Is Coolief Covered By Medicare
Medicare should cover Coolief treatment. Although, we recommend confirming with your doctor and insurance provider. This method of treatment doesnt require any incision, no overnight hospital stay, and pain relief can last up to 12 months.
Most patients report an increase in mobility. In the Coolief clinical study, they found the treatment was longer-lasting and gave greater pain relief than the steroid injections. However, there are risks to all medical procedures discussing your options with your doctor is very important.
Find Medicare Plans in 3 Easy Steps
We can help find the right Medicare plans for you today
The Benefits Of Getting A Flu Shot
Influenza is a common and potentially serious viral infection that can lead to hospitalization and sometimes even death. Receiving the annual flu vaccine is one of the best ways to protect against infection and subsequent complications, reports the CDC.
The flu shot can:
- Reduce the risk of flu illness by 40% to 60% among the general population during seasons when current flu viruses are well-matched to those used to make flu vaccines
- Reduce the severity of illness in people who get vaccinated but still get sick
- Prevent millions of illnesses and flu-related doctor visits annually
- Reduce the risk of flu-associated hospitalization
- Help protect people around the person who gets vaccinated
The CDC currently recommends that adults at least 65 years old receive either a higher dose or adjuvanted flu vaccine over the standard dose vaccine for additional protection, due to the fact that older adults are at higher risk of having serious health complications from the flu. The three recommended vaccines include the Fluzone High-DoseQuadrivalent vaccine, Flublok Quadrivalent recombinantflu vaccine and Fluad Quadrivalent adjuvanted flu vaccine. All of these vaccines are quadrivalent vaccines, meaning they protect against four flu viruses.
Does Medicare Cover Synvisc
Medicare Part B may cover Synvisc if your doctor deems it medically necessary to treat your knee pain due to osteoarthritis after other conventional therapies fail to treat your pain.
If you have a Medicare Advantage plan, your plan will cover qualified Synvisic treatment that would be covered by Medicare Part B.
Many Medicare Advantage plans also include coverage for other prescription drugs that may not be covered by Original Medicare.
Find Medicare Advantage plans with drug coverage
Or call 1-800-557-6059TTY Users: 711 24/7 to speak with a licensed insurance agent.
You can also compare Part D prescription drug plans available where you live and enroll in a Medicare prescription drug plan online when you visit MyRxPlans.com.
You May Like: Must I Sign Up For Medicare At 65
How Much Will Medicare Pay For Total Knee Replacement
If its an inpatient surgery, Medicare will cover most of the cost. Youll be responsible for the Part A deductible, as well as additional cost-sharing in the form of coinsurance. If its an outpatient surgery, Medicare will cover 80% of the cost.
Youll be responsible for the Part B deductible and 20% of the cost. Any prescriptions given at the hospital will also be covered under Part B. Any prescriptions that youre prescribed to take at home wont have coverage unless you have a stand-alone Part D plan. Or, if you have an Advantage plan that covered prescriptions.
If you have a Medigap plan, depending on the letter plan you enrolled in, you could have zero out of pocket costs for total knee replacement surgery. If you have a Medicare Advantage plan, youll have to check with the carrier you enrolled with to determine what youll have to pay out of pocket.
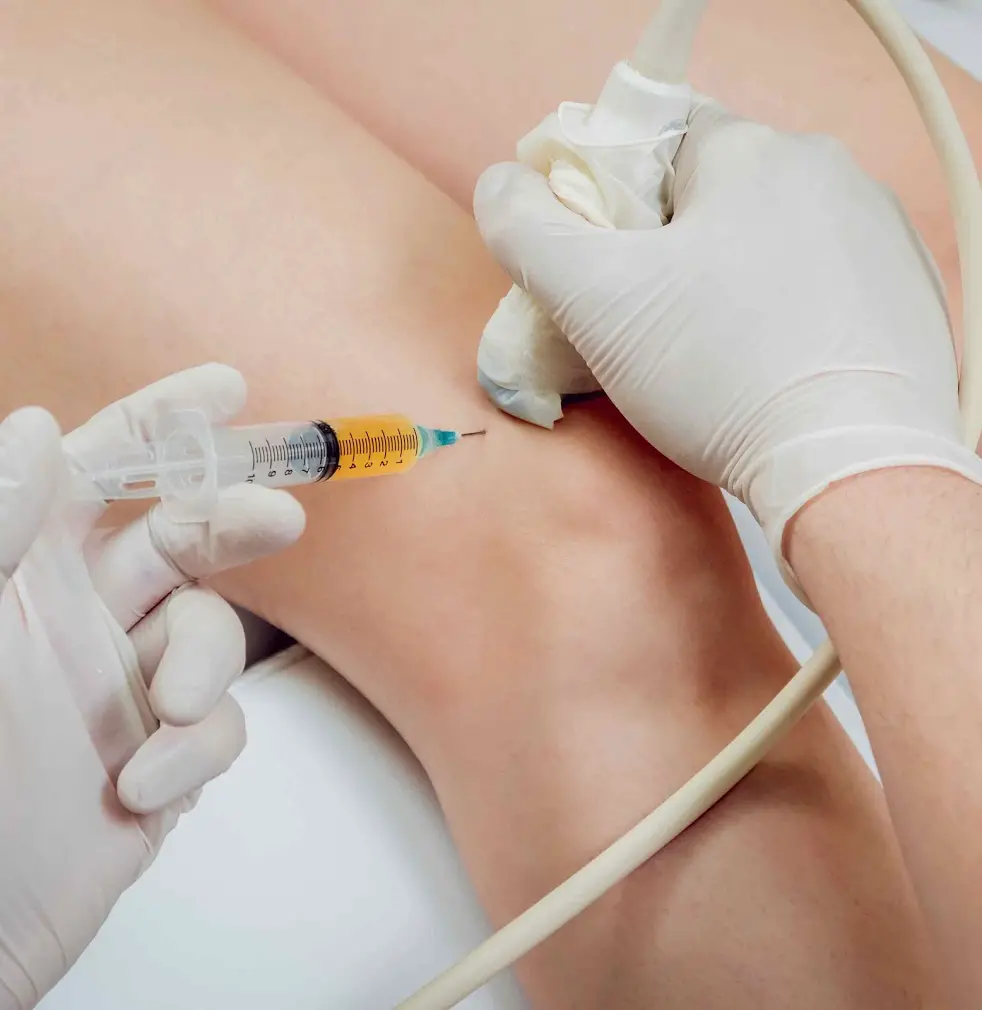
What Are Knee Gel Injections
In cases of severe knee osteoarthritis, many physicians may suggest either having knee replacement surgery or treatment with gel injections in the knee. The gel injection treatment is non-invasive and helps by temporarily relieving the pain and restricted mobility that comes with osteoarthritis.
Knee gel injections, also known as viscosupplementation, are gels that consist of hyaluronic acid, a substance found naturally in the synovial fluid around all the joints. A supplement of this fluid, injected into the knee, can provide better lubrication and cushioning so the joint bones dont rub together.
Don’t Miss: How Much Do Medicare Supplements Increase Each Year
Does Medicare Advantage Cover Hyaluronic Acid Injections
Generally, Medicare Advantage plans must cover at least as much as Medicare Parts A and B do. As a result, your plan is likely to at least match the coverage provided by Original Medicare if you’re eligible for Synvisc injections. You may need to receive the injection at a hospital, clinic or doctor’s office in your plan’s network and will likely be responsible for a copay or coinsurance. Your insurance provider can give you more information about coverage for hyaluronic acid injections.
Different Types Of Knee Injections
Here are a few of the most common types:
- Corticosteroid When injected in the knee or other joints, Corticosteroid injections reduce pain and inflammation. These effects generally last for 2-3 months. A patient can only receive a limited number of these injections per year.
- Platelet-Rich Plasma PRP shots use a patients plasma to promote healing of the soft tissue and reduce inflammation. Doctors frequently use these injections to treat osteoarthritis, as they are low risk and have limited side effects.
- Hyaluronic Acid Injections or Viscosupplementation These are the technical terms for knee gel injections. As outlined above, a Hyaluronic Acid injection reduces pain and inflammation by mimicking the effects of natural joint fluid. They are best for patients with diabetes, as they do not raise blood sugar levels like Corticosteroid shots. Gel-One is one of the most commonly prescribed forms of HA treatment.
Recommended Reading: How Much Is Medicare Deductible Per Year
Finding A Specific Code
Some articles contain a large number of codes. If you are looking for a specific code, use your browser’s Find function to quickly locate the code in the article. Sometimes, a large group can make scrolling thru a document unwieldy. You can collapse such groups by clicking on the group header to make navigation easier. However, please note that once a group is collapsed, the browser Find function will not find codes in that group.
How Much Do Knee Gel Injections Cost
Knee gel injections cost can vary. But, on average in the United States you can expect that each injection could be about $1,200.
Remember, the amount you pay will vary based on youre the Medicare coverage you have.
Original Medicare will cost 20% coinsurance. Knee gel injections covered by insurance will vary based on the carrier and plan you have.
If you have a Medicare Supplement Plan paired with Original Medicare your could be lower.
Medigap Plan Coverage Examples:
So, if you have a Medicare Advantage Plan , the cost will vary depending on the carrier and plan you have.
Talk to a licensed insurance agent today that can help determine what your insurance. Call 866-633-4427 and one of our friendly, licensed team will help you.
Don’t Miss: Does Medicare Part D Cover Shingrix Vaccine
How Many Times Can You Get Gel Shots In Your Knee
You can receive knee gel treatment every 6 months.
Depending on the type of gel used, you may need more than one shot per treatment, administered over the course of several weeks.
Some patients have had injections done for years to help delay knee surgery.
Results may vary and its best to consult with your physician about your condition.
Are There Any Side Effects
While all medicines can potentially have side effects, some patients may experience them and others may not. Side effects associated with joint fluid replacement injections are generally quite rare but can include the following:
- Mild pain and swelling around the site of the injection, which usually goes away within a few days
- A rash or hives and itching
- Breathing difficulties
Your doctor will be able to advise you about any potential side effects before beginning treatment. You should always seek medical attention if you experience any side effects after receiving a joint fluid replacement injection.
What’s next?
Don’t Miss: When Can You Get Medicare Health Insurance
How Much Does A Three
Drugs.com reports that the average cost of one 2mL Synvisc injection is around $417 and that a three-dose course usually costs a little more than $1,000. However, exact pricing varies depending on your plan and pharmacy.
If you have Original Medicare and your Synvisc injections are covered by your Medicare coverage, a Medicare Supplement plan could help pay your Medicare copays, deductibles and other out-of-pocket costs.
Which Providers Accept Medicare For Flu Shots
Many hospital networks, health care providers and pharmacies nationwide accept Medicare for flu shots. Contact your preferred provider to learn whether they accept Medicare for annual flu vaccinations before scheduling your appointment. You can also visit Medicare.gov and use its provider search tool to determine who in your care network accepts Original Medicare, the coverage used for flu vaccinations.
Don’t Miss: Does Medicare Pay For Stairlifts
How Much Do Vaccines Cost
The cost for vaccines depends on which portion of Medicare is paying and what the vaccine is.
You wont pay anything for vaccines that Medicare Part B covers. But if you have Medicare Part C , you should check with your insurance plan.
You may need to get your vaccine from a plan-approved provider or pharmacy. If youre following the rules of your Medicare Advantage plan, you shouldnt have to pay anything for your vaccine.
If you get a vaccine that Part D covers, your Part D insurance company will negotiate a price that includes the vaccine costs and its administration. The costs include:
- vaccine administration fee
- vaccine ingredient costs
Your doctor will bill your Part D plan directly. You may be responsible for costs that include a copayment or coinsurance.
Sometimes, your plan may require you to pay your provider up front for the Medicare Part D vaccine, then submit a claim to your Part D plan for reimbursement. When this is the case, you may want to contact your plan before getting the vaccine just to confirm your coverage.
Which Vaccines Does Medicare Cover
Vaccines are important for preventing illness and keeping you well. Because vaccines may get less effective over the years, you may need to talk with your doctor about how frequently you should get certain ones.
Medicare Part B is the part of original Medicare that covers medical costs. It also covers several immunizations. These include:
- hepatitis B vaccines
- influenza vaccine
Don’t Miss: What Does Medicare Part B Cover
Indications For Tdap Vaccination
In addition to the standalone tetanus shot, it is also recommended that you get at least one Tdap booster as an adult, which protects against tetanus, diphtheria, and pertussis . It is also recommended during the third trimester of pregnancy.
However, the Tdap vaccine is currently not covered under the Part B benefit and may or may not be covered by your Medicare Advantage plan or Part D plan. Check your plan’s formulary.
What Is A Synvisc Injection
Synvisc is an injection that lubricates the knee joints. Synvisc is also known by its chemical name, Hylan G-F 20.
The medication contains an active ingredient known as hyaluronate. Hyaluronate lubricates and cushions joints, and as a result, it reduces the pain in the knees.
Like many other medications, Synvisc has its fair share of side effects. Major side effects that users may experience include bruising, swelling, discoloration of the skin in the injected area, stiffness, and mild pain in the knees or the area near it.
The treatment course for Synvisc involves one injection each week for three weeks. So, three injections total. Synvisc must only be administered by an experienced healthcare provider who has proper knowledge and experience in injecting medications.
Don’t Miss: Does Medicare Pay For Power Chairs
Bluewave Insurance Is Here To Help
So, does Medicare cover for knee gel injections? Yes, Original Medicare does pay for knee gel injections. However, that doesnt mean that everyone with Medicare coverage qualifies.
You will still need to show proof that you have osteoarthritis, and that other treatments have been ineffective. Even though Medicare covers part of the costs, you may still need help paying for drugs, deductibles, or copayments as well. This is where an MAPD or Medigap insurance plan with Bluewave Insurance can help.
thumb
If you have any further questions about Medicare or want to learn more about cost-sharing Medigap options, call us attoday!
Types Of Gel Injections For Knees
There are several brands of hyaluronic acid for knee injections.
Consult with your physician about which brand of gel use for treatment. In some cases, it can be a single shot. Or you may have to get 3-5 injections spaced a week apart.
After receiving treatment, you should plan on limited weight-bearing activity for 1-2 days.
Also Check: Will Medicare Pay For Lasik Eye Surgery
When Does Medicare Pay For Synvisc
Generally, Medicare pays for Synvisc when deemed medically necessary under the definition established by the program. When Medicare covers Synvisc, how much you can expect to pay for Synvisc out of pocket depends on where you’re receiving treatment and what type of coverage you have as this article will discuss.
Medicare Part A and Part B are often referred to as Original Medicare. Your Original Medicare benefits can help pay for an osteoporosis injectable drug and visits by a home health aide nurse to inject the drug if you meet certain conditions, according to Medicare.gov the official Medicare website:
- Youre a woman.
- Youre eligible for Part B and meet the criteria for Medicare home health services.
- You have a bone fracture that a doctor certifies is related to postmenopausal osteoporosis.
- Your doctor certifies that youre unable to learn to give yourself the drug by injection and your family members or caregivers are unable and unwilling to give you the drug by injection.
If you have a Medicare Advantage Prescription Drug plan or a Medicare Part D Prescription Drug Plan , your play may offer additional Synvisc coverage. Speak with your plan carrier directly for more information.
If you’re comparing new Medicare Advantage plans or new Medicare Part D drug plans and looking for a plan that helps pay for Synvisc, you can request free plan quotes online or call to speak with a licensed Medicare insurance agent.
What Is The Procedure Like Will It Hurt
Each injection takes just a few minutes and is done in the office. Local numbing medicine is applied and the skin is prepared and cooled, all decreasing if not eliminating the mild discomfort of the injection. You may feel some pressure but rarely is it painful. In some cases the Synvisc-One is accompanied by a cortisone injection without having to make a separate injection.
Read Also: Does Medicare Pay For Visiting Nurses
Additional Coverage For Knee Treatment And Therapy
While Original Medicare will provide coverage for knee replacement surgery and gel injections, it may not cover other treatments. For example, if you need prescription drugs to manage your pain, youll need to get extra coverage. You could get drug coverage with a Part D or Medicare Advantage Prescription Drug plan .
That said, Original Medicare will cover most knee therapies. Medicare Part A covers inpatient surgeries, while Medicare Part B covers outpatient physical therapy. Part B also covers doctors visits and Durable Medical Equipment .
Call us at to compare Medicare plans that may cover knee gel injections
Does Medicare Cover Booster Shots
As of July 2022, a first booster shot is being recommended five months after a Pfizer or Moderna primary series and two months after a J& J primary series. A booster regimen has not yet been established for Novavax. That said, people who are immunocompromised only need to wait three months for their first Pfizer or Moderna booster.
The CDC is currently recommending a second boost shot for people 50 and older and for people who are immunocompromised. It can be given four months after the first booster dose.
The CDC is recommending booster shots using Pfizer and Moderna vaccines, regardless of the type of vaccine you got for the primary series. Medicare is going to pay for these boosters, no matter which manufacturer it is. All boosters are being covered by Medicare and Medicare Advantage at no cost to the Medicare recipient.
Also Check: Will Medicare Pay For Hospice Care
How Many Vaccine Doses Does Medicare Cover
The number of doses of vaccine you get will vary based on your medical history and the specific vaccines you get. You could be eligible for as many as five covered doses. The following summarizes COVID vaccines for adults, not children, based on what primary series was used.
- Pfizer or Moderna, 18 -49 years old, not immunocompromised: 3 doses
- Pfizer or Moderna, 50+ years old, not immunocompromised: 4 doses
- Pfizer or Moderna, 18+ years old, immunocompromised: 5 doses
- Johnson & Johnson, 18 â 49 years old, not immunocompromised: 2 doses
- Johnson & Johnson, 50+ years old, not immunocompromised: 2 doses
- Johnson & Johnson, 18+ years old, immunocompromised:
As recommendations change, on both federal and state level, it may take a few days for the computer systems and staff training to catch up, so be patient for a few days after big announcements.
Medicare Advantage Plans May Cover More Vaccines Than Original Medicare
Medicare Advantage plans are sold by private insurance companies as an alternative to Original Medicare.
Every Medicare Advantage plan must provide the same hospital and medical benefits as Medicare Part A and Part B, and most plans include Medicare prescription drug coverage.
MAPDs must help cover a number of commercially available vaccines that arent covered by Original Medicare when reasonably and medically necessary to prevent illness. However, specific rules of administration and costs will vary depending on the Medicare Advantage plan you enroll in.
A licensed insurance agent can help you compare Medicare Advantage plans in your area, including what vaccinations may be covered.
Find Medicare plans that cover your vaccinations
Or call 1-800-557-6059TTY Users: 711 to speak with a licensed insurance agent. We accept calls 24/7!
About the author
Christian Worstell is a senior Medicare and health insurance writer with MedicareAdvantage.com. He is also a licensed health insurance agent. Christian is well-known in the insurance industry for the thousands of educational articles hes written, helping Americans better understand their health insurance and Medicare coverage.
Christians work as a Medicare expert has appeared in several top-tier and trade news outlets including Forbes, MarketWatch, WebMD and Yahoo! Finance.
A current resident of Raleigh, Christian is a graduate of Shippensburg University with a bachelors degree in journalism.
Also Check: Does Medicare Cover Vitamin D Testing
