Is Radiation Therapy The Same Thing As Chemotherapy
No, while both are used to fight cancer, radiation therapy and chemotherapy are two different treatments. Radiation therapy uses radiation to shrink or kill cancerous cells and tumors. Chemotherapy has the same goal but uses medications and chemicals to do it. Unlike radiation therapy, chemotherapy is often less targeted, causing the medication to spread throughout the body. This can make the side effects more widely felt.
Radiation therapy and chemotherapy are often used together to treat some kinds of cancer.
Does Medicare Cover Breast Cancer
Medicare pays 100% of the cost of an annual breast cancer screening. Part A pays for inpatient breast cancer surgery or breast implant surgery after a mastectomy. Breast surgeries done at a doctors office or outpatient center are covered by Part B.
Part B also covers breast prostheses after a mastectomy.
Defining Medically Necessary Dental Services
The 1997 Balanced Budget Act, which provided for this study, included no definition of medically necessary dental services. One definition of such services is found in a bill submitted earlier in 1997 . It called for coverage of dental services that are medically necessary as a direct result of, or will have a direct impact on, an underlying medical condition if the coverage of such services is cost-effective . It also included explicit provisions for Medicare to cover dental care related to several specific illnesses. The bill’s languageminus the wording about cost-effectivenessis similar to that used three years earlier in a bill that included medically necessary oral health care in a proposed set of basic benefits to be covered as part of broad health care reform . This earlier proposal also included oral care intended to control pain and infection and to restore function. The committee understands these definitions of medically necessary servicesparticularly the one proposed in 1997to be narrowly constructed to continue the general exclusion of Medicare coverage for dental care but to broaden the scope of the exceptions to include dental care needed to prevent or effectively manage systemic conditions including the oral complications of specific illnesses or their medical treatment.
Don’t Miss: Is Medicare Plan F Still Available
Medicare Coverage For Prostate Cancer Testing
For men over age 50 with Medicare, one digital rectal exam and one prostate-specific antigen blood test are covered every 12 months. This coverage starts the day after your 50th birthday.
Medicare coverage for lung cancer testing
Medicare covers lung cancer screening with a low dose CT scan once per year if you have Medicare, are 55-77 years old, have a tobacco smoking history of at least 30 pack years*, and you either continue to smoke or you have quit smoking within the last 15 years.
Does Medicare Pay For Cancer Radiation Treatments
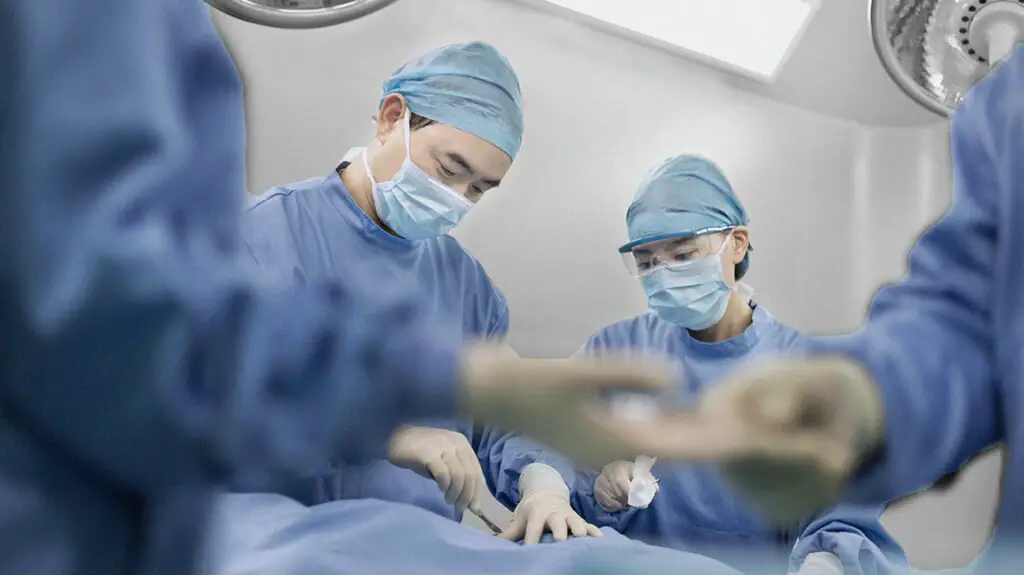
Original Medicare Medicare Part A and Part B covers radiation treatments for cancer that are performed in either a hospital or a freestanding clinic. Medicare Advantage plans are required by law to cover everything that Original Medicare covers, but Medicare Advantage plans may provide additional benefits.
You may still be responsible for out-of-pocket costs associated with your radiation treatment. A Medigap policy may help cover your out-of-pocket costs. Talk with your plans provider to find out exactly what benefits are available to you.
Types of Radiation Therapy Medicare Covers
- Internal Radiation
- Medicare covers this type of treatment in which radiation is delivered in a liquid or solid form, typically through an IV, pills or small pellets that are inserted inside your body.
- External Beam Radiation
- Medicare covers this type of treatment in which a machine directs beams of energy to a specific site on or inside your body in order to target a tumor while limiting exposure to the area around it.
- Proton Beam Therapy
- Medicare generally covers proton beam therapy. This is a more targeted treatment than external beam radiation because the proton beam stops after reaching the cancer. Proton beam therapy is a relatively new form of radiation treatment, and there may be certain requirements for coverage. Before committing to the treatment, make sure you check with Medicare or your Medicare Advantage plan provider to see that its covered in your case.
Don’t Miss: Will Medicare Pay For A Roho Cushion
How Much Does Immunotherapy For Cancer Cost With Medicare
Even if Medicare covers your immunotherapy, there are some out-of-pocket costs you should expect to pay, which may include:
- Medicare Part B deductibleYou must meet your Part B deductible before your Medicare coverage kicks in. In 2019, the Medicare Part B deductible is $185 per year.
- Medicare Part B coinsuranceOnce you meet your Part B deductible, you are typically responsible for paying a coinsurance of 20 percent of the Medicare-approved amount for most doctors services.
There is no annual limit on how much you could pay for the Part B coinsurance in a given year. This means that your Part B coinsurance costs could add up quickly for immunotherapy and other cancer treatments.
Oral Health Problems Associated With Radiation Treatment Of Cancers Of The Head And Neck
Because radiation therapy disrupts cell division in healthy tissue as well as in tumor, it also affects the function and structure of the oral mucosa and underlying organs and tissues such as salivary glands and bone. If directed at the lymph nodes in the jaw area, radiation may impinge in varying degrees on the salivary glands, which are very sensitive to radiation effects. Radiation can irreversibly damage these glands, resulting in insufficient production of saliva, known technically as xerostomia . Saliva is important to keep the oral tissues moist and to buffer the acidity of the oral environment, which is critical both to reducing bacterial growth and infection and to laying down new mineral deposits that keep the teeth strong and dense. After radiation, the teeth tend to become demineralized and to develop cavities easily, a tendency so marked that it has the special name radiation caries.
The likelihood of ORN is increased by trauma to the bone, including the trauma to the jawbone caused by a tooth extraction . The effect of such trauma on the risk of ORN is especially marked when the extraction or other trauma occurs near the time of the radiation . This occurs presumably because the radiation damage to blood vessels makes healing a recent extraction wound more difficult.
Read Also: Does Medicare Pay For Private Duty Nursing
Does Medicare Cover Chemotherapy
Yes, Medicare will cover chemotherapy if you have cancer. Medicare Part A provides coverage if youre a hospital inpatient, and Part B will provide coverage if you receive chemotherapy in a hospital outpatient setting, doctors office or freestanding clinic.
If you receive chemotherapy as an outpatient, the location where you get treatment impacts how much you pay. In a hospital outpatient setting, you will have a copayment. For chemo given in your doctors office or a freestanding clinic, youll pay 20 percent of the Medicare-approved amount and will also be responsible for the Part B deductible.
Medicare Part D plans may also cover some chemotherapy treatments and related prescription drugs. Part D plans may cover the following cancer drugs: anti-nausea drugs, oral prescription drugs for chemotherapy, pain medication or other drugs used as part of your cancer treatment.
Effectiveness Of Dental Care In Improving Health Outcomes For Head And Neck Cancer Patients Treated With Radiation
No randomized controlled trials have compared the effectiveness of tooth-preserving protocols and protocols that emphasize tooth extraction without preventive care for head and neck cancer patients undergoing radiation therapy. One of the earliest retrospective studies comparing tooth-preserving and aggressive tooth extraction protocols was carried out at Walter Reed Army Medical Center . It showed that patients in the tooth-preserving protocol lost fewer teeth than their predecessors treated under an aggressive tooth extraction protocol. Patients in the tooth-preserving protocol also required fewer dental visits both before and after radiation therapy . ORN rates were historically low before and after the change in protocol, so the study did not demonstrate an effect on ORN.
Studies to identify causes of ORN have repeatedly identified extractions and lack of preventive dental care as major contributing factors . As tooth-preserving treatments have become more common and the rate of ORN has dropped, unknown causes of ORN are proportionately more likely to be identified as causes than are extractions.
Also Check: Does Medicare Cover Assisted Living In Illinois
Your Costs For Radiation Treatments On Medicare
While Medicare covers most of the cost of radiation treatment, you will still be responsible for a portion of the cost. Your responsibility will vary depending on the Medicare coverage you have. Each part of Medicare covers different costs associated with your cancer treatment.
Your Share of Radiation Therapy Costs Under Each Part of MedicareDon’t Leave Your Health to Chance
For Breast Cancer Medicare Covers Two Different Mammograms
- A screening mammogram once every 12 months at no cost if your doctor accepts Medicare assignment for women with Medicare age 40 or older.
- A diagnostic mammogram if medically necessary. Frequency will vary based on your individual situation. Medicare will cover 80 percent of the cost of this type of mammogram, while you will be responsible for the other 20 percent and the Part B deductible.
You May Like: Does Medicare Cover You When Traveling Abroad
Committee Findings And Conclusions
The committee utilized the extensive review of literature provided by the panel of background paper authors, four experts in dental research. The committee also benefited from a two-day public workshop featuring many guest speakers and attended by members of the public with expertise in dental research and hospital-based dental practice . Unfortunately, little systematic research is available to assess the prevention and management of the oral-medical problems examined in this chapter. Standards of practice for these problems have been developed, often on the basis of plausible biological reasoning but without much evidence from well-controlled clinical trials. The committee’s findings, as discussed in this chapter, are summarized briefly below. Its conclusions about Medicare coverage follow.
Cancer Services Covered By Medicare Part B

Medicare Part B covers a variety of medically-necessary cancer treatments received as an outpatient. It also provides a number of cancer screenings, such as yearly mammograms and prostate exams.
Cancer services covered by Medicare Part B include:
- Doctor visits, including specialist care from an oncologist
- Chemotherapy drugs administered intravenously, as well as some oral chemotherapy medications
- Radiation therapy received as an outpatient
- Diagnostic screenings, including x-rays and CT scans
- Durable medical equipment, including wheelchairs, oxygen tanks, and walkers
- Outpatient surgical procedures
Read Also: Does Medicare Cover Varicose Vein Treatment
Does Medicare Cover Cancer Treatment
In 2018, over 1.7 million new cases of cancer will be diagnosed in the United States, according to the National Institutes of Health . The good news is that cancer mortality is much lower than cancer incidence . Cancer incidence is 439.2 per 100,000 while cancer deaths are only 163.5 per 100,000 . Some lives are saved through cancer treatment.
What Are The Costs Associated With Radiation Therapy
Radiation therapy treatment at public or partnership radiation therapy centres is generally provided without a cost to the patient.
Radiation therapy at a private centre may incur out of pocket costs, also known as a gap or gap payment. This is the difference between the cost of treatment and Medicare rebate. You are required to pay the full cost yourself before you can claim a rebate from Medicare.
Any direct costs charged by a radiation therapy centre, Medicare rebates applicable to you and any out of pocket costs that you will need to pay must be made clear to you before treatment begins.
You will also need to confirm with the radiation therapy centre what other costs you are likely to need to pay as part of your overall treatment and recovery. Allied health care providers may be free of charge in the public system or may incur a cost if they are private providers. Your doctor or the radiation therapy centre may be able to advise you about your eligibility for government assistance for travel and accommodation.
You have the right to choose the radiation therapy centre who will provide your treatment based on your needs and considering all the costs involved. Many radiation therapy centres have accounts staff to talk you through these considerations.
Also Check: Does Medicare Have A Limit
How Is Prostate Cancer Treated
There are several options your doctor might consider to treat prostate cancer. Their methods typically depend on how advanced your cancer is, as well as the Surveillance, Epidemiology and End Results stage, which determines whether your cancer is localized to one area or has begun to spread throughout the body.
Typical treatments for prostate cancer include:
- Active surveillance
Like Most Health Insurance Medicare Covers A Variety Of Cancer Treatments Including Radiation Therapy
Medicare covers radiation therapy as well as a variety of cancer treatments and screenings. Most of these services are included with your Medicare Part B benefits. However, some cancer treatments, such as surgery to remove a tumor, are covered by Medicare Part A.
As with most Medicare coverage, the first question is whether a treatment is deemed medically necessary by your healthcare provider. Then, determining which “part” of Medicare applies usually depends on whether the service is inpatient or outpatient.
Read Also: Does Medicare Pay For Maintenance Chiropractic Care
What Is The Medicare Safety Net
The Medicare Safety Net is a Federal Government health program that provides a higher Medicare benefit for eligible services, including radiation therapy, when a health consumer reaches a threshold of out of pocket costs . This threshold depends on personal circumstances, for example, if the health consumer holds a concession card.
You need to meet certain criteria to be eligible for the Medicare Safety Net.
The Medicare Safety Net thresholds and any reimbursements are reviewed annually on 1 January and calculated for the calendar year. Single individuals are automatically registered but families need to formally register with the program.
The Medicare Safety Net provides an extra benefit to health consumers with high out of pocket medical treatment costs. It reduces the amount of out of pocket costs for radiation therapy.
The Medicare Safety Net does not reduce the direct cost of radiation therapy treatment. It results in a higher Medicare rebate, reducing the out of pocket cost to you.
The standard Medicare rebate and the additional Medicare Safety Net rebate are automatically calculated and paid into your bank account once a fully paid claim is lodged with Medicare.
For more information about the Medicare Safety Net visit
Some Regions Pay For Prostate Treatment Others Don’t
The medical tool’s catchy name, CyberKnife, evokes digital accuracy. But the way the federal Medicare system treats CyberKnife seems anything but precise.
CyberKnife is a new but fast-growing radiation treatment for prostate cancer, spurred by radio and newspaper ads that stress its convenience and results. Its top selling point is that CyberKnife treatments take five days instead of the eight weeks for conventional prostate cancer radiation, although many experts say they believe that the medical evidence is inconclusive on whether it works as well as those older methods.
But geography may play as big a role as medicine in determining which men diagnosed with prostate cancer are eligible for CyberKnife. As it turns out, Medicare pays for the treatments in 33 states – but not in 17 others.
States that do not provide coverage include big ones like California and Texas, but also less populous places like Alaska and South Dakota. Medicare will pay for a man’s CyberKnife treatments in New Hampshire, but not across the border in Vermont.
Many health policy experts applaud refusing reimbursement for treatments not supported by medical evidence. But some also point to CyberKnife as emblematic of the inconsistent way that the federal Medicare budget – expected to be $477 billion in the current fiscal year – is spent, region to region.
“You can live on one side of the street and get a procedure, but on the other side of the street you can’t,” Pearson said.
Also Check: What Medicare Plans Do I Need
What To Expect With Radiation Treatments
If you and your doctor have decided that radiation therapy is right for your type of cancer, youll begin with a radiation simulation. During the simulation, youll lie on a table and a CT scan or X-ray will be done to see where your cancer is and where the energy beams should focus.
After the images are taken, your treatment team will mark the area where radiation is needed. This will help the team direct the radiation precisely to the right place.
During radiation therapy, youll likely have treatments 5 days per week for up to 10 weeks. How much radiation you receive and for how long will depend on the extent and type of your cancer.
Depending on the kind of treatment you get, you may experience
Effectiveness Of Dental Care In Improving Health Outcomes For Leukemia And Lymphoma Patients
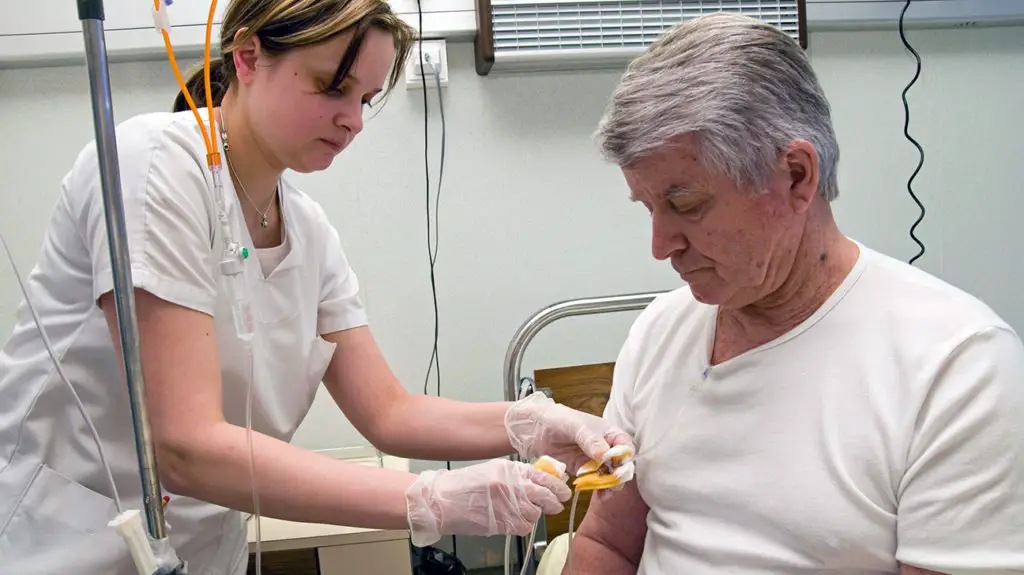
No large, multicenter, randomized clinical trials have assessed the effectiveness of dental interventions to prevent or manage oral or systemic complications of chemotherapy for leukemia or lymphoma patients. A few controlled studies suggest that dental care for leukemia patients prior to chemotherapy may prevent or reduce subsequent episodes of septicemia and prevent or reduce the severity of common oral complications of chemotherapy that are associated with the prior burden of oral disease . Unfortunately, these studies involve few elderly patients.
A recent study with no control group that tested the effect of not treating chronic dental disease prior to chemotherapy concluded that treatment for chronic problems could be safely postponed with little effect on the subsequent risk of acute dental disease . It also concluded that a prechemotherapy oral examination was still needed to identify acute dental disease for treatment to prevent local exacerbations or systemic spread of infection
These few studies of prechemotherapy dental treatment have involved mostly or entirely leukemia patients, who tend to receive aggressive, combination chemotherapy that is associated with more severe immunosuppression. Additional studies would be needed to determine the effects of prechemotherapy dental treatment on lymphoma patients.
Recommended Reading: How To Qualify For Extra Help With Medicare Part D
