For People Who Choose To Be Screened With Colonoscopy
Many people choose to be screened with colonoscopy. While it might not be right for everyone, it can have some advantages, such as only needing to be done once every 10 years. And if the doctor sees something abnormal during the colonoscopy, it can be biopsied or removed at that time, most likely without needing any other test.
Although many private insurance plans cover the costs for colonoscopy as a screening test, you still might be charged for some services. Review your health insurance plan for specific details, including if your doctor is on your insurance companys list of in-network providers. If the doctor is not in the plans network, you may have to pay more out-of-pocket.
Soon after the ACA became law, some insurance companies considered a colonoscopy to no longer be just a screening test if a polyp was removed during the procedure. It would then be a diagnostic test, and would therefore be subject to co-pays and deductibles. However, the US Department of Health and Human Services has clarified that removal of a polyp is an integral part of a screening colonoscopy, and therefore patients with private insurance should not have to pay out-of-pocket for it .
Purpose Of A Cologuard Test
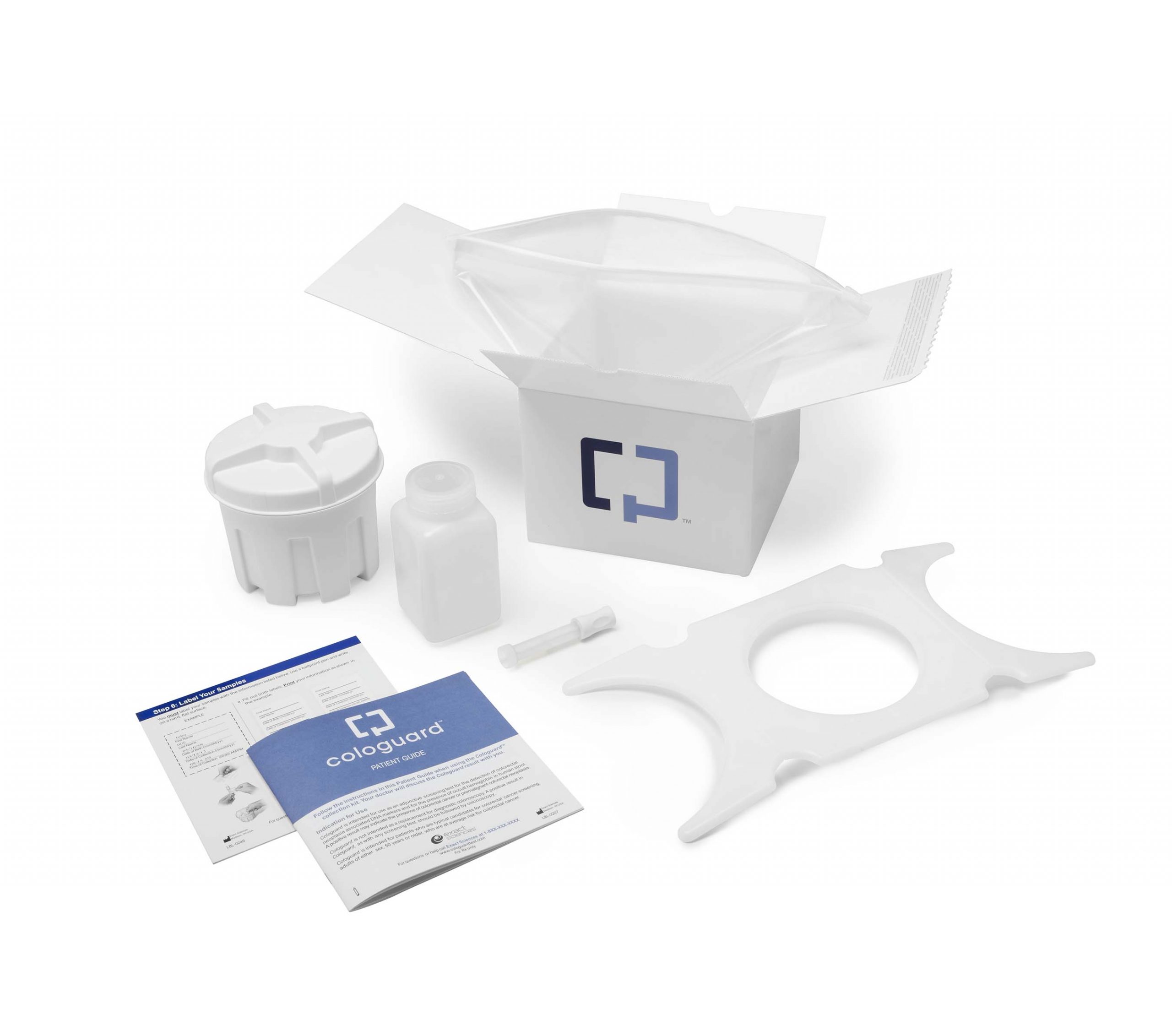
The Cologuard test uses a stool sample to look for microscopic blood and altered DNA. It starts with at-home test collection using special containers for the stool sample. After you have the stool sample ready, you send it to a lab for testing.
Cologuard looks for changes in your DNA that could indicate precancerous polyps or colon cancer. It combines two tests: fecal immunochemical testing to look for microscopic amounts of blood and DNA screening for abnormal cancer cells.
Colon cancer can be detectable using Cologuard because the lining of the colon sheds cells several times a day. These cells end up in the stool. Abnormal cells from a cancerous tumor or precancerous polyps are also shed into the stool, along with blood from any broken blood vessels.
Does Medicare Cover A Prostate Specific Antigen Test
- Get the facts about Medicare coverage for the prostate specific antigen test. Find out when and how frequently Medicare will pay for prostate cancer screening.
Prostate cancer ranks second only to skin cancer as a leading type of cancer in men. Approximately one in every eight men will develop prostate cancer at some point during their lives, according to the American Cancer Society. Early detection can greatly improve the chances of successful treatment, making prostate cancer screenings, such as the prostate-specific antigen test or PSA, important. Medicare typically pays for these tests. Read on to learn more.
Read Also: Stage 2 Cancer Symptoms
Also Check: What Are The Advantages And Disadvantages Of Medicare Advantage
Update: Cologuard Stool Dna Screening Test
This month, the Centers for Medicare & Medicaid Services issued its final National Coverage Decision for Cologuard, making it the first FDA-approved stool DNA test for the detection of colon cancer and precancer covered for Medicare patients throughout the country. This came after the exciting US FDA approval of Cologuard in August. You may have heard some buzz earlier this week about Cologuards availability to the public. It turns out some of these facts were incorrect. In order to eliminate any confusion around this new colon cancer screening test, were setting the record straight. Check out our updated FAQ to find out what you need to know.
I have Medicare. Is Cologuard now covered under my insurance?
Yes, on October 9, 2014 the Centers for Medicare & Medicaid issued a final determination and declared that Cologuard would be covered immediately for those on Medicare. Speak with your medical professional to determine if Cologuard is right for you.
I have insurance through another provider. Is Cologuard now covered for everyone?
No, Cologuard is not yet covered by private insurance. Exact Sciences, the maker of Cologuard, is actively working to get Cologuard approved for coverage by private insurance. We currently do not know when this will become effective.
Even though Cologuard is not covered by private insurance, can I still reach out to my insurance provider to see if they would approve the Cologuard test for me?
Additional Questions?
Does Medicare Cover Colonoscopy Prep

If your physician orders a colonoscopy prep kit, your Medicare Part D prescription drug plan will likely provide coverage. However, each Medicare Part D plan provides different coverage.
Thus, your plan may leave you responsible for a copayment or coinsurance when you receive the prep kit. Remember that Medicare prescription drug coverage is not part of Original Medicare. To receive this benefit, you must sign up for a policy through a private insurance company.
Also Check: What Glucometer Is Covered By Medicare
What Are The Different Types Of Colorectal Cancer Screenings And Eligibility Requirements For Each
The following are Medicare-covered colorectal cancer screening exams :
- A fecal occult blood test is a lab test used to check stool samples for hidden blood. Original Medicare covers this test every twelve months if you are age 50 and older.
- A screening colonoscopy is covered by Original Medicare as often as every 24 months for those at very at high risk, or once every 10 years if you are not at high risk. There is no minimum age requirement if medically-indicated by risk.
- Cologuard is the brand name of a test that you might have seen on television. It is less invasive than colonoscopy, and is an alternative that your physician might recommend if you are at low risk for colon cancer. If so, it is a Medicare-covered test.
- A flexible sigmoidoscopy is similar to a colonoscopy, but is much less widely recommended because it does not probe your entire colon. If ordered by your physician for a specific accepted indication, will be covered by Medicare.
- A barium enema is an X-ray of the colon after it has been filled with barium. It is generally not used for screening. However, if ordered by your physician for a specific accepted indication, will be covered by Medicare.
Medicare Advantage plans cover these same colorectal cancer screenings without applying deductibles, copayments or coinsurance as long as you see an in-network provider and meet Medicares eligibility requirements for these services.
When To Think About Taking A Cologuard Test
Your healthcare provider might recommend a Cologuard screening every three years after age 45. The test is recommended for people who have an average risk for cancer.
Average risk means you do not have:
- A personal history of colon polyps or colon cancer
- Family history of colon cancer
- Inflammatory bowel disease
Also Check: Can I Switch Medicare Supplement Plans
Does Medicare Cover Other Tests For Colon Cancer
Medicare covers three alternative methods for colon cancer screening. These tests can be done at home or by providing a blood sample, and they’re free if ordered by a doctor or other qualified health care provider. The alternative tests are only for patients who have no signs or symptoms and are at average risk of developing colorectal cancer. Coverage may vary by test type and age group.
| Test type | |
|---|---|
|
Fecal occult blood test |
This at-home test is covered annually for Medicare recipients aged 50 plus. |
| Multitarget stool DNA test | Medicare only pays for the Cologuard brand of sDNA test. The test can be done at home and is covered every three years for people aged 50-85. |
| Blood-based DNA test | Also known as a liquid biopsy, this test uses blood rather than a stool sample to detect colorectal cancer. This minimally invasive test is covered every three years for patients aged 50-85. |
Is A Colonoscopy Free Under Medicare
If your medical provider accepts Medicare, everything about the colonoscopy procedure is covered unless polyps are found.
Suppose polyps or other tissue are removed during the colonoscopy for analysis. In that case, the procedure is no longer preventive, and you may be subject to the standard 20% coinsurance for Part B services. You may also face a copay if the procedure is in an out-of-office setting where facility fees are typically charged.
Don’t Miss: Can You Have Medicare Part D And Private Insurance
Cpt Codes Covered If Selection Criteria Are Met:
44401 – 44408 Computed tomographic colonography, screening, including image postprocessing 74270 Radiologic examination, colon contrast enema, with or without KUB 74280 air contrast with specific high density barium, with or without glucagon 81528 Oncology screening, quantitative real-time target and signal amplification of 10 DNA markers and fecal hemoglobin, utilizing stool, algorithm reported as a positive or negative result 82270 Blood, occult by peroxidase activity , qualitative feces, consecutive collected specimens with single determination, for colorectal neoplasm screening 82272 Blood, occult, by peroxidase activity , qualitative, feces, 1 – 3 simultaneous determinations, performed for other than colorectal neoplasm screening 82274 Blood, occult, by fecal hemoglobin determination by immunoassay, qualitative, feces, 1-3 simultaneous determinations
How Medicare Covers Screening Colonoscopies
Colonoscopy is considered the gold standard of colorectal cancer screening.2 If youre at high risk for colorectal cancer, Medicare will cover a screening colonoscopy once every 24 months. For those not at a high risk, Medicare will cover a screening once every 120 months or 48 months after a previous flexible sigmoidoscopy.
Medicare will cover the costs of this test so long as your health care provider accepts assignment. You could face costs, such as a copayment, if a polyp or other tissue is found and removed during the procedure.
Also Check: Is My Spouse Covered Under My Medicare
What Is The Cash Price For Cologuard
The cost of Cologuard is around $500. Part of that cost may be covered by some insurances depending on your plan, co-pay, and deductible. Diagnostic testing is subject to deductibles and coinsurance. Screening colonoscopies are not subject to copays and deductibles and usually have no out-of-pocket costs for patients.
Who Needs A Colonoscopy

The U.S. Preventive Services Task Force recommends that people at average risk of colorectal cancer should have regular colonoscopies starting at age 50. The American Cancer Society recommends people start screening at 45.
The USPSTF concluded that colonoscopies provide a substantial benefit to people aged 50 to 75. But it found that a colonoscopy may not be as beneficial to people 76 to 85 whove had previous screenings.
Colorectal cancer is most often diagnosed in people from 65 to 74 years old, and the average age of death from the disease is 73.
Recommended Reading: What Is Uhc Medicare Advantage
The Affordable Care Act
Regardless of the insurance you are having, the Affordable Care Act mandates the insurance providers to follow the guidelines of the U.S. Preventive Services Task Force for coverage. If the screening test has received an A or B rating by this agency, private insurance companies would cover the cost of the test without charging a co-pay.
But, Medicare is exempted from this mandate and you may need to pay co-pays and co-insurance.
You May Like: Do I Need Medicare If I Have Other Insurance
What Is A Colonoscopy
A colonoscopy is an outpatient procedure in which a healthcare provider looks inside your large intestine. They do this with a flexible camera called a scope. The scope is inserted into the rectum and a small amount of air is pushed into your colon to allow the scope to see the colon walls.
Prior to the procedure, you will undergo bowel preparation that typically involves a low-fiber diet for a few days before the colonoscopy. It also usually involves drinking a liquid bowel preparation product. Drinking the colonoscopy prep through a straw or cooling it in the refrigerator can help make drinking the solution easier.
The goal of this preparation is to completely empty your colon by inducing watery diarrhea. Closely follow all prep instructions, including a mostly liquid diet the day before the procedure. Drinking plenty of fluids will help you avoid becoming dehydrated.
The entire procedure takes about 30 minutes. If polyps need to be removed, it will take longer. Youll stay in a recovery room after the procedure, although the duration of your stay depends on sedation and pain medication given.
Many colonoscopies are performed under general anesthesia, but you may also choose twilight, conscious sedation. Whatever method of anesthesia you choose, you will need someone to drive you home. Its usually advised to wait until the next day to resume your normal activities.
You May Like: What Is Medicare Plan G Supplement
Does Medicare Cover A Colonoscopy
Colonoscopies are an important test for early detection of colon cancer and precancerous polyps. Colorectal cancer is most commonly found in adults aged 65 to 74. The American Cancer Society estimates that in 2021, 104,270 new cases of colon cancer and 45,230 cases of rectal cancer emerged1. Because colon cancer is the third most common type of non-skin cancer in both men and women, and is the second leading cause of cancer death in the United States, early detection of colon cancer is important.1
If you are on Medicare and have been referred for a colonoscopy, you may have questions about whether your plan will pay for the test. The answer is yes, but there are some limits to how often and when Medicare will cover a colonoscopy. In some cases, you may need to undergo earlier tests or preventive measures.
Read Also: Invasive Ductal Cancer Prognosis
What Does A Positive Cologuard Test Really Mean
A positive Cologuard test means that DNA and/or hemoglobin biomarkers that are associated with colorectal cancer were detected in the stool. A negative Cologuard test means that Cologuard did not detect significant levels of DNA and/or hemoglobin biomarkers in the stool that are associated with colorectal cancer.
Read Also: How To Check Medicare Deductible
Does Aetna Medicare Cover Alternative Colorectal Screening Tests
Part C plans, such as Aetna Medicare, cover some alternative colorectal screening methods, including Cologuard and other blood-based biomarker screening tests. However, beneficiaries typically need a doctor’s referral, and they may also need to meet plan-specific age or medical criteria. Aetnas Medicare Advantage plans may also differ widely by region and policy type, so you should contact Aetna directly to find out more about your individual coverage.
Capsule Endoscopy For Colorectal Cancer Screening
Houwen and Dekker noted that the European Union recommends FIT as the preferred method for population-based screening programs, followed by colonoscopy in FIT-positive individuals. Such FIT-based programs have high participation rates, and a PPV of approximately 40 %, which makes it not so attractive to follow a positive FIT by another non-invasive test where no therapy nor pathology-based diagnosis is possible. Thus, CCE might only be a sensible option for those FIT-positive individuals who are unwilling to undergo colonoscopy. In other countries, depending on many factors like availability of endoscopy services and finances, the preferred screening methods might be different, and primary screening by colonoscopy may be recommended. In these areas, participation-rates could possibly be increased by offering CCE as an alternative screening method however, data of prospective studies on aspects like participation rates, accuracy, patient burden, logistics and cost-effectivity are needed first
In addition, European Society of Gastrointestinal Endoscopy and European Society of Gastrointestinal and Abdominal Radiology s guideline on Imaging alternatives to colonoscopy: CT colonography and colon capsule did not suggest CCE as a 1st-line screening test for CRC .
Don’t Miss: Do Any Medicare Plans Cover Dental
Does Medicare Cover Colonoscopies In 2022
Medicare Colonoscopy CoverageCost with MedicareOther Colon ScreeningsFinal ThoughtsFAQsIts Time for Medicare Annual Enrollment: Are You Ready?
If youre deemed a high risk for colorectal cancer, then Medicare will cover the full cost of colonoscopy screenings once every two years. For patients who arent at high risk, Medicare will still cover screenings every 10 years. In this article, Ill go over Medicares coverage for colonoscopies and whether other types of colon cancer screenings are included.
Does Medicare Cover Cologuard
Cancer is among the leading causes of death in the United States, and according to the American Cancer Society, colorectal cancers account for nearly 150,000 new cancer cases each year. While some colon and rectal cancers have a high level of treatment success, the key to beating these types of cancers is often to catch them early.
For most people, early detection can be done through a colonoscopy procedure along with other imaging studies.
Medicare Benefits Solutions
Unfortunately, a colonoscopy procedure is invasive and may make patients uncomfortable. Even though someone undergoing a colonoscopy is sedated, the procedure can have side effects that include pain and the potential for internal injury.
To add to this, the preparation for a colonoscopy can involve fasting and the use of specialized laxative medications to cleanse the colon. Thankfully, modern medicine has an answer to these problems through the use of testing solutions like Cologuard.
Recommended Reading: What Medicare Supplement Covers Hearing Aids
Does Medicare Cover Both Screening And Diagnostic Colonoscopies
Medicare pays for both screening and diagnostic colonoscopies. The tests are done the same way, with similar equipment, but are covered differently by Medicare.
A screening colonoscopy is a preventive procedure done to make sure the colon is healthy. You’re covered for a screening every 10 years if you’re at low risk for colorectal cancer, meaning you:
- Had no lower gastrointestinal signs or symptoms before the colonoscopy
- Had no polyps or masses found during the colonoscopy
- Have no family or personal history of polyps or colon cancer
If you’re at high risk for developing colorectal cancer, Medicare will cover your screening test every two years. You’re considered high risk if you:
- Have a personal history of colorectal cancer, a certain type of polyp or an inflammatory bowel disease such as Crohns disease or ulcerative colitis
- Have a close relative a parent, sibling or child who had colorectal cancer or a potentially cancerous polyp
- Have a family history of inherited ailments linked to colorectal cancer
Original Medicare covers screening colonoscopies at 100%. You pay no Part B deductible or coinsurance for a screening test.
A diagnostic colonoscopy is a different type of test. It looks for potential problems due to stomach pain that doesnt improve, anemia or if you’ve had polyps within the past 10 years.
Original Medicare covers diagnostic colonoscopies at 80%. You won’t pay a deductible but will pay the remaining 20% of the procedure cost.
