Funding For Services Not Included In Medicare Coverage For Home Health Care
Other sources of funding and service options are available to address what Medicare coverage for home health care does not pay. Your loved one may not qualify for all of these programs, but you may find your out-of-pocket burden eased by utilizing one or more of them.
Medicaid. Each state has its own Medicaid program so coverage and eligibility will vary. Unlike the Medicare program, Medicaid does fund custodial in-home care which includes many of the above services. Their community-based programs often include home-delivered meals and transportation services.
Veteran Benefits. There are a variety of home health benefits available to veterans, each with their own qualification requirements. They include:
- Homebound Program
- Homemaker and Home Health Aide Program
- Skilled Home Care Services
- TeleHealth Care
- Home Based Primary Care
To apply for any of these Veterans benefits, contact your VA social worker/case manager and complete the Application for Extended Care Benefits . You can also call the VA toll-free at 877-222-VETS .
Program of All-inclusive Care for the Elderly . This is a joint Medicare/Medicaid program with the goal of keeping seniors in their homes and communities. To qualify for PACE you must:
- Live in the service area of a PACE organization
- Need a nursing home-level of care
- Be able to live safely in the community with help from PACE
Specific Conditions For A Temporary Ostomy
Persons with a temporary ostomy have been eligible for the annual lump-sum payment only since October 1, 2018. You may qualify if you register and provide the required documents. As of April 1, 2019, this amount has been paid out in 2 instalments, indexed annually:
- As soon as the application is admissible
- 6 months after the surgery
What Should I Do If Medicare Denies My Ostomy Supply Claim
The first thing you should do is file an appeal. Review your denial letter from Medicare. Take your following Medicare claim to a healthcare professional whos familiar with ostomy supplies and Medicare ostomy claims.
To learn more about denied Medicare claims, contact Medicare toll-free at 1-800-633-4227.
Also Check: What Is Medicare Advantage Otc Card
Using Medicare To Pay For Your Ostomy Supplies
Whether youve had a colostomy, ileostomy, or urostomy, you need to get your ostomy supplies from a reliable supply provider. Additionally, you probably want ostomy products from high-quality brands that will be both comfortable and reliable. Lastly, if you have Medicare, you probably want to find cost-effective ostomy supplies covered by Medicare.
Emergency Ostomy Supply Options Near Me

If you run out of ostomy supplies, dont panic. Dial 211 on your telephone to connect with your states community support assistance and explain your ostomy concerns. UOAA, or United Ostomy Association of America has affiliated groups like Kinders Closet who can assist with short-term ostomy provisions.
To get more of your Medicare questions answered, subscribe to our free monthly newsletter
Medicare Benefits Solutions is a non-government website. This is a solicitation for insurance. By submitting information on this site, I am providing my written consent for Medicare Benefits Solutions, herein after referred to as Medicare Benefits, which is a brand operated by HealthCompare Insurance Services Inc., its sales agents, or affiliates to contact me at the phone number or email address listed to provide me with quotes or information about Medicare Advantage, Medicare Supplement, and Medicare Part D plans. I further consent to such calls or texts sent via autodialer, automated technology, prerecorded message and/or artificial voice. I understand my consent is not a condition of purchase and that I can revoke my consent at any time via medicarebenefits.com/about-us/contact-us. Additional charges may apply to SMS, call, or Internet usage depending on your data providers.
You May Like: Does Medicare Pay For Tdap Shot
Understanding Medicares Coverage Of Ostomy Supplies
Medicare covers ostomy supplies if you have a surgically created opening, or stoma, to divert urine or stool to outside your body.
These medically necessary supplies are covered by Medicare if youve undergone certain surgeries, including a colostomy, ileostomy or urinary ostomy.
You must have a prescription, signed and dated by your doctor, on file with the supplier who provides your ostomy materials.
You can order ostomy supplies from large mail-order distributors and local durable medical equipment suppliers.
You generally cant get ostomy supplies from a local drugstore or retail pharmacy.
Are Ostomy Bags Covered By Insurance
There is no one-size-fits-all answer to this question, as insurance coverage for ostomy bags varies from policy to policy. However, in general, most insurance companies will cover at least a portion of the cost of an ostomy bag, with the patient typically responsible for a copay or coinsurance. Some insurance plans may also require preauthorization for ostomy bag coverage.
Recommended Reading: Are You Required To Get Medicare At 65
What You Need To Know
- The procedure creates an opening in the abdomen called a stoma.
- People with stomas need special equipment to collect bodily waste.
- Getting Medicare to pay for ostomy products is increasingly difficult.
Its estimated that anywhere between 750,000 to 1 million people have ostomies in the United States, a surgical procedure used to treat diseases of the digestive or urinary systems that creates an opening on the abdomen called a stoma.
The stoma connects from one organ to the outside of the body and can either be permanent or temporary depending on a patients condition. These individuals rely on durable medical equipment to collect bodily waste from all ostomy procedures, making access to ostomy supplies extremely important.
Yet, its increasingly difficult for patients to get the supplies they need because the margins on ostomy products are low and are extremely complicated. Most providers will not accept assignments, which would mean the patient would have to pay upfront and bill Medicare themselves or shop around where their provider choices are extremely limited.
In the event they can get a provider with a product, most likely they will be unable to give the patient the exact product they need due to low margins. Instead providers will push them to a different product that does not meet their highly individualized need, which may cause complications.
You May Like: What Is Medicare Payer Id Number
What If Medicare Denies My Ostomy Supply Claim
Getting the medically necessary ostomy products you need can be tricky unless you follow certain Medicare rules and procedures.
When you are being discharged from the hospital to your home following ostomy surgery, your doctor should send the prescription for your supplies to a supply distributor approved by Medicare.
This prescription will include your list of ostomy supplies, amount and manufacturer reference numbers.
Similarly, if you are discharged home with home care, the home health care agency should be provided with this information from your doctor.
Keep in mind that home care agencies reimbursed by Medicare often have ostomy supply costs bundled into the payment for home care.
How to Prevent Medicare Denials of Ostomy Supplies
If Medicare denies your claim for ostomy supplies, you can file an appeal.
It may be helpful to review the denial with a health care professional whos familiar with ostomies prior to filing an appeal. He or she might be able to identify the problem and provide a solution.
You can also call Medicare at 1-800-633-4227 for more information about why your claim was denied, and if needed, assistance with filing an appeal.
Don’t Miss: How Can I Get A Medicare Card
Living With A Colostomy Bag
After a patient is fitted with a colostomy bag, doctors, nurses stoma care experts or colostomy specialists will thoroughly explain how to maintain the stoma and what lifestyle changes may be necessary for adapting to using the pouch. Below is some general information and advice that should be noted by all colostomy bag users.
Dont Miss: How Do I Apply For Medicare At Age 65
Average Monthly Cost Of Ostomy Supplies
The average monthly cost of ostomy supplies will vary depending on the type of supplies needed and the quantity required. However, a general estimate for the average monthly cost of ostomy supplies is between $100 and $200.
My friend asked for my advice on where to buy ostomy supplies, specifically the Cymed brand. Several pages on Reddit discuss prices for a specific brand, but none of them discuss prices for that brand. If you buy something on the internet with cash, you might save money. This Canadian website, Canmeddirect.ca, certainly has that product, in my opinion. The Canadian International Pharmacy Association also verifies sites heres a list of verified sites and a search tool. Furthermore, they have stated that they are unable to ship to the United States. If you live in Canada, you can ship there and have someone pick up the package.
Also Check: Does Medicare Cover Dementia Care Facilities
How To Change A Colostomy Bag
The pouch can be changed as often as needed usually, shortly after a bowel movement.At first, the procedure may prove difficult but will get easier with practice. For basic guidelines, follow these six steps:
Dont Miss: What Are All The Medicare Parts
What Is The Medicare Limit On Ostomy Supplies
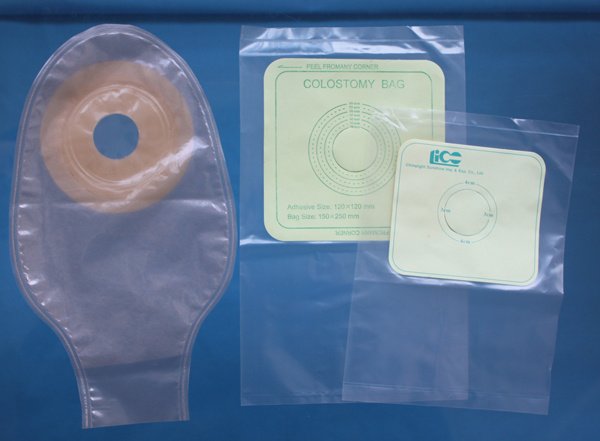
Medicare will cover up to a three-month supply of ostomy products at one time. You must have a prescription from your doctor to receive coverage under Medicare. The supplier must also be accredited and contracted with Medicare.
| Ostomy Supplies Covered by Medicare | Amount Allowed Per Month |
| Skin barrier wipes or swab, each | 150 each / 6 months |
Don’t Miss: What Does Medicare A And B Not Cover
Are Colostomy Bags Dme
Picture source: clinimed
A colostomy bag is a medical device that is used to collect human waste from a person with an ostomy. The waste is collected in the bag, which is then disposed of properly. There are many different types of colostomy bags available on the market, but they are all considered to be Durable Medical Equipment .
How Many Ostomy Supplies Does Medicare Cover Per Month
Picture source: 180medical
There is no set answer to this question as Medicare coverage for ostomy supplies can vary depending on the individuals needs. Some people may only need a few supplies per month while others may need many more. Ultimately, it is up to the Medicare-approved supplier to determine how many supplies are needed and how often they need to be replaced.
As long as your doctor writes a prescription for these items, Medicare covers them, and you get them from a medical supplier that accepts Medicare. You will be responsible for 20% of the cost of the ostomy supplies you order. All of our fact-checkers begin by vetting all relevant and authoritative sources. If you have a surgically designed opening known as an ostomy, or stoma, to divert urine or stool, you may be able to receive Medicare coverage for these supplies. A doctors prescription, signed and dated by the doctor, must be on file with the supplier who provides ostomy materials. There are numerous types of Medicare ostomy supplies that can be purchased. In 2019, the improper payment rate for ostomy supplies was 29.4%, amounting to approximately $64.5 million in lost revenue. The prescription for your supplies must be sent to a supply distributor approved by Medicare. If Medicare fails to pay your claim, you have the right to file an appeal.
Also Check: What Is Centers For Medicare And Medicaid Services
How Many Ostomy Bags Does Medicare Pay For A Month
It is important to understand that Medicare will only pay for prescribed ostomy supplies for three months at a time. Because ostomy supplies can cost between $300-$600 a month, it is wise to work closely with your physician to maintain refillable, on-time prescriptions.
Discuss suppliers with your physician, too, for a broader range of available supplies in case of shortages or other delivery concerns. Each supplier must have a signed and dated prescription by your physician. Otherwise, Medicare will not approve coverage.
Information Necessary On The Medical Prescription
The medical prescription must contain the following clearly legible information:
- Your first and last names
- Your date of birth or Health Insurance Number
- The date and type of surgery
- Confirmation of the permanent or temporary character of the ostomy
- The first and last names, and the permit number of the physician
- The date of the prescription
- The physicians signature
Dont Miss: Who Provides Medicare Advantage Plans
Also Check: What Does Regular Medicare Cover
Ostomy Supplies: 10 Questions To Ask Before You Choose A Health Plan
Class I medical devices include ostomy supplies and accessories, such as ostomy bags. Manufacturers of Ostomy Supplies and Accessories are subject to the fewest regulatory controls, including registration of the facility where the device is manufactured, adherence to the FDAs Good Manufacturing Practices , labeling requirements, and prohibitions against misbranded and substandard products. Despite the fact that health insurance companies cover the vast majority of ostomy supplies, their reimbursement varies by state. Check to see if the plan will cover the items you require and how they will cover them. Before you make any decisions about your health insurance, consider these ten questions to ask yourself: What are your top health insurance options?
How Does A Pouching System Work
An opening is made in the skin barrier of the pouching system that matches the size and shape of the stoma. For example, if the stoma is round-shaped, the opening is round if the stoma is oval-shaped, the opening is oval. When the skin barrier is applied it should fit to the skin stoma junction providing skin protection. As the stool drains from the stoma it will pass over the skin barrier into the pouch and be contained in the pouch until emptied. There are many types of pouching systems available. The ostomy nurse will help you find the best, most secure fit.
Also Check: How Much Is Withheld From Social Security For Medicare
Recommended Reading: How Much Does The Medicare Coach Cost
Why Are Ostomy Supplies So Expensive
The annual out-of-pocket costs for ostomy supplies can be as high as $3,000 per year with insurance, but Medicare enrollees won’t typically pay as much as that. Eligible Medicaid enrollees typically get their ostomy supplies for free or pay a modest copayment. However, costs such as copayments and deductibles can be high if you rely on private insurance, causing many people with ostomies to experience financial distress.
Many countries provide medically necessary ostomy supplies for free through their public health care schemes, but the United States doesn’t. People with ostomies need to change their ostomy bag every 3 to 4 days, and they may need to change them daily if they experience complications. Therefore, the need for frequent changes means that supplies cost between $300 and $600 per month.
What Ostomy Supplies Are Covered By Medicare

Medically necessary ostomy bags are considered for coverage under the Part B portion of Original Medicare benefits plan if youve had an ileostomy, urostomy, or colostomy. For sufficient aftercare and appropriate Medicare coverage that serves your medical circumstances best, discuss the types of covered ostomy supplies your physician recommends.
Medicare Part B does require Medicare beneficiaries to pay the deductible, as well as 20% of the total cost of the ostomy supplies. Because an ostomy requires an extension of the body it is considered as a limb or prosthetic device that is considered medically necessary. Medicare will cover prosthetics.
Find a new Medicare plan
Get recommendations based on what’s important to you, and compare them to your existing plan.
Recommended Reading: Can You Work And Get Medicare
License For Use Of Physicians’ Current Procedural Terminology Fourth Edition
End User Point and Click Amendment:CPT codes, descriptions and other data only are copyright 2021 American Medical Association. All Rights Reserved . CPT is a trademark of the American Medical Association .
You, your employees and agents are authorized to use CPT only as agreed upon with the AMA internally within your organization within the United States for the sole use by yourself, employees and agents. Use is limited to use in Medicare, Medicaid or other programs administered by the Centers for Medicare and Medicaid Services . You agree to take all necessary steps to insure that your employees and agents abide by the terms of this agreement.
Any use not authorized herein is prohibited, including by way of illustration and not by way of limitation, making copies of CPT for resale and/or license, transferring copies of CPT to any party not bound by this agreement, creating any modified or derivative work of CPT, or making any commercial use of CPT. License to use CPT for any use not authorized herein must be obtained through the AMA, CPT Intellectual Property Services, AMA Plaza 330 N. Wabash Ave., Suite 39300, Chicago, IL 60611-5885. Applications are available at the AMA Web site, .
Do You Need A Prescription For Ostomy Supplies
There is no definitive answer to this question as it depends on a number of factors, including the type of ostomy supplies needed and the country in which you are located. In general, however, it is advisable to speak to a healthcare professional before purchasing any ostomy supplies, as they will be able to advise you on the best products for your individual needs. In some cases, a prescription may be required in order to obtain certain supplies, so it is always best to check with your healthcare team in advance.
You May Like: Does Medicare Cover Ct Lung Cancer Screening