Outpatient Care Covered By Medicare Part B
Outpatient care covered by Medicare Part B is the doctor care and services you receive in a hospital. However, it does not require an overnight stay in the hospital. Examples of services covered as an outpatient may include surgery, lab work, and medicine administered intravenously. In addition, EKGs are covered under outpatient care. Also, an Emergency Department visit is considered an outpatient service covered by Medicare Part B.
What Medicare Part D Doesnt Cover
Medicare Part D is optional prescription drug coverage. You can enroll in this coverage through a stand-alone Medicare Part D Prescription Drug Plan, or through a Medicare Advantage Prescription Drug plan.
Each Medicare Prescription Drug Plan has a formulary. The formulary may change at any time. You will receive notice from your plan when necessary.
Generally, Medicare Part D will cover certain prescription drugs that meet all of the following conditions:
- Only available by prescription
- Approved by the Food and Drug Administration
- Sold and used in the United States
- Used for a medically accepted purpose
- Not already covered under Medicare Part A or Part B
Based on these criteria, there are certain drugs that Medicare Part D does not generally cover:
- Weight loss or weight gain drugs
- Erectile or sexual dysfunction drugs
- Over-the-counter, non-prescription drugs
- Hair growth drugs, or drugs used for cosmetic reasons
- Fertility drugs
- Drugs used for symptomatic relief of coughs or colds
- Prescription vitamins and minerals
If you are taking a medication that is not covered by Medicare Part D, you may try asking your plan for an exception. As a beneficiary, you have a guaranteed right to appeal a Medicare coverage or payment decision.
- If you prefer, I can speak with you by phone or email you information just use the links below to request either of those.
- To look at Medicare plan options at your pace in the convenience of your home, use the Compare Plans buttons on this page.
Coverage For Psychiatric Hospitalization
For inpatient psychiatric care, Medicare Part A will pay for the same kinds of services as if you were hospitalized in a general hospital:
- Semiprivate room
- Rehabilitation services, such as physical or occupational therapy
- Prescription drugs administered in the hospital
- Medical supplies
- Lab tests, X-rays, and radiotherapy
An important distinction from care in a general hospital is that you must use a facility that accepts Medicare assignments on all claims. Deductibles and coinsurance costs are the same as for a regular inpatient hospital stay. In the course of your life, Medicare will only pay for 190 days of inpatient psychiatric care .
Don’t Miss: Is Stem Cell Treatment Covered By Medicare
Medical Equipment And Supplies
Splints, casts, prosthetic devices, body braces, heart pacemakers, corrective lenses after a cataract operation, therapeutic shoes for diabetics, and medical equipment such as ventilators, wheelchairs, and hospital beds if prescribed by a doctorare all covered by Part B medical insurance. This includes glucose monitoring equipment for people who have diabetes.
To learn more about the many types of medical equipment and supplies Medicare Part B covers, and how different equipment may be rented or purchased, see Medicare’s online publication Medicare Coverage of Durable Medical Equipment and Other Devices. To find a Medicare-certified supplier of medical equipment near you, go to the Medicare website home page at www.medicare.gov and click on “Help & Resources” and then “Where to get covered medical items.”
What Does Part B Cover
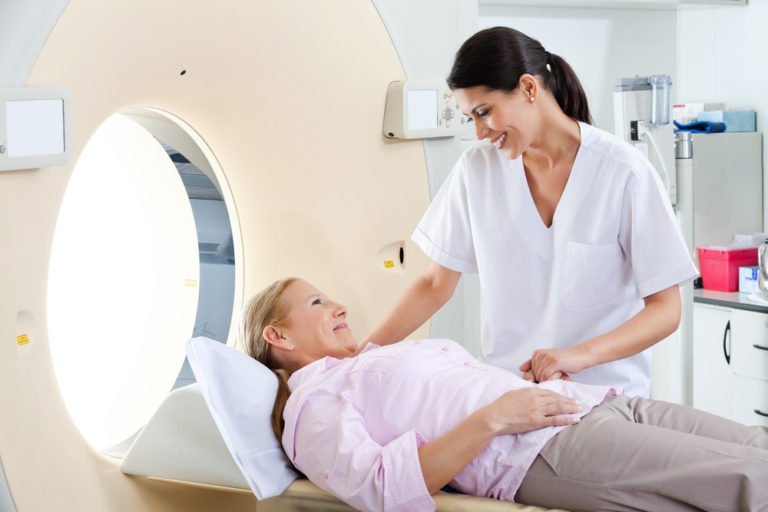
If a person has to stay at an ER overnight or for longer than 24 hours, hospital personnel should give them a Medicare Outpatient Observation Notice .
Receiving a MOON form usually means that Part B, not Part A, will cover the initial ER visit.
Medicare Part B usually covers most aspects of an individuals visit to an ER, as long the doctor does not admit them to the hospital for reasons related to the visit.
If the doctor discharges a person from the ER to their home, they may be responsible for some or all of the following costs under Part B:
- a copayment for the emergency department visit
- a copayment for hospital services provided, such as imaging studies, medications, or lab work
- 20% of the Medicare-approved amount for a doctors services
- the deductible, which applies for doctors services
One exception to the ER coverage rules applies when a person returns to a hospital in need of inpatient care within 3 days of their initial visit to the ER.
If the hospital admits the person with the same medical condition, they do not have to pay their Part B copayment twice.
Medicare Part B also pays for ambulance and helicopter transportation when a person urgently requires moving to another location and is unable to get there without medical assistance.
The out-of-pocket expenses for emergency transportation to an ER include the 20% coinsurance. The Part B deductible applies to this amount.
Otherwise, they may have to pay more for seeking care at an out-of-network facility.
You May Like: Does Medicare Pay For Drug Rehab
Medicare Doesn’t Cover Long
One of the largest potential expenses in retirement is the cost of long-term care. The median cost of a private room in a nursing home was roughly $105,800 in 2020, according to the Genworth Cost of Care Study a room in an assisted-living facility cost $51,600, and 44 hours per week of care from a home health aide cost $54,900.
Medicare provides coverage for some skilled nursing services but not for custodial care, such as help with bathing, dressing and other activities of daily living. But you can buy long-term-care insurance or a combination long-term-care and life insurance policy to cover these costs.
Is Medicaid Part Of Medicare
Medicare and Medicaid are different programs. Medicaid is not part of Medicare. Heres how Medicaid works for people who are age 65 and older: Its a federal and state program that helps pay for health care for people with limited income and assets. A basic difference is that Medicaid covers some benefits or services that Medicare doesnt like nursing home care or transportation to medical appointments .
Visit your states Medicaid/Medical Assistance website or medicare.gov for more information. Learn more in the article Can I get help paying my Medicare costs?
WANT TO KEEP LEARNING HOW MEDICARE WORKS?
You May Like: What Nursing Homes Take Medicare
How To Enroll In Medicare Part A
If you believe you would benefit from Part A coverage and qualify for it, the final step is the Part A enrollment process. If you are near the Medicare eligibility age of 65, its crucial to understand how your Initial Enrollment Period works.
Your IEP begins three months before the month you turn 65. The IEP is open for a total of seven months and allows you to enroll in Medicare Part A and Part B. During your IEP, and after you enroll in Part A and Part B, you can choose to add coverage like Part D or enroll in a Medicare Advantage plan that replaces Parts A and B.
Is It Hard To Find A Medicare Doctor
Youre not tied to a specific doctor with Original Medicare, so you can switch providers at any time.
You might find that the doctor you want has simply stopped accepting new patients, just like youd encounter with private insurance. Medicare is great, but it cant magically solve healthcare problems.
A significant minority of Medicare beneficiaries have had to shop around for a doctor who accepts new Medicare patients. Its always a good idea to ask around and learn who your friends or coworkers see. You may have to call more than one doctor to find care, but there should always be a qualified doctor available for you.
You May Like: Which Medicare Plan Covers Hearing Aids
How Much Does Observation In Hospital Cost With Medicare
If you receive hospital observation services but are not admitted as an inpatient, your doctors services are covered by Medicare Part B.
You typically must pay a 20 percent coinsurance for your Part B-covered care after you meet the Part B deductible .
Theres no limit to how much you might be charged for the Part B 20 percent coinsurance.
If you have a Medicare Advantage plan, however, your plan includes an out-of-pocket spending limit. This could potentially save you money in out-of-pocket Medicare costs related to your hospital stay.
Speak with your doctor for specific cost and coverage information related to your observation services.
Medicare Coverage Of Home Health Services
Medicare Part A covers certain home-health services, such as physical therapy, occupational therapy, speech-language pathology services, and part-time or intermittent skilled nursing care.
You may be covered if you need the above types of services and your doctor certifies that youre homebound, meaning that you have a health condition that makes it difficult to leave the house without assistance or major effort. You must be receiving the home health services through a Medicare-certified home health agency and be under a plan of care that is created by and regularly reviewed by your physician.
Medicare home health coverage doesnt include round-the-clock home care, home-delivered meals, homemaker services, or custodial care.
You May Like: What Weight Loss Programs Are Covered By Medicare
In General Part A Covers:
Medicare Parts A and B coverage details| Services | You pay in 2021 | ||
|---|---|---|---|
|
HospitalizationSemi-private room and board, general nursing and other hospital services and supplies |
First 60 days |
||
|
91st to 150th day (60 reserve days may be used only once |
All but $742/day |
||
|
All costs |
|||
|
Skilled nursing facility careSemi-private room and board, skilled nursing and rehabilitative services and other services and supplies |
First 20 days |
||
|
All costs |
|||
|
Home health carePart-time or intermittent skilled care, home health aide services, durable medical equipment and supplies and other servicesNote: Doctor must order care and a Medicare-certified home health agency must provide it |
Unlimited, as long as you meet Medicare requirements for home health care benefits |
100% of approved amount 80% of approved amount for durable medical equipment |
Nothing for services 20% of approved amount for durable medical equipment |
|
Hospice carePain relief, symptom management and support services for the terminally ill – meaning you have a life expectancy of six months or less |
For as long as doctor certifies need |
All but limited costs for outpatient drugs and inpatient respite care |
Limited cost sharing for outpatient drugs and inpatient respite care |
|
Blood*When furnished by a hospital or skilled nursing facility during a covered stay |
Unlimited during a benefit period if medically necessary |
All but first three pints per calendar year |
For first three pints |
1 – Neither Medicare or Medigap insurance pay for most nursing home care .
Get More From Your Medicare Coverage
To learn more about your Medicare Advantage plan options and to compare plans that cover transportation that may be available where you live, call to speak with a licensed insurance agent today.
Or call to speak with a licensed insurance agent. We accept calls 24/7!
About the author
Christian Worstell is a licensed insurance agent and a Senior Staff Writer for MedicareAdvantage.com. He is passionate about helping people navigate the complexities of Medicare and understand their coverage options.
His work has been featured in outlets such as Vox, MSN, and The Washington Post, and he is a frequent contributor to health care and finance blogs.
Christian is a graduate of Shippensburg University with a bachelors degree in journalism. He currently lives in Raleigh, NC.
Where you’ve seen coverage of Christian’s research and reports:
1 Lyft. Economic Impact Report 2019. Retrieved Aug. 2019 from https://www.lyftimpact.com/stats/national.
2 Minemyer, P. Why Lyft is making Medicare Advantage a key focus of its healthcare work. FierceHealthcare. Retrieved from www.fiercehealthcare.com/payer/why-lyft-making-medicare-advantage-a-key-focus-its-healthcare-work.
3 Lyft. Addressing Health and Wellbeing Through Better Transportation. . Retrieved from blog.lyft.com/posts/2019/2/5/addressing-health-and-wellbeing-through-better-transportation.
Medicare has neither reviewed nor endorsed this information.
You May Like: Will Medicare Pay For My Nebulizer
Do You Need Medicare Part A For Hospital Coverage
If you, like most people, dont have to pay a monthly premium for Part A, there is no downside to enrolling when you become eligible at age 65. You dont have to pay a premium if you have paid Medicare taxes for at least 10 years.
If you face an inpatient hospital stay and have Part A, you will still be responsible for some costs. Those costs, however, are significantly reduced.
Medicare Doesn’t Cover Deductibles And Co
Medicare Part A covers hospital stays, and Part B covers doctors services and outpatient care. But youre responsible for deductibles and co-payments. In 2021, youll have to pay a Part A deductible of $1,484 before coverage kicks in, and youll also have to pay a portion of the cost of long hospital stays — $371 per day for days 61-90 in the hospital and $742 per day after that. Be aware: Over your lifetime, Medicare will only help pay for a total of 60 days beyond the 90-day limit, called lifetime reserve days, and thereafter youll pay the full hospital cost.
Part B typically covers 80% of doctors services, lab tests and x-rays, but youll have to pay 20% of the costs after a $203 deductible in 2021. A medigap policy or Medicare Advantage plan can fill in the gaps if you dont have the supplemental coverage from a retiree health insurance policy. Medigap policies are sold by private insurers and come in 10 standardized versions that pick up where Medicare leaves off. If you buy a medigap policy within six months of signing up for Medicare Part B, then insurers cant reject you or charge more because of preexisting conditions. See Choosing a Medigap Policy at Medicare.gov for more information. Medicare Advantage plans provide both medical and drug coverage through a private insurer, and they may also provide additional coverage, such as vision and dental care. You can switch Medicare Advantage plans every year during open enrollment season.
Read Also: What Is The Difference Between Medicare Supplemental And Advantage Plans
Skilled Nursing Facilities And Home Health Care
Under some circumstances, Medicare will cover some of the cost of inpatient treatment in a skilled nursing facility or visits from a home health care agency. Your stay in a skilled nursing home facility or home health care is covered by Medicare Part A only if you have spent three consecutive days, not counting the day of discharge, in the hospital. Your skilled nursing stay or home health care must begin within 30 days of being discharged. For more information, see our articles on Medicare coverage of skilled nursing facilities and Medicare coverage of home health care.
Medicare Part A Coverage
In summary, there are a lot of key coverage benefits received from Medicare Part A:
- In-patient hospital care including: Long-term care hospitals, Acute care or critical access hospitals, Rehabilitation facilities and more
- Skilled nursing facilities and the following services: Semi-private room, Skilled nursing care, Meals, Physical and occupational therapy, Medications, Medical social services and more
- Medicare inpatient mental health coverage. If youre getting care in a psychiatric hospital, Medicare Part A covers up to 190 days of inpatient hospital services in your lifetime.
- Medicare hospice coverage. If a beneficiary qualifies, they are eligible to receive: Physician services, Nursing services, Durable Medical equipment, Physical therapy and occupational therapy, Prescription drugs and more
- Home health services including physical therapy, occupational therapy, speech-language pathology services, and part-time or intermittent skilled nursing care
This website and its contents are for informational purposes only. Nothing on the website should ever be used as a substitute for professional medical advice. You should always consult with your medical provider regarding diagnosis or treatment for a health condition, including decisions about the correct medication for your condition, as well as prior to undertaking any specific exercise or dietary routine.
New To Medicare?
You May Like: How Much Is Medicare Going Up
How Do Medicare Part A Premiums Work
Once you turn 65, youll either be eligible for premium-free Part A, or you can choose to pay Part A premiums if you havent worked long enough to earn premium-free coverage.
The amount you owe will depend on how long you or your spouse worked and paid Medicare taxes:
| $471 per month |
You have the ability to go without buying Part A and only purchase Part B. But, often, if you decide to buy Part A, you will need to have Part B and to pay monthly premiums for Parts A and B.
Heres What Medicare Part A Covers
Medicare Part A generally covers medically necessary services and supplies needed to treat a certain disease or condition and care when youre a hospital inpatient in a Medicare-enrolled hospital. The following list describes some of the main services and supplies Part A specifically covers .
- Hospital care: If youre admitted as an inpatient, Medicare covers semi-private rooms, prescription drugs given as part of your inpatient treatment, meals, general nursing, and more.
- Long-term care hospitals: Medicare covers long-term care hospital services if you were transferred from an acute-care hospital or admitted to the long-term care hospital within 60 days of being discharged from an inpatient hospital stay.
- Skilled nursing facility care: If your doctor determines that you need care in a Medicare-certified skilled nursing facility, Medicare Part A covers certain services and supplies, generally for a limited time.
Medicare may cover services and supplies including, but not limited to: semi-private rooms, meals, skilled nursing care, medications, medical supplies and equipment, and ambulance transportation. There are several qualifying factors that determine whether Medicare will cover your stay in such a facility.
Don’t Miss: What Are The Advantages And Disadvantages Of Medicare Advantage
What If A Doctor Refuses My Medicare Card
If youre having billing issues, relax and make sure youre using the right card. The card you need to use will depend on your plan and the care youre seeking. If you have supplementary coverage, you may need more than one card.
Medicare cards are generally just used to verify your eligibility and billing information. You may not need to provide them after you visit a doctor for the first time.
If your card is faded from use, you can replace your card by:
- Logging into your Social Security account at ssa.gov,