Medicare Coverage Of Sleep Studies
Medicare Part B covers certain medically necessary sleep study tests if your doctor believes you have obstructive sleep apnea and you have clinical signs and symptoms for this condition you pay 20% of Medicare-approved charges plus any applicable Part B deductible. Medicare covers the PSG test test only if it is performed in a certified sleep lab facility. It may also cover certain types of home sleep study monitors if you have clinical signs and symptoms of obstructive sleep apnea. If youre diagnosed with obstructive sleep apnea, Medicare may also cover a three-month trial for CPAP therapy to determine how well you are responding to treatment for sleep apnea with a CPAP machine.
Because the Medicare coverage requirements are quite specific, its important to talk to your health-care provider about the test being ordered and whether the sleep study lab accepts Medicare assignment to determine your costs for any sleep studies he or she recommends.
Do you have more questions about Medicare coverage for sleep studies at home or in a sleep lab? Im available to discuss Medicare plan options with you at your convenience you can learn more about me by clicking the View profile button below. If you prefer, you can schedule a phone call or request an email by clicking one of the links below. To view plans in your area you may qualify for, click the Compare Plans button.
For more information on sleep studies:
Who Can Interpret A Sleep Study For A Medicare Patient
Once the sleep study is completed and the data is scored, the report is sent to a sleep specialist for review and interpretation. Only a sleep boarded or board-eligible physician can interpret sleep studies for Medicare patients. The physician must meet one of the following requirements:
- Current certification in Sleep Medicine by the American Board of Sleep Medicine or,
- Current subspecialty certification in Sleep Medicine By a member board of the American Board of Medical Specialties or
- Completed residency/fellowship training by an ABMS member board
- Completed all requirements for subspecialty certification in sleep medicine and only until the time of reporting of the first exam which physician eligible or,
How Is Sleep Apnea Diagnosed
According to the National Heart, Lung, and Blood Institute , a doctor can make a diagnosis of sleep apnea based on your medical and family history, a physical exam, and results from a sleep studyyour doctor may recommend a home sleep apnea test or a sleep study test performed in a lab. A sleep study test is the most accurate way to diagnose sleep apnea.
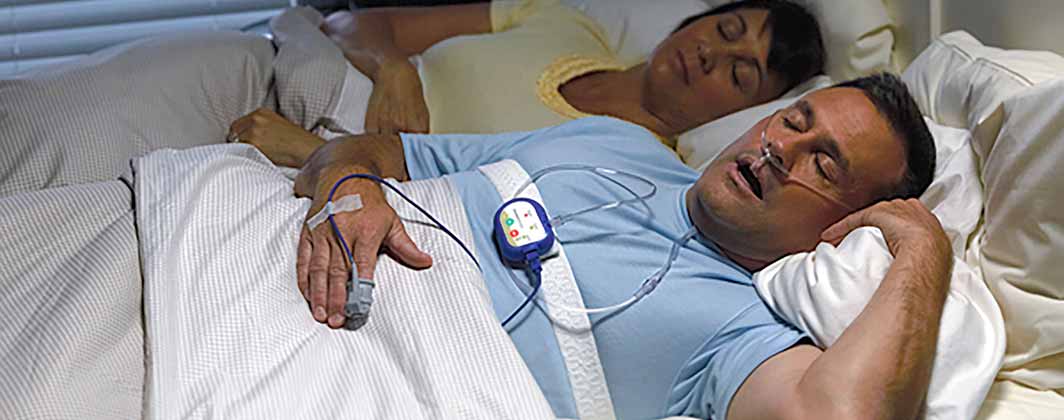
A sleep study can be done at a certified sleep lab or center. During a sleep study, you are connected to a number of health monitors and observed overnight while you sleep. During a home sleep apnea test, you wear a small monitor while you sleep and return the equipment to a sleep specialist who will interpret the results. This can help identify sleep and breathing patterns that suggest sleep apnea.
Also Check: Can I Change Medicare Plans Anytime
Does Original Medicare Cover Cpap Supplies
Yes. Original Medicare helps pay 80% of the cost of the following equipment after youve met your Part B deductible:6
- CPAP machine rental for a 3-month trial if youre newly diagnosed
- CPAP rental for 13 months if youve been using it consistently
- Masks or nose pieces you wear when using the machine
- Tubing to connect the mask or nose piece to the machine
Original Medicare has certain rules for replacing CPAP machine supplies. Contact your doctor or device supplier for more information.
Note: Part B also helps pay up to 80% of the costs of your sleep study if you have clinical signs and symptoms of sleep apnea. Costs covered include Type I, II, III, and IV sleep studies and devices.7
How Can Sleep Apnea Be Treated
There are many ways sleep apnea can be treated. The most common and widely used treatment for moderate to severe sleep apnea is the use of positive airway pressure machines with breathing masks. The mask is worn over the beneficiarys nose during sleep while the machine pumps pressurized air into their airways. This form of therapy is often referred to as continuous positive airway pressure . Alternative forms of treatment for sleep apnea include:
- Wearing an oral/dental appliance
- Palate surgical procedures such as uvulopalatopharyngoplasty , expansion sphincter pharyngoplasty or lateral pharyngoplasty
- Undergoing a weight management program
- Positional therapy
Recommended Reading: Is Medicare Part B Based On Income
What If I Have A Medicare Advantage Plan
Medicare Advantage plans are private insurance products that combine the services offered by original Medicare with some extras, depending on the plan.
These types of plans may offer additional coverage for medical equipment and services that fall under Medicare Part B coverage. The amount youll pay for these devices will depend on the plan you choose and how much you can afford to pay in monthly premiums for the added coverage.
However, some Medicare Advantage plans may place additional restrictions and conditions on the suppliers and providers you can choose based on their network.
If your doctor orders CPAP therapy for you, Medicare will cover 80 percent of the cost of the following equipment after youve met your deductible:
- CPAP machine rental for a 3-month trial if youre newly diagnosed
- CPAP rental for 13 months if youve been using it consistently
- masks or nose pieces you wear when using the machine
- tubing to connect the mask or nose piece to the machine
This Medicare coverage applies only if your doctor and supplier participate in the Medicare program.
You may be asked to pay the entire cost up front and then be reimbursed by Medicare.
If the amount of your equipment is more than what Medicare allows or your supplier doesnt participate in Medicare, you could have to pay more than 20 percent of the cost even the entire amount.
Supplemental Medicare Coverage For Sleeping Problems
Although Original Medicare helps cover seniors with certain sleeping disorders, it does not cover everything. If you have been diagnosed with sleep apnea and need additional coverage, you may want to consider a Medicare Supplement Plan .
Get a quote from Medicare.org. We offer free comparisons for Medicare Advantage Plans , Medicare Supplement , and Medicare Prescription Drug Plans. Contact a licensed sales agent at TTY 711 to help you find the right Medicare coverage for your needs.
You May Like: Does Medicare Cover Depends For Incontinence
Does Medicare Cover Sleep Apnea
Home / FAQs / Medicare Coverage / Does Medicare Cover Sleep Apnea
Sleep apnea is a common condition with which many people struggle. Medicare Part B provides coverage for sleep apnea including doctor visits, sleep studies, and equipment to treat the disorder. Depending on the Medicare plan you have, you may be responsible for a portion of the cost.
Your Cost For A Sleep Study Under Medicare
Sleep studies are considered a diagnostic test and must be ordered by your doctor to qualify for Medicare coverage.
Sleep studies are covered by Medicare Part B. You will owe 20 percent of the Medicare-approved cost of the study, and the Part B deductible applies.
You may owe less if you have supplement insurance, such as Medicaid or a Medigap policy.
If youre enrolled in a Medicare Advantage plan, you may be restricted to sleep centers and clinics within your plans provider network.
Read Also: How Do I Pay Medicare Premiums
How Do I Qualify For Cpap Coverage Medicare Cpap Guidelines
To have Medicare cover your CPAP equipment youll have to meet the following guidelines:
- Be enrolled in Medicare. To enroll, you must be 65 or older and a U.S citizen . You can learn more about enrollment at www.Medicare.gov.
- Be diagnosed with Obstructive Sleep Apnea . This will require a sleep study, which can be performed in-lab or at-home.
- Get a prescription for a CPAP machine. Your prescription must come from a doctor that participates in the Medicare program.
- Order a new CPAP machine from a Medicare-approved DME supplier. We make this part easy! CPAPsupplies.com is an approved durable medical equipment supplier!
- Complete a 90-day Compliance Period. Think of this like a 3-month trial of CPAP therapy. This shows that youre using your CPAP machine and that your CPAP therapy is effective.
Is Sleep Apnea Covered By Medicare
If youve been diagnosed with sleep apnea, Medicare Part B may provide coverage for a three-month trial of Continuous Positive Airway Pressure therapy. Coverage may be extended longer if your doctor determines the therapy is helping.
A CPAP machine is a form of positive airway pressure ventilation that provides a constant level of pressure to the upper airway and is used to help treat sleep apnea. Medicare Part B and Medicare Advantage plans will cover the rental of the machine and the purchase of necessary supplies.
Medicare Part D plans and Medicare Advantage plans with prescription drug coverage may cover medications used to treat sleep apnea and other sleep disorders.
You can compare Medicare Advantage and Part D plans online for free, with no obligation to enroll.
Read Also: Does Costco Pharmacy Accept Medicare
Ama Disclaimer Of Warranties And Liabilities
CPT is provided âas isâ without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose. AMA warrants that due to the nature of CPT, it does not manipulate or process dates, therefore there is no Year 2000 issue with CPT. AMA disclaims responsibility for any errors in CPT that may arise as a result of CPT being used in conjunction with any software and/or hardware system that is not Year 2000 compliant. No fee schedules, basic unit, relative values or related listings are included in CPT. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this file/product is with CMS and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this file/product. This Agreement will terminate upon no upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
What Other Sleep Apnea Devices Does Medicare Cover

People who have mild to moderate sleep apnea or cannot tolerate a CPAP machine are good candidates for oral appliances. Like a sports mouth guard, the oral appliance holds the jaw forward in a way that keeps the airway open. Oral appliances are comfortable to wear and are quieter and more portable than CPAP machines.
If a CPAP machine isnt effective in treating your sleep apnea, its possible that a bi-level positive airway pressure, or BiPAP, machine could work for you. BiPAP machines provide more air pressure for inhalation and less for exhalation than a CPAP machine. Medicare will pay for a BiPAP machine if the beneficiary has obstructive sleep apnea and has tried a CPAP machine but hasnt found relief.
Don’t Miss: How Do I Cancel Medicare Part A
What Is Medicare Cpap Compliance
Once you receive your CPAP or BiPAP equipment, youll begin a compliance period. Think of it like a three-month trial period. This is to demonstrate both that youre using your equipment and that its an effective treatment option for your OSA.
During the compliance period your doctor will monitor how often you use your CPAP. This is recorded by your CPAP device, either through an SD memory card or via Bluetooth connectivity.
To meet compliance, Medicare requires that you use your CPAP machine 1) at least 4 hours per night, 2) for at least 70% of nights, 3) for 30 consecutive days of the first three months.
That can be a little confusing, but what you need to know is: Use your CPAP machine for 30 days in a row, and at least 21 of those days need to be 4 hours or more per night.
Lastly, youll need to meet with your doctor between the 31st and 90th day of the compliance period!
How Much Does A Cpap Machine Cost With Medicare
You will pay a 20 percent coinsurance based on the Medicare-approved amount for a CPAP machine. Medicare Part B covers the other 80 percent of the cost. The Part B deductible applies.
Medicare helps pay to rent your CPAP machine for a total of 13 months, but only if you continue to use it without interruption. After 13 months of rental, you own the CPAP machine.
If you have a Medicare supplement plan , the plan may cover your CPAP coinsurance payment for the rental period. If you have a Medicare Advantage plan , you need to check with the plan for details about what a CPAP machine would cost. Medicare Advantage plans must provide at least the same coverage as Part B, but each plan sets its own cost terms.
Read Also: Does Medicare Cover Lasik Eye Surgery
How Often Will Medicare Cover A Sleep Study
It depends on the circumstances requiring the new study. There is no lifetime limit for sleep studies. Generally, an initial diagnostic PSG and a follow-up titration to evaluate effectiveness should be all that is needed for several months unless their is an extraordinary change in the patients well being. One such example is if the patient is discontinues CPAP therapy or fails during the three-month trial period. Then the testing and trial period must start again.
Medicare will approve additional sleep studies as long as there is a face-to-face evaluation with the patient.
Is A Sleep Study Covered By Insurance Ideas
Is A Sleep Study Covered By Insurance. A home sleep test is a calmer and often more reliable alternative. A recent story on npr news reported that half of all patients win their appeal of denials by health insurance companies.
A sleep study is performed on a patient with suspected osa. Alternatively, a home sleep study is affordable and convenient.
Also Check: Does Medicare Supplemental Insurance Cover Pre Existing Conditions
Diagnosing Sleep Apnea At Home
Getting a sleep apnea diagnosis does not need to be a stressful experience. You should always make regular visits to your doctor, but, if they want you to get tested for sleep apnea, they will just refer you to a sleep lab or a home sleep test provider. Rather than jumping through costly, drawn-out hoops, you are able to diagnose your sleep apnea at home with a home sleep testing kit.
Most at-home sleep testing kits do not even required a referral. You can take our patient questionnaire to see if you are a good candidate for sleep testing, and receive your kit in as few as 2-3 business days. Dont wait because your home sleep testing kit is the first step to a better nights sleep and a better quality of life.
Cms Requirements For Nocturnal Supplemental Oxygen
*People who require oxygen during the day do not fall under these rules*
- No home testing is allowed currently.
- CMS will no longer pay solely for Nocturnal Supplemental Oxygen should patient have the diagnosis of Sleep Apnea. The Sleep Apnea patient must be using PAP therapy in order to be in consideration for oxygen.
- Should a person show non-compliance:
- They will not have oxygen approved by CMS
- They will not get PAP supplies approved by CMS
- If the PAP machine is a newly purchased, this too will be not approved by CMS and they will have the DME pick up the machine from your house.
- The entire process will have to be started over per CMS guidelines
Don’t Miss: What Age Am I Medicare Eligible
What Is A Cpap Machine
If you have OSA, continuous positive airway pressure machines, opens new window are one of the most common treatments. A CPAP machine is a device with a face or nose mask attached to a small pump. The pump pushes pressurized air through a hose, into the mask and into your airway. The steady flow of air keeps the airway open to improve breathing and sleep quality. Some people may require extra CPAP supplies like humidifiers and heating tubes for effective treatment.3
Does Medicaid Cover Sleep Studies

- If you might have a sleep disorder, your doctor could order a clinical sleep study to learn more. Find out whether Medicaid will cover any costs for a sleep study.
If your doctor believes you’re exhibiting signs of sleep disorders, he may refer you to a polysomnography more widely known as a clinical sleep study. These studies require overnight evaluation to diagnose the severity of your symptoms and how they’re affecting your sleep continuity, cardiac functions and other factors. This may be in the form of a sleep lab study or a home test. Find out more about whether Medicaid covers sleep studies below.
Recommended Reading: Does Medicare Cover Cpap Masks
If Youve Already Been Diagnosed With Sleep Apnea
The good news is that under the Affordable Care Act insurance providers are not allowed to discriminate against people with preexisting conditions, including sleep apnea. In addition, patients cannot be denied coverage or charged more because of their diagnosis of sleep apnea.
A PAP machine is considered durable medical equipment , which means it may be subject to a new tax under the Affordable Care Act. Patients with Medicare are able to test a PAP machine for three months, and if the results are shown to be beneficial, Medicare will rent it for a period of 13 months prior to purchasing it.
Most insurance plans will continue to cover the costs of a PAP machine, but will require proof of patient compliance from the equipment provider before they pay for on-going device rental, purchase or additional replacement supplies.
In fact, most insurance compliance guidelines require that you show proof of using your device for a minimum of 4 hours per day at least 22 days out of a consecutive 30 day period within the preceding 90 days .
Dont Miss: Do I Qualify For Medicare If I Am Disabled
