Glucose Monitor And Test Strips
Cost with Part B: 20% or about $16 for at-home blood sugar monitor
Part B coverage: For those who have diabetes, Medicare Part B covers blood sugar self-testing equipment including glucose monitors, test strips, lancet devices, lancets and control solutions for testing equipment.
If you meet additional criteria, such as needing to continuously adjust your insulin intake, you may also be covered for a continuous glucose monitor and related supplies. The cost for this is also 20%, which is about $52 for the monitor system.
You’ll only have coverage for glucose monitoring equipment if you get a prescription from your doctor and you use a pharmacy or medical supplier that accepts Medicare. Refills for test strips and lancets are not automatic. You must ask for a refill and renew your prescription annually.
When deciding what brand of glucose monitor to choose, start by looking for a retailer that accepts Medicare. The retailer, which could be your local pharmacy, will know which brands of glucose monitors will be covered based on your prescription.
Find Medicare Supplement Plans That Help Cover Your Diabetic Supplies
A Medicare Supplement Insurance plan can help cover some of the Medicare copays and other costs for your diabetic supplies.
For example, each of the 10 standardized Medigap plans that are available in most states provide at least partial coverage for the Medicare Part B coinsurance or copayments you might face when you receive covered outpatient treatments and covered supplies.
A licensed agent can help you decide on a Medicare option that works for you. Call today to speak with a licensed agent and compare the Medigap plans that are available where you live.
What Diabetic Supplies Does Medicare Cover
When you research what parts of Medicare cover diabetic supplies, turn your attention toward Medicare Part B. You must be enrolled in Part B to receive preventive services authorized for people at risk for diabetes. Part B also covers diabetic equipment, therapeutic shoes and supplies like Medicare-approved diabetic testing strips.
Also Check: Which Of The Following Is True Regarding Medicare Supplement Policies
How To Get Diabetes Supplies Through Medicare Part B
To get your diabetes supplies under Medicare Part B, you need a prescription from your doctor. The prescription should state:
Simply hand one of the Medicare cards shown here and your prescription to your pharmacist when you go to the pharmacy.
What Diabetic Supplies Are Covered By Medicare

In order to have your supplies covered by Medicare, you musthave a prescription from your doctor, and receive the items over the counterfrom an authorized seller. The items must also be on Medicares approved list,otherwise they wont be covered.
Your local pharmacy is most likely an authorized seller, butits best to confirm with them that they accept Medicare before making yourpurchase. If you buy your supplieswithout a prescription, or from a seller thats not authorized, Medicare wontcover any of the costs.
Medicare Part B covers the following supplies, if they areprescribed by your doctor following their guidelines:
- Glucose test strips
Recommended Reading: How Long Do You Have To Sign Up For Medicare
Does Medicare Cover Diabetic Supplies
- Medicare Part B covers certain diabetic supplies and preventive screenings.
- Medicare Part D covers oral diabetic medications, injectable insulin, and self-injection supplies.
- Get prescriptions from your doctor for any medication, supply, or service youll want Medicare to cover.
- Check that your pharmacy or device supplier accepts Medicareset payment rates to avoid overpaying.
Diabetes is a metabolic condition that leads to high blood sugar levels. Most people who have diabetes have type 2 diabetes. According to the American Diabetes Association, around 14 million Americans 65 and older have diabetes, some who are undiagnosed.
Older adults with diabetes face unique challenges including hypoglycemia, brain and nervous system problems, and social support issues that require special monitoring to manage risks.
There are many types of diabetic supplies needed for preventive screening, monitoring, and managing the condition. Medicare has several parts that cover different types of supplies and services. Cost and coverage depend on the type of plan.
What Diabetic Supplies Are Covered By Original Medicare
Original Medicare Part B covers some diabetic supplies, including:
- Blood sugar test strips
- Blood glucose monitors, lancet devices, and lancets
- Glucose control solutions for checking the accuracy of test strips and monitors
- Insulin if you are using a medically necessary insulin pump
- Therapeutic shoes or inserts
There may be coverage limits on the quantity and frequency you can get these supplies.
Original Medicare Part B does not cover these diabetic supplies:
- Insulin
- Insulin pens, syringes, or needles
- Alcohol swabs or gauze
Read Also: How To Pay Medicare Premium
Free Diabetic Supplies With Medicare
There are three ways you can reduce your costs:
- Free diabetic supplies: In addition to the coverage you get through Medicare, free diabetic supplies may be available through manufacturers or through nonprofit assistance programs. For example, Accu-Chek offers free glucose meters. Some restrictions may apply, and we recommend checking that your Medicare plan will cover the test strips of the free glucose meter.
- Cheap insulin: Anyone can get cheap insulin by choosing a Medicare plan that participates in the Insulin Savings Program. Those who meet the financial requirements can get even cheaper copayments for insulin through the Medicare Extra Help program.
- Discounts on your Medicare costs: If you meet the financial requirements of a Medicare Savings Program, you can reduce or eliminate different out-of-pocket costs such as the Medicare Part B copayments, deductible and monthly premium.
Diabetes Supplies And Services Covered By Medicare Part B
- Blood glucose testing supplies and equipment
- Insulin pumps and insulin used with a pump
- Diabetes self-management training
- Medical nutrition therapy, including diet and lifestyle counseling
- Hemoglobin A1C tests to monitor blood glucose control
- Foot exams and treatment for diabetes-related nerve damage
- Therapeutic shoes or inserts
Read Also: Does Medicare Cover Cataract Surgery And Lenses
How To Sign Up For Medicare
If you are close to turning 65 and are not getting Social Security or Railroad Retirement Board benefits, you must sign up for Medicare. Even if you are eligible for premium-free Part A coverage, you still must enroll.
If you arent getting Social Security benefits, you will not automatically receive any information from Medicare. You must call Social Security at least three months before the month you turn 65 to avoid any late penalties.
To be eligible for Medicare, you must meet these requirements:
- You are turning 65 or have a qualifying disability.
- You or your spouse worked and paid Medicare taxes for at least 10 years.
- You are a U.S. citizen or permanent legal resident who has lived in the U.S. for at least five years.
- You are receiving Social Security or RRB benefits or have worked long enough to be eligible for those benefits but are not collecting them yet.
You can sign up for Medicare during:
- Your Initial Enrollment Period
- A Special Enrollment Period
- The General Enrollment Period
To enroll, you can:
Find Medicare Advantage Plans Cover Diabetes Supplies
1 10-minute claim is based solely on the time to complete the e-application if you have your Medicare card and other pertinent information available when you apply. The time to shop for plans, compare rates, and estimate drug costs is not factored into the claim. Application time could be longer. Actual time to enroll will depend on the consumer and their plan comparison needs.
MedicareAdvantage.com is a website owned and operated by TZ Insurance Solutions LLC. TZ Insurance Solutions LLC and TruBridge, Inc. represent Medicare Advantage Organizations and Prescription Drug Plans having Medicare contracts enrollment in any plan depends upon contract renewal.
The purpose of this communication is the solicitation of insurance. Callers will be directed to a licensed insurance agent with TZ Insurance Solutions LLC, TruBridge, Inc. and/or a third-party partner who can provide more information about Medicare Advantage Plans offered by one or several Medicare-contracted carrier. TZ Insurance Solutions LLC, TruBridge, Inc., and the licensed sales agents that may call you are not connected with or endorsed by the U.S. Government or the federal Medicare program.
Plan availability varies by region and state. For a complete list of available plans, please contact 1-800-MEDICARE , 24 hours a day/7 days a week or consult www.medicare.gov.
Medicare has neither reviewed nor endorsed this information.
Recommended Reading: How Are Medicare Rates Determined
Other Useful Information On Diabetic Supplies
- Generally, you pay 20% of Medicare-approved amounts for your supplies, and the Medicare Part B deductible applies.
- Make sure you refill your supplies in a timely manner, and only accept supplies you have requested. Medicare wonât pay for supplies you didnât order for example, if a supplier automatically sends you items, you cannot get reimbursed by Medicare.
- You may rent or purchase certain diabetic supplies. For more information, call 1-800-MEDICARE . TTY users call 1-877-486-2048. Customer service representatives are available 24 hours a day, seven days a week.
- Ask if the supplier is a participating supplier in the Medicare program before you get durable medical equipment for diabetes. If the supplier is a participating supplier, he or she must accept assignment. If the supplier is enrolled in Medicare but isnât âparticipating,â he or she has the option to accept assignment or not. If a DME supplier doesnât accept Medicare assignment, there is no limit to what you can be charged. You also may have to pay the entire bill at the time you get the DME.
- All Medicare-enrolled pharmacies and suppliers must submit claims for diabetic testing supplies. You canât send in the claim yourself.
Diabetic Supplies: Therapeutic Shoes And Inserts

Medicare Part B coverage includes therapeutic shoes or inserts for diabetics who have certain conditions â ask the doctor who treats your diabetes if you need them. To make sure these supplies are covered by Medicare, please note:
- A qualified doctor must prescribe the shoes or inserts.
- A qualified doctor must provide and fit you for the shoes or inserts.
- Medicare Part B covers one pair of custom-molded shoes or one pair of depth-inlay shoes per calendar year.
- Medicare also covers two additional pairs of inserts each calendar year for custom-molded shoes and three pairs of inserts each calendar year for depth-inlay shoes.
- In certain cases, shoe modifications may be substituted for inserts.
- The supplier must have an order on file signed and dated by the treating doctor if you switch to a different supplier, you may need to have your prescription transferred or get a new prescription from your doctor. Make sure your supplier is enrolled in Medicare.
Don’t Miss: Does Medicare Cover Dexcom G6 Cgm
Diabetes Testing Supplies And Services Covered By Medicare
If youve been diagnosed with diabetes, monitoring your glucose levels and managing your symptoms can seem daunting. Your physician may recommend services and supplies youll need to keep your diabetes in check. But, if youre on Medicare, youll have access to programs and benefits that can help you manage your disease.
Medicare Benefits Solutions
Medicare Drug Coverage For Diabetes
If you are enrolled in a Part D plan, either as a stand-alone Prescription Drug Plan or part of a Medicare Advantage plan, Medicare may cover the cost of:
- Insulin and devices that deliver insulin continuously
- Supplies designed to inhale or inject insulin, such as a syringe
- Disposable pumps
- Drugs you take orally
Check your plan for the level of coverage as Part D benefits vary among different insurers and across states.
The Part D Senior Savings Model is a new program that started on January 1, 2021. If you have a Medicare Advantage plan with drug coverage or a stand-alone Medicare drug plan that participates in this model, the Senior Savings Model can save you money on insulin.
Many types of insulin under this program cost no more than $35 per month. Note that if you fully participate in the Extra Help program, your monthly supply of insulin may be less than $35 per month.
Recommended Reading: What Is Blue Cross Blue Shield Medicare Advantage
What Brand Of Diabetes Supplies Is Covered By Medicare
There are a number of brands of diabetes supplies that are covered by Medicare, specifically:
- OneTouch
- Abbotts
- Bayer
However, not all brands are covered by Medicare, so check your coverage before purchasing any supplies. You can ask your doctor, pharmacist or supplier to check for you, or contact Medicare directly.
Does Medicare Cover Insulin
Medicare Part B will not coverinsulin unless it is used in an insulin pump. Medicare Part B also does not cover certain medical supplies used to administer insulin such as syringes, needles, insulin pens, alcohol swabs or inhaled insulin devices.
Medicare does not cover anti-diabetic drugs used to maintain blood sugar.
Recommended Reading: A Medicare Supplement Policy Is
What Does Medicare Cover For Diabetics
If you have diabetes, you know its a day-to-day reality that needs to be attended to. It can feel like a full-time job, but you dont have to do it alone.
Medicare covers various diabetes medications, supplies and services to help treat diabetes and keep your blood glucose in a healthy range.
- Medicare Part B covers blood glucose testing and other supplies you may need plus some medical and education services.
- Medicare Part D covers diabetes medications and supplies for injecting or inhaling insulin.
Heres a rundown of the diabetes supplies and services that Medicare covers. Some require a prescription or recommendation from your doctor. Coverage limits may include the amount of some supplies you can get or how often some services are covered.
How Much Does Medicare Pay For Diabetic Supplies
Medicare alone doesnt pay in full for most medical services, including diabetic supplies. Medicare Part B covers about 80% of the costs of a variety of supplies that are used to treat diabetes. Part B will typically cover these services and supplies up to 80%, leaving you responsible for the other 20% as well as any deductibles or copays. In order to help with the expenses, most people have a Medicare Supplement plan or a Medicare Advantage plan.
Its important to note that Medicare Supplement plans rangein coverage, and theyll all pay their portion as long as Medicare pays first. Thecost of your supplies may differ depending on which Medicare Supplement planyou choose.
If you have aMedicare Advantage plan, its your primary coverage instead of Medicare. Forinformation on what your Advantage plan covers, you should contact yourprovider directly.
Also Check: What Is Medicare Part B Reimbursement
Do I Qualify For These Benefits
Many diabetic supplies are a covered benefit of Medicare Part B. If you are enrolled, or eligible to enroll, in original Medicare, youll receive coverage for diabetic supplies and services.
Medicare pays the majority of the cost, but you are still responsible for 20 percent. You will also pay for any coinsurance, deductible, and copayment costs.
You can buy a supplemental plan to help offset some of these costs, such as a Medigap plan. Review different plan options to find one that best meets your needs.
For Medicare to cover diabetic supplies, your doctor needs to write prescriptions that explain:
- you have received a diagnosis of diabetes
- any special devices/monitors you need and why
- for special shoes, a podiatrist or other foot specialist has to explain why you need special shoes and provide a prescription
- how often you need to test your blood sugar levels
- number of test strips and lancets you need
New prescriptions are needed each year from your doctor. If you need to monitor your blood sugar more often, your supply limits for each month will need to be increased.
How Do You Get Diabetes Supplies Covered By Medicare
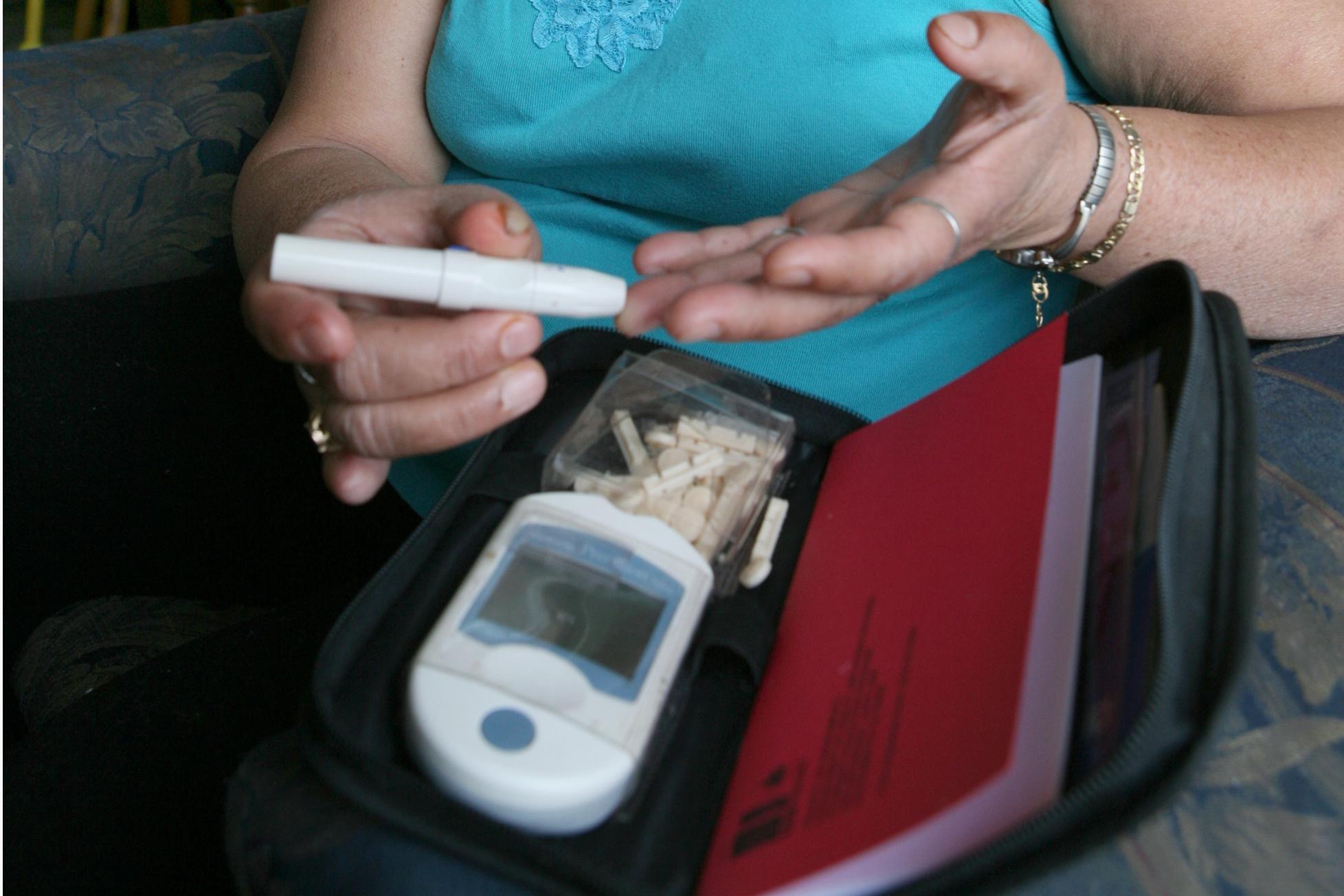
For most diabetic self-testing equipment and supplies, you need to get a prescription from your doctor in order for Medicare to cover it.
The prescription should specify:
-
How often you should test your blood sugar
-
How many test strips and lancets you need
You can either order and pick up your supplies at a pharmacy thatsenrolled in Medicare, or have them delivered to your home using a national mail-order contract supplier.
Recommended Reading: How To Apply For Medicare In Hawaii
How Much Will You Pay For Diabetes Supplies Through Medicare Part B
After you have met the Part B deductible, you’ll pay co-insurance of 20% of the Medicare-approved payment rate for necessary supplies and services. Many Medicare beneficiaries have additional coverage that may help them pay the co-insurance.
All diabetes supplies are reimbursed at the same rate under Medicare Part B.2,3 You won’t pay more to get quality Accu-Chek diabetes products available at all major retail pharmacies.
You can also receive your diabetes supplies through the Medicare national mail-order program, although mail-order suppliers may offer fewer brands than your local pharmacy. If the supplier you contact doesn’t carry Accu-Chek products, visit your local retailer to fill your Accu-Chek Guide test strip prescription.
Sign up for Accu-Chek news and offers
Get emails sent directly to your inbox with the latest updates and deals on Accu-Chek products.
1Centers for Medicare and Medicaid Services. Medicare’s coverage of diabetes supplies and services. Available at: . Accessed August 17, 2018.
2Medicare. Medicare’s national mail-order program for diabetes testing supplies. Available at: . Accessed August 16, 2018.
3Accu-Chek test strips are covered when medically necessary for the patient and prescribed by a physician.
