Regular Mammograms Can Help Detect Breast Cancer Three Years Earlier Than You Would Feel A Lump
One in eight U.S. women will develop breast cancer over the course of her life.
In 2021, more than 300,000 new cases of breast cancer were diagnosed in women in the U.S., and as of January 2021, more than 3.8 million women had a history of breast cancer.
Even though it’s now the most commonly diagnosed cancer among American women, some forms of breast cancer can be prevented, treated, and irradicated successfully. The first step in protecting yourself and lowering your risk of developing breast cancer is by getting regular screening mammograms.
How Much Does A Diagnostic Test Cost
Depending on your region, this figure should sit between $65 and $100. RepairPal reports that a car diagnostic test costs between $88 and $111 before taxes, and Popular Mechanic says it can cost from $20 to $400. As with any financial decision, itâs smart to check at least three places before you commit.
You May Like: Does Medicare Cover Family Counseling
Mammograms And Dense Breasts
Breasts are composed of fatty, fibrous, and glandular tissue. Mammograms look at this tissue using X-rays. Fat appears dark on X-rays, while glands and fibrous connective tissue appear white. Cancerous changes, like clusters of calcium or tumors, can look white too.
As many as 48% of women have dense breast tissue. To be clear, dense breasts are a radiologic finding, not something you can feel.
Dense tissue appears whiter on mammograms because it contains either less fat or there are areas of more fibrous and glandular tissue. Having dense breasts can make it harder for a radiologist to see small changes that could be related to cancer.
Unfortunately, women with dense breast tissue are at higher risk for breast cancer. Not only that, traditional mammograms are not as effective at detecting cancer in these women.
Digital mammograms help by increasing the sensitivity of the test. Still, they are not as accurate as they are in women with less dense breasts.
Also Check: Do Oral Surgeons Accept Medicare
Does Medicare Cover Annual Breast Exams
A breast exam is another diagnostic breast cancer tool that can be used to detect lumps or other abnormalities within the breasts. Medicare Part B covers annual breast exams, separately from screening and diagnostic mammograms, as part of your pelvic exam. Medicare will cover a pelvic and breast exam once every 12-24 months, depending on your cervical and vaginal cancer risk.
What extra benefits and savings do you qualify for?
What Is An Annual Exam

An annual exam is a once-a-year visit to your primary care provider for a general health check, including a breast exam and pap smear. An annual exam visit does not include discussion of new problems or detailed review of chronic conditions. Annual exams are also called routine check-up, yearly exam, annual pap, and preventive visit.
Please schedule a separate appointment if you have health concerns other than your routine physical exam.
Recommended Reading: Do Teachers Get Medicare When They Retire
Read Also: Do You Have To Take Medicare
Medicare Supplement Insurance Can Help Cover Mammograms
Medicare Supplement Insurance helps cover some of Original Medicare’s out-of-pocket costs, including the deductibles, copayments and coinsurance you might face if you get a diagnostic mammogram.
A licensed agent can help you decide on a Medicare option that works for you. Call today to speak with a licensed agent and compare the Medigap plans that are available where you live.
Research Shows Need For Pap Smears Past Age 65
As many as 20% of cervical cancer cases occur in women aged 65 and older, according to research out of the University of Alabama at Birmingham.1 Study results also showed that the rate of cervical cancer diagnosis was higher in women age 70 79 than in women age 20 29. Prior to these findings, the view was that cervical cancer was usually only diagnosed in younger women.
The outlook for cervical cancer is favorable when the disease is caught early, and regular Pap smear tests are the key to early diagnosis.
Don’t Miss: Does Medicare Cover Ct Scans
How Often Does Medicare Pay For Mammograms
If youre under age 65 and on Medicare, Medicare will pay for one baseline mammogram when youre between 35 and 39 years old. Once youre 40, Medicare pays for a screening mammogram every year. When the doctor accepts assignment, you pay nothing for the screening.
If the test is diagnostic, youll pay 20% of the costs. The average cost of a diagnostic Mammogram with Medicare is around $170. But, depending on your area and if you have extra insurance, your costs could be different.
Get Womens Health Coverage
Fortunately, Original Medicare covers most womens health needs. However, Medicare Advantage and Medicare Supplements can supplement your Original Medicare coverage. If you are looking for additional health benefits through Medicare Advantage or financial benefits through Medicare Supplements, our licensed agents can help. They are contracted with all the major carriers so they can enroll you in a plan without bias. With Medicare Plan Finder, theres never an obligation to enroll and appointments are always cost-free to you. Fill out this form or give us a call at 833-438-3676.
You May Like: What Medications Are Covered By Medicare
Getting A Dbt Mammogram
Getting a DBT mammogram is similar to getting a 2D mammogram.
A DBT mammography machine provides both a 2D mammogram and an enhanced 3D image based on multiple 2D images. All the images are taken on the same machine, so you stay in one place while all the images are taken.
A DBT mammogram takes a few seconds longer than a 2D mammogram because more images are taken. If youve had a 2D mammogram in the past, you may not notice a difference.
DBT may give a slightly higher radiation dose than standard 2D mammography . This higher dose is within FDA guidelines .
You May Like: What Does Original Medicare Not Cover
How Much Do You Have To Pay Out
As mentioned above, a screening mammogram is covered with no cost at all to you under Medicare Part B.
For a diagnostic mammogram, however, you will pay 20% of the cost after your Part B deductible is met. That deductible is $233 at the time of this writing. If you have a Medicare Supplement plan, you may have coverage for some or all of the deductuble and coinsurance.
This is the same whether you have a 2D or a 3D mammogram, although the 20% coinsurance may be a higher amount for a 3D mammogram, which may cost more overall.
Medicare Advantage will also pay for a screening mammogram at no cost. Medicare Advantage plans have varying levels of deductibles, coinsurance, and copays, so you will need to check with your plan to find out what a diagnostic mammogram will cost.
You May Like: How To Apply For Medicare In San Diego
Pros And Cons Of Breast Ultrasound
When there are questions about a mammogram finding or a mammogram cannot be performed, a doctor may recommend a breast ultrasound to get more information.
A breast ultrasound is a relatively low-cost test that uses sound waves to generate an image of the breasts. It is hard to detect small abnormalities like breast calcifications on ultrasound, but it can be a helpful test for people with cysts, masses, and breast implants.
Using a mammogram and breast ultrasound together improves the detection of breast cancer in people with dense breasts. One study shows that sensitivity increased from 74% with mammogram alone to 96% when both studies were used.
More breast cancers are detected thanks to breast ultrasound. Case in point, states with dense breast notification laws have seen an increase in the number of ultrasounds performed and the number of cancers diagnosed.
These laws require a letter be sent to anyone whose mammogram shows dense breast tissue, even if their mammogram was otherwise normal, to let them know about their increased risk for cancer.
Unfortunately, breast ultrasounds increase false positive results too. This means that people who do not have cancer could be told they might have it. This can lead to unnecessary worry and testing.
Find The Best Medicare Health Insurance For Gynecologist Exams
While Medicare Part B covers your basic gynecological care, you can always add additional coverage through Medicare Advantage or Medigap. Even if youre over 65, you still need to have pelvic exams and pap smears to stay healthy.
So, does Medicare cover annual gynecological exams? Medicare Part B does, but you should shop around for the best rates if youre interested in Medicare Advantage. If you want to get a sense of what quotes might look like for you, enter your ZIP code into our free tool.
Recommended Reading: How Do I Pay Medicare Premiums
Also Check: How To Register For Social Security And Medicare
What Free Preventive Services Does Medicare Offer
- May 12, 2020
Its not often you can get something for nothing. But the authors of the Affordable Care Act believed that its cheaper to prevent illness than to treat it, so they added to Medicare free mammograms, colonoscopies and other preventive services.
Many of these tests and medical services used to require a co-payment, but not anymore. Some preventive services are covered with a copayment or coinsurance.
Also, be aware that coverage for some services depends on the patients age.
How Much Does The Average Mammogram Cost
One recent study found that roughly 23 percent of women report having to pay some out-of-pocket costs for a mammogram. If you have Medicare and want to know how much a mammogram will cost, you should first understand what Medicare will cover.
If you have Medicare Part B or Medicare Advantage, coverage for mammograms includes:
- 100 percent of yearly screening mammogram costs
- 80 percent of necessary diagnostic mammogram costs
Medicare beneficiaries pay nothing for yearly mammogram screenings. However, there may be some out-of-pocket costs for diagnostic mammograms. These costs generally include any premiums and deductibles owed, plus a coinsurance of 20 percent of the Medicare-approved costs for this test.
Having to pay out-of-pocket medical costs can greatly affect the likelihood someone will seek medical care.
One study found that when the Affordable Care Act eliminated cost sharing for mammogram screenings, more women received mammograms during their recommended screening periods.
If youre in need of a mammogram but havent been approved for Medicare yet, you may be eligible for
types of mammography to choose from:
With your Medicare coverage, both conventional and
Also Check: Are Hospital Beds Covered By Medicare
What Is The Average Cost Of A Mammogram
According to an article in The Journal of Womens Health, roughly 23% of women reported paying some out-of-pocket costs for a mammogram. Medicare Part B and Medicare Advantage coverage for mammograms include:
- 100% of yearly screening mammogram expenses
- 80% of required diagnostic mammogram expenses
It is worth noting that those with Medicare will not pay anything for their yearly mammogram screening, but there may be out-of-pocket costs for diagnostic mammograms. This amount typically includes premiums and deductible owed, plus the 20% copayments of the Medicare-approved expenses.
Medicare Advantage Plans Have Other Healthcare Benefits
Medicare Advantage plans are privately-sold alternatives to Original Medicare .
Every Medicare Advantage plan must cover everything that Part A and Part B covers, which means that if your Pap smear is covered by Original Medicare, it will also be covered by a Medicare Advantage plan.
Most Medicare Advantage plans also offer prescription drug coverage. Some plans may even cover things like routine dental and vision care.
A licensed insurance agent can help you compare Medicare Advantage plans that are available in your area.
Recommended Reading: Does Medicare Cover Biologics For Ra
How Often Does Medicare Cover Mammograms
Medicare Part B covers:
- One baseline mammogram for women ages 35-39
- Screening mammograms once every 12 months if you’re a woman aged 40 or older
You pay $0 for a screening mammogram if your provider accepts assignment. This applies for both 2D and 3D mammograms, as well as a digital mammogram.
Diagnostic mammograms are covered more frequently than once per year if it’s medically necessary, though you’d pay 20% of the Medicare-approved amount and the Part B deductible applies.
It’s recommended that women between the ages of 50-74 have a screening mammogram every year, though your doctor may recommend additional screenings. Medicare mammogram coverage doesn’t stop at a particular year, so women in their 80s, 90s, or even 100s can still get a screening or diagnostic mammogram and it will be covered.
How Much Does Medicare Pay
Does Medicare pay 100% for mammograms?
As long as you receive your screening mammogram from a provider that accepts Medicare assignment, Medicare Part B will cover 100% of your mammogram costs even if you have not met your Part B deductible for the year. However, Medicare will only provide full coverage of this service once every 12 months, so its important to make sure that you are scheduling your mammograms 12 months apart.
Medicare covers ongoing diagnostic mammograms as part of your treatment-related services for breast cancer. However, unlike yearly screening mammograms, Medicare does not cover the full cost of diagnostic mammograms. Instead, you will be required to pay the remainder of your Part B deductible, if applicable, and a 20% coinsurance of the Medicare-approved amount for the mammogram.
Speak with your doctor to learn more about your out-of-pocket costs for diagnostic mammograms.
Also Check: Does Medicare Cover Hospital Bills
How Often Is A Mammogram Covered Under Medicare
- Medicare will cover a mammogram every year for women aged 40 and older. Medicare covers screening mammograms and diagnostic mammograms slightly differently, so it helps to know how your coverage works before going to your doctor.
The American Cancer Society advises women over the age of 55 to undergo a mammogram at least every two years, if not annually. Early detection is one of the most important factors in helping protect women from breast cancer.
Medicare typically covers a mammogram every year for women once they reach age 40. How Medicare covers mammograms depends on whether it is a screening mammogram or a diagnostic mammogram. Read more to learn exactly how Medicare mammogram coverage works and the costs involved.
How Often Will Medicare Cover Mammograms
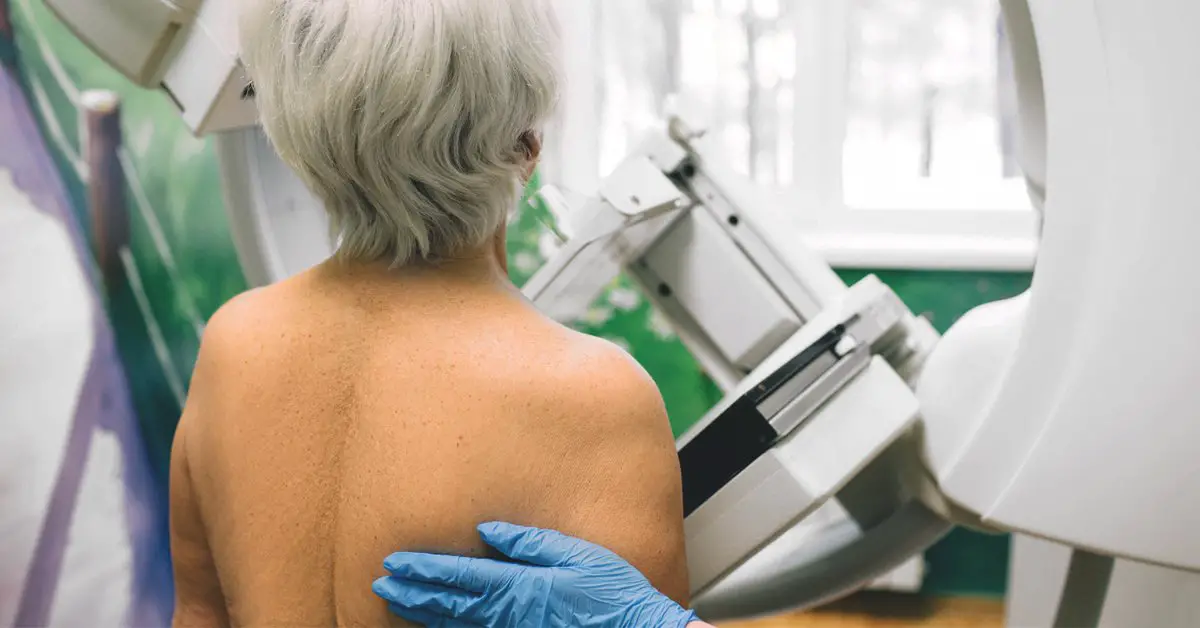
For screening mammograms, Medicare covers one test per 12-month period for all women on Medicare over age 40. This is in line with the recommended annual mammogram recommendations by the American Cancer Society.
Part B will cover 80% of additional mammograms done during the 12-month period if they are deemed medically necessary. If you have a supplement, it will pick up the remaining 20% coinsurance.
Read Also: How To Know If I Have Medicare
Do Medicare Advantage Plans Cover Annual Mammograms
Medicare Advantage plans offer the same coverage as Original Medicare Parts A and B, which means that all Medicare Advantage plans must cover both screening and diagnostic mammograms. However, while annual screening mammograms are fully covered by Medicare Advantage plans, the costs for diagnostic mammograms may differ from Original Medicare, depending on your plan.
When Should You Stop Getting Mammograms
For women with no history of cancer, U.S. screening guidelines recommend that all women start receiving mammograms when they turn 40 or 50 and to continue getting one every 1 or 2 years. This routine continues until they turn about 75 years of age or if, for whatever reason, they have limited life expectancy.
Don’t Miss: What Is The F Plan For Medicare
How Does Medicare Cover Mammograms
If you are a woman enrolled in Original Medicare and you are age 40 or over, Part B will generally cover the allowable charges for one screening mammogram every 12 months so you have no charge. Your Part B deductible and coinsurance amounts may apply. Usually eleven full months must have elapsed since your last screening mammogram before Medicare will pay for another one.
If you are a Medicare beneficiary between the ages of 35 and 39, Part B will generally cover the allowable charges for one baseline mammogram prior to age 40.
If your doctor orders a diagnostic mammogram that is medically necessary for your care, Part B also covers 80% of the allowable charges after youve met your deductible.
Individuals who are enrolled in a Medicare Advantage plan may also pay little or nothing out-of-pocket for mammograms. Some plans charge a small copayment or waive the deductible for screening tests like mammograms. Medicare Advantage plans must cover everything that Original Medicare covers , but they can and often do include additional benefits for members such as no-cost screening exams and even routine vision, hearing, and dental coverage. With a Medicare Advantage plan you must continue to pay your Part B premium.
How To Get Medicare Coverage For Your Mammograms
Medicare covers one test per 12-month period for screening mammograms for all women on Medicare over the age of 40, in line with the recommended annual mammogram recommendations by the American Cancer Society.
Part B will cover 80% of supplementary mammograms done during the 12 months if considered medically required. If enrolled in a supplement plan, it will cover the remaining 20% coinsurance.
To learn more about Medicare Advantage or Medigap plans that suit your needs for mammogram coverage, contact our professionals today.
Don’t Miss: Do I Have To Have Medicare When I Turn 65
How Medicare Helps Cover Gynecological Care
You can also opt to have the gynecological portions of your Wellness exam performed by your gynecologist rather than your primary doctor. You will just need to make sure that your doctor marks them as deferred during your regular Wellness exam.
If you have an abnormal Pap smear or are at risk of cervical or vaginal cancer, Medicare will cover a gynecological exam once every 12 months.
If you see an in-network provider for these exams, you do not pay any out-of-pocket expenses, including your health care deductible and copayment or coinsurance. However, if your doctor begins diagnostic testing for symptoms that are noticed during your exam, you may have to pay your deductible and copayment or coinsurance for the tests.
