Does Medicare Cover Acupuncture For Allergies
Acupuncture is sometimes used to treat allergies. Some Medicare Advantage plans help cover acupuncture even though it is considered alternative medicine and is not covered by Original Medicare.
Note: coverage and costs will vary depending on the Medicare Advantage plan youre enrolled in, and not every Medicare Advantage plan covers acupuncture.
A licensed insurance agent can help you compare Medicare Advantage plans in your area and get you enrolled in a plan that works for you.
Find Medicare Advantage plans in your area
Or call 1-800-557-6059TTY Users: 711 to speak with a licensed insurance agent. We accept calls 24/7!
Get the Scoop!
Join our email series to receive your Medicare guide and the latest information about Medicare and Medicare Advantage.
Medicare Advantage Coverage For Allergy Tests
Medicare Advantage, also known as Medicare Part C, refers to private insurance plans that are regulated by the federal government. If you are eligible for Medicare, you will have a choice between Original Medicare and Medicare Advantage. Original Medicare refers to Part A and Part B of Medicare.
Medicare Advantage is required to cover everything that Original Medicare does. However, Medicare Advantage plans may also cover things that Original Medicare doesnt cover. Some Medicare Advantage plans come bundled with prescription drug plans but can also provide dental coverage or wellness benefits.
These additional benefits will vary a lot between plans. When you compare plans, ask if there are any extra benefits that are related to allergy care. It may be easier to get testing done, and additional therapies could be covered.
Medicare Covers Allergy Tests When:
- You are in an environment with a reasonable probability of exposure to the substance in question.
- The test correlates with your history and physical findings.
- The test technique used for allergen detection provides accurate results in scientifically valid medical studies published in peer-reviewed literature.
You May Like: How To Pay For Medicare Without Social Security
When Does Medicare Cover Allergy Testing
The basic principle behind Medicare coverage for allergy tests is medical necessity. Medicare defines medically necessary services as “Health care services or supplies needed to diagnose or treat an illness, injury, condition, disease, or its symptoms and that meet accepted standards of medicine.”
This means that if you wanted to get an allergy test without guidance from any provider, Medicare would not cover it. However, if a Medicare-credentialed healthcare provider confirms that you need to be tested, then it will be covered by Medicare once you meet your Part B deductible.
Confirming medical necessity is just one of the requirements. Your provider will also need to state that your allergic symptoms arent being managed by other methods and that the allergy testing is part of a larger treatment plan. The doctor and lab that administer the testing must accept Medicare assignment.
Most people who have severe allergies can meet these requirements easily. If you have questions about your specific scenario, you can contact Medicare at 1-800-633-4227. Your physician should also be able to answer any questions you may have.
Does Medicare B Pay For Allergy Shots
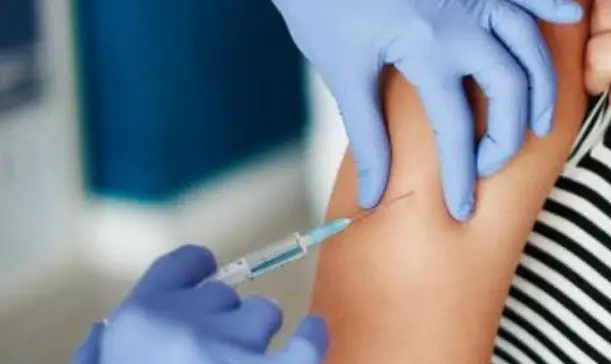
Medicare can pay for a portion of your allergy shots if a doctor determines allergen immunotherapy is medically necessary. If you qualify for coverage, Part B will often pay 80%, leaving you with a 20% copay once your deductible is met.
Part C may also cover your allergy shots. Medicare Advantage plans offer at least the same Part B coverage, but you may have different copays and coinsurance based on your plans details. If you have to see a different doctor or a specialist for your allergy treatment, make sure that the provider is in your Medicare Advantage network, or you could wind up paying for 100% of the costs.
What extra benefits and savings do you qualify for?
Also Check: Does Medicare Pay For Medical Alert Bracelets
What To Expect When Getting Allergy Shots
It is important to note that allergy shots may take years to function, and you should visit your doctors office for every injection. If you break the injection cycle, you may need to repeat the process, depending on the duration you took the shots. Common reactions can include the following.
- Sneezing
- Swelling, redness, or irritation at the shot site
- Nasal congestion
Some individuals may experience a severe reaction, referred to as anaphylaxis, which may be fatal if not treated immediately. That is why you receive an it in the physicians office, where they will watch you for a minimum of 30 minutes to ensure you do not have a serious reaction.
Do Medicare Advantage Plans Cover Allergy Testing
Medicare Advantage Plans can be purchased through Medicare-approved private insurers. They provide the same benefits as regular Medicare, which means that they will cover any allergy tests covered by Medicare Part B if you’re eligible.
Medicare Advantage Plans may include additional benefits not covered by Original Medicare, such as dental treatment, prescription drugs and vision care. Coverage varies according to provider, and some policies may cover allergy treatments not included in Medicare Part A or B. For example, Original Medicare doesn’t cover acupuncture to treat allergies, but it may be included in certain Medicare Advantage Plans.
Don’t Miss: Does Medicare Cover You When Out Of The Country
What Allergy Tests Does Medicare Cover
Medicare only covers allergy tests proven toprovide accurate and effective results for specific types of allergens.
For example, Medicare typically covers percutaneous tests leading to IgE-mediated reactions tosuspected allergens, such as:
- inhalants
- specific types of medications, such as penicillin
- insect stings or bites
- food
If the percutaneous tests show up negative, your doctor may suggest intracutaneous, or intradermal, testing.
These tests involve the injection of a small amount of an allergen into your skin. They may be covered by Medicare if IgE-mediated reactions occur to suspected allergens, such as:
- inhalants
- specific types of medications
- insect stings or bites
Talk with your doctor to see if Medicare will cover your particular allergy testing needs and treatment. Usually, it comes down to your particular Medicare plan and your doctors certification that the testing is necessary, reasonable, and part of a treatment program that:
- is safe
Is Allergy Test Covered By Medicare
There are several types of Medicare-approved allergy tests your doctor can perform if you qualify. Not all allergy tests are accepted by Medicare, however. Ensure your doctor verifies that your allergy testing meets the Medicare requirements if you need it covered by Part B. As a guide, Medicare typically covers the following types of allergy testing:
- Skin tests to examine your bodys allergic reaction to different substances, including pollen, pet dander, and more
- Intradermal tests under the skin if needed following standard skin tests
- Blood testing to examine your bodys antibodies
- Outpatient food challenge testing to determine your bodys food allergies
Read Also: Does Medicare Cover Bladder Control Pads
When Does Medicare Part B Pay For Allergy Shots
Medicare does not have specific guidelines about how it covers allergy shots and allergy treatments. Coverage decisions are made on a case-by-case basis and may depend on the types of allergies you have and their severity.
If your doctor determines that an allergy shot is medically necessary, Medicare Part B or a Medicare Advantage plan may cover the cost of your shot.
A doctor may determine your allergy shots are medically necessary for one of the following reasons:
If Medicare covers your allergy shot, you will typically pay a 20% coinsurance or copay after you meet your annual Part B deductible, which is $203 in 2021.
All Medicare Advantage plans are required by law to provide at least the same minimum coverage as Medicare Part A and B, so a Medicare Advantage plan will also cover at least 80% of the cost of your allergy shots if your doctor says they are medically necessary.
Compare Medicare Advantage plans online to find the best plan for you. You may be able to find a plan that covers your allergy shots and other allergy medication you need.
If Your Doctor Thinks It’s Medically Necessary Medicare Typically Covers Allergy Testing
Medicare covers allergy testing, but only in certain circumstances. Allergy tests are used by physicians to get a better understanding of which allergies affect you. If you are dealing with serious allergies, your physician may order a series of allergy tests that can provide them with the information they need to create an allergy treatment plan for you.
Certain types of allergy tests may not be covered if you dont fulfill a number of requirements. This article explains which tests Medicare will pay for and when.
Don’t Miss: Is Wellcare The Same As Medicare
Patch Testing With Metal Alloy Discs
Thomas and associates noted that intolerance reactions to metal implants may be caused by metal allergy. However, prior to implantation, prophetic/prophylactic patch testing should not be performed. Pre-implant patch testing should only be done to verify or exclude metal allergy in patients with a corresponding history. In case of implant-related complications — in particular following replacement arthroplasty — such as pain, effusion, skin lesions, reduced range of motion or implant loosening, orthopedic causes should be ruled out first. Work-up of suspected metal implant allergy should then be done using the Deutsche Keramische Gesellschaft standard series, which includes nickel, cobalt, and chromium preparations. Various studies assessing the usefulness of metal alloy discs for patch testing have shown this particular approach to be ineffective with respect to providing reliable information on metal allergy. Any positive reaction in such tests cannot be assigned to a specific metal contained within the alloy. Furthermore, there is a risk of broad and indiscriminate use of these readily available discs. Accordingly, given the lack of additional benefit compared to patch testing with standardized metal salt preparations, the authors, on behalf of the DKG, did not recommend patch testing with metal alloy discs.
Chronic Urticaria Index Testing

Cho et al compared the prevalence of basophil-activating autoantibodies in patients with CU, rheumatoid arthritis , and systemic lupus erythematosus . Clinical characteristics and laboratory studies were examined for an association with the CU Index. Adult patients, 27 with CU, 27 with RA, and 26 with SLE, and 20 healthy controls were compared on the basis of the CU Index panel, anti-IgE, and anti-thyroid antibodies. The CU Index values were significantly higher in the CU group when compared with the RA group but not when compared with the SLE group. 33 % of CU, 23 % of SLE, 3.7 % of RA, and 15 % of controls had a positive CU Index. Elevated anti-thyroid antibody levels did not correlate with a positive CU Index in any of the groups. An elevated CU Index in the SLE group was not associated with age, sex, ethnicity, disease severity, or history of atopy. The authors concluded that the CU Index values were elevated in patients with CU and SLE. The presence of these autoantibodies did not correlate with disease activity or presence of thyroid antibodies. They stated that functional autoantibodies may not be specific for CIU, and their role in non-urticarial systemic autoimmune diseases requires further investigation.
You May Like: How Long Does It Take To Get Medicare B
Does Tricare Cover Allergy Medicine
The U.S. Department of Health and Human Services provides prescription allergy medications and testing through TRICARE. The Food and Drug Administration regulates drugs. As well as over-the-counter allergy medications, TRICARE also covers the active ingredients cetirizine and loratadine without out-of-pocket costs for beneficiaries. If you have a prescription, you can get them covered.
Cost Of Allergy Shots
The cost of allergy shots may vary depending on the coverage plan and incidental costs. It will also depend on if you meet the eligibility requirement of Medicare. When beginning treatment, you will generally receive two shots every week over six months. Your costs have two parts:
- Administrative fees for the physician and the medical center
- The allergy serum
Without insurance, shots can cost between $1,000 and $4,000 every year or more when treatment begins. At the maintenance phase, you will receive one or two shots per month for around 3-5 years to lower the costs at that time.
You May Like: What Age Do You Register For Medicare
Allergies Can Be Very Troublesome Call Us Today For Treatment
If you are suffering from allergies, do not feel lonely. Many individuals experience uncomfortable symptoms triggered by daily exposure to allergens like cat dander, dust mites, and pollen. Other people experience seasonal allergies, whereas some experience symptoms throughout the year. Although over-the-counter allergy medications are available, many individuals may require to see an allergy doctor in Los Angeles. Treatment for serious allergies might include allergy shots and prescription medications. If you qualify for Medicare, you might be questioning what care your insurance might cover and how much you should pay from your pocket. Lets explore how much allergy shots might cost and how they can benefit you with Medicare.
Ama Disclaimer Of Warranties And Liabilities
CPT is provided as is without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose. AMA warrants that due to the nature of CPT, it does not manipulate or process dates, therefore there is no Year 2000 issue with CPT. AMA disclaims responsibility for any errors in CPT that may arise as a result of CPT being used in conjunction with any software and/or hardware system that is not Year 2000 compliant. No fee schedules, basic unit, relative values or related listings are included in CPT. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this file/product is with CMS and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this file/product. This Agreement will terminate upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
You May Like: Is Medicare Advantage Part Of Medicare
American Hospital Association Disclaimer
The American Hospital Association has not reviewed, and is not responsible for, the completeness or accuracy of any information contained in this material, nor was the AHA or any of its affiliates, involved in the preparation of this material, or the analysis of information provided in the material. The views and/or positions presented in the material do not necessarily represent the views of the AHA. CMS and its products and services are not endorsed by the AHA or any of its affiliates.
Does Insurance Cover Allergy Treatment
The majority of allergy shots are covered by health insurance. It is possible that you will have to pay a copay for each visit. A copayment is usually a nominal fee. The cost of allergy shots can be thousands of dollars a year if you do not have health insurance, have a high deductible, or do not have allergy shots covered by your plan.
You May Like: How To Win A Medicare Appeal
Igg4 Testing For The Evaluation Of Allergy
The AAAAI stated that Dont perform unproven diagnostic tests, such as immunoglobulin G testing or an indiscriminate battery of immunoglobulin E tests, in the evaluation of allergy. Appropriate diagnosis and treatment of allergies requires specific IgE testing based on the patients clinical history. The use of other tests or methods to diagnose allergies is unproven and can lead to inappropriate diagnosis and treatment. Appropriate diagnosis and treatment is both cost effective and essential for optimal patient care.
Does Medicare Cover Allergies
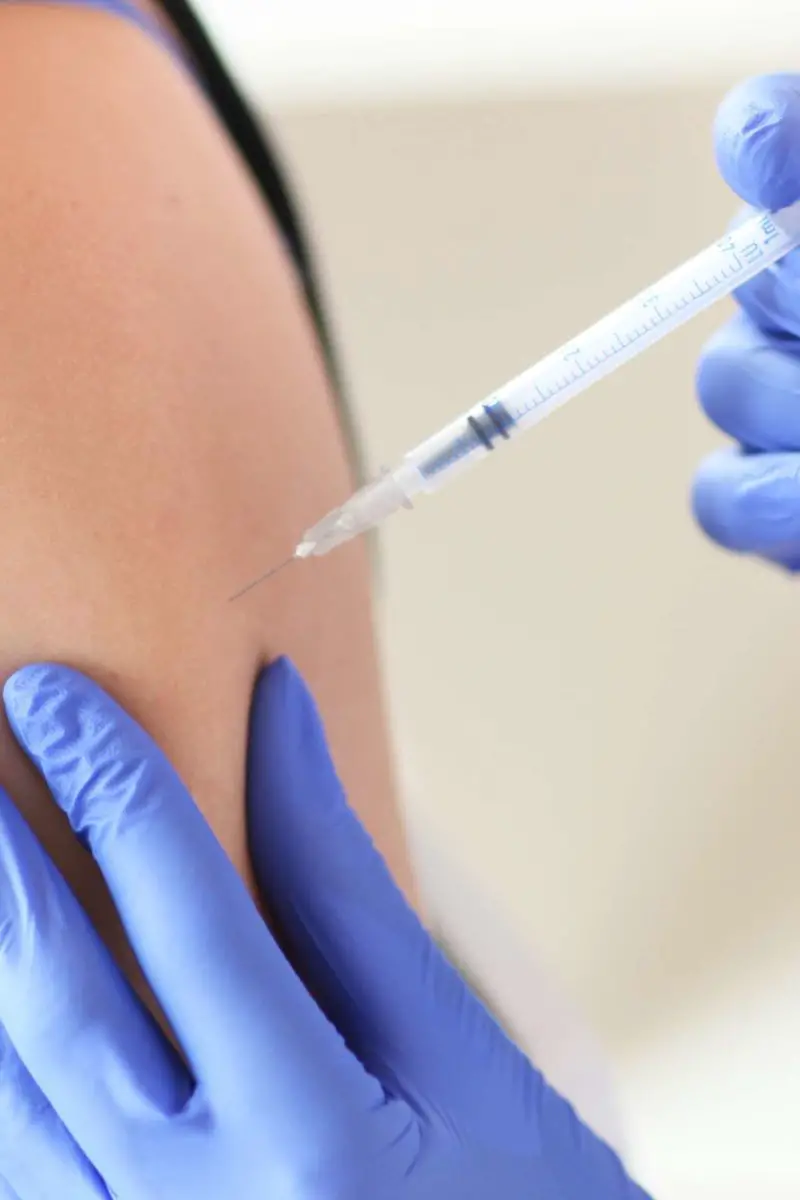
Allergies affect more than 50 million Americans every year, but reactions range from inconvenient sneezing or coughing fits to more severe, life-threatening events. While some people can manage occasional or seasonal allergies with over-the-counter drugs, many people face a more consistent need for treatment from a medical professional. According to the Centers for Disease Control and Prevention , allergies are the 6th leading cause of chronic illness in the United States, and seniors can be especially vulnerable to serious complications. If you are 65 years of age or older, or under 65 with certain disabilities, and are enrolled in Medicare, your insurance can help you get the allergy care you need at a price you can afford.
What are Allergies?
Allergies are an overreaction of the immune system, and while allergies cannot be prevented, they can be controlled by medication and immunotherapy when avoidance is not an option.
Types of Allergies
There are many types of allergies that can affect your daily activities and overall health. The most common allergic diseases include:
- Asthma
If you experience any of these issues, please call your physician immediately.
How Can Medicare Help?
Also Check: What Medications Are Covered By Medicare
How Do I Get My Insurance To Cover My Allergy Testing
Unfortunately, there is no way to guarantee that a health care plan or insurance policy will cover allergy testing. Most insurers and state and federal plans only cover medically necessary allergy testing. Therefore, your doctor needs to provide as much evidence as possible of your need for testing.
Your provider may restrict the types of allergy tests it covers, which means it may not fund your doctor’s preferred testing regimen. In this situation, you may wish to consider asking your doctor if there is a suitable alternative covered by your policy.
How Do I Bill For An Allergy Test
CPTallergy testingCPTtestingallergytestingtestingtests
. Correspondingly, what is the CPT code for allergy testing?
If percutaneous or intracutaneous single test and “sequential and incremental” tests are performed on the same date of service, both the “sequential and incremental” test and single test codes may be reported if the tests are for different
what is procedure code 86003? Quantitative or semi-quantitative in vitro allergen specific IgE testing is covered under conditions where skin testing is not possible or is not reliable. The number of tests done, frequency of retesting and other coverage issues, are the same as for skin testing.
Simply so, how do I bill for allergy shots 2019?
Use CPT procedure codes 95115 and 95117 to report the allergy injection alone, without the provision of the antigen.
Does Medicare pay for allergy testing?
Medicare Part B may cover allergy testing if your clinically significant allergic history or symptoms are not manageable by therapy. Medicare Advantage also cover allergy testing when medically necessary. Most Medicare Advantage plans also offer additional benefits, such as prescription drug coverage.
Also Check: What Is The Difference Between Medicare Advantage And Regular Medicare
