Are Medicare Plan F Premiums Tax
When filing your federal tax return, Medicare Plan F premiums would be tax-deductible. Additionally, any medical expenses that you pay for out-of-pocket can also be deducted on your taxes. You would need to itemize these medical expenses, but the tax deductions could provide valuable additional returns. During the itemizing process, you would only be able to deduct expenses that exceed 10% of your adjusted gross income.
Ready To Find Your Plan
For California residents, CA-Do Not Sell My Personal Info, .
This Website serves as an invitation for you, the customer, to inquire about further information regarding Medicare Supplement insurance, and your call will be routed to a licensed agent who can provide you with further information about the insurance plans offered by one or more of our third party partners. Submission of your contact information constitutes permission for an agent to contact you with further information, including complete details on cost and coverage of this insurance.
We and the licensed agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program. Medicare has neither reviewed nor endorsed the information contained on this website. This is not a complete listing of plans available in your service area. For a complete listing please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
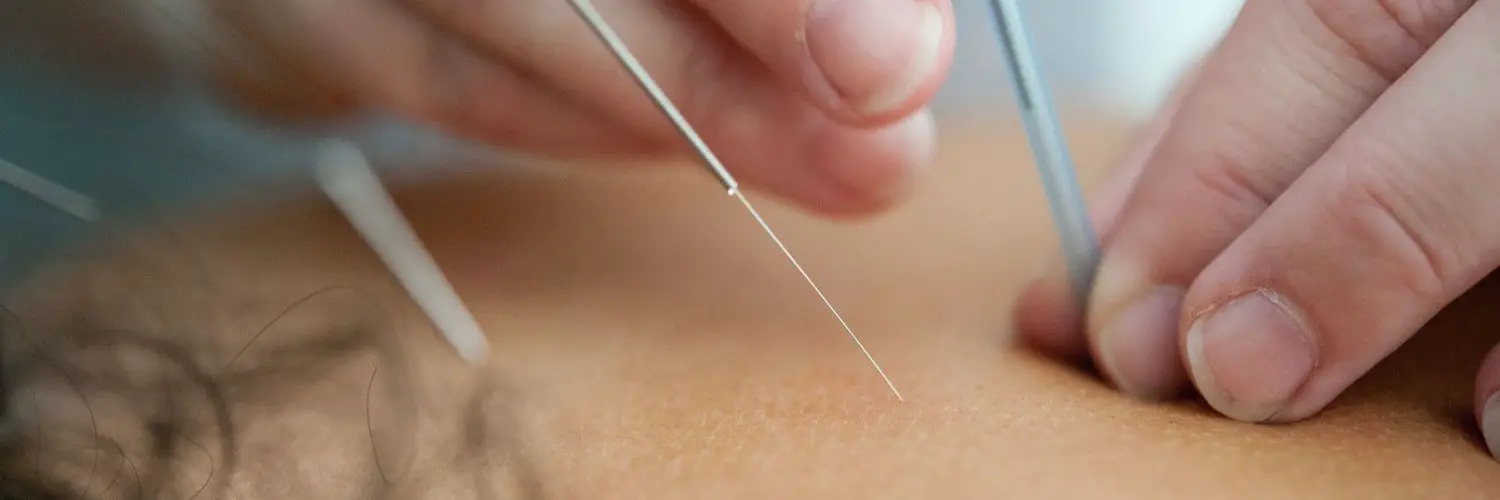
Is Acupuncture Covered By Medicare
As of January 2020, Medicare covers acupuncture treatment for chronic low back pain, according to the Centers for Medicare & Medicaid Services.1 The coverage is subject to limitations on the number of sessions and the type of provider administering the treatment.2
Heres a deeper look into acupuncture and Medicare.
Read Also: Is A Nursing Home Covered By Medicare
What Does Medicare Supplement Plan F Cover
Medicare Supplement Plan F only covers services that are covered by original Medicare . If you receive a medical treatment that Medicare does not cover, such as acupuncture, Plan F will also not cover it. Plan F also does not cover medications under most circumstances, since these are covered by Medicare Part D.
After your Plan F deductible has been met, you can expect Plan F to pay the following:
Does Medicare Cover Chiropractic Services
Chiropractic services focus on the diagnosis, conservative care, and prevention of spine-related disorders. Chiropractors focus on well-being and spinal health. Additionally, they can provide you with lifestyle recommendations, nutritional advice, fitness coaching, and soft-tissue therapies. So, does Medicare cover chiropractic services? Medicare does cover some chiropractic services, but not all. Keep reading to find out what Medicare covers!
Read Also: Is Xolair Covered By Medicare Part B
Is There An Alternative To Plan F
Since Plan F has been phased out for newer members, the best alternative is Plan G. Medicare Plan G covers all the same things that Plan F covers, except for the Medicare Part B deductible. Plan G doesnt cover the Part B deductible, which was a selling point with Plan F. The cost of Plan F and Plan G is very similar, so thats a good alternative to Plan F.
What Does Medicare Plan F Cover
Those who have Medicare Plan F won’t pay out-of-pocket costs for Medicare parts A and B. Policyholders would only pay the premiums, which start at $0 for Part A and $135.50 for Part B. Additionally, individuals would not have to pay the deductible, which is $1,364 for Part A and $185 for Part B.
Supplemental Medicare Plan F will cover:
- Medicare Part A coinsurance and hospital costs
- Medicare Part A deductible
- Hearing aids and routine hearing tests
- Cosmetic surgery
- Prescription drugs
The most important to note of these coverage gaps are prescriptions drugs and we would recommend purchasing Medicare Part D if you need this coverage. Medicare Plan F does provide coverage for injectable or infusion drugs given in a clinical setting but does not pay for other prescription drugs. The ideal coverage package would include Medicare parts A and B, along with the Part D prescription drug plan and a supplemental Medigap policy such as Plan F.
Unfortunately, none of the Medicare and Medigap policies cover dental care. If you are looking for dental coverage, then you would need to purchase a stand-alone dental insurance policy.
Don’t Miss: Does Medicare Cover International Medical Emergencies
How Does Innovative G Upgrade Medicare Coverage
You may know that Acupuncture is now covered by Medicare. You are allowed 12 sessions, and if your doctor thinks you are showing improvement, you can get approved for 8 more. The main disadvantage is that you need to fulfill some requirements before you can get this coverage, like proving that you have been in pain for more than 3 months and not having had surgery recently. Technically, if you purchased an Innovative G with Health Net, you could get coverage for an additional 20 Acupuncture visits.
In the case of Chiropractic care, as stated above, Medicare only covers Chiropractic visits for manipulation of the spine in a particular case. If you were to enroll in HealthNets Innovative G, you could be reimbursed for up to 20 Chiropractic additional visits for any reason as long as it was medically necessary. Remember this new plan only covers for a combined 20 visits between Acupuncture AND Chiropractic so you could not get 20 acupuncture visits and 20 chiropractic visits covered in the same year.
Other Medicare Supplement Plans
1 Insured by Cigna Health and Life Insurance Company, American Retirement Life Insurance Company, Loyal American Life Insurance Company or Cigna National Health Insurance Company. In Kansas and Pennsylvania, Medicare Supplement insurance policies are insured by Cigna National Life Insurance Company. American Retirement Life Insurance Company, Loyal American Life Insurance Company and Cigna Health and Life Insurance Company plans are not available to residents of Kansas or Pennsylvania.
2 A benefit period begins on the first day you receive service as an inpatient in a hospital and ends after you have been out of the hospital and have not received skilled care in any other facility for 60 days in a row.
3 Notice: When your Medicare Part A hospital benefits are exhausted, the insurer stands in the place of Medicare and will pay whatever amount Medicare would have paid for up to an additional 365 days as provided in the policys Core Benefits. During this time, the hospital is prohibited from billing you for the balance based on any difference between its billed charges and the amount Medicare would have paid.
4 Once you have been billed $203 of Medicare-approved amounts for covered services, your Part B deductible will have been met for the calendar year.
5 State variations apply. The Household Discount is not available in HI, ID, MN, and VT. For residents of WA, the discount only applies to spouses .
- Customer Plan Links
You May Like: Does Medicare Cover Handicap Ramps
How Is Medicare Part D Prescription Drug Coverage Changing For 2022
For stand-alone Part D prescription drug plans, the maximum allowable deductible for standard Part D plans is $480 in 2022, up from $445 in 2021.
And the out-of-pocket threshold will increase to $7,050 in 2022, up from $6,550 in 2021. The copay amounts for people who reach the catastrophic coverage level in 2021 will increase slightly, to $3.95 for generics and $9.85 for brand-name drugs.
Some Medicare beneficiaries with Part D coverage will continue to have access to insulin with a copay of $35/month, and more insurers are participating in this program for 2022.
The Affordable Care Act has closed the donut hole in Medicare Part D. As of 2020, there is no longer a hole for brand-name or generic drugs: Enrollees in standard Part D plans pay 25% of the cost until they reach the catastrophic coverage threshold. Prior to 2010, enrollees paid their deductible, then 25% of the costs until they reached the donut hole, then they were responsible for 100% of the costs until they reached the catastrophic coverage threshold.
That amount gradually declined over the next several years, and the donut hole closed one year early in 2019, instead of 2020 for brand-name drugs.
The donut hole is still relevant, however, in terms of how drug costs are counted towards reaching the catastrophic coverage threshold, and in terms of who covers the costs of the drugs . Heres more about how that all works.
Does Medicare Cover Chiropractic Care
Medicare does cover medically necessary chiropractic services. According to the CMS, Medicare Part B covers 80% of the cost for manipulation of the spine if medically necessary to correct a subluxation. There is no cap on the number of medically necessary visits to a chiropractor.
Under Original Medicare, without any additional insurance, you would have to pay your part B deductible and 20% coinsurance for all medically necessary chiropractic appointments.
Also Check: Does Medicare Help With The Cost Of Hearing Aids
What Is Massage Therapy
Massage therapy is the practice of rubbing and kneading your bodys soft tissues. It may focus on a specific part of your body to help relieve pain. It can also be done all over your body for a relaxing, therapeutic effect.
Massage therapy can be helpful for a variety of conditions and ailments. The benefits of massage therapy include:
- increased flexibility
- reduced muscle and joint pain
- increased circulation
- fewer headaches and migraines
Massage therapy may also be beneficial for certain conditions, including arthritis, cancer-related pain, carpal tunnel, muscle strain from an injury, and more.
What Does Medicare Supplement Insurance Plan F Cover
Medicare Supplement Plan F covers costs that Medicare doesnt cover, says Laura Decker, co-founder and president of the Employee Benefits Division at SSGI, a Maryland-based employee benefits insurance agency.
Specifically, this includes costs for Medicare Part A and Part B like:
- Copayments
- Coinsurance
- Deductibles
In addition to the deductibles and copayments, Medicare Plan F also covers things like hospice care coinsurance, skilled nursing facility coinsurance, up to three pints of blood, and foreign travel emergency care.
Read Also: How To Verify Medicare Eligibility Online
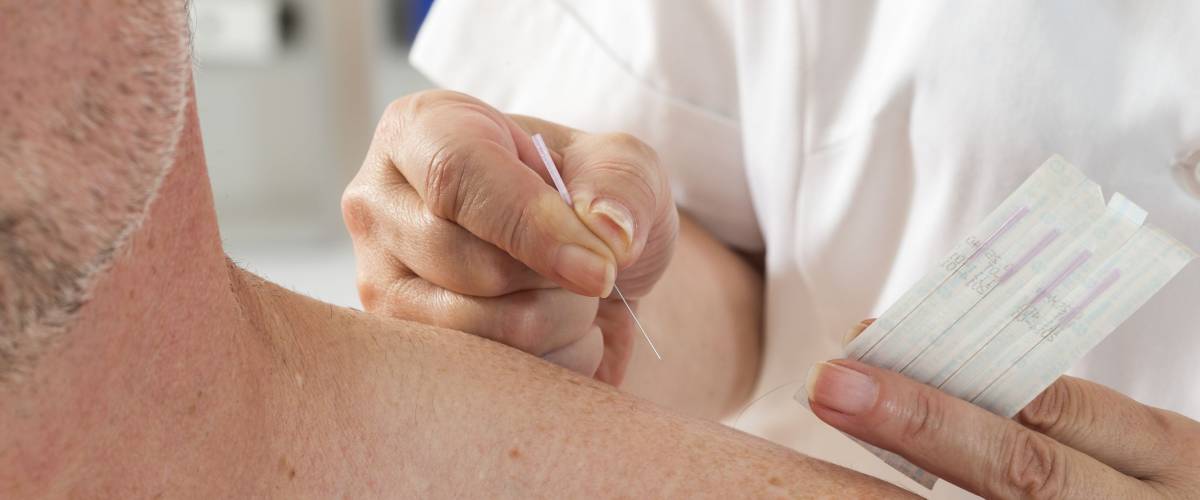
Are All Acupuncture Services Covered By Medicare
While Medicare pays for some acupuncture services, not all acupuncture sessions are covered.
Acupuncture is covered by Medicare Part B . Its only covered to treat chronic lower back pain. To qualify, you must meet these requirements:
- Your pain has to have existed for 12 weeks or longer.
- There’s no identifiable cause, such as an infectious disease or inflammation.
- Your pain isn’t related to surgery or pregnancy.
Medicare will cover up to 12 acupuncture visits in 90 days. If you show improvement, it will cover up to eight additional sessions, but you cant get more than 20 covered sessions in a year.
According to the CMS, to get Medicare coverage for your pain treatments, acupuncture must be administered by a doctor or healthcare provider with the following qualifications:
- A master’s or doctoral degree in acupuncture or Oriental medicine from a school accredited by the Accreditation Commission on Acupuncture and Oriental Medicine
- A current, full, active, and unrestricted license to practice acupuncture in the state where youre getting treatment
Which Parts Of Medicare Cover A Chiropractor
With all the parts of Medicare, which ones cover a chiropractor? Medicare Part A doesnt cover chiropractic services. It covers inpatient hospital care, and since seeing a chiropractor is an outpatient service, it is not covered by Part A.
Medicare Part B covers preventive services as well as medically necessary outpatient services. Preventative services include flu shots, wellness visits, and some mental health services. Medicare Part B covers manual manipulation of the spine to correct subluxation when it comes to chiropractic care. Medicare covers this chiropractic service as long as it is medically necessary. There is no limit on the number of visits that Medicare will cover for spinal subluxation treatment.
Once youve met the yearly deductible, Medicare will pay 80% of the the approved service. Diagnostic tests and massage therapy that your chiropractor requests will not be covered by Medicare Part B.
Medicare Part C, also known as Medicare Advantage plans, may cover a chiropractor appointment. As mentioned above, each plan differs. You can refer to your plans Summary of Benefits or call your insurance provider for more information on your cost-sharing for chiropractic services. Since Medigap plans must cover what Medicare covers, you would not have to contact your Medigap carrier. Instead, you would only need to call Medicare if you had any questions.
Recommended Reading: Is Rollator Walker Covered By Medicare
Where Can I Get Acupuncture Treatments Paid For By Medicare
Medicare will only cover acupuncture treatments administered by a doctor or healthcare provider with the following credentials:
- A masters degree or doctorate in acupuncture or Oriental medicine, from a school accredited by the Accreditation Commission on Acupuncture and Oriental Medicineand
- An active and unrestricted license to practice acupuncture in the state where care is being provided6
Find Cheap Medicare Plans In Your Area
Acupuncture is covered by two types of Medicare insurance plans Original Medicare and Medicare Advantage along with Medicare Supplement policies. Medicare limits the number of acupuncture sessions you can receive and who can provide those services.
When comparing how each option covers acupuncture, we found that Medicare Advantage generally offers lower cost plans with the same or better coverage than Original Medicare. This makes Medicare Advantage plans particularly HMOs our choice for best overall value.
Medicare covers acupuncture only for chronic low back pain, which the agency defines as:
- Pain not associated with surgery or pregnancy
- Having no known cause
- Lasting 12 weeks or longer
You are covered for up to 12 acupuncture visits in 90 days. Medicare will cover eight additional sessions if you show improvement, which means you can receive up to 20 acupuncture treatments in a calendar year. If your doctor decides the treatment is not helping or your condition is getting worse, Medicare won’t cover the extra acupuncture services.
Remember that Medicare doesn’t cover acupuncture for any condition other than chronic low back pain.
You May Like: Does Aetna Medicare Advantage Cover Dental
Q: What Are The Changes To Medicare Benefits For 2022
A: There are several changes for Medicare enrollees in 2022. Some of them apply to Medicare Advantage and Medicare Part D, which are the plans that beneficiaries can change during the annual fall enrollment period that runs from October 15 to December 7.
But there are also changes to Original Medicare cost-sharing and premiums, the high-income brackets, and more.
The standard premium for Medicare Part B is $170.10/month in 2022. This is an increase of nearly $22/month over the standard 2021 premium, and is the largest dollar increase in the programs history. But the 5.9% Social Security cost-of-living adjustment is also historically large, and will more than cover the increase in Part B premiums for beneficiaries who receive Social Security retirement benefits.
CMS noted that the significant Part B premium increase is due to several factors, including costs associated with COVID, uncertainty around potential spending increases due to Aduhelm , and the fact that 2021 premiums were lower than they would otherwise have been, due to a short-term spending bill enacted in 2020 that limited the Part B premium increase for 2021. Under the terms of the spending bill, the increase for 2021 was limited to 25 percent of what it would otherwise have been.
Looking for Medicare coverage with lower costs? Talk with a licensed advisor now. Call .
Is The Medicare Advantage Out
Medicare Advantage plans are required to cap enrollees out-of-pocket costs for Part A and Part B services . The cap does not include the cost of prescription drugs, since those are covered under Medicare Part D .
For several years, the cap was $6,700, although most plans have had out-of-pocket caps below that level. For 2021, the maximum out-of-pocket limit for Medicare Advantage plans increased to $7,550 , and its staying at that level for 2022. As usual, most plans will continue to have out-of-pocket caps below the governments maximum.
Recommended Reading: When Is The Last Day To Change Medicare Plans
How To Get Covered For Acupuncture
If youre already paying for acupuncture or chiropractic treatments out-of-pocket, or suspect you may need them in the future, then look for a Medicare Advantage plan that covers them. Paying a higher monthly premium may be worth it if you expect to use these treatments regularly.
You have more flexibility to switch between Medicare Advantage plans that you do with Original Medicare and Medigap, so be sure to check your coverage each year to find out if its changed or if another plan offers more extensive coverage.
If you want to switch to a plan that covers acupuncture or chiropractic care, you can only do that during the Open Enrollment Period, which takes place twice per year.
Another option is to see if these services will be covered by any secondary insurance you have, such as a spouses insurance plan or by federal employee health coverage.
Why Doesn’t Medicare Cover Hearing Care

As this clinical review explains, “The Medicare Act of 1965 statutorily excluded coverage of hearing aids under the premise that they were ‘routinely needed and low in cost,’ suggesting that consumers would be responsible for their purchase.” Also, at the time, many seniors didn’t live as long as they do today, and so fewer people had age-related hearing loss. There also was little understanding of how important it is to treat hearing loss to reduce depression and social isolation.
Also Check: Does Medicare Cover Family Counseling
What Acupuncture Treatments Are Not Covered By Medicare
The new Medicare rule applies to acupuncture for chronic lower back pain. Theres no Medicare coverage for acupuncture to treat neck pain, headaches, stress, or relief from chemo. Medicare does NOT cover acupuncture to treat pain in other parts of the body.
Also, Medicare doesnt pay for acupuncture to treat temporary acute pain, such as pain from a recent injury. Further, it wont cover pregnancy-related lower back pain.
