What If You Have Private Insurance And Medicare
If you already have healthcare coverage through a commercial insurer when you become eligible for Medicare, you have the option to keep both types of insurance and the option to use both. Your private plan can be the primary payer that handles your healthcare costs before Medicare does, or the private plan can be secondary to Medicare. Your choice depends on individual circumstances. One critical consideration: Medicare requires everyone 65 and older to have adequate prescription drug coverage defined as and your employer plan may not qualify.
You may choose to build your primary health coverage on private insurance if your spouse relies on that plan for coverage, or choose Medicare as your primary insurer after considering the deductibles, copayments, and coinsurances of both options.
Medicare and other insurance plans coordinate to avoid duplicate payments. If Medicare is your primary payer, it will pay first and then your private plan will kick in to cover some or all of the remaining costs. If Medicare is secondary, then the opposite occurs. Typically, Medicare cannot be changed from a primary payer to a secondary payer.
Whether Medicare is primary or secondary to existing insurance generally depends on the source of the other insurance policy. If you are uncertain about which insurer is your primary or secondary, you can check with your private plan or call Medicares Benefits Coordination & Recovery Center at 1-855-798-2627.
% Of Esrd Patients Are Under 65 Years Old But Only 11% Currently Have Medigap Coveragewe Must Do Better
Medigap provides dialysis patients with financial security and access to lifesaving transplant surgery. Medicare only pays for 80% of an individuals health care costs, making access to Medigap coverage critical for helping dialysis patients cover the remaining 20%. We need your support to help ensure all dialysis patients gain access to Medigap coverage regardless of age. Contact your Members of Congress today.
See how your state is doing in providing access to affordable Medigap coverage by using the interactive map below click on a state or simply select it from the dropdown menu. You can also download any state factsheet to share with your Members of Congress and/or state legislators.
Antecedents To The 1972 Legislation
A brief review of the evolution of federal government policy regarding hemodialysis and kidney transplantation is useful at this point. An extended treatment can be found in the literature . In 1944, in Nazi-occupied Holland, Willem Kolff first succeeded in prolonging the life of a patient using his primitive artificial kidney machine. After the war, Kolff sent four of his machines to Europe and the United States, where they provided a basis for successful treatment of acute renal failure in the Korean War.
In 1960, Belding Scribner of the University of Washington in Seattle, working with Wayne Quinton, an engineer, invented a permanent vascular access device and placed his first patient on long-term, continuous, intermittent hemodialysis. That patient, Clyde Shields, lived 11 years. In 1963, when the hemodialysis procedure for treating chronic kidney failure was barely three years old, the Veterans Administration announced its intention to establish approximately 30 dialysis treatment units in VA hospitals across the country. These efforts, among others, would later prompt the Bureau of the Budget to question the fiscal implications of dialysis. In fact, when the Gottschalk Committee was formed in the mid-1960s, for example, Pierre Palmer, the Budget Bureau staff officer assigned to it, was the examiner for the VA hospital program.
Recommended Reading: What Does Plan C Cover In Medicare
When Medicare Coverage Starts For Esrd
Eligibility for Medicare coverage due to ESRD is different from other types of Medicare eligibility. If someone is eligible for Medicare because of ESRD and doesnt enroll immediately, their coverage could still begin up to 12 months prior to the month they apply, known as retroactive coverage. How this looks will depend on whether they are on, or need, dialysis, or require a kidney transplant.
In the event a Medicare patient is on dialysis, their coverage typically begins on the first day of the fourth month of dialysis treatment. Do note, this four-month waiting period starts even if someone hasnt yet signed up for Medicare.
If someone is covered by an employer group health plan, their coverage will still begin the fourth month of dialysis. As well, the group health plan may cover the first three months of treatment.
Medicare coverage begins as soon as the first month of a regular course of dialysis treatments if all of the following are true:
-
The patient participates in a home dialysis training program during the first three months of a regular course of dialysis
-
The patients doctor expects them to complete home dialysis training, meaning they can perform self dialysis at home
-
They continue regular course dialysis treatments throughout the waiting period
Medicare coverage for kidney transplants works differently than dialysis. Learn more at this resource. Learn more at this resource.
What Distinguishes Medicaid From Medicare
Although Medicaid and Medicare may sound similar, they are two separate federal programs.
While Medicaid is open to all members of society who are poor, Medicare is only available to people over the age of 65 or who have a disability.
Both types of financial aid are available at the same time, and they often cover different parts of medical treatment.
Read Also: What Age Can You Start To Collect Medicare
When Does Medicare Pay For Kidney Dialysis
Medicare coverage for your kidney dialysis may depend partly on your age.
-
If a Medicare beneficiary is age 65 or older, dialysis is available immediately.
-
If the beneficiary is under 65, Medicare will pay for dialysis starting the first day of the fourth month of treatments. Waiting periods may apply to those under the age of 65.
You must receive services and supplies from Medicare-approved facilities, doctors and vendors for dialysis to be covered by Medicare.
Medicare patients under age 65 can qualify for home dialysis, and services will be covered by Medicare from the first month of treatment.
There are three requirements for home dialysis:
The beneficiary takes part in a home dialysis training program in a Medicare-approved training facility
The beneficiary begins training before the third month of dialysis treatments
The beneficiary expects to do dialysis treatments in the home
The Adoption Of Section 299i
The formal legislative history of Section 299I is quite brief. The provision was not considered by the House Ways and Means Committee in hearings or in any executive session on H.R. 1. The Senate kidney amendment was added to H.R. 1 on the Senate floor, with no prior hearings, on a Saturday morning, September 30, 1972. The joint House-Senate conference committee agreed to the Senate amendment barely two weeks later. On October 30, the brief kidney provision was included in the 300-page bill signed by the President. The informal legislative history, however, is far more complicated.
Ways and Means: November and December 1971
The House Ways and Means Committee, as part of its hearings on national health insurance, devoted the end of the morning of November 4, 1971, to testimony about ESRD . It particular, it heard from representatives of the National Association of Patients on Hemodialysis . These included Shep Glazer, vice president of the group and a dialysis patient from New York William Litchfield, a dialysis patient from Houston Roland Fortier, an NAPH member from Connecticut Peter Lundin, a medical school student who was also a dialysis patient and NAPH member from California June Crowley, a dialysis patient from New York and Abraham Holtz, a dialysis patient from New York.
Glazer made an official statement for NAPH, and then spoke about his personal situation:
Senate Finance Committee: 1972
The Joint House-Senate Conference Committee: 1972
You May Like: How To Apply For Medicare By Phone
Does Medicare Cover Kidney Transplants
Original Medicare Parts A and B cover some of the costs for kidney transplants. Your costs may differ if you are enrolled in a Medicare Advantage plan.
Generally, youll have to pay the regular out-of-pocket Medicare costs associated with Medicare Part A and Part B. This includes coinsurance or copayments and deductibles.
Under Medicare Part B, that means youll have to pay your deductible and 20% of the Medicare-approved amount. Medicare will pick up the other 80%.
Your doctor is limited in how much they can charge if they dont accept Medicare. If your doctor does not take assignment, you are limited to paying 15% above the Medicare-approved cost for your services.
Medicare will pay for laboratory tests and will help you pay for blood services necessary for your transplant. You will be responsible for paying for the first three units of blood.
Your deductible and a copayment will apply to the rest. You can replace the blood with blood donations, either your own or from people you know or are related to.
Does Medicare Cover Transportation To Dialysis
Medicare typically does not cover transportation to a dialysis facility. The only caveat to this rule would be if you qualified for ambulance services and were transported to a facility in an ambulance.
Ambulance services are covered when you need to get to a hospital or other facility and transportation in a normal vehicle could be life threatening. Some Medicare Advantage plans offer expanded coverage for transportation to facilities.
Don’t Leave Your Health to Chance
Recommended Reading: What Is Medicare Id Number
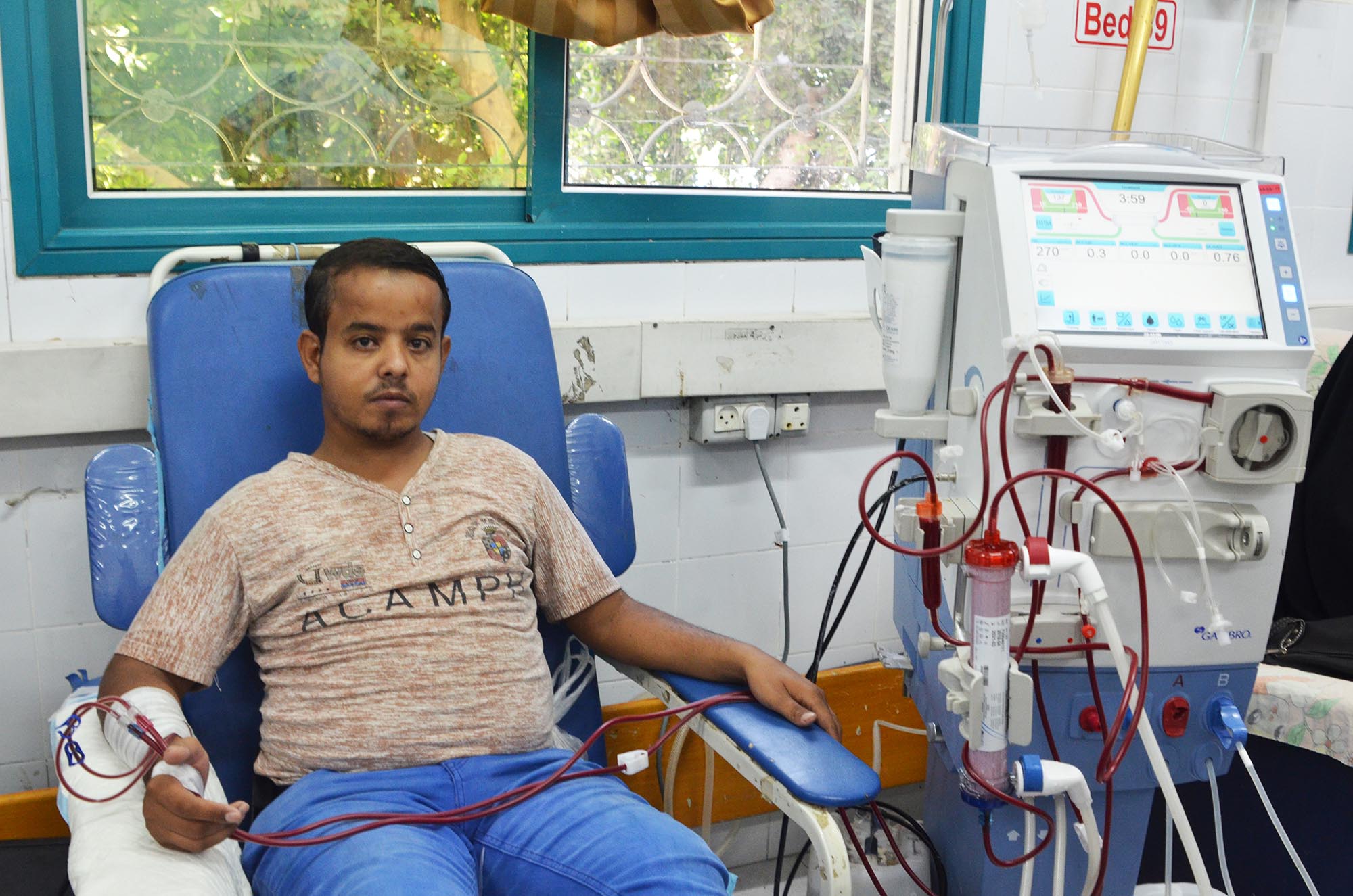
What Is Renal Disease
Renal disease, also known as end-stage kidney failure, occurs when the kidneys in the human body no longer work effectively and are not filtering the blood as they should.
This condition worsens over time and can be caused by a variety of chronic renal illnesses, but the final result is always the same: the patient requires dialysis to filter the blood and have a chance of recovery or a new organ transplant.
Hemodialysis is a hard and costly procedure that requires a lot of time and effort from the patient, but most importantly, a lot of money. This is why individuals frequently inquire if Medicaid covers dialysis costs and how to find out.
Continue reading to find out all the information.
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
- Kidney transplants
- Outpatient dialysis from a Medicare-certified hospital or dialysis facility
- Immunosuppressant drugs after a kidney transplant
- Home dialysis training from a dialysis facility
Recommended Reading: When Are You Eligible For Medicare Part A
If Youre Getting A Kidney Transplant
If youre admitted to a Medicare-certified hospital for a kidney transplant and the transplant takes place that month or in the next 2 months, Medicare can begin that month.
Medicare coverage can begin 2 months before your transplant if the transplant is delayed more than 2 months after being admitted to the hospital.
If youre only eligible for Medicare due to permanent kidney failure, your coverage will stop:
- 12 months after the month dialysis treatments are stopped
- 36 months following the month you have a kidney transplant
Medicare coverage will resume if:
- within 12 months after the month, you stop getting dialysis, you start dialysis again or have a kidney transplant
- within 36 months after the month you get a kidney transplant you get another kidney transplant or start dialysis
Eligibility For Part C
Starting in 2021, people with ESRD are eligible to enroll in a broader range of Medicare Advantage plans.
If you want to switch from original Medicare to a Medicare Advantage plan, you will be able to do so during the annual open enrollment period, which takes place from .
If you currently have a Medicare Advantage Special Needs Plan but want to switch to a different type of plan, you can do this during Medicare Advantage open enrollmentfrom .
Read Also: Can You Get Medicare If You Retire At 62
How Much Does Medicare Pay For Dialysis
Just one year of hemodialysis may cost you $72,000. And a single year of peritoneal dialysis can cost you around $53,000 each year.
Keep in mind, Medicare will only cover 80%, youll be left with the remaining costs. Even with the majority of your treatment covered, youll still have costly bills.
Get A Free Quote
Find the most affordable Medicare Plan in your area
You can opt into buying a Medigap plan, or Advantage policy. If youre on costly medications, a Part D drug plan can help lower your costs.
How Is Medicare Advantage Different From Original Medicare
Original Medicare plans cover different areas of healthcare:
- Part A covers inpatient hospital care, hospice, some nursing home care, and home healthcare.
- Part B covers all outpatient care, including dialysis services, doctor visits, and certain medications, including some for dialysis or kidney transplants.
- Part D helps with prescription costs not covered by Part B.
For the most complete coverage available under Original Medicare, you must sign up for Parts A, B, and D.By comparison, Medicare Advantage can offer all-in-one plans with all the benefits of Parts A, B, and Dplus more. Medicare Advantage plans are often easier to manageyou have coverage benefits in 1 plan instead of several, and the convenience of only 1 insurance card. Other ways Medicare Advantage differs from Original Medicare include:
- Annual out-of-pocket expenses are capped, lowering overall costs. Note: Its important to make sure you understand out-of-pocket costs on the plan you choose.
- Plans are managed by private health insurance companies approved by Medicare.
- Extra benefits are available, including dental, vision, hearing, and transportation.
- Medications for dialysis or post-kidney transplant are often covered, however, its important to make sure your medications are included in the plan you choose.
- Plans use networks, like employer group health plans, so its important to make sure your nephrologist and other doctors are in-network.
- Monthly premiums are lowmany as low as $0.
Read Also: Does Medicare Pay For Cialis
Another Coverage Choice If You Have Esrd
You might be eligible for a Special Needs Plan, a specific type of Medicare Advantage plan that targets individuals who live in an institution, have Medicaid, or have certain chronic conditions . These plans include prescription drug coverage as part of the plan, and a Chronic-Condition Special Needs Plan for people with ESRD may also cover certain services to help you manage your condition. If there is a Special Needs Plan for beneficiaries with end-stage renal disease in your area, you may be able to enroll and get your Medicare benefits that way.
Read Also: Can Chocolate Cause Kidney Stones
Who Qualifies For Medicare Parts A And B
Your become eligible for Medicare in one of three ways:
-
When you reach age 65
-
If you have a disability
-
You become disabled with permanent kidney failure or amyotrophic lateral sclerosis
Medicare is divided into several different parts: Part A covers costs related to hospitalization, while Part B covers expenses related to visits to your healthcare providers as well as any other care you receive as an outpatient.
Also Check: How Does Medicare Work When You Turn 65
Medicare Advantage Dialysis Coverage
As of January 2021, people with ESRD can join a Medicare Advantage planMedicare Advantage , also known as Medicare Part C, are health plans from private insurance companies that are available to people eligible for Original Medicare â¦.. Previously, only Original MedicareOriginal Medicare is private fee-for-service health insurance for people on Medicare. It has two parts. Part A is hospital coverage. Part B is medical coverageâ¦. was available to people diagnosed with ESRD. Special Needs Plans may be available in some areas to address the specific needs of ESRD patients. SNP-C plans are customized to the particular needs of their covered condition, providing benefits and additional services that go beyond what Medicare usually covers, which can include:Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
- A care team of specialists for the special condition
- A case coordinator to optimize the coordination of services you need
- Extra hospital days
- Drug coverage formularies tailored to your condition
These benefits may not be available for every Medicare Advantage SNP. Ask your local Medicare Advantage providers about which SNPs they offer and what benefits they provide.Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
How Do You Apply For Medicare Parts A And B
Youre first eligible to sign up for Medicare 3 months before you turn age 65 or earlier, if you have a disability, ESRD, or ALS. After you turn 65, you can sign up for Medicare Part A with or without Part B. You have a 7-month window for Medicare Part A enrollment that begins 3 months before you turn 65, includes your birth month, and ends 3 months after you turn 65.
If you already receive Social Security retirement or disability benefits at the time you turn 65, you are usually automatically enrolled in Medicare Part A and Part B.
The fall open enrollment is the time period when Medicare beneficiaries and those enrolling can make the most changes to their coverage. Its open to everyone eligible for Medicare every year from . You can enroll in Medicare by visiting its website and following the instructions.
Read Also: What Is Medicare Extra Help
Esrd Medicare Coverage For Prescription Drugs
After someone becomes eligible for ESRD Medicare, they can enroll in a Medicare drug plan during a seven-month period. This seven-month period begins three months prior to the first month they are eligible for Medicare. It will end three months following the first month theyre eligible.
Prescription drug coverage begins at the same time as Medicare coverage. It may also start the first month after a request is sent, whichever date is later.
Finally, Medicare Part B will pay for most of the drugs needed for dialysis, though it wont cover prescription medication for other health conditions. In this scenario, patients would need to enroll in Medicare Part D, which is prescription drug coverage.
I Have Private Insurance Through The Affordable Care Act
- You do not need to apply for Medicare at any time unless you choose to. If you choose to apply for Medicare, and your private insurance plan is through the Affordable Care Act, you will lose your private plan coverage. This is because Affordable Care Act insurance plans are for people who no other insurance options. Once you have Medicare, you are considered to have other coverage and would no longer qualify for coverage through the Affordable Care Act.
Recommended Reading: Can Grape Juice Change Urine Color
Read Also: How Much Does Medicare Pay For A Doctors Office Visit
