Which Medicare Plans Cover Diabetic Supplies
To understand the Medicare coverage of diabetes supplies, it is important to understand how Medicare works. There are four main parts of Medicare:
- Medicare Part A covers in-patient hospital services, so this part does not include diabetic supplies.
- Outpatient medical services, such as doctor examinations and diabetes treatment, are covered under Medicare Part B. Medicare Part B may cover an insulin pump as medical equipment, if you use one.
- Medicare Advantage, also called Medicare Part C, is a private version of Medicare you can enroll in instead of Original Medicare.
- And finally, Medicare Part D is the optional part of Medicare that covers prescription drugs, including insulin and anti-diabetic drugs if they are listed on a plans formulary and you have a prescription from your doctor.
All parts of Medicare can be advantageous to consumers with diabetes. Although Part A does not cover any diabetes supplies, it does cover in-patient hospital services, which could be diabetes-related. That said, Medicare Part B and D are the most beneficial to people with diabetes. Here is a complete breakdown of what each plan covers in relation to diabetes care:
Telehealth: How Does It Work
As an endocrinologist or a GP treating a patient in a telehealth eligible area, you can refer the patient to a specialist for a consultation via telehealth. During the consultation, the patient and the GP or another health professional will be able to see and hear each other via video conferencing and the specialist may also be at the patient-end of the consultation, to provide clinical services where appropriate.
Find out more information here:
Do Medicare Advantage Plans Cover Diabetic Supplies
Medicare Advantage plansMedicare Advantage , also known as Medicare Part C, are health plans from private insurance companies that are available to people eligible for Original Medicare …. are required to cover the same services as Original MedicareOriginal Medicare is private fee-for-service health insurance for people on Medicare. It has two parts. Part A is hospital coverage. Part B is medical coverage…., which includes the diabetic supplies covered by Part B. Some Medicare Advantage plans also bundle a Part D plan for prescription drug coverage, which you can use for your insulin and other prescriptions.Medicare.gov, How do Medicare Advantage Plans work?, Accessed November 24, 2021
However, your out-of-pocket costs with a Medicare Advantage plan may be different than those with Original Medicare. Also, Medicare Advantage plan rules may require their members to use in-networkDoctors, hospitals, pharmacies, and other healthcare providers that agree to health plan members’ services and supplies at a set price are in-network providers. With some health plans, your care is only covered if you get… providers for all of their services, supplies, and durable medical equipment.Medicare.gov, How do Medicare Advantage Plans work?, Accessed November 24, 2021
Also Check: Can You Have Two Medicare Advantage Plans
What Does Medicare Pay For Diabetes Supplies And Services
In general, Medicare pays 80% and you pay 20% of the Medicare-approved amount for diabetes supplies and services covered by Part B after the yearly deductible is met. Your percentage share of the cost is called coinsurance.
You may pay a coinsurance amount or a copayment for items covered by Part D. What you pay depends on the terms of your specific Part D plan.
Some services, such as medical nutrition therapy and A1C tests, may be provided at no additional cost to you.
Medicare Advantage plans cover diabetes supplies and services, too, and often additional services such as vision, dental and hearing care. The costs and items covered will depend on the specific plan you have.
When it comes to managing diabetes, be sure to review how your Medicare coverage may cover what you need. Also, your annual Medicare Wellness Visit is a great time to talk to your doctor and make sure youre up to date with preventive care services that support your diabetes care.
Which Insulin Pumps Are Covered By Medicare
Medicare coverage for insulin pumps is determined by the type of pump you have. Tubed pumps are durable medical equipment. They are covered by Medicare Part B.
Tubeless pumps are patches that contain insulin. They are covered by Medicare Part D .
Get the health benefits and savings youre entitled to.
Also Check: Does Medicare Cover Varicose Vein Treatment
How Much Does Insulin Cost
Insulin usage varies. People with Type 1 diabetes typically use more than those with Type 2 diabetes. GoodRx lists retail prices from $92 to $417 for a 10-ml vial, or higher, depending on the products features and delivery system.8 Most patients use two to three vials per month, while others use four. Also, those with Type 1 diabetes often require more than one type of insulin.
Recommended Reading: Can I Use Medicare For Dental
How Medicare Part B Covers Diabetes
Medicare Part B covers the fasting blood glucose test, which is a diabetes screening. Medicare covers two diabetes screenings each year for beneficiaries who are at high risk for diabetes. High risk factors for diabetes include: high blood pressure, history of abnormal cholesterol and triglyceride levels, obesity, or a history of high blood sugar. If diabetes runs in your family, you may also need regular diabetes testing. Your doctor may also recommend services that Medicare doesnt cover.
You generally pay nothing for these diabetes tests if your doctor accepts the amount approved by Medicare for the diabetes screening. However, you may have to pay 20% of the amount approved by Medicare for the doctors visit.
If your doctor diagnoses you with diabetes, Medicare covers the supplies you need to control your diabetes, including blood sugar testing monitors, blood sugar test strips, lancet devices and lancets, and blood sugar control solutions.
Medicare Part B may cover an external insulin pump and insulin as durable medical equipment. You pay 20% of the amount approved by Medicare, after the yearly Medicare Part B deductible.
Medicare may also cover medical nutrition therapy for diabetes, if referred by a doctor. You pay 20% of the amount approved by Medicare after the yearly Medicare deductible for services related to diabetes.
Don’t Miss: Does Medicare Cover Ice Therapy Machines
What Glucose Monitor Is Covered By Medicare
Not every glucose monitor is covered by Medicare. Several CGM systems that contain glucose monitors are available for beneficiaries. They include:
- Eversense
- Freestyle Libre
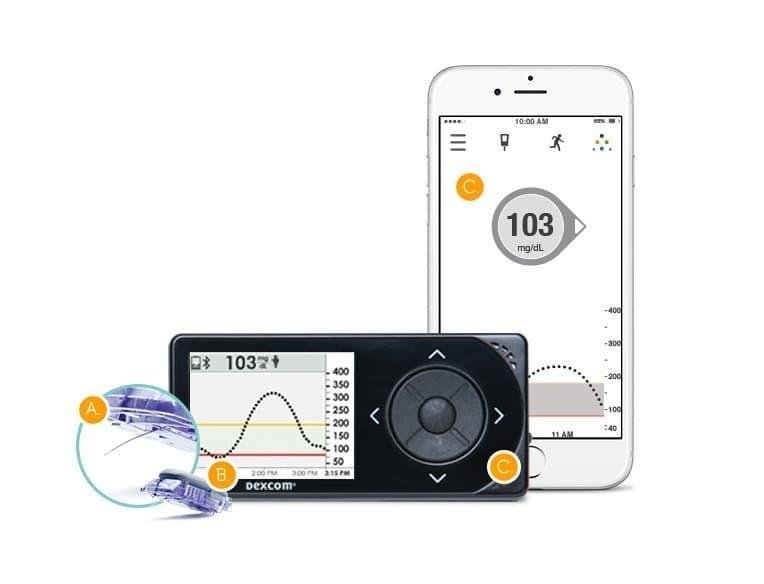
- Dexcom G6
If you have Medicare Part C, your plan may cover additional glucose monitors. Each plan varies, so make sure to check before you buy. In many instances, you will need preapproval from your plan or Original Medicare before purchase.
What extra benefits and savings do you qualify for?
When Does Medicare Cover Insulin
Medicare does cover insulin and some related supplies, but what’s covered depends on your plan.
For example, most people using Medicare Part B pay all of the costs for:
- Needles
People who have Medicare Part D pay for:
- Insulin pump supplies
The best way to decrease your total out-of-pocket cost for insulin under Medicare is to have both Part B and Part D.
You May Like: Who Can Get Medicare Insurance
Confirming Medicare Advantage Insulin Coverage
While most MA-PD and Part D plans may cover insulin, its important to verify coverage with the specific plan before enrolling. Additionally, an MA-PD or Part D plan may include coverage for insulin-related supplies such as gauze, syringes, needles and alcohol swabs.
Finally, seniors should note that MA-PDs and Part D plans dont directly cover insulin administered with an insulin pump. Pumps are considered durable medical equipment and may be covered, along with insulin, through Medicare Part B. Seniors enrolled in Medicare Advantage are by default also enrolled in Medicare Parts A and B.
Does Medicare Cover Diabetic Sensors
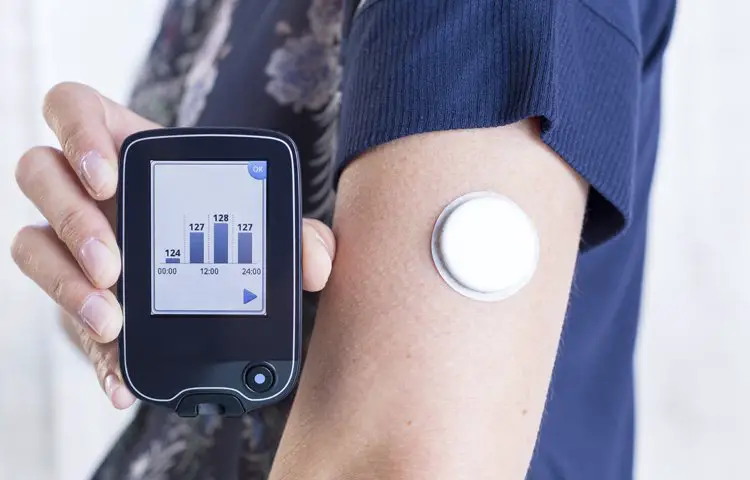
Diabetic sensors are also referred to as glucose sensors. Theyre used to measure blood sugar as part of a CGM system. Medicare does not cover every CGM system. If your system is covered, your diabetic sensor will be, too.
Diabetic sensors are professionally inserted under the skin, usually on the abdomen or arm. They take continual glucose measurements, which you can monitor at a glance. You can share your readings with a mobile device, such as your smartphone.
Are you eligible for cost-saving Medicare subsidies?
You May Like: Does Medicare Call To Verify Information
Medicare Coverage For Diabetes Screenings
If you have Medicare and your doctor considers you at risk for diabetes, you may be eligible for up to two blood sugar screenings per year under Medicare Part B you dont pay anything for the screening itself if you use a Medicare-assigned provider at a Medicare-approved facility. However, you may have to pay 20% of the Medicare-approved amount for the visit to the doctors office.
Risk factors that may qualify you for a Medicare-covered diabetes screening include:
- High blood pressure
- High blood sugar levels when fasting
Therapeutic Shoes And Inserts

Medicare Part B may also cover therapeutic shoes or inserts if you need them for your diabetes, but you have to meet certain conditions. You may qualify for one pair of depth-inlay shoes and three pairs of inserts per year.
If you cant wear depth-inlay shoes, Medicare may pay for one pair of custom-molded shoes and two pairs of inserts.
You have to meet certain conditions, including being diagnosed with diabetes, are in a comprehensive treatment plan and require the shoes and inserts.
You also must have at least one of these conditions:
- Diabetes-related nerve damage with signs of callus problems
- Foot deformity
- Partial or complete foot amputation
- Poor circulation
You will also need a podiatrist or other qualified health care professional to prescribe the shoes and to fit and provide them.
Read Also: Is Medicare Solutions A Legitimate Company
Early And Comprehensive Provider And Patient Education Regarding Medicare Part D
The introduction of Medicare part D will necessitate greater patient and provider education regarding numerous aspects of the MMA including PDP enrollment, potential credits, PDP characteristics, formularies, and the appeals process for uncovered drugs. Both patients and providers will need to be educated regarding paperwork, guides, and web-based systems introduced to assist Medicare beneficiaries enroll in and compare part D plans. There will be a mass of patients with information needs regarding the Medicare part D benefit and the earlier the provider and patient undertake education initiatives, the more efficient the transition under MMA will be. There are several resources available to both patients and providers . Additional education and implementation efforts must be launched to address the unique needs of certain populations including dual-eligible beneficiaries and minorities. In addition to basic outreach strategies, community-based initiatives involving personal interactions between providers and beneficiaries will be critical.
What Medicare Members Would Pay
CMS had originally proposed three different categories of payment for those using the different types of CGM technology. The logic was that some didnt require fingersticks so users wouldnt need reimbursement for test strips, as would other systems that still require calibration . It also viewed the FreeStyle Libre flash glucose monitoring a bit differently than other tech, like Dexcom and Eversense. So it proposed different reimbursements for those varying styles of tech.
However, CMS has re-thought that move after public outcry. In its new December 2021 rule comments, the agency noted this:
After consideration of public comments, CMS does not believe it is necessary at this time to further stratify the types of CGMs beyond the two categories of non-adjunctive and adjunctive CGMs.
Read Also: What Medicare Plans Do I Need
Are Glucose Monitors Covered By Medicare
Medicare Part B covers Glucose monitors as durable medical equipment that your doctor has prescribed for your use at home.
You will need to get your monitor from a Medicare-approved supplier. Medicare will determine if your monitor must be rented or purchased. In some instances, you may be able to choose between those options.
As part of a CGM system, glucose monitors connect wirelessly with insulin pumps. They provide all-day readings of your blood sugar levels without the need for most finger pricks.
Which Diabetic Supplies Are Covered By Medicare
For those with diabetes, Medicare Part B covers three main areas of diabetic supplies: blood sugar self-testing equipment and supplies, insulin pumps, and therapeutic shoes or inserts. For these areas, Medicare typically covers 80% of the visit and you will pay 20% if you do not have coinsurance. These costs can also go toward the Part B deductible.
Medicare Part B also covers certain diabetic screenings and services.
If you have an insulin pump, Medicare Part B covers the pump as well as the insulin under durable medical equipment instead of as medicine under Part D, explains Lindsey Hudson, APRN, NP-C, and certified diabetes care and education specialist working in Charleston, South Carolina, and a member of the SingleCare Medical Board.
Medicare Part B also covers certain diabetic screenings and services. For the supplies, screenings, and services below, note that Medicare consumers may have to pay coinsurance, copays, and/or deductibles depending on their plan.
Recommended Reading: Can I Sign Up For Medicare Before I Turn 65
Other Useful Information On Diabetic Supplies
- Generally, you pay 20% of Medicare-approved amounts for your supplies, and the Medicare Part B deductible applies.
- Make sure you refill your supplies in a timely manner, and only accept supplies you have requested. Medicare wont pay for supplies you didnt order for example, if a supplier automatically sends you items, you cannot get reimbursed by Medicare.
- You may rent or purchase certain diabetic supplies. For more information, call 1-800-MEDICARE . TTY users call 1-877-486-2048. Customer service representatives are available 24 hours a day, seven days a week.
- Ask if the supplier is a participating supplier in the Medicare program before you get durable medical equipment for diabetes. If the supplier is a participating supplier, he or she must accept assignment. If the supplier is enrolled in Medicare but isnt participating, he or she has the option to accept assignment or not. If a DME supplier doesnt accept Medicare assignment, there is no limit to what you can be charged. You also may have to pay the entire bill at the time you get the DME.
- All Medicare-enrolled pharmacies and suppliers must submit claims for diabetic testing supplies. You cant send in the claim yourself.
Dont Miss: When Does Medicare Coverage Start
Does Medicare Part B Cover Insulin
Medicare Part B covers insulin when it is medically necessary with the use of an insulin pump, since it is recognized as durable medical equipment in this case. That insulin is covered 80%, and you will need to pay 20% of the Medicare-approved cost unless you have a Medicare supplement plan to pick up the difference.
Also Check: Who Pays The Premium For Medicare Advantage Plans
What Doesnt Medicare Part B Cover For Diabetic Supplies
That is an important question because, despite all of the diabetic supplies and services it covers, Medicare Part B doesnt cover insulin. Specifically, Part B will not cover insulin unless it is for use with a medically necessary insulin pump. Medicare also does not provide coverage for:Medicare.gov, Insulin, Accessed November 23, 2021
- Insulin pens
- Alcohol swabs
- Gauze
If you want coverage for injectable insulin and the supplies in the bullet list above, you will have to enroll in Medicare Part D.
Does Medicare Pay For Insulin
The cost of your insulin, insulin pens, and insulin pumps depends on several factors:
- Your Medicare coverage and any supplemental coverage
- The type of insulin youre using
- How much of the medication you use each month or year
- Whether your Medicare drug plan requires a coinsurance or copayment for this medication
- Your income level and the state you live in
- The pharmacy you use to fill prescriptions
Read Also: Who Offers Medicare Supplemental Insurance
Medicare Coverage Requirements For Continuous Glucose Monitoring System
Medicare patients with type 1 and type 2 diabetes on intensive insulin therapy may be able to obtain reimbursement if the following Medicare coverage criteria are met:
- The patient has diabetes
- The patient is insulin-treated with three or more daily administrations of insulin or a continuous subcutaneous insulin infusion pump
- The patient’s insulin treatment regimen requires frequent adjustments based on BGM or CGM testing results
- Within six months prior to ordering the CGM, the patient had an in-person visit with the treating practitioner to evaluate their diabetes control and determine that the above criteria have been met and
- Every six months following the initial prescription of the CGM, the patient has an in-person visit with the treating practitioner to assess adherence to their CGM regimen and diabetes treatment plan.
In order to qualify for Medicare coverage of your Dexcom G6 supplies, Medicare requires that you have a receiver that is compatible with Dexcom G6 Continuous Glucose Monitor and that you use that receiver with your supplies, even if you also use a compatible smart device. Medicare does not cover Dexcom G6 supplies that are only used with a smartphone or other mobile device.
Medicare covers Dexcom G6 for insulin-requiring patients who meet the Medicare coverage criteria. For the full list of Medicare coverage criteria, visit the Centers for Medicare and Medicaid services website.
How Does Medicare Cover Diabetic Supplies
Medicare Part B covers a wide range of diabetes testing supplies, including:Medicare.gov, Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs, Accessed November 23, 2021
- Blood sugar monitors
- Lancet devices and lancets
- Glucose control solutions used to verify test equipment accuracy
Medicare covers the testing equipment and supplies listed above whether you use insulin or not. However, the number of supplies covered by Medicare Part B varies:Medicare.gov, Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs, Accessed November 23, 2021
If your doctor determines that its medically necessaryServices or supplies that are needed for the diagnosis or treatment of your medical condition and meet accepted standards of medical practice…., and completed the required documentation, Medicare will cover additional test strips and lancets. If you meet the necessary criteria, Medicare will cover a therapeutic continuous blood glucose monitor and related supplies.Medicare.gov, Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs, Accessed November 23, 2021
Recommended Reading: Can Permanent Residents Get Medicare
