Overseas
Medicare usually doesnt cover care you receive while traveling outside of the U.S., except for very limited circumstances . But some medigap plans will cover 80% of the cost of emergency care abroad up to a certain limit. Additionally, some Medicare Advantage plans cover emergency care abroad. Or you could buy a travel insurance policy that covers some medical expenses while youre outside of the U.S. and may even cover emergency medical evacuation, which can otherwise cost tens of thousands of dollars to transport you aboard a medical plane or helicopter.
How Long Will Medicare Pay For You To Be In A Nursing Home
Medicare pays up to 100 days of skilled nursing facility care each benefit period in a skilled nursing facility. If you require skilled nursing facility care for more than 100 days within a benefit period, you will be required to pay out of pocket. If your care is coming to an end because you have exhausted your allotted days, the facility is not obligated to give you with written notification.
You May Like: Can You Sign Up For Medicare Part B Anytime
What Does Medicare Cover For Transitional Care
Medicare will cover TCM when its coordinated by a healthcare provider whos approved by Medicare.
TCM services are covered under Medicare Part B . This is the part of Medicare the covers various outpatient services as well as some preventive care services.
Under Part B, youll be responsible for paying these costs:
- Part B monthly premium. Your monthly premium is the amount that you pay every month for your Part B coverage. The standard Part B monthly premium for 2021 is $148.50.
- Part B deductible. A deductible is the amount you must pay out of pocket before Part B begins covering services like TCM. The Part B deductible for 2021 is $203.
- Coinsurance.Coinsurance is the portion of the cost you pay for covered services after youve met your Part B deductible. For Part B, youre typically responsible for paying 20 percent of the Medicare-approved amount.
TCM involves a face-to-face visit with the provider whos managing your transition within 2 weeks of your discharge. Theyll also communicate with you at home via telephone or email during your transition period.
Will Medicare Cover Physical Occupational And Speech Therapy
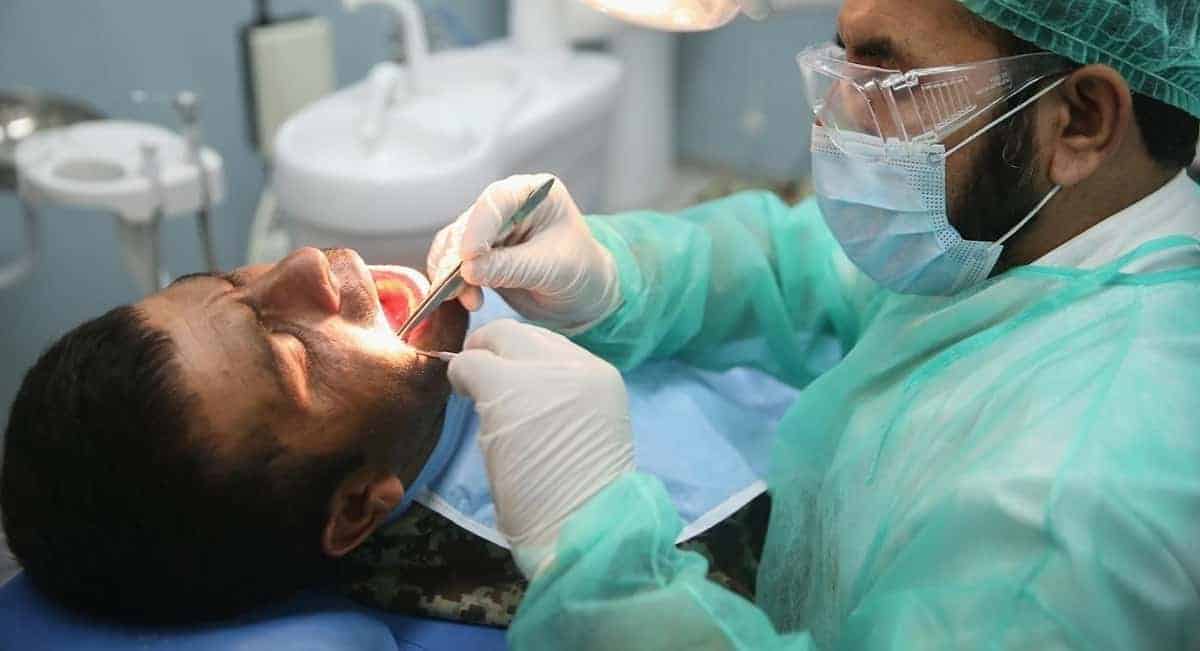
Medicare will pay for physical therapy when its required to help patients regain movement or strength following an injury or illness. Similarly, it will pay for occupational therapy to restore functionality and speech pathology to help patients regain the ability to communicate.
However, Medicare will only pay for these services if the patients condition is expected to improve in a reasonable, predictable amount of time, and if the patient truly needs a skilled therapist to administer a maintenance program to treat the injury or illness at hand.
Recommended Reading: How To Get Medicare To Pay For Hearing Aids
What Are The Requirements For Medicare Nursing Home Coverage
Before Medicare covers skilled nursing home costs, you must have a qualifying hospital stay of at least three inpatient days prior to your nursing home admission. You must have inpatient status for at least three days time spent in the emergency department or observation unit doesnt count toward the three-day requirement.
If you refuse nursing care or medical therapies recommended by your doctor while you are in a skilled nursing facility, you may lose your Medicare nursing home coverage.
Is Skilled Nursing Care Covered
Medicare covers intermittent nursing services. This means that nursing care is provided fewer than seven days a week, or for less than eight hours a day, up to a limit of 21 days. In some cases, Medicare will extend the window if your doctor can provide an accurate assessment of when the care will end.
Skilled nursing services are usually employed to help treat an illness or assist the patient with recovering from an injury. The nurse needs to be licensed to administer the medical treatment you need .
You May Like: Is A Disabled Child Eligible For Medicare Benefits
You May Like: How Much Does Humira Cost With Medicare
How Can I Get Help Paying For A Caregiver
If you or your loved one have exhausted your financial resources paying for in-home caregivers, you may be eligible for both Medicare and Medicaid.
Every state has at least one home- and community-based health services waiver program. If you meet the eligibility guidelines, this type of waiver program could help you pay for things like:
- adult day care
- help with daily personal care
- modifications to your home
- help with housekeeping
If you think you or someone in your family might need custodial care, you may want to consider a long-term care insurance policy to help you cover the cost.
A Medicare supplement plan may also help you pay some of the costs that Medicare wont cover.
Does Medicaid Cover Home Care
Medicaid is a bit less black and white than Medicare because it is administered by the states. Therefore, the state you live in determines which home care services are covered and what eligibility requirements you must meet. In general, you can expect that if you qualify for Medicaid in your state, some level of home care will be covered.
Did You Know: In some states, family members can be paid by Medicaid for providing personal care to their aging loved one.2
To find out whether you are eligible for Medicaid home care and which services are available to you, find your state’s Medicaid profile on Medicaid’s Home & Community Based Services page. Then, contact your state’s Medicaid department directly.
Also Check: How To Get Medical Equipment Through Medicare
Which Parts Of Medicare Pay For Medical Procedures
Which part of Original Medicare pays for what procedures is broadly easy to summarize, but the details can get complicated. As a rule, all of the treatments you get during a multiple-night stay in the hospital fall under Part A, while outpatient treatments, including surgery, are covered by Part B. There are exceptions to these rules:
- Emergency room visits are generally billed to Part B, outpatient treatment, even if you are held overnight in the ER.
- Hospital care after admission through the ER may also be billed as a Part B service if your stay in the hospital is short enough generally less than two consecutive midnights.
- A procedure that is normally done on an outpatient basis, such as nail clipping for people with diabetes, might be billed as an inpatient service if you are already in the hospital for an unrelated matter, such as an invasive surgery.
What Is A House Call Doctor
A house call doctor, or house call physician, is simply a doctor who performs medical visits in the patients place of residence. House call doctors may be employed by an agency, or they may have their own practice.
What Are the Benefits of Physician House Calls?
The primary benefit of physician house calls is that patients receive quality care, from qualified physicians, in the comfort and convenience of their own home or place of residence. Additional benefits of physician house calls include the following:
- It ensures regular medical care to patients who have few or no other options
- It helps monitor and treat both preventable and chronic conditions to keep patients out of ERs and hospitals
- It encourages patients to keep up with regular medical visits by bringing the doctor directly to the patients home
- It saves the patient time and money traveling to the doctors office
Though there are many benefits associated with medical house calls, there are also some challenges, namely that house calls are not ideal for emergency medical problems, and availability of physicians and scheduling options may be limited in some areas.
How Often Do House Call Doctors Visit?
House call visits can be scheduled as often as required by the patient, but on average patients are seen on a monthly basis. Visits are typically scheduled on weekdays, though the physician may be available by phone on weekends or after hours.
Dont Miss: Is Medicare Advantage A Good Choice
Read Also: Can You Be Dropped From Medicare
What Home Health Care Isnt Covered By Medicare
Medicare doesnât cover personal errands that arenât directly related to your care. These services include:
- Laundry
- Grocery shopping
- Cleaning the house
Medicare also doesnât cover many long-lasting supplies. Home health care agencies usually donât use these types of items for your treatment. These supplies include:
- Motorized stairway elevators
Medicare doesnât cover prescription drugs as part of home care.
Medicare Doesn’t Cover Routine Vision Care

Medicare generally doesnt cover routine eye exams or glasses . But some Medicare Advantage plans provide vision coverage, or you may be able to buy a separate supplemental policy that provides vision care alone or includes both dental and vision care. If you set aside money in a health savings account before you enroll in Medicare, you can use the money tax-free at any age for glasses, contact lenses, prescription sunglasses and other out-of-pocket costs for vision care.
Also Check: How To Cancel Medicare Online
Medicare Coverage For Nursing Home Care
It is not that Medicare does not pay for any nursing home care. It does pay for some, but only if you were recently admitted to the hospital and only if you require skilled care at least five days per week.
Not only do you need to have been hospitalized to qualify for this Medicare Part A coverage, but you need to have been admitted as an inpatient for at least three days. Trickily, the day you are transferred to the skilled nursing facility does not count, and even more tricky is how CMS defines inpatient care.
These days you can stay overnight in the hospital, but that does not mean you are an inpatient. Thanks to legislation put forth in October 2013, known as the Two-Midnight Rule, you may only be considered for inpatient care if your stay is expected to last longer than two midnights and if your level of care is considered medically necessary. That means you cannot be in the hospital receiving care that could just as easily be administered elsewhere.
Otherwise, you will be placed under observation, care that is covered by Medicare Part B.
In the case that you do get approval for skilled nursing care, Medicare Part A covers the first 20 days for you. For days 21 to 100, you will pay $176 per day as of 2020. After 100 days, you are on your own.