Medicare Part B Reimbursement In Recent Decades
In the 1990s, the Office of Inspector General detected fraudulent activity at nursing homes in the form of excessive billing and charges for unused supplies. The Benefits Improvement and Protection Act of 2000 limited the consolidated billing requirement to Medicare services not covered by Part A. Further, Congress required the OIG to monitor Medicare Part B payments that were not covered by Part A.
The Balanced Budget Act of 1997, meanwhile, established annual per-beneficiary Medicare spending limits or a therapy cap for outpatient physical therapy, occupational therapy, and speech-language pathology services provided under Medicare Part B. Under the Bipartisan Budget Act of 2018, the cap was repealed though cap limits were retained, meaning, additional claims must be filed after reaching the cap.
For instance, if a resident meets the cap for occupational therapy, which is $2,110 in 2021, the long term care facility will have to put a modifier on the claim for any other service for which the resident has a diagnostic code. This applies to physical therapy and speech-language pathology as well, for which the combined cap is $2,110.
Medicare Reimbursement For Original Medicare
Original Medicare includes Part A and Part B . Under this program, your Medicare providers send your claims directly to Medicare, and you wonât see a bill. Typically, you pay coinsurance or a copayment for Medicare Part A and Part B services, as well as Part A and Part B deductibles. But in most cases, you donât have to pay for the entire medical service up front and file for reimbursement.
Medicare providers and suppliers must send their claims to Medicare, so itâs typically the providers and suppliers who have to file for reimbursement.
The Centers for Medicare & Medicaid Services sets reimbursement rates for Medicare providers and generally pays them according to approved guidelines such as the CMS Physician Fee Schedule.
How Does Medicare Reimbursement Work
Medicare allows you to see any doctor you choose, but that doesnt mean all providers handle billing in the same way. Medicare has a schedule of rates it will pay for its covered healthcare services. Those rates are typically much less than a private insurance company would pay.
Most healthcare doctors are participating providers that accept Medicare assignment. They have agreed to accept Medicares rates as full payment for their services.
If you see a participating doctor, they handle Medicare billing, and you dont have to file any claim forms. However, certain doctors dont bill Medicare directly.
If you want Medicare to pay for your care, youll need to send a form to request reimbursement.
Seeing a Non-participating Doctor
These doctors accept Medicare patients, but they havent agreed to Medicares rates. They may choose to accept Medicare rates in your case, or they may decide to bill you up to 15% more than the Medicare rate. The extra charge is an excess charge. Non-participating doctors may bill Medicare directly. But they may also ask you to pay up-front and seek reimbursement from Medicare.
Foreign Travel Care Reimbursement
Receiving care outside the United States that is covered by Medicare. In general, Medicare doesnt pay for services in foreign countries. But there are a few exceptions where you can file a claim and get reimbursement for your costs.
Improper Provider Billing
If you are close to the deadline, you can seek reimbursement.
Recommended Reading: Can You Sign Up For Medicare Part A Only
Medicare Part B Premium Reimbursement
When Medicare is primary to NYSHIP coverage, NYSHIP reimburses you for the standard Medicare Part B premium you pay to SSA, excluding any penalty you may pay for late enrollment.
How will I be reimbursed for IRMAA?
A.
To be reimbursed for IRMAA, you must complete the IRMAA Reimbursement Request application and submit it to the Employee Benefits Division along with proofs of payment of your Medicare Part B premium. Please refer to the IRMAA Reimbursement Application instructionsfor more information.
Fehb Plans Offering Reimbursement
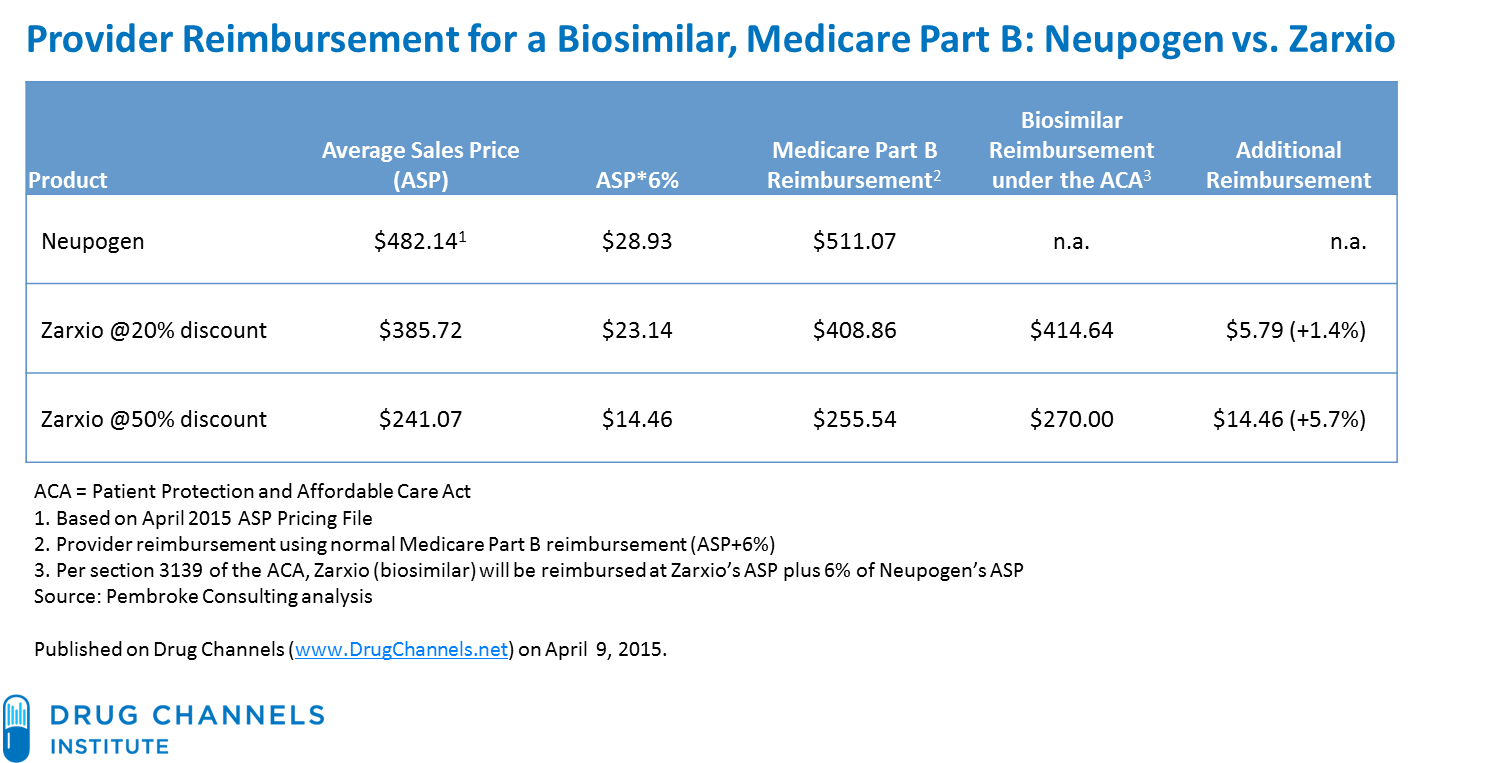

Here is the list of FEHB plans offering at least partial Medicare Part B premium reimbursement in 2018:
- Aetna Direct, members can request reimbursement for Medicare premiums that will be reduced from the medical fund amount.
- BlueCross Blue Shield PPO Basic Option Limited HRA is provided to any member enrolled in Medicare Part A and Part B reimbursement is to be used exclusively to pay Medicare Part B premiums $600 annually.
- Aetna HealthFund HDHP reimburse Medicare premiums using HRA funds.
- Aetna Health of Utah HDHP reimburse Medicare premiums using HRA funds.
- CareFirst HDHP reimburse Medicare premiums using HRA funds.
- GEHA HDHP reimburse Medicare premiums using HRA funds.
- Independent Health HDHP reimburse Medicare premiums using HRA funds.
- Kaiser Northern California, High Option Limited HRA reimbursement up to $125 of Medicare Part B monthly premium.
- Kaiser Northwest High Option reimburse Medicare B premiums up to $125 per month.
- Kaiser Health Plan of Washington HDHP reimburse Medicare premiums using HRA funds.
- MHBP Consumer Option reimburse Medicare premiums using HRA funds.
- TakeCare HDHP reimburse Medicare premiums using HRA funds.
- United Healthcare Insurance Choice Plus HDHP reimburse Medicare premiums using HRA funds.
Partial reimbursement may not cover the full cost of Part B premiums in 2018, but it is a help.
Recommended Reading: Does Medicare Cover Bone Grafts
To Update Your Part B Reimbursement For Premiums Paid During The 2021 Calendar Year:
Please submit a copy of your:
- Social Security New Benefit Amount statement for 2021 or
- Form SSA 1099 for 2021 or
- First Medicare monthly or quarterly billing statement for 2021
We recommend that you redact or avoid providing any personal identifiable information such as your address, birthdate, and all but the last four digits of your Social Security Number from the documents before you submit them. If the document does not have the last four digits of your SSN, please include that at the top of your documents. Please send all documents to LAFPPs Medical & Dental Benefits Section via:
- Fax to: 628-7782 or
- Mail to: Department of Fire and Police Pensions, Attn: Medical & Dental Benefits, 701 E. 3rd Street, Suite 200, Los Angeles, CA 90013
Due to the anticipated high volume of submissions, it may take at least two to three months to process your Part B documentation and update your reimbursement amount on your LAFPP pension payment.
As a reminder, Part B reimbursement only applies to Retired Members or Qualified Survivors who are eligible for an LAFPP health subsidy and are enrolled in both Medicare Parts A and B. Any additional Part B fees or penalties charged by CMS are not eligible for reimbursement.
Who Is Eligible For Medicare Reimbursement
Any Medicare beneficiary who pays their entire healthcare bill upfront, rather than only their specified portion, is entitled to Medicare reimbursement. Reimbursement may be full or partial, based upon the services received and the agreement the provider has with Medicare.
Any doctor, provider or facility that accepts Medicare assignment is eligible for Medicare reimbursement. Non-participating Medicare providers who agree to accept Medicare for specific procedures or services are also eligible for Medicare reimbursement.
While thats true, the form of Medicare reimbursement that matters to you is the money you are due to be paid when you overpay. If that happens, heres what you do.
Find a local Medicare plan that fits your needs
Also Check: What Medicare Part D Plan Is Best For Me
Sometimes You May Need To File A Medicare Claim
There may be occasions when you need to pay for medical services at the time of service and file for reimbursement. For example, if your health-care provider isnât âMedicare-assigned,â you might have to pay for the service or supply and file for reimbursement. If a provider or supplier accepts Medicare assignment, that means he or she has an agreement with Medicare to accept the Medicare-approved payment for that service or supply, and not bill you an additional amount.
Some health-care providers are considered âparticipatingâ providers they accept Medicare assignment for all Medicare-covered services. âNon-participatingâ providers can still decide to accept Medicare assignment for individual services.
Note: If you visit a doctor who doesnât accept Medicare assignment, you might have to pay the entire cost at the time of service however, the provider can only charge you up to 15% more than the Medicare-approved cost of the service in most cases.
If you use a medical supplier who doesnât accept Medicare assignment, your costs might be higher, and the limiting charge might not apply. See Medicareâs supplier directory for more information.
If you do need to file for reimbursement from Medicare:
Medicare Part B Give Back Benefit
Although many Medicare beneficiaries receive premium-free Part A coverage, they must always pay a monthly premium for Part B coverage. The standard Part B premium in 2022 is $170.10. This amount can really start to add up for those on a fixed income, like Social Security retirement benefits. The Medicare Part B Give Back benefit can help cover some of this cost, and it sometimes even covers your entire Part B premium. So, what exactly is the Give Back benefit, and how does it work? Keep reading as we give you all the details about this plan, including what it is, how it works, and how you can sign up.
Also Check: Where Can I Go To Apply For Medicare
I Receive A Monthly Social Security Payment But I Did Not Receive / Cannot Locate My New Benefit Amount Statement From Social Security What Should I Do
You may call or visit your local Social Security Administration office. You may also access proof of your 2021 Medicare Part B basic premium online at the SSA website: www.ssa.gov/myaccount. You may be required to create or register your SSA account. Please note that once you have an online account, your SSA notifications will be emailed to you.
What Is The Part B Premium Reduction Benefit
The giveback benefit, or Part B premium reduction, is when a Part C Medicare Advantage plan reduces the amount you pay toward your Part B monthly premium. Your reimbursement amount could range from less than $1 to the full premium amount, which is $170.10 in 2022.
While you don’t technically get money back, you do pay the reduced premium amount, which keeps dollars in your wallet. If your premium comes out of your Social Security check, your premium payment will reflect the lower amount. Please note that it could take the Social Security Administration up to 3 months to process your premium rebate. After that time, you’ll see an increase in your check amount.
If you don’t pay your monthly Medicare Part B premiums through Social Security, the giveback benefit would be credited to your monthly statement. Instead of paying the full $170.10, you’d only pay the amount with the giveback benefit deducted.
For example, if you typically pay $170.10 per month, but your MA plan’s giveback benefit is $50, you don’t get $50 back each month. Instead, you’d only pay $120.10 per month . If your plan offers a full $170.10 refund, you wouldn’t have a Part B monthly premium to pay.
Read Also: Is Signing Up For Medicare Mandatory
How To Fill Out Medicare Part B Reimbursement Forms
Some seniors and disabled individuals are automatically enrolled in Medicare Part B, while others must , which can either be done online or by mail.
Those who want to enroll in Medicare Part B must either send or fax the following to their local Social Security office:
- CMS 40B, the enrollment form for Medicare Part B
- CMS L564, the form to request employment information
- Proof of employment
- Proof of Group Health Plan or Large Group Health Plan coverage
Local Social Security offices can be found here. For more information, visit the CMS site for 40B.
Those who are not enrolled in Medicare Part A must first do so. They can apply online here. Those unsure whether or not they have Part A can look on their red, white, and blue Medicare card, which will show Hospital on the lower-left corner.
Alternatively, they can call their local Social Security office or call Social Security at 1-800-772-1213.
It is important that those who wish to sign up for Part B do so quickly, as delaying the process may require them to pay a late enrollment penalty. The form for recurring Medicare Part B services, meanwhile, can be found here.
Helping A Loved One With A Medicare Reimbursement Claim
In some cases, Medicare participants may ask a loved one or other trusted person for help with completing and submitting a Medicare claim, or to check its status. In this instance, an Authorization to Disclose Personal Health Information form must be completed first.
Once submitted, this form enables another person to deal with Medicare on your behalf. They can then give and receive personal information related to your care.
You May Like: What Age Am I Medicare Eligible
Medicare Reimbursement For Medicare Prescription Drug Coverage
Original Medicare does not typically cover prescription drugs you take at home. If you want this kind of coverage, you need to enroll in a stand-alone Medicare Part D Prescription Drug Plan. Or you can enroll in a Medicare Advantage Prescription Drug plan as an alternative way to get your Original Medicare benefits, and thus get all of your Medicare coverage through a single plan. You still need to pay your monthly Medicare Part B premium, in addition to any premium the Medicare Advantage plan may charge.
If you have a Medicare Prescription Drug Plan or Medicare Advantage Prescription Drug plan that doesnât cover a prescription medication your doctor prescribes, you can file an appeal. However, you might first want to speak with your doctor to see if any prescription drug your plan does cover can be substituted.
This website and its contents are for informational purposes only. Nothing on the website should ever be used as a substitute for professional medical advice. You should always consult with your medical provider regarding diagnosis or treatment for a health condition, including decisions about the correct medication for your condition, as well as prior to undertaking any specific exercise or dietary routine.
Before Filing A Medicare Claim
Before filing a claim on your own, Medicare.gov says that participants should first contact the healthcare provider or medical equipment supplier directly and ask them to file a claim for reimbursement. They are required by law to do this for all Original Medicare participant services.
If you have Medicare Advantage which means youre receiving basic Medicare benefits through a private insurance companythis same mandate doesnt apply. That being said, Medicare.gov says that having to file a claim generally only occurs in very rare cases. This suggests that even Plan C providers are still likely to request reimbursement from Medicare directly versus making participants take this action on their own behalf.
Either way, if the healthcare provider or business does not file a claim and you have filed it yourself, you only have up to 12 months from the date of service to do this. So, if youre close to the end of this timeframe, its recommended that you file the claim yourself. And if youre unsure when this one-year period ends, you can call Medicare at 1-800-MEDICARE and theyll provide this information.
Read Also: What Is The Best Medicare Supplement Insurance Plan
Medicare B Reimbursement Included In Some Fehb Plans For Federal Retirees
Reimbursement of Medicare B premiums is included in some Federal Employee Health Benefit plans. If youre retired from the federal government, this can help lower your healthcare costs.
At the age of 65, those who are retired from the federal government are eligible for Medicare B, which covers the costs of ambulance services, some prescription drugs, mental health treatment, and durable medical equipment such as canes and crutches. Choosing to enroll in Medicare B coverage is an important decision for retirees when they become eligible for the coverage. This is because for every full 12-month period that a retiree is eligible but doesnt enroll, theres a 10% penalty added to their monthly premium when and if they do choose to enroll later. Note that the penalty cost will not be reimbursed by any FEHB plan.
Do Some Medicare Advantage Plans Pay For A Portion Of The Part B Premium
premium. Some plans will help pay all or part of your Part B premium. This is sometimes called a “Medicare Part B premium reduction.” The amount you must pay for health care or prescriptions before Original Medicare, your Medicare Advantage Plan, your Medicare drug plan, or your other insurance begins to pay.
Also Check: Is Skyrizi Covered By Medicare
Medicare Part B Premium Reimbursement For 2022
SPECIAL NOTICE: This article only applies to Retired Members and Qualified Surviving Spouses/Domestic Partners of the Los Angeles Fire & Police Pension Plan.
The Centers for Medicare and Medicaid Services has increased the standard Medicare Part B monthly premium to $170.10 effective January 1, 2022 however, you may pay a different amount determined by CMS.
- If you are a new Medicare Part B enrollee in 2022, you will be reimbursed the standard monthly premium of $170.10 and will only need to provide a copy of your Medicare card.
- If you received a Medicare Part B reimbursement of $148.50 or less on your pension check in 2021, you will need to provide documentation to update your Part B reimbursement amount for 2022.
- If you have been receiving a Part B reimbursement that is lower than your basic Part B premium, you may be retroactively reimbursed for your Part B premiums for up to 12 months.
Types Of Provider And How They Assign Out
A healthcare provider can have one of the following statuses in relation to Medicare reimbursement:
- A Medicare-certified provider: Providers can accept assignments from Medicare and submit claims to the government for payment of their services. If an individual chooses a participating provider, they must pay a 20% coinsurance.
- A non-participating provider: These providers have not signed an agreement with Medicare to accept assignments, but they can choose to accept individual patients. They can choose to charge more than the Medicare reimbursement amount for a particular service.
- An opt-out provider: An individual may still be able to visit a healthcare provider who does not accept Medicare. However, they may have to pay the full cost of treatment upfront and out-of-pocket.
Choosing a Medicare-approved healthcare provider means that a person is only responsible for the relevant out-of-pocket cost.
You May Like: How Can A Provider Check Medicare Eligibility
