Are Back Braces Covered By Medicare
Yes, a Medicare coverage policy can cover your back brace. Under Part B of Medicare back braces are covered as durable medical equipment.
According to Medicare.gov, the back brace must have medical benefits that are medically necessary to be covered by your plan. The same medical necessity criteria apply to other braces, including neck, leg, and arm. This means you will need a prescription for the brace from your doctor.
Medicare Coverage For Wrist Braces
Medicare covers wrist braces if they are medically necessary to treat a medical condition. For example, Medicare will cover wrists braces if the doctor has diagnosed carpal tunnel syndrome.
Suppose you have Carpal Tunnel Syndrome, and your doctor recommends wearing a brace at night or during the day while you are up and active. In that case, it is considered medically necessary by Medicare standards.
If your doctor advises that wearing the brace will relieve pain, fix the problem, or reduce permanent damage, its also covered.
Wrist braces can be covered if Medicare approved as durable medical equipment .
Can Csa Medical Supply Bill My Insurance For My Back Brace
Yes, CSA Medical Supply does have the ability to bill your insurance company for the purchase of a medical grade back brace. We currently accept Medicare, Florida Medicaid, and most private insurances. If you are interested in having your insurance company cover the purchase of your back brace or support please contact us at 272-6335 and one of our insurance specialist will be happy to assist you.
Read Also: Where Do I Get A Medicare Card
Durable Medical Equipment Generally Covered By Medicare If You Qualify
If you dont find the equipment you are looking for in my list of Medicare covered DME below, you can use this link to Medicare.gov
Air-Fluidized BedAlternating Pressure Pads and MattressesAudible/visible Signal Pacemaker MonitorPressure reducing beds, mattresses, and mattress overlays used to prevent bed soresBead BedBed Side RailsBed Trapeze covered if your loved one is confined to their bed and needs one to change positionBlood sugar monitorsBlood sugar test stripsCanes Commode chairsContinuous passive motion machinesContinuous Positive Pressure Airway Devices, Accessories and TherapyCrutchesVentilators WalkersWhirlpool Bath Equipment if your loved one is home bound and the pool is medically needed. If your loved one isnt home bound, Medicare will cover the cost of treatments in a hospital.
What Forms Of Scoliosis Treatment Are Available

According to the Mayo Clinic, for many people scoliosis can be managed without surgery. In some cases, scoliosis treatment might require surgery to relieve pain or restore balance in the spine. For example, you might need surgery if:
- You have persistent pain in the back or legs
- An overly tilted spine
- Arthritis in your spine
The Scoliosis Research Society adds that doctors might recommend scoliosis treatment with surgery in certain other situations, such as:
- Non-surgical treatments havenât worked
- You have disabling pain and spinal imbalance
- You have a poor quality of life because you canât move well or do many basic activities.
Most adults with scoliosis do not have disabling symptoms, according to the Scoliosis Research Society. If your doctor says you donât need surgery, he or she might recommend scoliosis treatments such as:
- Periodic doctor visits to observe the condition
- X-rays so your doctor can measure the spine curvature
- Over-the counter pain relievers
- Exercises to strengthen the core muscles of the abdomen and back and improve flexibility
- Braces for short-term use in relieving pain
For more severe symptoms, scoliosis treatment may include magnetic radiology imaging , epidural or nerve block injections, or prescription pain medication.
Two common surgical procedures for scoliosis treatment include surgical stabilization and surgical fusion .
You May Like: What Makes You Eligible For Medicare
Does Medicaid Cover Back Braces And Other Dme
Medicaid has a very different structure from Medicare, as its programs are funded both federally and by each individual state.
Concretely, this means that each individual state has quite a lot of leeway with what it does on its Medicaid programs, so long as it follows the Medicaid guidelines.
It is not uncommon for Medicaid to allow a state to waive some of its eligibility requirements for a program, so that a state may be able to give health care to people who might otherwise not get it.
When this is done, its known as a Waiver, and each different waiver can have specific eligibility requirements targeting specific elements of the population, and often with limited places.
This has resulted in hundreds of waivers, all with different eligibility, and all across the US.
Money Follows The Person
Money follows the person this Medicaid program works with elderly adults who are in nursing care, and if they are able, helps to transition them back to living, somewhat independently, in their own homes.
Items which are required both for making the transition, and then to the elderly person maintaining their independence, are paid for by the program.
This can be buying standard DME, or it can be as much as remodeling parts of a home to make the move possible.
The range of DME allowed is considerably wider than with Medicare, which certainly does not cover home modifications.
Don’t Miss: How Old Do You Need To Be To Receive Medicare
Now You Have A Signed Prescription From Your Medicare
Now that you have your prescription
- you will have to find a Medicare-enrolled DME supplier
- only go through a supplier who is a Medicare-enrolled participating supplier who accepts assignment this ensures you pay only what you have to
- Medicare only gives coverage to pretty basic models of each equipment type, although you may sometimes be able to upgrade with certain DME by paying the difference yourself
- select your DME that you have been prescribed from the available choices
- sort out the necessary paperwork with the supplier any forms etc
Medicare part B covers 80% of the Medicare-approved price for DME if you used a Medicare-enrolled supplier with a signed prescription from a Medicare-enrolled doctor saying that your item is medically necessary.
If you used a Medicare-enrolled participating supplier who accepts assignment, you will just have to pay your Medicare 20% co-payment of the Medicare-approved price for your DME, and your deductible if it applies.
Do get your item through a Medicare-enrolled supplier who is a Medicare-enrolled Participating supplier who accepts assignment, if you dont, you can end up paying way too much.
Medicare will either rent or purchase DME for the majority of equipment, and especially the pricier items, Medicare will rent from the supplier.
If your equipment is rented, you will just pay a 20% co-payment of the monthly rental, and if it applies, your deductible, at the outset.
Prosthetic And Orthotic Items
Orthopedic shoes only when theyre a necessary part of a leg braceArm, leg, back, and neck braces , as long as you go to a supplier thats enrolled in MedicareArtificial limbs and eyesBreast prostheses after a mastectomyOstomy bags and certain related suppliesUrological suppliesTherapeutic shoes or inserts for people with diabetes who have severe diabetic foot disease.
You May Like: What Is Step Therapy In Medicare
Back Brace Scams Target People On Medicare
Scammers have been targeting Medicare recipients with a scheme to get free or low-cost back and knee braces. Theyre calling, running television ads, and mailing letters to get people to give their Medicare information. But if you give them your information, theyll use it to fraudulently bill Medicare for braces or other medical equipment. This uses up your medical benefits, which means you might not be able to get the right brace later, if your doctor prescribes one.
If you or someone you know is covered by Medicare, please share these ideas on how to avoid these scams:
If youve seen or heard about this or other scams, report it to the FTC online or by calling 1-877-FTC-HELP .
Does Medicare Cover Ankle Braces
Yes, Medicare will help cover the costs of ankle braces. Beneficiaries pay only 20% of the cost for ankle braces with Part B. Benefits may include ankle braces, straps, guards, stays, stabilizers, and even heel cushions.
Acute and chronic ankle or foot pain is a common, everyday use for these devices. Other conditions may benefit from using ankle braces such as ankle instability or osteoarthritis.
- Was this article helpful ?
Read Also: Are Hospital Beds Covered By Medicare
License For Use Of Physicians’ Current Procedural Terminology Fourth Edition
End User Point and Click Amendment:CPT codes, descriptions and other data only are copyright 2021 American Medical Association. American Medical Association. All Rights Reserved . CPT is a trademark of the American Medical Association .
You, your employees and agents are authorized to use CPT only as contained in the following authorized materials of CMS internally within your organization within the United States for the sole use by yourself, employees and agents. Use is limited to use in Medicare, Medicaid or other programs administered by the Centers for Medicare and Medicaid Services . You agree to take all necessary steps to insure that your employees and agents abide by the terms of this agreement.
Any use not authorized herein is prohibited, including by way of illustration and not by way of limitation, making copies of CPT for resale and/or license, transferring copies of CPT to any party not bound by this agreement, creating any modified or derivative work of CPT, or making any commercial use of CPT. License to use CPT for any use not authorized herein must be obtained through the AMA, CPT Intellectual Property Services, AMA Plaza, 330 Wabash Ave., Suite 39300, Chicago, IL 60611-5885. Applications are available at the AMA Web site, .
What Are Knee Braces Used For
Knee braces are used to help support, stabilize, and rehabilitate the knee when it becomes difficult and painful to walk and move around. They help shift weight from the problem area of the knee to the healthy part. Or, if the whole knee is an issue, a brace helps alleviate pressure all over.
The largest cause of knee problems in elderly people is osteoarthritis, which is the most common form of arthritis in America. Around 30 percent of seniors suffer from the condition, and the most-affected joints are the knees. Other leading causes including trauma to the knee and bone spurs.
Osteoarthritis occurs when the padding between joints in your body, such as your knees, wears down over time and causes the joints to rub together. This causes pain, swelling, reduced range of motion, discomfort, and a clicking or cracking sound, according to the Arthritis Foundation. Osteoarthritis makes the simple act of moving around on your feet difficult and painful.
This Is Where Knee Braces Can Help. They Have Four Main Functions:
Relieving Pain And Pressure:
This is the primary function of knee braces for the elderly, especially those with arthritis. They can help take the pressure off the joint and reduce pain. In doing this, an elderly persons independent mobility can increase.
Stabilize The Knee:
Rehab The Knee:
Prevent Injury:
Read Also: How Does A Medicare Supplement Plan Work In General
Does Medicare Cover Scoliosis Treatment
If your spine is curved sideways â for example, in an S or a C shape -you could have a condition called scoliosis. People of all ages can have scoliosis, notes the National Institute of Arthritis and Musculoskeletal and Skin Diseases. If your scoliosis is painful or interferes with movement, you may want to find out about scoliosis treatment.
Adult scoliosis may have originated during childhood, according to the Mayo Clinic. It can also be the result of spinal degeneration, or conditions such as osteoporosis .
Scoliosis can cause pain in your back and/or shooting down your legs, or numbness, according to the Scoliosis Research Society. Such discomfort might drive you to find scoliosis treatment.
When Will Medicare Cover Back Braces
There are certain criteria that must be met in order for back braces to be covered by Medicare as durable medical equipment:
Don’t Miss: Can I Cancel My Medicare
Medicare Advantage Plans Can Cover Braces
Medicare Advantage plans must provide the same hospital and medical benefits as Original Medicare .
This means that if your knee brace would be covered by Original Medicare, it will also be covered by a Medicare Advantage plan.
Medicare Advantage plans are sold by private insurance companies as an alternative to your Part A and Part B benefits.
In addition to the standard hospital and medical benefits provided by Original Medicare, most Medicare Advantage plans cover prescription drugs, and many offer additional benefits such as:
How Back Braces Are Covered By Medicare
Back braces are categorized as durable medical equipment, or DME. Durable medical equipment consists of products and items used for medical purposes, such as crutches, wheelchairs, braces and more.
Items classified as DME are covered by Medicare Part B.
Because Medicare Advantage plans are required by law to include all of the same basic benefits as Medicare Part A and Part B, back braces are also covered by Medicare Advantage plans.
Don’t Miss: Are You Eligible For Medicare If You Never Worked
Does Aflac Pay For Back Braces And Other Appliances
Yes! AFLAC covers several medical devices. APPLIANCES BENEFIT: Aflac will pay the applicable amount shown below when a Covered Person receives a medical appliance, prescribed by a Physician, as an aid in personal locomotion, for Accidental Injuries sustained in a covered accident. Benefits are payable for the following types of appliances:
| Back Brace |
Qualifying For A Back Brace With Medicare
Back pain complicates your lifestyle and interferes with your ability to enjoy your daily activities. When the pain worsens over time or you notice a problem with the treatment plan, an Orlando chiropractor may recommend a back brace. The challenge you may face is determining when your Medicare covers the cost of the brace and when it may not qualify for coverage.
Don’t Miss: What Does Plan N Medicare Supplement Cover
Does Medicare Cover Neck Braces
Neck braces may include cervical collars or other neck supporting devices. Cervical traction collars are the exception. Currently, Medicare doesnt pay for these devices.
Find Medicare Plans in 3 Easy Steps
We can help find the right Medicare plans for you today
Cervical collars may be either soft or hard. Soft collars are more comfortable typically, these braces are made of foam, felt, or rubber.
Hard neck supports may keep the head and neck completely still. After invasive surgery or severe neck injury, your doctor may prescribe hard neck support. Soft braces are best following a less strict procedure for only a few hours each day.
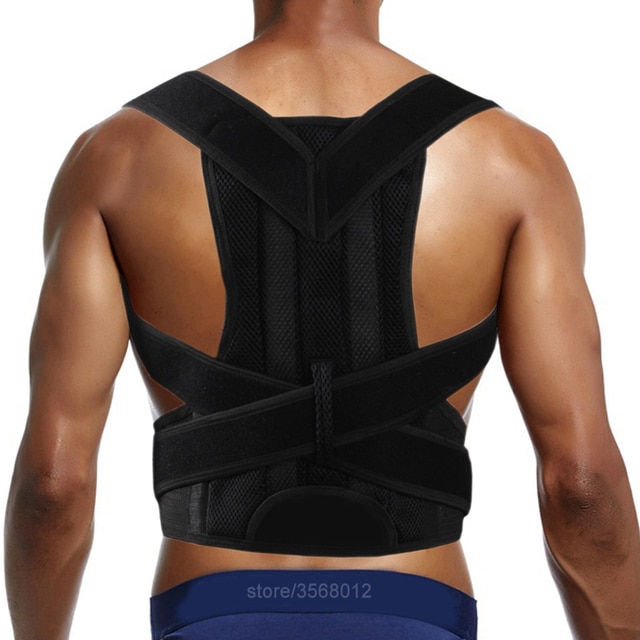
Back Brace Through Medicare
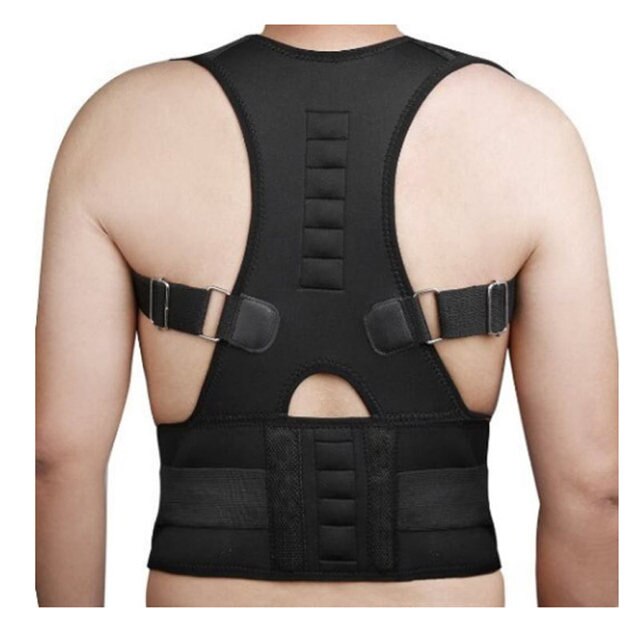
If youre a Medicare recipient, you may qualify for a back brace through Medicare that provides exceptional support and comfort for all-day wear. If you suffer from back pain and need to use a back brace, you may not have to pay for one out-of-pocket. Our staff at Affinity Medical Supplies can assist you with looking at braces and assessing your insurance benefits to see if youre eligible for our free products. Many of our clients are fully covered by their insurance plan lets find out if youre covered, as well. Contact us regarding your Medicare back brace for free.
What Qualifies a Back Brace For Medicare?
If your Medicare-approved physician has already prescribed a back brace for your pain, youre free to shop for a DME brace wherever you choose. The only stipulation is that the brace must be durable, used in your home, and have an expected lifetime of 3+ years. Affinitys MetForce back braces meet all Medicare criteria and are ideal for protection and recovery from injury. Click the Products link on our websites homepage to learn more about MetForce braces and how they benefit our customers.
FAQs on Affinity
Medicare Approved Pain Relieving Back Braces
- Chronic back pain
- And many other back issues
The Best Back Brace Covered by Medicare
Read Also: How To Check My Medicare Account
Medicare Prior Authorization Changes For Off
If you are involved with Medicare durable medical equipment , you should be aware of some upcoming rule changes that may affect you in the next few months. These changes will require suppliers to obtain a prior authorization before dispensing and billing for a back or knee brace.
These changes apply to suppliers and will also affect healthcare providers and patients.
What Prior Authorization Means For Healthcare Providers
Healthcare providers and clinics that supply off-the-shelf knee and back braces to patients will have to submit the prior authorization request and receive a decision before services are performed or items are provided to patients.
The prior authorization request must include a written order/prescription, as well as relevant information from the patient medical record , and supplier-produced documentation. Once the prior authorization request is received, a decision will be made and affirmation or non-affirmation will be provided. For orthoses like knee and back braces, the decision will be made within five business days from receipt of the request.
If a prior authorization request is not submitted and affirmed prior to billing a claim, the claim will be denied payment.
With prior authorization, providers will know that the braces they order will be covered and paid for. However, there is a concern for time delays and access to care for patients, to which the Federal Registry documentation states: If at any time we become aware that the prior authorization process is creating barriers to care, we can suspend the program. For concerns or complaints about this program, be sure to contact 1-800-Medicare.
Read Also: Should I Get Medicare Supplemental Insurance
