Costs And Other Savings Options
The average cost of contact lenses can vary. Contacts range in features from daily disposable lenses to those that correct astigmatism or act as bifocals. A basic pair of soft contact lenses you replace every 2 weeks usually costs about $22 to $26 for a box of six pairs. When you consider costs per eye, youll usually spend about $440 to $520 for contact lenses alone per year.
Youll also pay for accessories that help you take care of your contacts. These can include contact lens cases, contact lens solutions, and eye drops if you have dry eyes.
Well be honest: Its a little harder to get help paying for contacts compared to eyeglasses when you have vision needs. Because glasses last longer than contacts and can be used and reused from donated materials there are more organizations that may help you get a pair of free or low-cost eyeglasses. However, you can save money on your contacts through these approaches:
Does Medicare Cover Eye Prostheses
Eye prostheses are covered for patients with absence or shrinkage of an eye due to birth defect, trauma or surgical removal. Medicare covers polishing and of the artificial eye, and typically covers replacement every five years.
You pay 20% of Medicare-approved amounts after the Part B deductible is applied.
Medicare Advantage Plans With Dental And Vision
Vision coverage is just one example of options offered by many Medicare Advantage plans. Unlike Original Medicare, many Medicare Advantage plans cover vision, dental and hearing coverage, and some plans also provide a yearly stipend that can be used to purchase personal items like vitamins and toothpaste.
If youre on Original Medicare and require or desire additional services, contact GoHealth to review your options.
Also Check: Does Medicare Pay For Dental Visits
What Medicare Covers Is Not Always Clear
Q. Does Medicare cover all items and services associated with cataract surgery?A.Q. Which items and services associated with cataract surgery are covered by Medicare?
A.Q. If we perform both an A-scan and an IOLMaster , may we bill one of the tests to the patient as a noncovered test?A.Q. Does Medicare cover anything else associated with cataract surgery?A.Q. If diagnostic tests are performed in the postoperative period after cataract surgery, are they covered by Medicare?A.Medicare Claims Processing ManualQ. Are Medicare beneficiaries required to sign an ABN before receiving any non-covered items or services?A.Q. Are there diagnostic tests that may be offered to cataract patients that would be considered noncovered by Medicare? A.Q. Are there any noncovered charges for evaluation and treatment of astigmatism at the time of cataract surgery?A.Q. Are there any noncovered charges associated with patients considering pseudophakic monovision? A.Q. Does the patient get to decide whether to have these noncovered tests?A.Q. Are there any noncovered services associated with conventional IOLs within an ambulatory surgery center?A.Q. Does the patient benefit from having these noncovered tests and services?A.Ms. McCune is vice president of the Corcoran Consulting Group. Contact her at .
The Current Healthcare Coverage Landscape Can Be Tricky To Navigate Knowing These Essentials Can Help
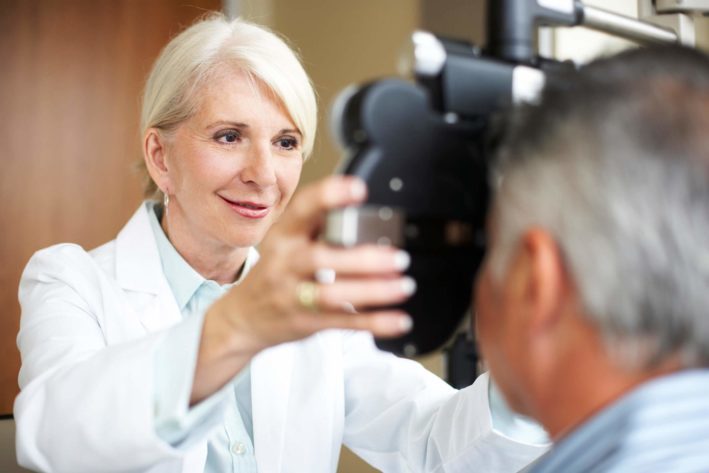
The dichotomy of todays healthcare environment can be both exciting and frustrating. Point-of-care innovations are at an all-time high, but the associated coverage is confusing and constantly changing. New technologies we would like to offer our patients may be out of reach due to blurred lines between medical coverage and refractive coverage, carrier coverage policy decisions and shifts in payer policyall of which force the consumer to take on a larger share of the cost through higher deductibles and copays.
This conundrum is best exemplified with the billing and coding of medically necessary contact lenses.
| Scleral lenses are often medically necessary for patients with irregular corneas, as seen here. |
No ConsensusThe definition of medically necessary contact lenses should be clear by now, yet it continues to be parsed, segmented and redefined by third party carriers. Practitioners may have to bear part of the blame for this as well, as some fall short in establishing and documenting true medical necessity for a contact lens fit with respect to specific pathologies. From the payer perspective, some waste and abuse has occurred, resulting in greater scrutiny and tightening of payer policies. Because of this, medically necessary contact lenses have different definitions based upon the carrier providing the benefits. Here are a few examples:
Anisometropia of 3D in meridian powers.
High ametropia exceeding -10D or +10D in meridian powers.
Read Also: Does Medicare Pay For A Rollator
Medicare Glasses Coverage: When Will Medicare Pay For Prescription Lenses
Although eye care is a common need as we age, Medicare coverage for most vision services is extremely limited. It is generally predicated on whether you experience certain medical conditions that may affect your eyesight.
Prescription lenses includes glasses and contact lenses. And the only time Medicare helps pay for glasses or contacts is if you have an intraocular lens implanted during cataract surgery. Coverage for this service falls under Medicare Part B.
At all other times, you are responsible for 100 percent of the cost of prescription eyeglasses or contact lenses.
Will Medicare Pay For Treatment For A Detached Retina
A detached retina can cause permanent vision loss if not treated quickly. Medicare will cover surgery to repair a detached retina, but youll be responsible for your Part B deductible and 20% coinsurance, which Medigap can help take care of. Depending on where you have your procedure, a copayment might apply as well. Similarly, Medicare Advantage will cover retina surgery to preserve vision, although your out-of-pocket costs will depend on your plan.
Read Also: How Does Medicare Part D Deductible Work
Undergoing Cataract Surgery With Part B
Part B covers your outpatient care and is most likely what you will use to cover your cataract surgery. Under Part B, only 80% of the cost of your cataract surgery will be covered. You will be responsible for the remaining 20%. Part B will cover your lens implant, removal, and the prescription glasses or contact lenses covered for the procedure. The Part B deductible is quite low at $198.
Will Medicare Cover Treatment For Glaucoma
Glaucoma is a disease that damages the optic nerve, potentially resulting in vision loss. Medicare Part B will cover annual glaucoma screenings for those considered high-risk, including diabetics and older Americans with a family history of the disease. African Americans aged 50 and older, and Hispanic individuals aged 65 and over are also considered high-risk.
Youll still be responsible for your Part B deductible and if youve already met the deductible, 20% of the cost of your exam. .
Glaucoma treatment is generally covered under Medicare. Outpatient laser surgery falls under Part B, and eye drops to address the condition fall under Medicare Part D. Your out-of-pocket costs associated with your drops will depend on your Part D plans formulary.
Because Medicare Advantage is required to provide coverage for the conditions that are covered by Original Medicare, it also covers glaucoma screenings and treatment. But because Medicare Advantage plans can design their own benefits, the out-of-pocket costs can vary considerably from one plan to another.
Medigap, meanwhile, can cover some or all of the costs associated with your glaucoma screening and treatment under Original Medicare by picking up the tab for your deductibles and coinsurance. And if you have supplemental coverage provided by an employer, your out-of-pocket costs will depend on the specifics of the plan.
Also Check: What Are The Types Of Medicare Advantage Plans
Does Medicare Part D Pay For Prescription Lenses
Medicare Part D provides prescription drug coverage, which is not included with Original Medicare. And although prescription lenses are prescribed by an eye doctor , they are not covered by Medicare Part D.
You can compare your Medicare Part D and Advantage plan options with our Find a Plan tool. Just enter your location and coverage start date to review Medicare plans in your area.
How Can I Get Medicare Coverage For Eye Exams
In most cases, the only way to get Medicare coverage for routine eye exams is through a Medicare Advantage plan. Medicare Advantage plans are offered by private insurance companies and have slightly different rules than Original Medicare.
Under federal law, all Medicare Advantage plans must offer, at a minimum, all the benefits available under Medicare Part A and Part B. Once those minimums are met, Medicare Advantage plans can offer other additional benefits that make them more attractive to their members. For example, many Medicare Advantage plans offer benefits for routine annual eye exams. You may have to pay a copayment or coinsurance amount for these exams, and depending on the plan you choose, you may have to see an eye doctor that participates in your plans network.
If you need prescription eye drops or other medications for an eye condition, most Medicare Advantage plans also include Part D coverage for prescription drugs. Some plans even include benefits or discounts for certain over-the-counter medications and drops.
Many Medicare Advantage plans also cover prescription eyeglasses and contact lenses. You may have to pay a copayment or coinsurance amount, or the plan may simply pay a flat fee amount toward the purchase of corrective eyewear.
Do you have any questions about your Medicare coverage of eye exams? Feel free to enter your zip code on this page to browse Medicare plan options in your area.
New To Medicare?
Read Also: How Do You Qualify For Medicare Part A And B
Does Medicare Cover Glaucoma Screening
Medicare Part B covers a glaucoma screening test once every 12 months for people at high risk for glaucoma. This includes people with diabetes, a family history of glaucoma, African Americans who are age 50 or older, and Hispanic Americans who are age 65 or older. The screening must be done or supervised by an eye doctor who is legally allowed to do this service in your state.
You pay 20% of Medicare-approved amounts, and the Part B deductible applies.
Which Lenses Are Covered By Medicaid

If you need a new pair of glasses, you must find out the types of lenses covered by Medicaid. Medicaid will pay for regular single-vision lenses, meant to correct near and distance vision.
If you need bifocals or trifocals, no need to worry, Medicaid will also pay for them. Bifocals and trifocals are expensive, so Medicaid only covers one pair per year.
For single-vision glasses, Medicaid will cover two pairs per year because they are relatively cheap.
Some of the lenses not covered by Medicaid include:
If youd like to get any of the above lenses, you can still use your Medicaid coverage. However, you will incur out-of-pocket costs because these are specialty lenses.
Read Also: Medicaid South Dakota Income Guidelines
Don’t Miss: Is Medicare A Form Of Socialism
When Does Original Medicare Cover Eye Exams
Eye exams may be covered for Medicare beneficiaries who have certain medical conditions. Coverage is under Medicare Part B. Your provider must accept assignment, the Part B deductible applies, and your out-of-pocket cost is 20 percent of the Medicare-approved amount. If you receive services as a hospital outpatient, your out-of-pocket may also include a copayment in addition to your 20 percent Part B coinsurance.
The following vision care is covered by Medicare Part B:
What Does Medicare Pay For
Most Medicare beneficiaries are enrolled in the Original Medicare program, which consists of Medicare Part A and Part B.
Part A is the hospital inpatient benefit that pays most of the cost for enrollees inpatient hospital stays. Part B is the outpatient services plan that pays for most medical office visits and some home services, medical supplies and other medically necessary outpatient treatments.
You May Like: Is Medical Part Of Medicare
Does Medicare Cover Cataract Surgery
- 80% of the cost of cataract surgery is covered under Part B.
- Coverage is the same whether or not laser technology is used.
- Most Medicare Advantage plans will cover cataract surgery.
Simply put, Medicare does cover cataract surgery. However, there are multiple types of cataract surgery, and Medicare only covers one very specific set of procedures.
- Lens implants
- One set of eyeglasses or contact lenses
Most cataract surgery isnt any more complex than the items included above, but there are a few special circumstances where your surgery may not be fully covered. We will discuss these special circumstances in more detail later on. Its important to emphasize that Medicare will cover one set of eyeglasses or contact lenses after your surgery, even though Medicare does not usually offer this coverage.
Does Medicare Cover Routine Vision Services
Original Medicare wont pay for routine vision services like eye exams, prescription glasses, or contact lenses. But theres an exception to this if youve just had cataract surgery in that case, Medicare Part B will cover some of the cost of a single pair of glasses or set of contact lenses . And if you have a medical condition that requires custom eyeglasses or contact lenses, Medicare might pick up the tab.
On the other hand, Medicare Advantage generally covers standard vision testing, as well as glasses or contacts. If youre going to stick to original Medicare but want coverage for routine vision services, supplement insurance wont solve that problem Medigap wont pay for vision care or eyeglass benefits, either. But if you have maintained supplemental coverage from a current or former employer, that coverage might include vision benefits, so be sure you understand any benefits you might have before you pay full price for eye exams and corrective lenses.
Recommended Reading: How Much Is Premium For Medicare
Medicare And Cataract Surgery Frequently Asked Questions
- How bad do cataracts have to be to qualify for surgery?
For Medicare coverage, your physician needs to determine that the procedure is medically necessary. Due to the slow progression of cataracts, many people may delay cataract surgery or choose nonsurgical methods on the advice of their physician. If cataracts affect your day-to-day activities and result in significant vision loss or blurred vision, then its time to reconsider.
Amie Clark
Amie has been writing about senior care products and services for the last decade. She is particularly passionate about new technologies that help improve the quality of life for seniors and their families. Seeing her parents and grandparents age made Amie ask herself, Would this be good enough for my loved ones? In her spare time, Amie enjoys outdoor adventures and spontaneous road trips. Learn more about Amie here
Information
Cost Of Cataract Surgery With Medicare
Cataract surgery can be expensive, but there are ways to offset the cost with certain Medicare plans. Out-of-pocket cataract surgery generally costs upwards of $3,700.
As a hypothetical example, Brenda is a 67-year-old woman with diabetes who needs cataract surgery for only one eye, which starts at $3,783. Medicare covers approximately 80 percent of the cost, but she would be required to pay the 20 percent coinsurance in addition to the Part B deductible, which is $203 for 2021.
Heres what Brendas costs may look like:
| Cost of cataract surgery | |
|---|---|
| $203 | $959.60 |
FYI: Are you looking for quality medical alert systems for people with vision problems? Read my article on medical alert systems for the blind.
Recommended Reading: Can You Get A Medicare Card Online
What Do Eye Exams Cost With Medicare
As mentioned, Medicare generally doesnt cover routine eye exams, but there are exceptions for high-risk patients.
The average cost of eye exams without insurance ranges between $50-$70. Most insurance policies dont usually cover routine eye exams and might have additional copays. Since routine eye exams are generally not covered by Medicare, youd pay 100 percent of their cost.
Also Check: What Does Cigna Medicare Supplement Cover
How Much Do Medicare Eye Exams Cost
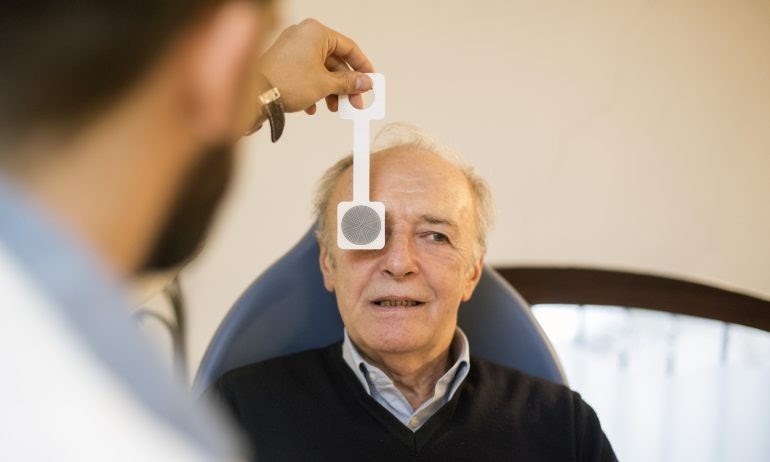
As previously stated, Medicare typically does not cover routine eye exams, but there are some exceptions for high-risk patients.
Without health coverage, the average cost of an eye exam is between $50 and $70. Most insurance plans do not cover routine eye exams, and there could be additional copays. You would be responsible for the entire cost because Medicare does not cover regular eye exams.
Also Check: Who Offers Medicare Supplemental Insurance
Does Medicare Part A Cover Eyeglasses
Original Medicare includes two parts. Part B is sometimes known as medical insurance, because it covers outpatient services like doctor visits and lab work. Medicare Part A is also known as hospital insurance. It helps pay for inpatient care received in a hospital or skilled nursing facility as well as hospice care.
Medicare Part A does not cover vision services, routine eye exams, or prescription lenses.
Do You Wear Glasses Youll Want To See This
According to the Vision Council of America, approximately 75% of adults use some sort of vision correction.1 Whether its eyeglasses, contacts or cheater readers, thats a pretty big number.
Given that number, you may be surprised to learn that, unlike most Medicare Advantage plans, Original Medicare does not cover routine vision care.
It does, however, cover medically necessary treatments that may improve or cure chronic eye conditions like glaucoma or cataracts. But youll need to check with your doctor to see if your condition makes the cut. For example, Lasik surgery for vision correction is not considered a medical necessity, so its not covered by Medicare.
Dont Miss: Does Medicare Pay For Breast Reconstruction
Don’t Miss: Will Medicare Help Pay For A Walk In Tub
Contact Lenses For New Orleans Medicaid Recipients At Eyes On Canal
Where contact lenses are concerned, the following is important to know for New Orleans Medicaid recipients:
- Medicaid does reimburse for both soft and rigid contact lenses
- If either soft or rigid lenses could be used, Medicaid will approve the least expensive type
- All contact lenses require prior authorization by Medicaid
- Contact lenses will be considered only when medically necessary and no other means can restore vision such as an eye disorder like astigmatism, irregular cornea, keratoconus, and more that are not correctable by eyeglasses
- Medicaid does not reimburse for contact lenses for cosmetic purposes.
