Deep Sleep Diabetes Remedy
When Scott Hansen was confronted with the raw possibility of shedding his better half to Type 2 Diabetes, he was desperate to discover a solution for her. He stumbled on a feasible service when he met an old pal Tom, that had actually relatively reversed his Type 2 Diabetes, shed 40lbs as well as currently appeared like he was 10 years more youthful, and much healthier. what brand of diabetic supplies are covered by medicare
Tom pointed Scott in the direction of a regional doctor he had satisfied in Thailand. It was also this doctor that patiently clarified to Scott about the genuine source of type 2 diabetic issues and just how to address it utilizing a special tea formula.
After confirming the details versus readily available study, Scott promptly came down to offering his other half this precise tea formula. To his delight, he saw her condition improve. It was additionally after that, that they concurred even more individuals required this service. They worked with a medical research study and nutrition specialist as well as fine-tuned the option right into a program: The Deep Sleep Diabetes Remedy. what brand of diabetic supplies are covered by medicare
This value-packed program includes the following as well as much more:
Medicare Eligibility For A Therapeutic Cgm
A therapeutic CGM is a medical device approved by the U.S. Food and Drug Administration as a replacement for home blood sugar monitors. It provides you and your doctor with the medically necessary information to make diabetes treatment decisions, such as changes in diet and your insulin dosage.
To qualify for a therapeutic CGM, you must be undergoing treatment for diabetes and meet certain other criteria.
To be eligible for a therapeutic CGM under Medicare, you must meet the following requirements.
- You are using insulin to treat Type 1 or Type 2 diabetes.
- You need to check your blood sugar four or more times per day.
- You must use an insulin pump or receive three or more insulin injections per day.
- You must make routine, in-person visits to your doctor.
- Your doctor has determined that you meet all Medicare eligibility requirements.
The decision between a therapeutic CGM or a traditional monitor is one you should make after talking to your doctor. A therapeutic CGM may be a better option if you use insulin and frequently change your dosage.
The Best Diabetic Supply Companies Of 2022
- Best for Medicare and Medicaid Insurance: Edgepark
- Best Support for Medtronic Users: Medtronic
- Best for Specialized Insulin Pump & Technology: Tandem
- Best for Pediatric Population: Insulet
- Best for Replacements: Dexcom
-
Will review all your insurance options to help save money
-
May not be available to all types of Medicare plans
-
Pump users may be locked into warranties
Why we chose it: Many health professionals and people living with diabetes recommended Byram Healthcare to us for diabetes supplies. Its deliveries are very reliable and because it offers so many products, it may serve as a one-stop-shop for diabetes supplies. Priding itself on convenience, affordability, and choice, Byram Healthcare offers a comprehensive product line of diabetes supplies ranging from diabetes test strips, lancing devices, lancets, control solution, batteries, blood glucose meters, insulin pump supplies, continuous glucose monitor supplies, insulin and pen needles, and more.
Don’t Miss: Which Medicare Part Covers Prescriptions
Medicare And Diabetes Coverage
Home / FAQs / Medicare Coverage / Medicare and Diabetes Coverage
Medicare and diabetes coverage is a concern for many Americans. Diabetes can cause a persons health and well-being to deteriorate over time. Close monitoring is often necessary because diabetes causes other health concerns and conditions. Below we go into full detail about what you need to know regarding Medicare and diabetes coverage.
Who Is It For
If you are prediabetic or experience Type 2 Diabetes, as well as you notice that you do not obtain enough high quality sleep during the night, Deep Sleep Diabetes Remedy program is most likely the program for you. Kill 2 birds with one rock: improve your sleep and also energy levels and also reverse your diabetic issues with this program. what brand of diabetic supplies are covered by medicare
One More Thing I Found An Awesome Free Bonus For You!
Ive obtained terrific news! I located a site offering a pretty considerable bonus on the Deep Sleep Diabetes Remedy. You can save a minimum of $47 on these bonus offers but you need to act now. To get the rewards for free, please click on the link below. Rush, since the reward is just offered for a restricted time. what brand of diabetic supplies are covered by medicare
Read Also: Is Medical Part Of Medicare
How Much Do Testing Supplies Cost
If youve met your Part B deductible , you will pay 20 percent of the Medicare-approved amount for diabetic testing supplies. Medicare pays the other 80 percent.
Depending on the type of equipment or supplies you need, you may need to:
- rent the equipment.
- buy the equipment.
- choose whether to rent or buy the equipment.
Additionally, your durable medical equipment will only be covered if your doctors and DME suppliers are enrolled in Medicare. You must also purchase your testing supplies from a supplier who accepts assignment. In this case, they can only charge you the coinsurance and Part B deductible.
Accepting assignment means the supplier agrees to be paid directly by Medicare and accepts the payment amount Medicare approves for the service. The Medicare-approved amount is the amount a supplier can be paid by Medicare, and you pay the rest.
To ensure your supplier is enrolled in Medicare, ask if they participate in Medicare before you order the supplies.
How much you will specifically pay for supplies depends on a variety of factors such as:
- Other insurance you may have.
- How much your doctor charges.
- Where you get your supplies.
- Whether your doctor and supplier accept assignment.
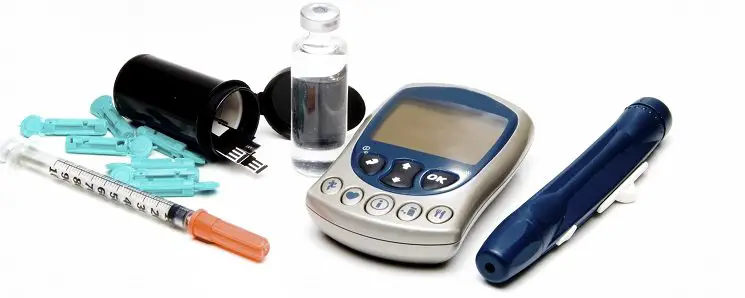
Medicare Part B Covered Diabetes Testing Supplies
Part B covers a number of blood sugar self-testing supplies and equipment, even if you dont use insulin. These include:
- Blood sugar monitors
- Lancet devices and lancets
- Glucose control solutions
These supplies are considered durable medical equipment, and the actual amount of supplies that are covered varies depending on whether or not you use insulin. For example, if you use insulin, you may be able to get up to 300 test strips and 300 lancets every three months, but if you dont use insulin you may only be able to get up to 100.
If your doctor says its medically necessary, Medicare will cover additional test strips and lancets.
Test strips can be used to help monitor certain substances in the blood. They are small, single-use pieces of paper-like substance that you place one or two drops of blood on, and insert into a testing device. These devices provide results within seconds, and you can address any concerns regarding blood glucose levels.
Don’t Miss: Does Medicare Come Out Of Your Paycheck
How Do I Get My Medicare Diabetes Supplies
You can order and pick up supplies from your pharmacy, or you can order them from a DME supplier.
If you order from a supplier, you must place the order yourself, meaning a doctor cannot call it in for you. However, you will still need a prescription from your doctor to place the order.
When you go to the pharmacy or supplier, show your red, white and blue Medicare card and your prescription.
You can also order supplies through the Medicare National Mail-Order Program, including test strips, lancets and lancet devices. If you want your supplies mailed to your home, you must use a Medicare national mail-order contract supplier. You can visit www.Medicare.gov or call Medicare for a list of contracted suppliers.
You need a new prescription from your doctor for lancets and test strips every 12 months, so dont forget to ask for refills for your supplies every year.
Best For Specialized Insulin Pump & Technology: Tandem
Tandem
-
Advanced technology to help maintain glucose control
-
Only available for people 6 years and older
Tandem Diabetes Care is the maker of the t:slim X2 insulin pump, which is approved for people with diabetes 6 years of age and older. Many people with diabetes prefer Tandem for maintaining tight blood sugar control due to its advanced technology. This insulin pump can be used with Basal-IQ and Control-IQ technology systems, which when paired with a compatible continuous glucose monitor can automatically suspend, increase, and decrease insulin delivery based on glucose monitor readings and predicted glucose values.
The technology is meant to help assist you with preventing glucose excursions . It is not meant to replace diabetes self-management such as blood sugar testing, paying attention to symptoms of low blood sugar, and carbohydrate counting. However, it is an added tool that can provide assistance to your daily diabetes routine. If you are using this insulin pump to manage your diabetes, you may choose to have your supplies delivered directly from the company.
Discuss with your physician if this is the right pump for you or your loved one. You may choose to request a pump online and have Tandem check your insurance for you. This process can be started online or you can reach out via phone, fax, or email.
Also Check: How Do I Find Out My Medicare Number
What’s The Best Way To Buy Diabetic Supplies
Who is this for?
If you have diabetes, this page will explain how to buy supplies through your Medicare plan.
When youre managing diabetes, medical supplies like insulin and blood glucose test strips can be a big part of your life. But they dont have to be a big expense.
Our Medicare Advantage plans cover diabetes monitoring supplies with no copay. Diabetes monitoring supplies include things like blood glucose monitors, blood glucose test strips, lancet devices, and insulin pumps.
Our plans also cover therapeutic shoes and inserts with no copay.
About Insulin And Medicare Part D
Medicare Part B does not cover insulin unless you use an insulin pump that is considered medically necessary. It also does not cover insulin pens, syringes, needles, alcohol swabs, or gauze.
In the case of an insulin pump, the insulin and the pump may be covered under durable medical equipment in Medicare Part B and for which youd pay the 20 percent coinsurance. However, you will want to make sure your doctor and contract supplier are all enrolled in Medicare.
Medicare Part D may cover insulin and some medical supplies that are used to inject insulin like syringes, and perhaps even gauze, and alcohol swabs. Medicare Part D does not cover insulin for use in an insulin pump .
For those with Medicare Part D who need insulin and dont use a pump, you will have meet your deductible and then pay the copay.
To find out how much your insulin, insulin pens, or syringes cost, talk to your doctor or health care provider. What you will pay depends on various factors:
- Other insurance you may have
- How much your doctor charges
- Whether your doctor accepts Medicare assignment
- The type of facility
- The location where you get your test, item, or service
Each Medicare Prescription Drug plan has a covered list of drugs called a formulary which varies between plans and can change at any time. You will be notified of any changes to the list of covered drugs.
Once you pay $4,950 out-of-pocket, then you fall under catastrophic coverage which means you pay smaller copays for the rest of the year.
You May Like: How Do I Contact Medicare Part B
Other Useful Information On Diabetic Supplies
- Generally, you pay 20% of Medicare-approved amounts for your supplies, and the Medicare Part B deductible applies.
- Make sure you refill your supplies in a timely manner, and only accept supplies you have requested. Medicare wont pay for supplies you didnt order for example, if a supplier automatically sends you items, you cannot get reimbursed by Medicare.
- You may rent or purchase certain diabetic supplies. For more information, call 1-800-MEDICARE . TTY users call 1-877-486-2048. Customer service representatives are available 24 hours a day, seven days a week.
- Ask if the supplier is a participating supplier in the Medicare program before you get durable medical equipment for diabetes. If the supplier is a participating supplier, he or she must accept assignment. If the supplier is enrolled in Medicare but isnt participating, he or she has the option to accept assignment or not. If a DME supplier doesnt accept Medicare assignment, there is no limit to what you can be charged. You also may have to pay the entire bill at the time you get the DME.
- All Medicare-enrolled pharmacies and suppliers must submit claims for diabetic testing supplies. You cant send in the claim yourself.
Find Plans in your area instantly!
Medicare Reimbursement For Diabetes Self
Medicare beneficiaries may get reimbursement for Diabetes Self-Management Training under certain circumstances. Part B DSMT benefit reimbursement rules are also known as the benefits coverage guidelines. The rules are exact and have adjusted and improved many times over the years. In the future, these rules may or may not change.
Also Check: What Do You Need To Sign Up For Medicare
What Was Our Selection Criteria For The 3 Best Diabetes Programs
When It Comes To Diabetes What Does Medicare Cover
There are many programs within Medicare that can help offset the costs of diabetes treatment.
Original Medicare
The Centers for Medicare & Medicaid Services reports that Medicare Part B will generally cover equipment and supplies like home blood sugar monitors and tools for measuring blood sugar, including:
- Lancets
- Test strips
- Glucose control solutions
Medicare Part B will also cover external insulin pumps and the insulin required for the pump, if you meet certain conditions.
The U.S. Department of Health and Human Services reports that those using Original Medicare can also have diabetes supplies delivered through the National Mail-Order Program. With this program, youâll select a national mail-order contract supplier for Medicare in your zip code using the official U.S. government website for Medicare. This supplier will help you get quality supplies at a discount.
Additionally, if you have diabetes and severe diabetic foot disease, Medicare Part B includes some specialized shoe coverage. One pair of custom shoes plus their inserts and one pair of extra-depth shoes are covered once a year under Medicare Part B, according to the official U.S. government website for Medicare.
Medicare Part D
Medicare Part D helps cover the cost of prescription drugs through private insurance companies. The Centers for Medicare & Medicaid Services notes that Medicare Part D covers the following:
Part D also covers diabetic supplies like:
- Syringes
- Gauze
- Insulin inhalers
You May Like: Does Medicare Pay For Stem Cell Knee Replacement
D Senior Savings Model
Coinsurance also applies every time you fill your prescriptions for insulin or other medications. Copayments depend on your Part D plan and what medications are covered by your plan formulary.
If youre over 65, you can get additional savings by enrolling in the Part D Senior Savings Model. This plan puts a cap on out-of-pocket spending for insulin. You can choose between several covered types of insulin, and your co-payment is capped at $35 for a 1-month supply.
What extra benefits and savings do you qualify for?
Medicare And Continuous Glucose Monitors
Dexcom G5 Mobile
As of January 12, 2017, people covered by Medicare with type 1 or 2 diabetes who intensively manage their insulin will qualify for coverage for a continuous glucose monitor .
Firstly, the CGM must be defined as a therapeutic CGM, which means you can make treatment decisions based on the device. As of today, only the Dexcom G5 Mobile system is approved by the FDA for meeting this criteria.
According to CMS, therapeutic CGM may be covered by Medicare when all of the following criteria are met:
- The beneficiary has diabetes mellitus and,
- The beneficiary has been using a home blood glucose monitor and performing frequent BGM testing and,
- The beneficiary is insulin-treated with multiple daily injections of insulin or a continuous subcutaneous insulin infusion pump and,
- The patients insulin treatment regimen requires frequent adjustment by the beneficiary on the basis of therapeutic CGM testing results.
Read Also: Does Medicare Pay For Entyvio
Diabetic Supplies: Therapeutic Shoes And Inserts
Medicare Part B coverage includes therapeutic shoes or inserts for diabetics who have certain conditions ask the doctor who treats your diabetes if you need them. To make sure these supplies are covered by Medicare, please note:
- A qualified doctor must prescribe the shoes or inserts.
- A qualified doctor must provide and fit you for the shoes or inserts.
- Medicare Part B covers one pair of custom-molded shoes or one pair of depth-inlay shoes per calendar year.
- Medicare also covers two additional pairs of inserts each calendar year for custom-molded shoes and three pairs of inserts each calendar year for depth-inlay shoes.
- In certain cases, shoe modifications may be substituted for inserts.
- The supplier must have an order on file signed and dated by the treating doctor if you switch to a different supplier, you may need to have your prescription transferred or get a new prescription from your doctor. Make sure your supplier is enrolled in Medicare.
Does Medicare Cover Diabetes
In addition to the diabetes services and supplies covered by Medicare Part B , others are covered by Part D .
Typically, Medicare Part B covers the services that may be needed by people who have diabetes, as well as preventive services for people who may be at risk or are pre-diabetic, including:
- Diabetes screenings
- Medical Nutrition Therapy services
- Foot exams and treatment
- Welcome to Medicare preventive visit
- Annual wellness visit
- Insulin pumps
- Therapeutic shoes or inserts
Medicare Part D covers a number of medical supplies you may need to help treat or control your diabetes. Coinsurance or copayments may apply to these supplies, as well as a Part D deductible. Covered supplies may include:
- Insulin
- Diabetes supplies such as syringes, needles, alcohol swabs, gauze, and inhaled insulin devices
Recommended Reading: Is It Mandatory To Have Medicare Part D
