Compression Socks Make My Legs Hurt More Is This Normal
Question: How big of a size do compression stockings come in? Answer: Compression socks should be comfortable and supportive. If the stockings are making your symptoms worse, it is likely that they do not fit you correctly. There are numerous companies that make standard sized compression stockings. Some make 7 to 8 different sizes. Additionally,
What Causes Varicose Veins
If you have varicose veins , it means that the veins in your legs aren’t working properly.
To reach your heart, your body must carry your blood upwards through one-way valves in your legs. Varicose veins occur when those valves give way and allow blood to flow backwards. This increases the pressure in the vein, often causing swelling, pain, heaviness, itching and discoloration.
If certain lifestyle changes and conservative treatments arent enough to treat varicose veins, there are several non-invasive treatments that can be performed to treat and manage varicose veins.
How Does Medicare Cover Varicose Vein Treatment
Varicose veins are twisted or bulging veins that lay right below the surface of the skin. They are common in the legs and other parts of the body. Varicose veins can happen when regular veins become weak and stretched out.
- Varicose veins can be treated with an injectable adhesive, such as Venaseal glue, to close the affected varicose veins.
- Alternately, Varithena foam can be injected into the veins through a small catheter. The foam irritates the lining of the varicose vein and causes it to close
If your varicose treatment is covered by Medicare, Part B medical insurance usually is responsible for covering the costs since as an outpatient procedure.
If you need inpatient hospital treatment for any reason, Part A will help cover your hospital costs.
You May Like: What Is The Best Medicare Supplement Company
We Work With You To Maximize Your Insurance Benefits
Since most varicose and spider veins are symptoms of vein disease, their treatment is typically covered by common insurance plans. Give us a call at to see if we work with your specific insurance plan.
For patients whose costs are not covered, we offer a range of financing options including CareCredit and HELPcard*, and HSA and FSA accounts may qualify, so financial concerns shouldnt stop you from getting the relief that you need.
What Treatment Options Are Available For My Cvi
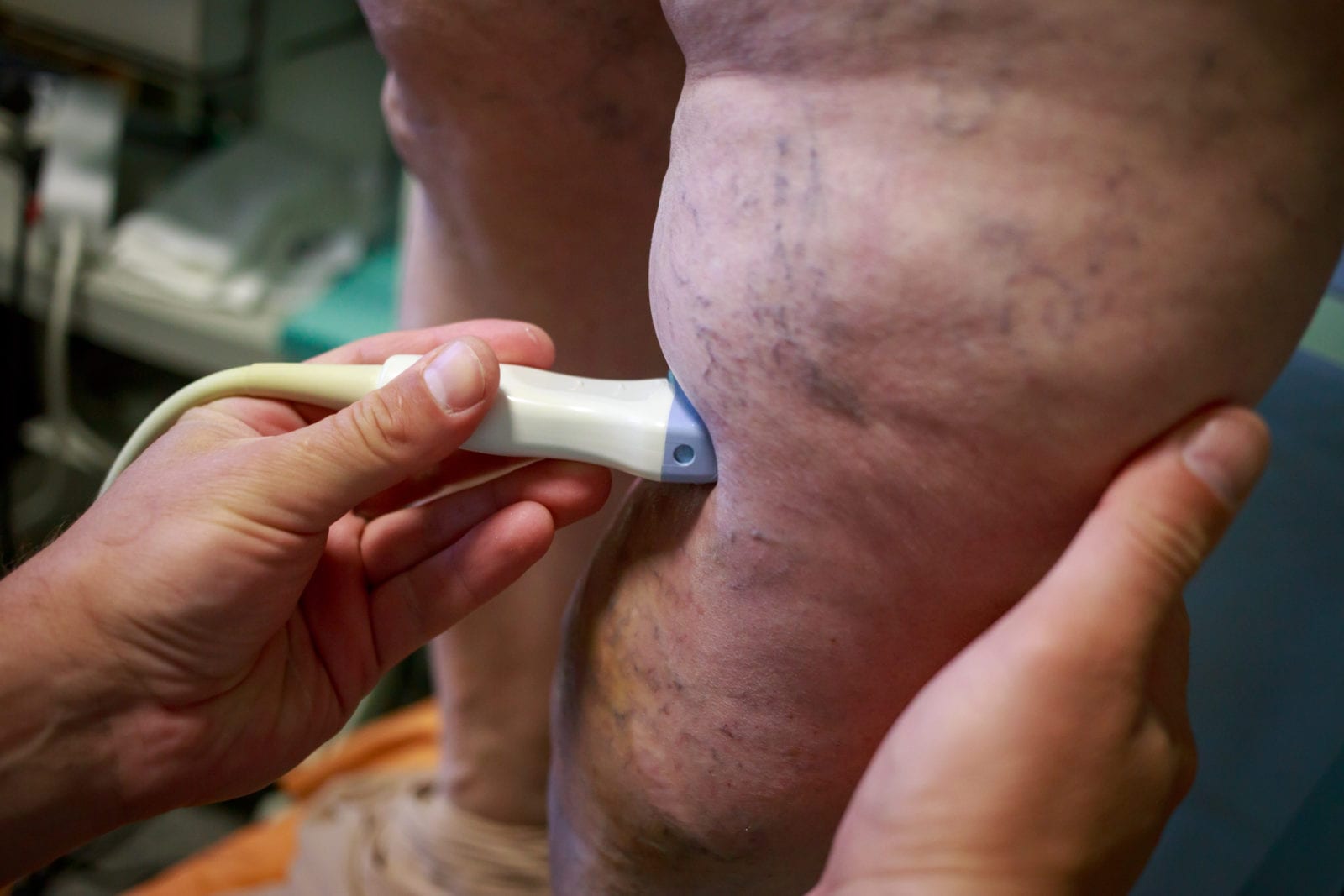
Question: What treatment options are available for my CVI? I cant sit or stand in one place and I have heavy, aching legs all of the time. I started to have achy, heavy leg feelings about a month after I sprained my right ankle and scratched my left knee last April. I was diagnosed with
Recommended Reading: Does Medicaid Pay For Part B Medicare
Are Varicose Veins Covered By Medicare
Varicose veins may be covered by Medicare, depending on whether its considered medically necessary. Generally speaking, Medicare provides rebates for the treatment of varicose veins which are 2.5mm or larger in diameter.
If your varicose vein treatment is covered by Medicare, as its an outpatient procedure it will fall under Part B, which means Medicare will pay the majority of the cost and youll only have to pay a small deductible. You may also be eligible for the Medicare safety net, depending on the type of vein treatment required.
You May Like: Does Medicare Cover Chronic Pain Management
Does Medicare Cover Varicose Vein Treatment
If youre over the age of 65 with twisted or bulging veins in your legs, you might be curious to find out whether Medicare covers varicose vein treatments.
The risk of varicose veins increases with age. Aging causes normal wear and tear on the valves inside your veins that help regulate blood flow. Over time, that wear can lead to weakened valves, which allow some blood to flow backward. This causes blood to pool and collect, which is the reason your veins may be more visible than they were when you were younger. This reflux can even lead to significant pain and discomfort if its left untreated.
Read Also: How Do I Check On My Medicare Application
How Much Does Varicose Vein Treatment Cost With Medicare
If Medicare covers your varicose vein treatment, there are some out-of-pocket costs you should expect to pay, which may include:
- The Medicare Part B deductible, which is $233 per year in 2022.
- After your Part B deductible is met, you are usually required to pay 20 percent of the Medicare-approved amount for most doctors services. There is no annual limit on how much you could pay for the Part B coinsurance in a given year.
- If your varicose vein treatment requires inpatient care, you will need to meet your Part A deductible before your Part A hospital insurance coverage kicks in. In 2022, the Part A deductible is $1,556 per benefit period.
Speak directly with your doctor for specific cost and coverage information for your varicose vein treatment.
Are Varicose Vein Treatments Covered By Medicare
Generally, Medicare will cover between 75% and 85% of the costs, so the fee you pay will depend on the severity of your case. Below is a breakdown of the estimated out-of-pocket costs you might expect from The Vein Institute:
- Initial consultation: 30 minutes with a Phlebologist. An ultrasound will be performed during this consultation. $215
- Spider vein treatment: Multiple sessions with a Phlebologist are required. $500 $1,500
- Varicose vein treatment: One session with a Phlebologist who will perform the recommended treatment: Endovenous Therapy, Radiofrequency Therapy or Medical Superglue. Between 2-5 follow up sessions with a Phlebologist where Sclerotherapy may be used to treat smaller veins surrounding the affected area. A post-care plan including compression stockings. $500 $3,000
Except for the smaller spider veins, which are considered cosmetic, all rebates are claimable through Medicare. In Australia, the Medicare Safety Net reimburses eligible patients once a threshold has been reached.
Read Also: When Do You Register For Medicare
Other Cpt Codes Related To The Cpb:
37252 Intravascular ultrasound during diagnostic evaluation and/or therapeutic intervention, including radiological supervision and interpretation initial noncoronary vessel 75820, 75822 Venography, extremity, unilateral or bilateral, radiological supervision and interpretation 93922 Limited bilateral non-invasive physiologic studies of upper or lower extremity arteries, 93923 Complete bilateral non-invasive physiologic studies of upper or lower extremity arteries, 3 or more levels , or single level study with provocative functional maneuvers 93924 Non-invasive physiologic studies of lower extremity arteries, at rest and following treadmill stress testing, complete bilateral study 93970 Duplex scan of extremity veins including responses to compression and other maneuvers complete bilateral study 93971
Compression Following Treatment For Varicose Veins
El-Sheikha et al stated that consensus regarding compression following treatment of VV has yet to be reached. This systematic review aimed to establish the optimal compression regimen after venous treatment. A systematic review of MEDLINE, Embase and CENTRAL was performed to identify RCTs investigating different compression strategies following treatment for superficial venous insufficiency. A total of 7 RCTs comparing different durations and methods of compression fulfilled the inclusion criteria. The treatment modality was open surgery in 3 trials, foam sclerotherapy in 2 and EVLA in 2 trials. The quality of the studies was variable, and significant sources of potential bias were present. Both the studies and compression regimens used were heterogeneous 10 products were used in 6 general regimens for a duration of 0 to 42days. One study suggested that 7days rather than 2days of stockings following EVLA was associated with superior QoL and less pain at 1week. Another study reported that, following surgery, application of a compression stocking after 3days of bandaging was associated with a slightly longer recovery than no compression after 3days. One study recorded compliance clearly, finding it to be only 40 %. The quality and heterogeneity of the studies precluded meta-analysis. The authors concluded that there is currently little quality evidence upon which to base any recommendations concerning compression following treatment for VV.
Also Check: When Can You Sign Up For Medicare Part D
Does Medicare Cover Varicose Vein Surgery
There are different types of surgeries for varicose veins the cost changes depending on the type and where you undergo the procedure. For example, vein stripping surgery prices are between $1,500 and $3,000 not including the facility fees. Additional facility or surgery center costs may increase the total amount.
Another varicose vein surgery is called ambulatory phlebectomy. Ambulatory phlebectomy is a much less invasive procedure compared to vein stripping and ligation. Prices change depending on how extensive the service is.
Get A Free Quote
Find the most affordable Medicare Plan in your area
The medical world has several available surgery options for treating varicose veins. Your doctor should discuss your condition and what surgeries may be best for you. Regardless of the surgery you and your doctor decide is best, youll have to pay 20% out of pocket if you dont have supplemental insurance.
About Vein Centers Of Connecticut
Our mission is for patients to be happy and productive by eliminating their pain and enhancing their appearance. Minimally invasive, pain free vein therapy enables patients to immediately resume normal activities. Aesthetic services are often their logical next step to building their relationship with us.
It is the expectation for our patients to become symptom free. With symptomatic resolution, they can enjoy active, pain free lifestyles and enjoy a new found confidence in their improved appearance. Seeing that smiling face and hearing how lives have been improved after a successful treatment is very rewarding to our team of physicians and certified medical professionals.
Also Check: Eye Doctors In Traverse City That Accept Medicaid
Recommended Reading: Does Medicare Pay For Dtap Shots
When Should I Get The Venaseal Treatment
There are several symptoms that may occur if you have varicose veins. If you are experiencing any of these, it is important to see a doctor and determine the best treatment option for you. The most common symptoms of varicose veins include:
- Veins that appear to be twisted or bulging, and may also be dark purple or blue in color
- An achy or heavy feeling in the legs
- Pain, swelling, itching, burning or cramping in the legs
- Bleeding veins, ulcers or skin inflammation
- Restless Legs Syndrome
We have doctors with years of experience recommending the best treatment options. We have several different treatment options, with VenaSeal among them. After most treatments, compression stockings are required to be worn for a short period of time, but with VenaSeal compression stockings are unneccessary. Because of this, VenaSeal is a great treatment option any time of year.
Now that VenaSeal is being covered by Medicare, it is the perfect time to get treatment for your varicose veins. today to get your treatment scheduled!
Medicare Coverage For Spider Veins
Spider veins are thin clusters of blood vessels that appear on the surface of the skin but they dont bulge outwards. These blood vessels are in the form of spider webs or tree branches. Spider veins are not dangerous in and of themselves, even though they look awful. However, spider veins are often symptomatic of underlying venous insufficiency.
As such, you need to seek proper diagnosis so the vein doctor can determine if your spider veins are caused by vein disease. You can receive medicare coverage for the underlying venous insufficiency but not to treat the superficial veins.
Basically, whether medicare will cover treatment depends entirely on whether your spider veins and varicose veins are caused by chronic venous insufficiency.
Read Also: Are Lidocaine Patches Covered By Medicare
Does Medicare Advantage Cover Varicose Vein Treatments
Carriers offering Medicare Advantage plansMUST include all the benefits of Medicare. So, if Medicare covers your varicose vein treatment, an Advantage plan will also cover the costs. But, Advantage plans often have a specific network of doctors and facilities the beneficiary must use.
Going outside the plans network may be costly. Check your plans policies and find out what doctors and facilities are in-network to avoid unwanted medical bills. The other crucial point with Advantage plans is they choose how much you pay out of pocket for a service, making your medical costs very unpredictable.
Sclerotherapy Why Doctors Choose This Treatment For Spider Vein Removal
Sclerotherapy is the treatment of choice for the removal of spider veins , reticular veins, and small varicose veins. Sclerotherapy is minimally invasive, safe, and relatively pain-free.
Doctors administer sclerotherapy by injecting a sclerosant into your vein. The most commonly used agents are hypertonic saline, sodium tetradecyl sulfate, polidocanol , and chromated glycerin. The sclerosant causes the vein to close and eventually be reabsorbed into the body. Your body naturally reroutes blood flow to the surrounding healthy veins.
Read Also: What Is The Medicare Part A
Rare Health Insurance Policy Exclusions
There are rare cases in which there is a fine print exclusion spelled out in the extremely long insurance document that most people have never had time to review. The exclusion would specifically state that your insurance plan does not cover any leg vein treatments. In our experience, this is found in less than 5% of health insurance policies. We would determine if you had any exclusion by speaking with your insurance plan prior to scheduling any treatment.
Does Medicare Cover Varicose Veins Repair
If you are on Medicare and are considering having your varicose veins repaired, youre probably wondering if your plan will cover the treatment. Medicare coverage varies by state and region, so the only way to know for sure if Medicare will cover your procedure is by having your doctor request a preauthorization the outcome of the preauthorization will provide 100% certainty whether your treatment will be covered or not.
However, in cases where varicose veins repair is covered, patients must meet certain conditions in order for the treatment to be paid for by Medicare. Use the guidelines below to determine how likely it is that your Medicare plan will pay for your varicose veins repair.
Spider Veins
Spider vein treatment is generally considered cosmetic and is rarely covered by Medicare. Spider vein treatment is only covered if spider veins are exhibiting dangerous symptoms, such as ongoing and substantial bleeding.
Health Impacts
Your varicose vein repair will be more likely to be covered if you are experiencing health issues or degradation in your quality of life due to venous disease. Patients who are experiencing pain caused by venous disease are more likely to qualify for coverage. Additionally, patients who have external bleeding from their varicose veins or external sores that wont heal caused by varicose vein hemorrhaging are likely to have treatments covered.
Alternative Treatments
Finding a Doctor
Also Check: Does Medicare Payment Come Out Of Social Security Check
Private Health Insurance For Varicose Veins
Generally, private health providers only cover treatments performed in-hospital, as they are protected by the hospital insurance.
The minimally invasive treatment options, such as EVLA and those available at The Vein Institute, are performed in a private medical practice. As a result, minimally invasive procedures are only covered by Medicare.
Surgical stripping is performed in-hospital and is as onerous as the name implies. It involves a couple of days in the hospital, general anesthetic and a long, painful recovery time.
What Causes Varicose Veins And Spider Veins
Problems in the valves in your veins can prevent blood from flowing normally and cause varicose veins or spider veins.
Your heart pumps blood filled with oxygen and nutrients through your arteries to your whole body. Veins then carry the blood from different parts of your body back to your heart. Normally, your veins have valves that act as one-way flaps. But, if the valves dont close correctly, blood can leak back into the lower part of the vein rather than going toward the heart. Over time, more blood gets stuck in the vein, building pressure that weakens the walls of the vein. This causes the vein to grow larger.
Don’t Miss: How Much Does Medicare A And B Cost Per Month
Who Is Eligible For Varicose Vein Treatments Through Medicare
Medicare only considers funding varicose vein treatment for beneficiaries with varicose veins wider than 4mm. It also requires enrollees to undergo at least 6 weeks of conservative treatment before it considers varicose vein treatment necessary.
Conservative treatments for varicose veins include weight loss, compression garments and elevating the affected extremity to reduce pressure. You will be expected to show records of which treatments you’ve tried. If you can’t wear compression garments for any reason, your doctor will need to explain why not.
Medicare may agree to pay for your varicose vein treatment if you are still symptomatic after exhausting all conservative treatment options. You will generally need to present with at least one of the following symptoms to qualify:
- Bleeding varicose veins
- Severe pain or swelling that interferes with your daily life
- Stasis dermatitis
Cpt Codes Not Covered For Indications Listed In The Cpb:
Polymorphism genotyping of matrix metalloproteinases genes, synthetic matrix metalloproteinases inhibitors, measurements of plasma growth factors , Ambulatory selective variceal ablation under local anesthetic and External valvuloplasty – no specific code 36011 Selective catheter placement, venous system first order branch 36468 Single or multiple injections of sclerosing solutions, spider veins limb or trunk 36473 Endovenous ablation therapy of incompetent vein, extremity, inclusive of all imaging guidance and monitoring, percutaneous, mechanochemical first vein treated 36474 Endovenous ablation therapy of incompetent vein, extremity, inclusive of all imaging guidance and monitoring, percutaneous, mechanochemical subsequent vein treated in a single extremity, each through separate access sites 36482 – 36483 Endovenous ablation therapy of incompetent vein, extremity, by transcatheter delivery of a chemical adhesive remote from the access site, inclusive of all imaging guidance and monitoring, percutaneous 37204 Transcatheter occlusion or embolization , percutaneous, any method, non-central nervous system, non-head or neck 37241 Vascular embolization or occlusion, inclusive of all radiological supervision and interpretation, intraprocedural roadmapping, and imaging guidance necessary to complete the intervention venous, other than hemorrhage 75894 Transcatheter therapy, embolization, any method, radiological supervision and interpretation
You May Like: Is Medicare Medicaid The Same
