What Is A Cpap Machine
If you have OSA, continuous positive airway pressure machines, opens new window are one of the most common treatments. A CPAP machine is a device with a face or nose mask attached to a small pump. The pump pushes pressurized air through a hose, into the mask and into your airway. The steady flow of air keeps the airway open to improve breathing and sleep quality. Some people may require extra CPAP supplies like humidifiers and heating tubes for effective treatment.3
Get A Second Clinical Evaluation
If Medicare covers your CPAP machine for the three-month trial period, you must undergo a second clinical evaluation to establish medical necessity for continued coverage. During the face-to-face evaluation, your doctor must document that your symptoms of sleep apnea have improved and that youve adhered to consistent CPAP therapy.
If you fail the initial 12-week trial period, youre eligible to requalify for a CPAP device by taking an in-person clinical re-evaluation and repeating the sleep test in a facility-based setting.
Does Medicare Pay For Cpap Machines And Supplies
Many or all of the products featured here are from our partners who compensate us. This may influence which products we write about and where and how the product appears on a page. However, this does not influence our evaluations. Our opinions are our own. Here is a list ofour partnersandhere’s how we make money.
Medicare pays most costs of CPAP, a common therapy for people with obstructive sleep apnea, or OSA. To get coverage, youll need a physician to prescribe a CPAP machine based on tests including a sleep study showing that you have OSA.
OSA, which afflicts 25 million adults in the United States, is a serious condition that, in addition to disturbing your sleep, increases the risk of cardiovascular disease, diabetes and depression. A CPAP machine provides continuous positive airway pressure via a mask to keep your upper airway clear for easier breathing, better sleep and improved overall health.
You May Like: Is Ed Medication Covered By Medicare
How Do You Treat Sleep Apnea
Mild cases of sleep apnea are often managed through simple lifestyle changes such as quitting smoking, losing weight or treating nasal allergies. For individuals who have a moderate or severe case of sleep apnea, treatment may be more complex, and can include supplemental oxygen, oral appliances or airway-pressure devices, including CPAP machines. Treatment for sleep apnea may also involve therapies for related medical conditions such as neuromuscular disorders.
What Are Medicare Guidelines For Cpap

You have a three-month trial period covered by Medicare. After three months, your doctor will check how the treatment is working for you. Medicare may cover CPAP therapy long-term if your doctor verifies in your medical record that:
- You are using the machine
- The therapy is helping you.
Remember, getting a prescription for a CPAP machine depends on a sleep studys results to determine if you have obstructive sleep apnea. Does Medicare cover sleep study testing and equipment? Yes, Medicare Part B covers the tests youll need to see if youre eligible for CPAP coverage.
Don’t Miss: What Are Medicare Part Abcd
Option : Use Medicares Website
If you have a Medicarehealthcare plan, you can also find in-network durable medical equipment providers by using Medicares Supplier Directory. After you click the link, enter your zipcode and select the corresponding product category. For CPAP machines and related supplies, select . After you click the search button, the website will provide you with a list of vendors in your area that provides CPAP equipment and accepts Medicare insurance.
For the lucky few of you, you may be able to find a MedicareDME provider that is relatively close to you however, for others, the drive from your home could be long and inconvenient. Luckily, Health Sqyre will ship your desired CPAP products right to your door!
When Should I Contact My Private Insurance
Once you think you have sleep apnea, check with your insurance company to find out what type of coverage you get for CPAP.
However, it is essential that you focus on the machine, mask, and accessories which best meet your therapy and comfort needs. We will encourage you to try different options in order to find the solution that works for your therapy needs and your budget.
VitalAire does not typically bill your insurance company directly because of privacy policy that protects your information, but we can provide any information wherever you need it
You May Like: Is Dental Care Included In Medicare
Insurance And Cpap Machines
The terms of your CPAP machine, insurance coverage depends on your provider. Some providers reimburse you for the cost of purchasing the machine outright, while others require a rent-to-own plan under which you must use the machine for a set amount of time before it becomes your property.
Costs for purchasing a machine outright can range anywhere from $250 to $1,000 or more, depending on where you live and the type of machine you need. Most CPAP machines cost between $500 and $800. BiPAP machines, which provide a different level of air pressure for exhalation and inhalation, frequently run in the thousands of dollars.
If you are on a rent-to-own structure, your monthly fee typically equals the cost of the CPAP machine divided by the number of rental months. Your insurance provider usually splits this cost with you, and the exact amount you pay depends on your policy. Bear in mind that if you are required to rent for longer than a year, you may need to pay a second deductible.
If your insurance company determines you are not using the machine frequently enough as per your policy, they may stop covering their portion of the machine rental. You must decide if you prefer to pay the full cost of the monthly rental, purchase the machine outright, or stop CPAP treatment altogether.
Does Medicare Part B Cover Cpap Supplies
Yes, Medicare Part B covers CPAP supplies. Medicare covers your CPAP supplies at 80% after you meet your deductible, much like CPAP machines. CPAP supplies can include tubing, filters and face masks. As with the coinsurance on CPAP machines, Medigap may help cover your out-of-pocket costs if you have Original Medicare.
Although Medicare Advantage offers the same coverage and benefits as Parts A and B, your plan may charge a different amount for Medicare CPAP supplies. To find out what youll pay, .
Read Also: What Is The Best Medicare Advantage Plan In Washington State
Where Do I Pay For My Machine
You must receive the CPAP machine through one of the WRHA contracted vendors Medigas or VitalAire. The $500 payment will be made directly to the vendor of the equipment. You will make arrangements directly with the vendor for payment. The vendor will work with WRHA to receive the remainder of the payment.
Sleep Apnea And Medicare
Navigating coverage for sleep apnea can be tricky, but luckily, Medicare often picks up a majority of the cost. If youre diagnosed with obstructive sleep apnea, you may qualify for CPAP therapy, including routine accessories for your CPAP machine.
If you already have sleep apnea and are considering a backup oxygen concentrator, there are plenty of affordable oxygen concentrators to consider. While there may be certain restrictions and requirements for Medicare coverage of your CPAP machine, it will definitely offer some form of assistance.
To learn more about Medicare coverage, check out our helpful guides:
You May Like: What Is Medicare Ffs Program
Motorcycle Vs Car Insurance
Category: Insurance 1. Does a Motorcycle or Car Have Cheaper Insurance Rates Generally speaking, motorcycle insurance is cheaper than car insurance. There are exceptions, though. Depending on the state that you live in and the value of Feb 18, 2021 Does car or motorcycle insurance cost more? Car
How Often Can You Get A New Cpap Machine Under Medicare
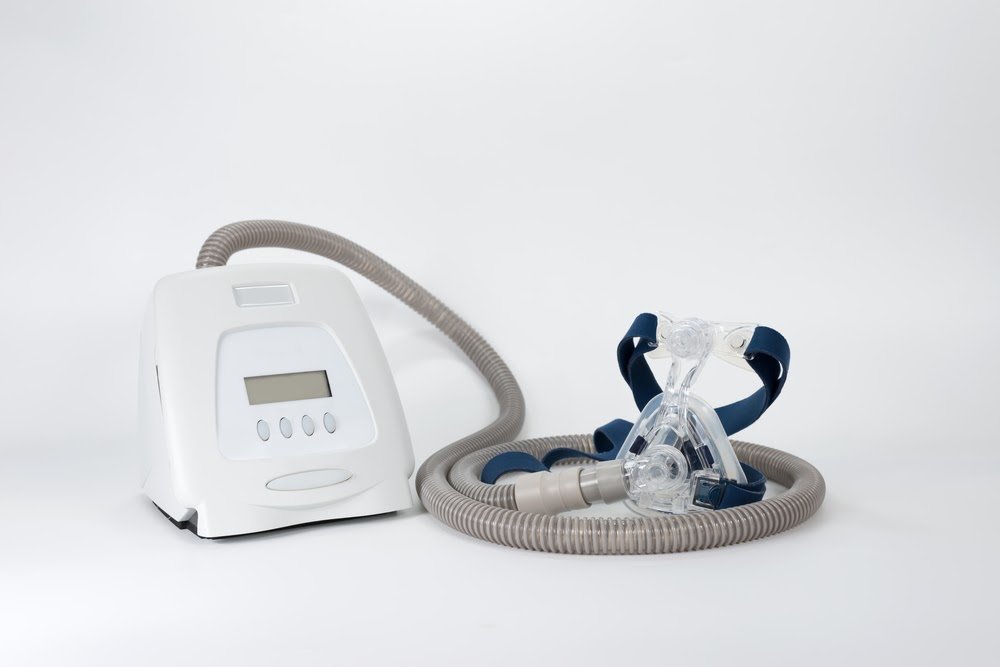
CPAP machines are used to deliver constant, steady air pressure to patients with obstructive sleep apnea while they are sleeping. Sleep apnea is a medical condition that causes pauses in breathing during sleep.
Medicare does cover CPAP machines if you are diagnosed with sleep apnea. Medicare Part B may cover a 3-month trial of CPAP therapy.
If the CPAP therapy is successful, your doctor may be able to extend the treatment and Medicare will cover it. If you rent a CPAP machine for 13 months, you own it.
Medicare Part B is usually responsible for covering durable medical equipment like CPAP machines.
Don’t Miss: What Weight Loss Programs Are Covered By Medicare
Does Medicare Pay For A New Cpap Machine
Yes, but there are stipulations. Medicare will usually help cover the cost of renting a CPAP machine for 13 months. If you use it without interruption throughout that time, youll own it at the end of the term. Talk to your doctor if your CPAP machine breaks or you need a new one. If its old enough or meets other guidelines, Medicare may pay for a new CPAP machine.
What extra benefits and savings do you qualify for?
Does Original Medicare Cover Cpap Supplies
Yes. Original Medicare helps pay 80% of the cost of the following equipment after youve met your Part B deductible:6
- CPAP machine rental for a 3-month trial if youre newly diagnosed
- CPAP rental for 13 months if youve been using it consistently
- Masks or nose pieces you wear when using the machine
- Tubing to connect the mask or nose piece to the machine
Original Medicare has certain rules for replacing CPAP machine supplies. Contact your doctor or device supplier for more information.
Note: Part B also helps pay up to 80% of the costs of your sleep study if you have clinical signs and symptoms of sleep apnea. Costs covered include Type I, II, III, and IV sleep studies and devices.7
Don’t Miss: Does Medicare Pay For A Caregiver In The Home
Does Medicare Cover The Sleep Apnea Test
Medicare can offer coverage for sleep studies. However, before treatment, there are specific requirements the patient must meet.
Part B of Medicare can cover a sleep study test if your doctor orders it, it is medically necessary to diagnose a condition such as sleep apnea, and sleep is recorded and staged. Medicare wont cove a sleep study for chronic insomnia.
Even with coverage, you may be responsible for some of the costs. If you have an Advantage plan, talk to your plan provider about in-network practitioners, coverage, and costs. Those with a Medigap policy may pay little to nothing out-of-pocket when receiving treatment.
People Are Also Reading
But even before you begin the trial, you must have a sleep test to determine that you meet the clinical criteria for obstructive sleep apnea. The good news is that if home sleep test equipment is available through a local physicians office or sleep clinic, you need not spend the night in a sleep lab.
Also Check: How Much Will Medicare Pay For Assisted Living
Will Medicare Cover A Cpap Machine
Medicare covers CPAP machines used to treat sleep apnea under the durable medical equipment benefit. To qualify for CPAP coverage, you must meet the following requirements:
- Complete a sleep test in a laboratory setting or by using an approved at-home test
- Be diagnosed with obstructive sleep apnea based on sleep test results
- Have a prescription for a CPAP machine from your doctor
- Get the CPAP machine from a participating Medicare supplier
Since CPAP treatment doesnt work for everyone, Medicare first covers the machine for a three-month trial period. After three months, your doctor will check how the treatment is working for you. Medicare may cover CPAP therapy long term if your doctor verifies in your medical record that you are using the machine and that its helping you.
Medigap And Cpap Machines
Medigap, also known as Medicare Supplemental Insurance, covers the gaps of Original Medicare and can provide additional coverage related to CPAP therapy. For instance, certain Medigap plans in tandem with Medicare coverage might be able to cover the full cost of CPAP machine rentals or accessories needed for the machine for your sleep apnea, as long as your physician certifies that it is medically necessary and is improving your health.
Pro Tip: There are currently 10 different types of Medigap plans offered by private insurers. To help you get started, read my list of affordable medicare supplement plans.
Don’t Miss: Does Medicare Cover Oral Surgery Biopsy
What Is A Cpap Cleaning Machine
Every time you use a CPAP you are required to clean it afterwards. That is because when your CPAP gets contaminated with various substances like germs and bacteria, you may inhale them. Inhaling germs, bacteria, and other foreign substances like molds will affect our respiratory and overall health and wellness.
That is what CPAP cleaning machines are made for. Their purpose is to clean the CPAP machines to prevent the user from getting sick. However, you dont necessarily have to buy a cleaning device to clean your CPAP machine.
You can clean the machine and detachable parts yourself using water and soap. The only advantage of having a cleaning machine is that you will not have to do it yourself.
What Is Medicare Cpap Compliance

Once you receive your CPAP or BiPAP equipment, youll begin a compliance period. Think of it like a three-month trial period. This is to demonstrate both that youre using your equipment and that its an effective treatment option for your OSA.
During the compliance period your doctor will monitor how often you use your CPAP. This is recorded by your CPAP device, either through an SD memory card or via Bluetooth connectivity.
To meet compliance, Medicare requires that you use your CPAP machine 1) at least 4 hours per night, 2) for at least 70% of nights, 3) for 30 consecutive days of the first three months.
That can be a little confusing, but what you need to know is: Use your CPAP machine for 30 days in a row, and at least 21 of those days need to be 4 hours or more per night.
Lastly, youll need to meet with your doctor between the 31st and 90th day of the compliance period!
Read Also: What Age Is For Medicare
Whats Covered Under Medicare For Cpap Therapy
Sleep Studies
Medicare Part B covers Type I, II, III, and IV sleep tests and devices if you have clinical signs and symptoms of sleep apnea.
CPAP Equipment
- and more visit
If your supplier accepts assignment you pay 20% of the Medicare-approved amount, and the Part B deductible applies.
Oxygen equipment & accessories
Medicare Part B covers the rental of oxygen equipment and accessories as durable medical equipment that your doctor prescribes for use in your home when all of these conditions are met:
- Your doctor says you have a severe lung disease or youre not getting enough oxygen and are in a chronic stable state.
- Your health might improve with oxygen therapy.
- Your blood oxygen level falls within a certain range.
- Other alternative measures have failed.
If you meet the conditions above, Medicare helps pay for:
- Systems that provide oxygen
- Tubing and related supplies for the delivery of oxygen and oxygen contents
You pay 20% of the Medicare-approved amount, and the Part B deductible applies.
Causes Of Sleep Apnea
The most common treatment for someone with moderate-to-severe sleep apnea is a breathing device, such as a CPAP machine. CPAP therapy delivers a flow of air through a mask to help keep the airway open while a person is asleep.
Other potential treatments for sleep apnea include:
- Oral appliance therapy: A person wears a custom-fitted mouthpiece that moves the tongue or jaw to help keep the airway open during sleep.
- Nerve stimulation: A surgeon inserts a device that stimulates the hypoglossal nerve, which goes to the tongue muscles, and helps move the tongue to a position that keeps the airway open.
- Positional therapy: A person who experiences sleep apnea only while sleeping on their back can learn to sleep on their side instead.
- Surgery: A doctor might recommend surgery for people with severe sleep apnea that has not responded to other treatments. The surgery might involve removing the tonsils or realigning the jaw.
- Weight loss: Losing weight may help alleviate sleep apnea in people with obesity.
You May Like: Does Medicare Cover Fall Alert Systems
Youre Our First Priorityevery Time
We believe everyone should be able to make financial decisions with confidence. And while our site doesnt feature every company or financial product available on the market, were proud that the guidance we offer, the information we provide and the tools we create are objective, independent, straightforward and free.
So how do we make money? Our partners compensate us. This may influence which products we review and write about , but it in no way affects our recommendations or advice, which are grounded in thousands of hours of research. Our partners cannot pay us to guarantee favorable reviews of their products or services.Here is a list of our partners.
Does Medicaid Cover Cpap
State Medicaid programs typically follow the same guidelines as Medicare. You need a sleep test, diagnosis of obstructive sleep apnea, and prescription from your doctor. Your AHI must also meet the same requirements as for Medicare:
- AHI index between 5 and 14, along with a comorbidity related to obstructive sleep apnea or
- AHI of at least 15.
If you meet these requirements, then Medicaid provides CPAP coverage for a 12-week trial. Coverage continues if your sleep apnea improves with the CPAP treatment. You must also adhere to the same compliance requirements as Medicare recipients, namely using the machine at least 4 hours every night on 70% of nights.
Don’t Miss: When Is The Next Medicare Open Enrollment
