Medicare Coverage Guidelines For Lower Back Pain Management Injections
Per the standard Medicare guidelines, cortisone injections usually receive coverage without prior authorization. Also, different doses have different costs. Make sure to ask your doctor about the allowable amount for each procedure.
Supplement coverage is crucial for those with lower back pain management needs. When undergoing pain management treatments, supplemental insurance protects you financially.
There are many different types of injections for treatment available to those with either chronic or acute conditions. Well acquaint you with some of the most common examples below.
The Risks Of Spinal Decompression
A review of the published data for the use of spinal decompression reveals very little risk associated with treatment. One study reported on a patient who developed severe pain while on the unit. A follow-up MRI of the spine revealed that this patients lumbar herniated disc had increased in size. The patient subsequently had lumbar surgery and it was reported that the patient recovered fully. Other studies report some increase in pain for a few participants.
What Spinal Decompression Is
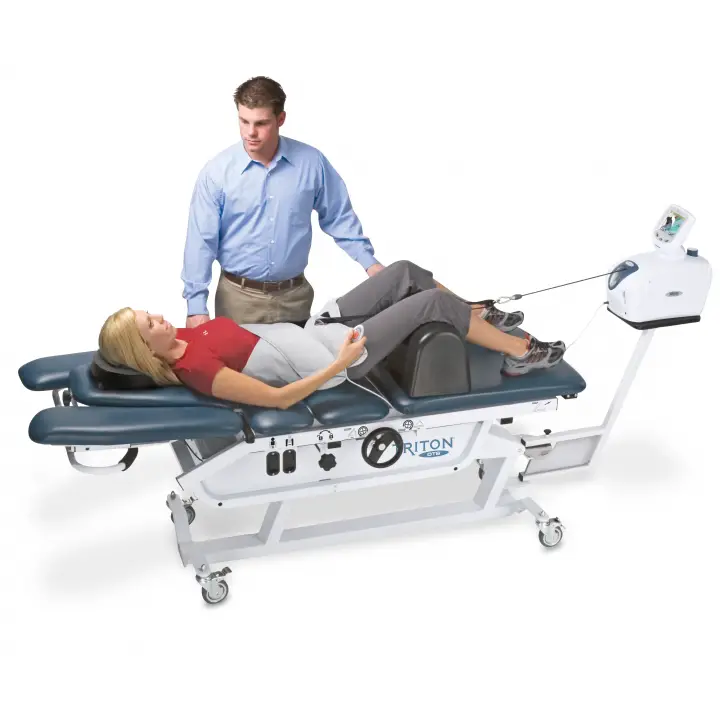
Spinal decompression is a form of mechanical spinal traction, which refers to the separation of the bones, joints, and discs of the back. It is theorized that this separation relieves pressure on the nerves in the back and helps decrease pain, and thus, improve function.
Many spinal decompression systems are operated by the use of a computer, allowing the healthcare provider to adjust the amount of traction force, the angle of traction provided, or the amount of time the traction force is applied. Common trade names of spinal decompression devices are the VAX-D System, the SpinalAid System, and the DRX-9000 System, among others.
Some spinal decompression units require that you lie on your stomach while treatment is rendered others have you lie on your back.
Don’t Miss: Is Tori Removal Covered By Medicare
What Type Of Chiropractic Treatment Does Medicare Cover
Spinal manipulation is the only type of treatment Medicare Part B will cover.2 Also known as an adjustment, spinal manipulation involves a controlled thrust to the spine using hands or a device. The goal is to correct bones in your spine that are out of position, called spinal subluxation. Results may include reduced pain, lower inflammation and restored function.
The Above Policy Is Based On The Following References:
Recommended Reading: Does Medicare Pay For Varicose Veins
Has A Chiropractor Ever Broken A Neck
Here is the short answer. There has been no documented proven case where a chiropractor ever accidentally killed their client by snapping their neck incorrectly? Chiropractic adjustments are statistically safer than any medical treatment, and safer than crossing the street.
What is chiropractic Chiropractic?
Chiropractic Chiropractic is a licensed health care profession that emphasizes the bodys ability to heal itself. Treatment typically involves manual therapy, often including spinal manipulation. Other forms of treatment, such as exercise and nutritional counseling, may be used as well.
Where can I get chiropractic treatment in Jakarta?
Fakultas Kedokteran Gigi Universitas Indonesia, located in Jakarta Pusat, Jakarta, Indonesia offers patients Chiropractic Treatment procedures among its total of 619 available procedures, across 13 different specialties.
What Is Nonsurgical Spinal Decompression
Nonsurgical spinal decompression is a type of motorized traction that may help relieve back pain. Spinal decompression works by gently stretching the spine. That changes the force and position of the spine. This change takes pressure off the spinal disks, which are gel-like cushions between the bones in your spine, by creating negative pressure in the disc. As a result, bulging or herniated disks may retract, taking pressure off nerves and other structures in your spine. This in turn, helps promote movement of water, oxygen, and nutrient-rich fluids into the disks so they can heal.
Doctors have used nonsurgical spinal decompression in an attempt to treat:
- Back or neck pain or sciatica, which is pain, weakness, or tingling that extends down the leg
- Bulging or herniated disks or degenerative disk disease
- Worn spinal joints
- Injured or diseased spinal nerve roots
More research is needed to establish the safety and effectiveness of nonsurgical spinal decompression. To know how effective it really is, researchers need to compare spinal decompression with other alternatives to surgery. These include:
- Nonsteroidal anti-inflammatory drugs
- Acupuncture
Don’t Miss: What Is Basic Medicare Coverage
Healthexporting Pain: Us Medical Devices Cause Serious Injuries Pain Overseas
The FDA has received about two dozen complaints about malfunctions in spinal decompression devices manufactured by various companies, some of which resulted in injuries. In 2010, a patient reported pain with every step after 20 treatments on the DRX9000. The patient described it as a modern version of a medieval torture device.
Many of the FDA complaints are about the Triton DTS machine. One alleged that in 2018, a rope attached to a patients harness pulled so hard that the patient had to be taken to an emergency room. A patient in 2015 described losing feeling in the legs and wrote, It felt like my lower body was separated in two pieces. The patient continued to have complications a year-and-a-half later, according to the complaint. DJO, the manufacturer in Vista, California, did not respond to a request for comment.
The FDA did not immediately respond to a request for documents showing what actions, if any, it took in these cases, but said that in general it requires device manufacturers to investigate adverse events and that the complaints are one tool the agency uses in deciding whether to take further action.
Taken together, the lawsuits and reports do not document widespread injuries from the devices, but they do undermine the claim, made by many practitioners, that spinal decompression is free of risk.
Are There Different Types Of Spinal Decompression Surgery
Your doctor may suggest one or more types of back surgeries to relieve the pressure in your spine. In addition, you may need spinal fusion to stabilize your spine. The following are the more common types of back surgery:
- Diskectomy: In this procedure, a portion of the disk is removed to relieve pressure on nerves.
- Laminotomy or laminectomy: A surgeon removes a small portion of bone — a section of bony arch or the entire bony arch — to increase the size of the spinal canal and relieve pressure.
- Foraminotomy or foraminectomy: A surgeon removes bone and other tissue to expand the openings for nerve roots.
- Osteophyte removal: During the surgery, bony growths are removed.
- Corpectomy: This procedure involves removing a vertebral body along with disks between the vertebrae.
Read Also: When Can A Disabled Patient Enroll In Medicare Part D
Does Medicare Cover Chiropractic Services
En español | Original Medicare pays for only one chiropractic service: manual manipulation of the spine if deemed medically necessary to correct a subluxation .
This procedure, when performed by a chiropractor or other qualified provider, is covered through Medicare Part B, the component of original Medicare that includes outpatient services.
Medicare will pay 80 percent of the Medicare-approved rate for this procedure. You will owe 20 percent of the amount. You must also pay your deductible for Part B before Medicare begins to pay its share.
You pay all the costs for other services provided or tests that a chiropractor orders, including acupuncture, massage therapy or X-rays. Medicare will cover the cost of an X-ray a physician orders to demonstrate that a spinal subluxation requires treatment but will not if a chiropractor ordered the X-ray.
Some Medicare Advantage plans offer routine chiropractic services as an additional benefit. Check with your plan provider about whats available.
Editor’s note: This article was originally published on July 15, 2015. It has been updated with the latest information regarding Medicare coverage in 2020.
What If Youre Out Of Network
In the midst of determining whether your insurance will cover your microvascular decompression procedure, you may find out that your neurosurgeon is considered out of network. This status does not necessarily mean your insurance will not cover your surgery. It simply means you will need to spend time exploring how your specific insurance plan handles out-of-network claims.
A smaller percentage may be covered than with an in-network provider. You may also have a different deductible and out-of-pocket maximum amounts. In addition, your surgeons office may not file insurance claims with an insurance company that considers them to be out of network, meaning youll have to file your own claim.
If your coverage is determined to be out of network, you will need to make a decision: continue working with the neurosurgeon youve already gotten to know and who knows your case, or find a different provider who is considered to be in network. While you may experience cost savings by changing providers, youll also need to start over from scratch with a different neurosurgeon. It can take considerable time to get an appointment with another neurosurgeon, which means your treatment will also be delayed significantly. You need to determine whether youd rather bear extra cost in return for faster relief, or whether you are able to wait and save money.
Read Also: When You Turn 65 Is Medicare Free
Medicare Coverage For Pain Management Injections
Usually, Medicare covers pain management injections when theyre determined to be medically necessary. Suppose youre receiving an injection during an inpatient stay at a hospital. In that case, it will receive coverage from Part A. If your doctor administers the procedure in an outpatient setting, Part B covers the injection.
Healthmost People With Back Pain Get Bad Treatment
One of the claims the regulators targeted was from a 2003 study by Dr. Thomas Gionis who had previously done prison time and had his license put on probation after being convicted of plotting an assault on his estranged wife that found 86 percent of patients treated with an unnamed spinal decompression device experienced an immediate resolution of symptoms.
The Florida attorney general, in its 2009 lawsuit against Axiom Worldwide accusing the company of deceptive and unfair trade practices, pointed out that the Gionis study lacked a control group and combined spinal decompression with other types of treatment. Six years later, without admitting any violations of the law, Axiom agreed to a permanent injunction promising only to make any claims based on competent and reliable scientific evidence and to reimburse the attorney general $19,000 for its costs.
Gionis, who maintained his innocence in the assault on his wife, did not respond to a request for an interview.
Musallam, who worked at Axiom before starting Excite Medical, eventually winning the intellectual property rights to the DRX9000 through protracted litigation, called the Gionis study worthless and said he didnt use it.
We try to stick to hard facts and things that are credible, he said.
Decompression 86% Effective, reads the headline over the Gionis study on the website of Natural Spine Care in Dublin, California, which offers treatment on a different device called ABS.
Recommended Reading: What Is The Monthly Premium For Medicare Part B
Spinal Decompression For Neck Pain
Spinal decompression surgery reduces pressure on the spinal cord or spinal nerve roots.
Surgery is only done to relieve severe symptoms caused by pressure on the nerve roots. This pressure may cause neck pain, but it can also cause arm pain, numbness, or tingling leg pain, numbness, or tingling or problems with bladder or bowel control. In these cases, surgery may not help the neck pain itself, but it usually helps relieve other symptoms.
To relieve the pressure, your doctor may remove:
- Bony growths and fibrous tissue that are narrowing the spinal canal and pressing on spinal nerve roots.
- Parts of the vertebrae to enlarge the spinal canal, to relieve pressure on the spinal nerve roots.
- Disc material from a herniated disc that pushes into the spinal canal.
In some cases, after bone and disc material are removed, the affected bone parts may be joined together to stabilize them.
Current as of: March 9, 2022
Author: Healthwise Staff
Medical Review:William H. Blahd Jr. MD, FACEP – Emergency Medicine& Adam Husney MD – Family Medicine& Kathleen Romito MD – Family Medicine& Robert B. Keller MD – Orthopedics
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.
To learn more about Healthwise, visit Healthwise.org.
Spinal Decompression Therapy Is Covered By Insurance
Is spinal decompression treatment covered by most health insurance carriers, workers compensation benefits and/or personal injury claims? Dr. Larry Van Such, DC, explains:
Spinal decompression therapy is covered by most insurance companies workers compensation and personal injury or auto accident claims.
You may have heard otherwise however spinal decompression therapy is a specialized form of traction and this is why it should be covered on your insurance policy.
Knowing this is why we are able to make it affordable to most people who need these services. Now in the event that you do not have any of these types of coverage, cash payment arrangements can be made through our office.
Again our goal is to make spout decompression therapy affordable to everyone.
Read Also: Will Medicare Cover A Lift Chair
What If Coverage Is Denied
At times, insurance companies may deny your pre-authorization request to cover your microvascular decompression procedure. This denial can happen for several different reasons, including:
- Your insurance policy not covering that specific procedure
- A determination that the procedure is not medically necessary
- A lack of supporting documentation to show why microvascular decompression is the correct procedure for your trigeminal neuralgia
Just because a pre-authorization request is denied doesnt mean you wont eventually get your insurance company to cover your surgery. First, you can appeal the decision. Your insurance company may allow you to begin the appeal process via phone or Internet, or you may need to file specific forms. You can provide additional paperwork that shows the progression of your trigeminal neuralgia, including the fact that medical management has not been successful. You can share imaging results to show your impingement. Your doctor can provide a statement defending microvascular decompression as the best choice to treat your trigeminal neuralgia. Additionally, you can obtain a second opinion to support the need to use microvascular decompression for your specific case.
Medicare Coverage For Conditions Of Lower Back Requiring Pain Management Treatments
Below, well go over some spine-related ailments the details of coverage for each treatment.
Sciatica
Only those feeling pain starting from the sacroiliac joint, or SIJ, have true sciatica. Those suffering from sciatica can obtain coverage for lumbar epidural steroid injections.
Disc Herniation
Sometimes, surgery, known as a discectomy, is performed to fix a herniated disc. But, Medicare doesnt cover discectomies because patients can often get relief for a herniated disc through non-surgical approaches. These avenues for relief include exercise, physical therapy, massage, and pain medication. Epidural steroid injections can also help.
Lumbar Stenosis
Medicare doesnt consider the treatment of percutaneous image-guided lumbar decompression , so there is no coverage.
Facet Joint Arthropathy
If medically necessary, epidural steroid injections for this condition obtain coverage from Medicare. Physical therapy may also help with this condition but might not get coverage unless a doctor refers you.
Lumbar Spondylolisthesis
Medicare doesnt cover lumbar artificial disc replacement surgery. Alternative treatments are pain management medications and physical therapy. The latter have coverage when a doctor refers you to help get back on your feet.
Recommended Reading: How To Apply For Medicare In Alaska
What Does Help Low Back Pain
While many treatments are available for your low back pain, the scientific data indicates that maintaining normal activity is a good treatment for acute low back pain. Exercises for your low back also received a grade of A for sub-acute and chronic low back pain.
The great thing about exercise is that it is a low-cost, easily implemented treatment. Your physical therapist can teach you how to improve your posture and implement the right exercise program for your specific condition to treat your low back pain.
Evaluating Your Insurance Benefits Working With A Benefits Specialist
Benefits specialists work within medical and surgical practices to arrange and coordinate appropriate insurance coverage for patients. These specialists are trained to understand how and what different insurance companies provide coverage for certain procedures and diagnoses. Your first step in asking the question, Does insurance cover microvascular decompression, is to meet with the benefits specialist at your neurosurgeons practice.
The practices benefits specialist can provide you with a lot of different information and support, including:
- What deductible you must meet before coverage kicks in
- Whether your neurosurgeon is considered in-network or out-of-network
- What percentage of the procedures costs will be paid by insurance
- What percentage of the procedures costs you will be responsible for
- What your out-of-pocket maximum is the point where insurance will cover costs at 100 percent for in-network procedures
- What additional pre-qualification steps or documentation you will need to follow or provide
Recommended Reading: Is Fehb Better Than Medicare