Types Of Pain Management Injections
- SIJ Injections: These are therapeutic injections where cortisone goes directly into the joint through the needle.
- Lumbar Facet Injections: These are therapeutic injections where cortisone goes directly into the joints from a needle.
- Lumbar Medial Branch Blocks: Diagnostic procedure in which Lidocaine tests the joints nerve endings verifying one responds with pain relief. Doctors hit the correct nerve when the patient feels relief, making them a candidate for a Radiofrequency Ablation.
- Radiofrequency Ablation or RFA: Therapeutic procedure where nerve findings come from the Medial Branch Blocks these nerves then receive cauterization for long-lasting relief.
- Lumbar Epidural Steroid Injection: Therapeutic injection where cortisone goes around the hurt disc and nerve endings for pain relief.
Who Qualifies For Cervical Disc Replacement
If you live in an area where cervical disc replacement is approved under the local coverage determination, all the following statements must be true for the procedure to be covered:
- The disc being used is approved by the FDA
- Youre considered to be skeletally mature this typically applies to anyone over the age of 25
- Youve either been experiencing pain that isnt relieved through over-the-counter medications and physical therapy for at least six weeks or your symptoms are progressing rapidly and the procedure is considered urgent
- Youve undergone a CT scan, an MRI or myelography to diagnose your condition
- The damaged disc is in the right location on your spine
If you have certain medical conditions or have previously undergone back surgery, you may be ineligible for Medicare coverage even in areas where the procedure is approved.
Recommended Reading: Does Medicare Pay For Licensed Professional Counselors
Is Disc Replacement Surgery Painful
There is usually some pain and discomfort in the days and weeks following cervical artificial disc replacement surgery. Most commonly, the recovering patient has some pain and soreness at the incision site at the front of the neck. Other symptoms may also be present, such as trouble with swallowing or speaking.
Read Also: What Part Of Medicare Covers Dental
Lumbar Partial Disc Prosthetics
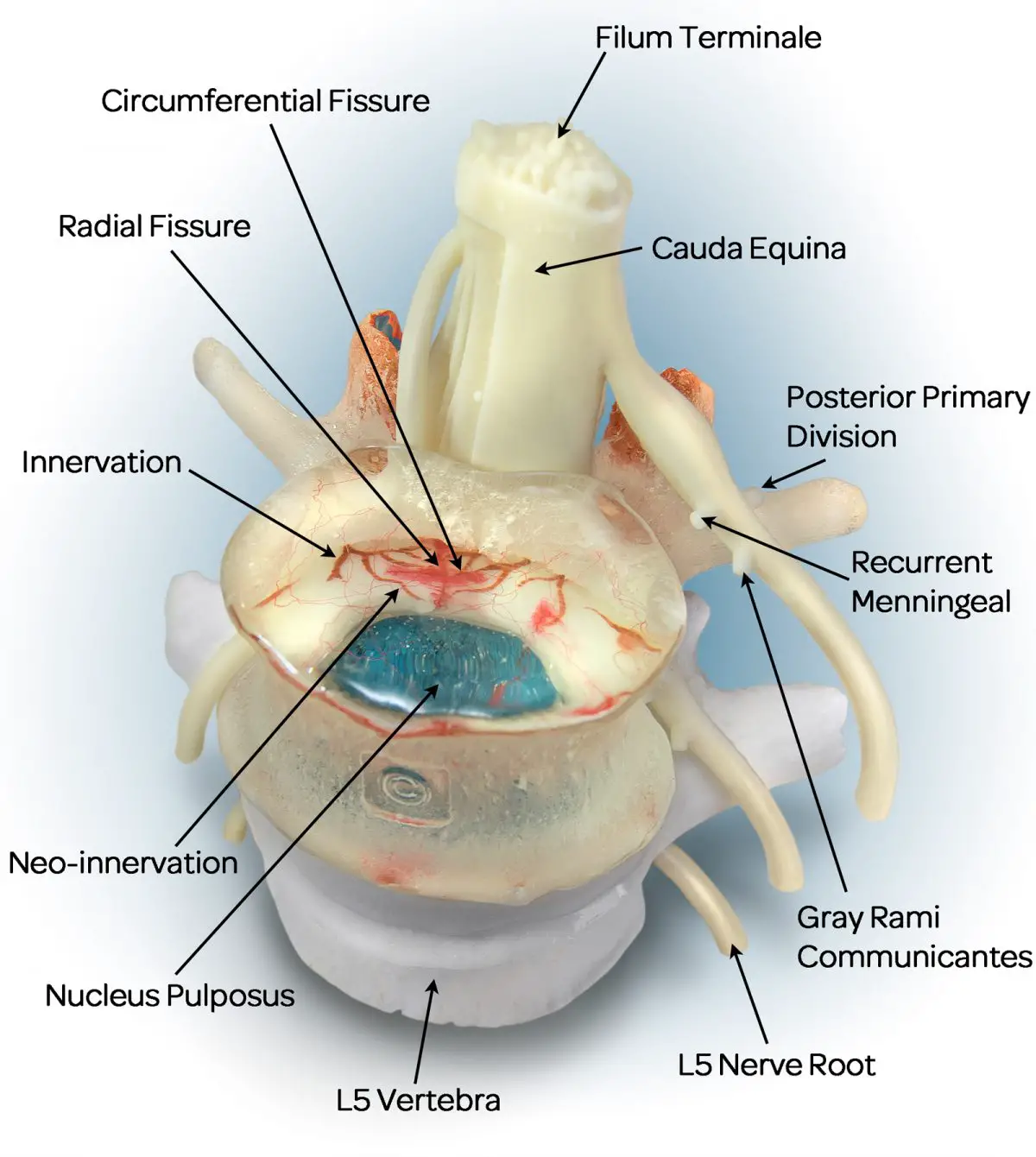
Lumbar partial disc replacement is a minimally invasive procedure that replaces only the nucleus pulposus in an attempt to fill the therapy gap between discectomy and fusion. The procedure targets only the nucleus pulposus as the origin of pain while attempting to restore the biomechanical function of the whole segment. Careful patient selection is crucial since the prosthetic nucleus is not fixed into position. An intact annulus and properly functioning endplates must be present. Exclusion criteria include osteoporosis, endplate problems, posterior element disorder , and infection tumors. There are several lumbar partial disc replacement devices currently under investigation. These devices use hydrogel, polymer/synthetic, or mechanical technologies, however, none are commercially available in the United States. All non-fusion spinal implants are considered Class III medical devices and require Pre-Market Approval from the FDA prior to market release in the United States.
Further clinical investigation with well-designed prospective, randomized trials is needed to determine the efficacy of nucleus replacement in the treatment of lumbar DDD, as well as its ideal indications.
You May Need Other Insurance
After surgery, your back will likely feel stiff and sore. It may be hard for you to sit or stand in one position for a long time and may need pain medication in the weeks following your surgery. It could take four to six weeks to return to simple activities, and it usually takes a few months for the bones to heal well.
While you recover, should you need prescription meds, think about getting additional insurance like a Part C or Part D plan to avoid paying high out-of-pocket costs. Medicare Supplement policies are also available when youre eligible for Medicare.
Also Check: What Is Aarp Medicare Supplement
Medicare Benefits For Back Surgery
If you have surgery in the hospital, Part A Medicare benefits cover your:
- Semi-private room
- General nursing services
- Necessary medication and other supplies
- Inpatient rehabilitation care if your doctor certifies you need intensive rehabilitation, your doctors oversight and coordinated care
You are responsible for the Part A deductible . If you require an inpatient stay beyond 60 days, you are responsible for coinsurance, starting at $389 per day.
Part B Medicare benefits cover:
- Hospital outpatient diagnostic and treatment services
- Outpatient surgery, X-rays and casts
- Physical therapy
- Your doctors services, whether you are an inpatient or outpatient
- Second surgical opinion
Your share of the cost is the Part B deductible and 20% coinsurance. If you use the services of a hospital outpatient department, the facility can charge you a copayment.
Use your Part D Medicare benefits for any medications your doctor prescribes to mitigate your pain or facilitate your recovery. Part D plans vary, so make sure that medications prescribed are included in your plans formulary or list of covered drugs.
TIP: Are you looking for help choosing a new health insurance plan? Try our handy Medicare plan finder tool that lets you compare different plans side-by-side.
Find a new plan
Get recommendations based on what’s important to you, and compare them to your existing plan.
Lumbar Spinal Fusion For Instability And Degenerative Disc Conditions
L33382
CPT codes, descriptions and other data only are copyright 2021 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT, and the AMA is notrecommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services.The AMA assumes no liability for data contained or not contained herein.
Current Dental Terminology & copy 2021 American Dental Association. All rights reserved.
Don’t Miss: Will Medicare Help Pay For A Walk In Shower
Getting Your Back Pain Treatment Covered By Medicare
As mentioned above, there are many back pain treatment options available and how Medicare may cover each varies. When considering a back pain treatment option, keep the following in mind:
When it comes to getting Medicare to cover back pain treatments, its paramount you speak with the physician providing your back pain treatment, Medicare, and your Medicare plan provider if you have a Medicare Advantage or Part D plan.
Tips For Preventing Back Pain
The National Spine Health Foundation offers these suggestions for avoiding back and neck pain:
- Maintain good posture so that your spine is aligned correctly.
- Learn about workplace ergonomics, so you can protect your back and neck when you work in an office.
- Practice safe lifting to reduce stress on your back.
- Try relaxation exercises to lower your overall stress level.
- Find the best sleeping position for your back.
- Be aware that smoking impacts your bone density, connective tissues and spinal health.
- Follow healthy behaviors for proper nutrition and weight management.
- Exercise to help prevent back pain and hasten recovery if the pain does develop.
TIP: for additional information on back pain, check out our companion blog on laser spine surgery.
MULTIPLAN_HCIMB35CBS_2022
You May Like: How Do Zero Premium Medicare Plans Work
Using Medicare Advantage Benefits
Medicare Advantage Plans are provided by private insurance companies, and they often provide you with extra coverage that’s not included with Medicare Part A and Part B. Depending on your coverage, you may be eligible for assistance with some of your out-of-pocket expenses, including your deductible or coinsurance payments. To determine what you’re covered for, it’s best to contact your Medicare Advantage Plan provider.
Medicare Coverage For Pain Management Injections
Usually, Medicare covers pain management injections when theyre determined to be medically necessary. Suppose youre receiving an injection during an inpatient stay at a hospital. In that case, it will receive coverage from Part A. If your doctor administers the procedure in an outpatient setting, Part B covers the injection.
Find Medicare Plans in 3 Easy Steps
We can help find the right Medicare plans for you today
Don’t Miss: What Is The Deadline For Medicare Open Enrollment
Laminectomy With Instrumented Fusion Versus Laminoplasty For The Treatment Of Multilevel Cervical Spondylotic Myelopathy
The authors stated that this review had several drawbacks. First, only 1 of the included studies was a RCT. Second, there was variability in choosing the indicators to evaluate clinical outcomes between the included studies, indicating a lack of standard outcome measurements. Third, the length of follow-up varied between studies, and this was important for surgical outcome evaluations. Finally, clinical heterogeneity might be caused by the various indications for operations.
The authors stated that this meta-analysis had several drawbacks. First, in most the studies selected were not RCT, while it did not influence the credibility of the results. Second, laminoplasty had different techniques, such as open door and French door and these differences were not considered. Third, the current research has not been registered and there may be some small bias, but these investigators still followed the steps of system evaluation strictly. Finally, clinical heterogeneity might be caused by the various indications for surgery and the surgical technologies used at the different treatment centers.
Learn More About Medicare

Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
| TTY 711, 24/7
This means if you spend a certain dollar amount out of pocket for your back surgery, your plan will pay 100 percent of the cost for covered services that go beyond the annual out-of-pocket limit. If you only have Original Medicare, there’s no limit to the amount of spending you may have to pay for your back surgery.
Also Check: Is Accu Chek Covered By Medicare
Laminectomy For Tarlov Cysts
Seo and colleagues noted that Tarlov cysts are lesions of the nerve root that are often observed in the sacral area. There is debate regarding whether symptomatic TCs should be treated surgically. These researchers presented the findings of 3 patients with symptomatic TCs who were treated surgically, and introduced sacral re-capping laminectomy. Patients complained of low back pain and hypesthesia on lower extremities . These investigators operated with sacral re-capping technique for all 3 patients. The outcome measure was baseline visual analog scale score and post-operative follow-up magnetic resonance images . All patients were completely relieved of symptoms following operation. The authors concluded that although not sufficient to address controversies, the findings of this small case series introduced successful use of a particular surgical technique to treat sacral TC, with resolution of most symptoms and no sequelae.
Does Medicare Cover Radiofrequency Ablation
When a doctor deems RFA medically necessary, it gets coverage. To determine this, you may need to prove that other methods werent successful in managing your pain. You could be responsible for a copayment, deductible, or coinsurance. If you have a Medicare Advantage plan, costs may vary, so contact your plan for details.
You May Like: Are Cancer Drugs Covered By Medicare
Laser Spine Surgery Performed By Experts
Dr. St. Louis, the surgical founder of Laser Spine Institute in Tampa, Fla., joined PPOA in January. Phillip Kravetz, M.D., another pioneer in the field, will perform these procedures in Texas.
Minimally invasive laser spine procedures are fast becoming the gold standard for addressing severe spine-related pain. Minimally invasive refers to the small incision and tiny instruments used to perform a procedure. Narrow dilation tubes are fed through the incision to spread the muscles surrounding the back. In contrast, traditional open back surgery uses a five- to six-inch incision. Through this a surgeon must cut and tear muscles to reach the spine.
The laser is mainly used for ablations and disc work.
Laser spine surgery isnt the only way PPOA ensures a good patient outcome. Its surgeons also use intraoperative neuromonitoring to further ensure safety of the patients neural system during the operation. IONM can see what neither the doctor nor the fluoroscopy machine can, and it helps avoid accidental injury.
The methods used in PPOAs minimally invasive laser spine surgery allow for a totally outpatient procedure. Most patients are able to walk out of the surgery center the same day, and resume activities in days or weeks, as opposed to months with traditional surgery.
Conservative Management For Lbp Includes
- Avoidance of activities that aggravate pain
- Chiropractic manipulation in the first 4 weeks if there is no radiculopathy
- Cognitive support and reassurance that recovery is expected
- Education regarding spine biomechanics
- Heat/cold modalities for home use
- Limited bed rest with gradual return to normal activities
- Low impact exercise as tolerated
- Pharmacotherapy , avoid muscle relaxants, or only use during the first week, avoid narcotics)
- Physical therapy
In the American Pain Society/American College of Physicians Clinical Practice Guideline on “Nonpharmacologic Therapies for Acute and Chronic Low Back Pain,” Chou and Huffman reached the following conclusions: “Therapies with good evidence of moderate efficacy for chronic or subacute low back pain are cognitive-behavioral therapy, exercise, spinal manipulation, and interdisciplinary rehabilitation. For acute low back pain, the only therapy with good evidence of efficacy is superficial heat.”
The APS guideline stated that, in patients with chronic non-radicular LBP, provocative discography is not recommended as a procedure for diagnosing LBP .
In patients with non-radicular LBP who do not respond to usual, non-interdisciplinary interventions, the APS guideline recommended that clinicians consider intensive interdisciplinary rehabilitation with a cognitive/behavioral emphasis .
- Any high-grade slip
- Iatrogenic spondylolisthesis
Also Check: Does Medicare Part D Cover Shingrix Vaccine
Medicare Advantage Plans Cover Back Surgery And May Offer Additional Benefits
A Medicare Advantage plan is sold by a private insurance company and provides the benefits of Medicare Part A and Part B into one single plan.
Some Medicare Advantage plans may also offer additional benefits not covered by Original Medicare, which can include some costs savings if your plan will cover more of your out-of-pocket costs for back surgery.
Explore Medicare Advantage plan benefits in your area
Or call to speak with a licensed insurance agent. We accept calls 24/7!
1 Smith, J.C., MA, DC. Back Surgery: Too Many, Too Costly and Too Ineffective. . To Your Health. Retrieved from www.toyourhealth.com/mpacms/tyh/article.php?id=1447.
2 Laser Spine Institute. Common Questions. Retrieved from www.laserspineinstitute.com/patient-process/spine-back-questions.
About the author
Christian Worstell is a senior Medicare and health insurance writer with MedicareAdvantage.com. He is also a licensed health insurance agent. Christian is well-known in the insurance industry for the thousands of educational articles hes written, helping Americans better understand their health insurance and Medicare coverage.
Christians work as a Medicare expert has appeared in several top-tier and trade news outlets including Forbes, MarketWatch, WebMD and Yahoo! Finance.
A current resident of Raleigh, Christian is a graduate of Shippensburg University with a bachelors degree in journalism.
Medicare has neither reviewed nor endorsed this information.
What Are The Risks Of Cervical Disk Replacement Surgery
While any surgery carries some risk, disk replacement surgery is a relatively safe procedure. Before you have surgery, you will need to sign a consent form that explains the risks and benefits of the surgery.
Disk replacement is a new type of spine surgery so there is little information on possible long-term risks and outcomes. Discuss with your surgeon the risks and benefits of disk replacement surgery compared with more traditional types of cervical spine surgery.
Some potential risks of cervical spine surgery include:
-
Reactions to the anesthesia
-
Broken or loosened artificial disk
-
Need for further surgery
There may be other risks, depending on your specific medical condition. Be sure to discuss any concerns with your surgeon before the procedure.
You May Like: Do I Need Supplemental Health Insurance With Medicare
Does Medicare Cover Laser Spine Surgery
Medicare may help pay for laser spine surgery if it is medically necessary. However, it may not help pay for facility fees only doctor and procedure fees.2
Laser spine surgery is a minimally invasive alternative to traditional back surgery. A doctor will make a small incision and use a laser or another type of instrument to treat the problem area. It may be effective for certain spinal conditions, but some patients may not be good candidates for the procedure.
Medicare Coverage For Lower Back Pain Treatment Options

There are many treatment options, including:
- Injection Based Treatments
- Surgical Intervention
While some individuals may require surgery, others consider it a last resort. Theres no guarantee that surgery will provide pain relief. Unless an orthopedic or neurosurgeon can guarantee over 50% improvement, you want to avoid surgery at all costs.
Also, any surgery with the lumbar spine includes the risk of complications. You want to consider surgery as a very last resort. Meaning you have tried all traditional treatments, including interventional pain management, and theyve failed.
Medicare will cover lower back surgery when its medically necessary. Well go over coverage for the treatments you should seek before you resort to surgery to help your lower back pain.
Don’t Miss: Does Medicare Pay For Assistance At Home
How Does Back Surgery Coverage Vary Between States
A 2019 study by Dr. David S. Casper at Thomas Jefferson University Hospital in Philadelphia looked at the variation of Medicaid reimbursement for common spinal surgeries in many states. It revealed that across 43 states Medicaid paid an average of only 78% of what Medicare paid for the same spinal surgeries.
However, from one state to the next, the payment for back surgery varied greatly. Medicaid payment was significantly low in Florida, New Jersey, New York and Rhode Island. In only four states Alaska, Arkansas, Nebraska and South Dakota Medicaid actually paid more than Medicare did.
The variation of payment may make it more difficult for Medicaid enrollees to get the back surgery they need in some states. When physicians receive low reimbursement for their services from Medicaid, they are less likely to be willing to take Medicaid enrollees.
Is Minimally Invasive Spine Surgery Covered By Insurance
If you suffer from back pain, chances are you want to explore treatment options. Whereas some back pain may be fixed with physical therapy or medication, some issues must be treated surgically. Surgery can be costly, so researching your options will be imperative.
While traditional surgery may be a viable option for some patients, minimally invasive surgery is also an attractive option. This procedure boasts afaster recovery, less pain, and only a small incision. It may seem like the obvious choice, but only a handful of doctors are skilled enough to practice this form of surgery. Dr. Hanson is the only orthopedic spine surgeon in Minnesota to perform endoscopic hemilaminectomies, foraminotomies, microdiscectomies and nerve transections.
Minimally invasive spine surgery is performed with many different surgical implements, including lasers, endoscopes, computer-assisted navigation systems, and operating microscopes. This allows the procedure to be performed through a small incision. The decision to use a specific technology is based on the needs of the patient.
Luckily, most insurance plans should cover minimally invasive spine surgery.
Spine surgery is only performed to treat an actual medical condition. Because it is not a cosmetic procedure, insurance companies should cover the cost of spine surgery as long as a doctor determines it is medically necessary and the patient has completed the conservative care requirements set by their specific insurance.
Don’t Miss: How To Get A Medicare Number As A Provider
