Does Medicare Cover Continuous Glucose Monitors For Diabetes
- Does Medicare cover continuous glucose monitors? Learn who’s eligible for monitors through Medicare, what additional supplies are covered and other ways to get a monitor.
In 2018, an estimated 13% of U.S. adults had diabetes. Among people aged 65 and over, that number rose to 26.8%. As older adults make up the bulk of the 63.3 million people enrolled in Medicare, its no surprise that the government is looking for better ways to help beneficiaries manage the condition.
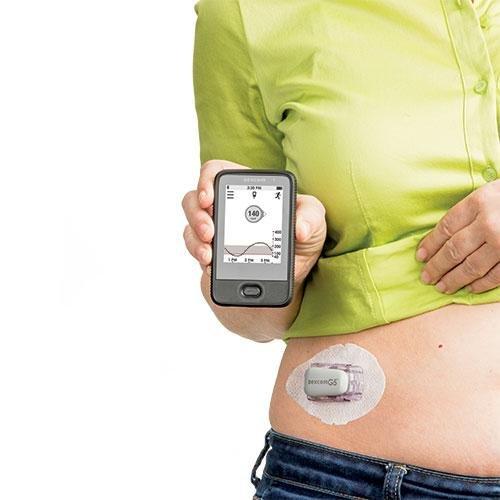
Continuous glucose monitors use sensors under your skin to monitor blood glucose levels 24 hours a day. This information is sent to a wearable device or smartphone, giving users the ability to easily track blood sugar levels and determine dosing needs. These devices have resulted in better glycemic control, so theyre increasingly being recommended to people with diabetes. Find out if and how Medicare covers continuous glucose monitors.
How Much Does It Cost To Get An Insulin Pump
Medicare covers 80% of the Medicare-approved cost of insulin pumps. You are responsible for the other 20%, plus the Part B deductible and monthly premiums.
Your pump must be prescribed by a Medicare-approved physician and purchased or rented from a Medicare-approved medical supplier for Medicare to cover it.
Does Medicare Cover Insulin
Medicare Part D covers diabetes medications and supplies for injecting or inhaling insulin. Heres a rundown of the diabetes supplies and services that Medicare covers. Some require a prescription or recommendation from your doctor. Coverage limits may include the amount of some supplies you can get or how often some services are covered.
Don’t Miss: Is Dental Insurance Included In Medicare
Contour Next Ez Glucose Meter
A basic glucometer that focuses on accuracy, not gimmicks
Specifications
Reasons to avoid
The Contour Next EZ Glucose Meter is primarily aimed at beginners or those who dont want a lot of fuss of high-end features when testing their blood sugar levels at home.
As such, its very simple in its design and what it offers, and while this isnt necessarily a bad thing, it does mean that you should look elsewhere in our best glucose meters guide if you want smart connectivity or sensors.
The Next EZ Glucose Meter requires you a small blood sample in order to read your blood glucose levels, and returns results within five seconds. A lancing device and replaceable lancets are included with this blood sugar monitor kit, as well as test strips, though you will soon need to buy new strips.
There are over 140 user reviews of the Contour EZ Glucose Meter on Walmart, with an average rating of 4.5 out of 5 stars. 106 of those of 5-star reviews. So the majority of customers are highly praising, though a few reported not having any test strips in the box.
The cost of these ranges depending on where you shop, but Contour offers a loyalty scheme that could give you access to bigger savings when buying direct. Speak to your insurance provider to see what they will cover.
Medicaid And Diabetes Health
As an insurer, Medicaid is dedicated to helping people achieve their health goals. Medicaid has many programs that are geared directly toward specific diseases. The programs are specifically designed to help you with your overall treatment plan and health management. A diabetes health program usually contains information and resources regarding medications, diet, and exercise. Please check with your state run Medicaid program to find out whats available to you as a person living with diabetes.
MedicaidSupplies.com understands that diabetes is a very complex and serious disease. We strive to provide people with valuable information and resources to help make living with diabetes that much easier.
Recommended Reading:
You May Like: Are Diabetic Test Strips Universal
Also Check: What Is Medicare Advantage Plan Mean
Does Medicare Pay For Livongo
Mountain View, CA April 30, 2019 Livongo, the leading Applied Health Signals company empowering people with chronic conditions to live better and healthier lives, today announced that it has been approved by the Centers for Medicare and Medicaid Services as an enrolled provider for Medicare Advantage members.
Easily Track Your Glucose Levels And More At Your Fingertips
Dr. Danielle Weiss is the founder of the Center for Hormonal Health and Well-Being, a personalized, proactive, patient-centered medical practice with a unique focus on integrative endocrinology. She enjoys giving lectures and writing articles for both the lay public and medical audiences.
Our editors independently research, test, and recommend the bestproducts, and articles are reviewed by healthcare professionals for medical accuracy. Youcan learn more about ourreview process here.We may receive commissions on purchases made from our chosen links.
Verywell / Sabrina Jiang
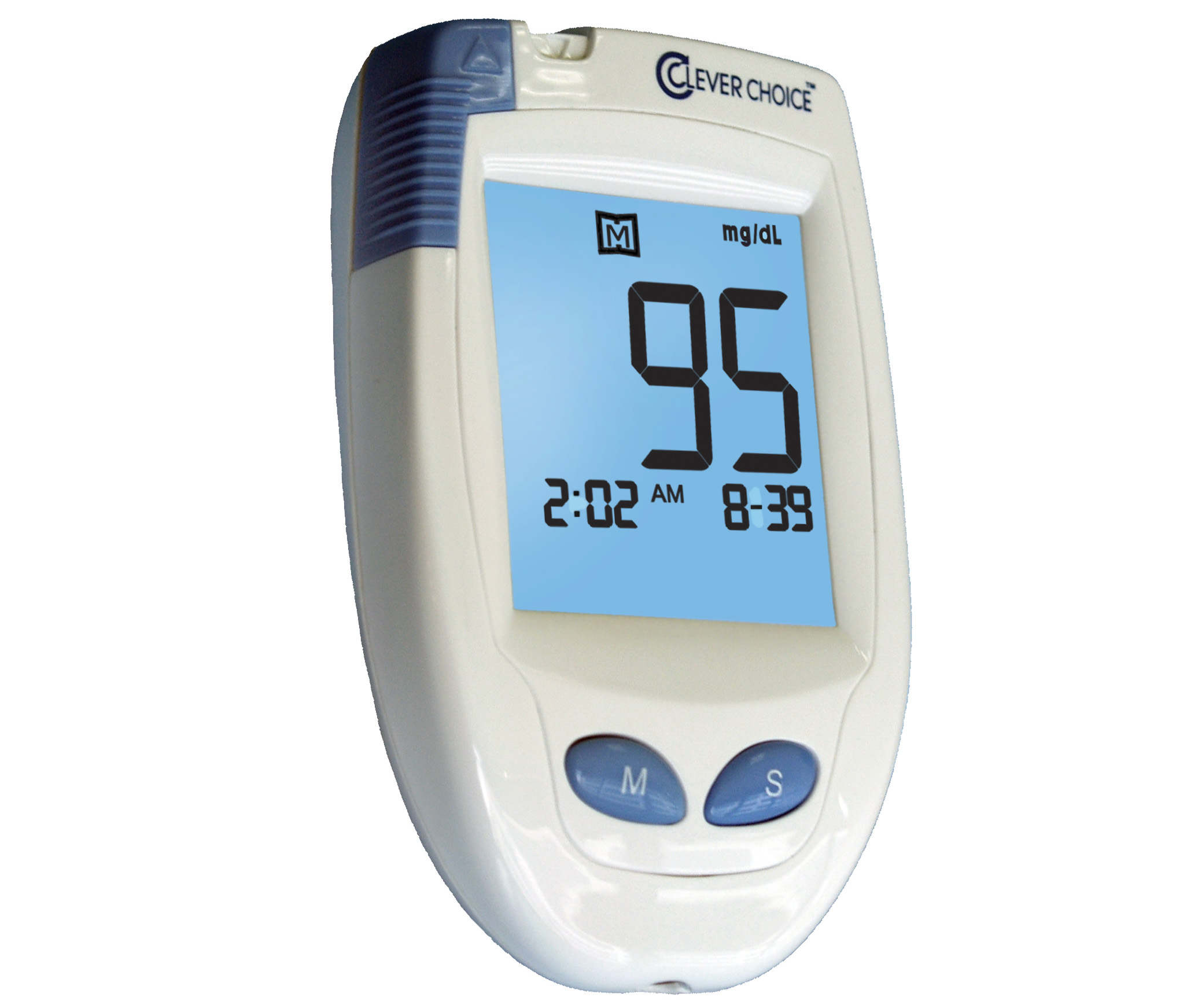
Daily blood sugar testing is a vital component of any successful diabetes management plan. It can help determine if you have your blood sugar under control, while also helping identify patterns that can lead to a spike or crash. It also reveals how factors like stress and exercise can impact your blood sugar, and it assists you in examining the effectiveness of any diabetes medications you may be taking.
While the frequency and cadence of your blood glucose testing depends on your specific diagnosis and your physicians recommendations, its up to you to select the glucometeror at-home blood sugar-monitoring devicethat will best support your needs.
-
No calibration required on test strips
-
Allows you to set reminder alarms
-
Saves pre- and post-meal glucose levels
Also Check: When You Turn 65 Is Medicare Free
Would You Like To Know More About Medicare Coverage Of Glucose Monitors
If you have questions about Medicare coverage for home glucose monitors, or would like more information about Medicare plan options to help you better plan for your expenses, Id be happy to discuss them with you. If youd like to schedule a phone call, or request a personalized email, click on the corresponding button below. The Compare Plans button on the page will show you some of the Medicare plan options available in your area.
The product and service descriptions, if any, provided on these Medicare.com Web pages are not intended to constitute offers to sell or solicitations in connection with any product or service. All products are not available in all areas and are subject to applicable laws, rules, and regulations.
New To Medicare?
Becoming eligible for Medicare can be daunting. But dont worry, were here to help you understand Medicare in 15 minutes or less.
Also Check: How Old Before Eligible For Medicare
Does Medicare Cover Hospice
Part A covers hospice care when you have a Medicare Advantage plan. Medicare Advantage plans cover glucose monitors in the same way as Medicare Part B and often offer additional benefits, such as vision, dental, and prescription drug coverage. Some types of Medicare Advantage plans use provider networks, and may reduce the amounts you pay …
Read Also: What Is The Best Medicare Supplement Plan In Arizona
Do You Need A Prescription For A Glucometer
Blood testing meters, strips, lancets and supplies are sold at pharmacies, adaptive equipment catalogs, and mail-order companies. You do not need a prescription from your physician to buy a blood glucose testing meter , strips and supplies, but without a prescription you will have to pay 100% of the costs.
Who Qualifies For A Continuous Glucose Monitor
Medicare will cover CGMs for people who:
- Have an established diagnosis of Type 1 or Type 2 diabetes
- Are currently using a traditional blood glucose monitor
- Must check their blood sugar a minimum of four times daily
- Use insulin to treat diabetes and require frequent adjustments to their regimens or have a subcutaneous insulin infusion pump
- Receive training from their doctors on how to use CGMs
Recommended Reading: Does Medicare B Cover Prescriptions
Medicare Coverage Of Cgm
Medicare has provided coverage for CGM systems since 2017, provided they are classified as therapeutic devices, meaning users can use them to make treatment decisions. These include things like changes to exercise regimen, diet or insulin dosage. While thats still the case, The Centers for Medicare & Medicaid Services have recently relaxed Medicares other coverage criteria somewhat. Previously Medicare coverage of CGM devices was limited to patients who met the following requirements:
-
Have a diagnosis of either type 1 or type 2 diabetes
-
Use a traditional blood glucose meter and test blood sugar levels four or more times a day
-
Are treated with insulin injections or insulin pump
- Require frequent adjustments to their insulin regimen
-
Have an in-person visit with a doctor to evaluate glycemic control and whether they meet the above criteria, as well as follow up appointments every 6 months after prescription
So whats changed? No longer are insulin injections the only acceptable form of insulin administration for those who are covered. Now, diabetics who are treated with inhaled insulin will be eligible for coverage. Additionally, the requirement for self-testing up to four or more times a day with a fingerstick test has been removed, so diabetics who test less frequently may also be eligible.
Does Medicare Pay For Psa Test
How Often Will Medicare Pay for a PSA Test? Medicare Part B pays for one prostate cancer screening test each year. You pay no out-of-pocket cost for a PSA test if your doctor accepts Medicare assignment, and the Part B deductible does not apply. Medicare Advantage plans also cover a yearly PSA test.
You May Like: What Is Difference Between Medicare And Medical
How To Learn More
- For more information on all of the options available under Medicare, visit: www.medicare.gov or call 1-800-MEDICARE . Also look for the Medicare and You handbook which Medicare mails to beneficiaries in the fall and is available by calling 1-800-MEDICARE .
- To read more about Medicare coverage of diabetes services and supplies, go to .
- For information from Medicare on how individuals might be able to get help paying Medicare costs visit www.medicare.gov/your-medicare-costs/help-paying-costs/get-help-paying-costs.html or call 1-800-MEDICARE .
- Free health insurance counseling and personalized assistance for Medicare beneficiaries is available in every state through the State Health Insurance Assistance Program . Call 1-800-MEDICARE or visit www.shiptacenter.org to find the telephone number of the SHIP office closest to you.
Medicare Coverage Of Glucose Monitors
Under Original Medicare , Part A covers health-care expenses you incur as an inpatient in a hospital, while Part B covers your outpatient care, including some glucose monitoring supplies and durable medical equipment. Medicare does not generally cover âcontinuous glucose monitoring,â which involves a sensor inserted under your skin for several days to a week.
If your health-care provider recommends a different way to monitor your blood sugar other than the finger-stick glucose monitor, you might want to check with Medicare to see whether itâs covered. You can reach a Medicare representative 24 hours a day, seven days a week, if you call 1-800-MEDICARE . TTY users can call 1-877-486-2048. If you have a Medicare Advantage plan, call your plan to ask about this coverage.
Also Check: Does Medicare Cover Assisted Living In Michigan
How Many Diabetic Test Strips Will Medicare Pay For
Medicare Part B covers the same type of blood glucose testing supplies for people with diabetes whether or not they use insulin. However, the amount of supplies that are covered varies. Uses insulin, they may be able to get up to 100 test strips and lancets every month, and 1 lancet device every 6 months.
Prodigy Diabetic Supplies Medicare And Insurance Coverage
Blood glucose testing is an important part of diabetes management. Most insurance companies and Medicare/Medicaid will pay for blood glucose testing supplies. With private insurance or managed care, patients will most likely be asked to pay a co-pay to cover part of the cost of the supplies. Medicare pays for 80% of supplies once the patient has met their yearly deductible and the patient is responsible for the remaining 20% of the cost. See the www.Medicare.gov site for a full explanation of how your blood glucose testing supplies are covered. Prodigy Diabetes Care is contracted with certain insurance providers and state Medicaid programs, which may make the Prodigy brand products available to those individuals at a lower co-pay or no co-pay depending on the program.Continue reading > >
Read Also: What Does Medicare Part B
Does Medicare Cover Continuous Glucose Monitors
- Get the facts about Medicare coverage of continuous glucose monitors . Find out who qualifies for CGMs and how much you can expect to pay out of pocket.
The U.S. Centers for Disease Control and Prevention advises that regular blood sugar monitoring can improve the effectiveness of treatments for Type 1 and Type 2 diabetes and lower the risk of serious complications like blindness, heart attack and stroke. Continuous glucose monitors make it easier to keep tabs on your blood sugar levels throughout the day, and the most popular models are often covered by Medicare.
$0 Copays On Preferred Brand Diabetic Test Strips And Glucose Meters For Medicare Advantage Members
In 2018, Independence will continue the requirement for Medicare Advantage members to use diabetic test strips and a glucose meter from the preferred manufacturer brands, Accu-Chekî and OneTouchî, in order to have their test strips and glucose meters covered at $0 copayment. All other manufacturersâ brand of test strips and glucose meters will not be covered by Keystone 65 HMO plans. For Personal Choice 65SM PPO plans, an out-of-network coinsurance will apply to all other manufacturersâ brand of test strips and glucose meters. If their current glucose meter does not work with either of the preferred brands of test strips, Medicare Advantage members can obtain a new glucose meter at no cost. Test strips can be purchased from either a network pharmacy or durable medical equipment supplier. The $0 copayment on Accu-Chek and OneTouch test strips will apply at both preferred and standard pharmacies. Providers may appeal if they feel a member is unable to use Accu-Chek or OneTouch test strips and glucose meters. Note: Independence Medicare Advantage plans will continue to offer a $0 copayment on all brands of lancets and solutions.Continue reading > >
Jeemin Kwon
The CGM Discount Access program provides discounted rates on the Guardian Sensor 3 continuous glucose monitoring system for people without insurance coverage for Medtronic CGMs.
To be eligible for the program, people must:
-
Not have insurance coverage for a Medtronic CGM
Recommended Reading: How To Make Medicare My Primary Insurance
Does Medicare Pay For Cgm Accessories And Supplies
Yes, Medicare generally pays 80% of the cost of CGM accessories and supplies. Under the guidelines, Medicare Part B covers:
- Patch refills based on the recommended replacement schedule. For example, if you use a CGM that requires a new patch every 14 days, Medicare will pay for two patches every 28 days.
- Up to 300 test strips every three months if you are being treated with insulin
- Up to 300 lancets every three months if you are being treated with insulin
Medicare Part D may also cover:
What Is Medicare Part C
If you have a Medicare Part C Medicare Advantage plan: Medicare Part C Medicare Advantage plans, also called Medicare Advantage plans, must cover everything that’s included in original Medicare Part A and Part B coverage. But sometimes a Part C plan covers more, with extra services or an expanded amount of coverage.
Recommended Reading: Does Medicare Pay For Contrave
What Supplies Are Covered By Medicare Part B
These supplies include: Blood glucose self-testing equipment and supplies Therapeutic shoes and inserts Insulin pumps and the insulin used in the pumps Blood Glucose Self-testing Equipment and Supplies Blood glucose self-testing equipment and supplies are covered for all people with Medicare Part B who have diabetes.
Best Glucose Meters: The Different Types
Currently, there are three main types of glucose meter:
- Basic blood glucose meters
- Continuous glucose monitors
- CGM-Insulin Pump Combos
The most simple glucometers are handheld devices with a digital screen that displays a reading, and these are the devices were mostly focusing on with our guide to the best glucose meters. These readings are gathered from disposable blood sugar test strips treated with specific chemicals that react to glucose. A new test strip is inserted into the glucometer for each new reading.
Standard glucometers are usually battery operated and capable of storing readings, and many can be connected to a computer so that you can download and store your readings to look back on as needed.
Some basic blood glucose meters are designed with a spring-loaded needle that pricks the side of your fingertip to draw a small drop of blood for testing. Others use an external lancing device.
Once blood is drawn, you touch it to the test strip, which will absorb your blood sample and display a reading on the glucometers screen. While response times vary between blood sugar monitors, were usually talking seconds.
Some glucose meters are approved for Alternate Site Testing . That means they give results within 20% of correct values when used on alternative sites such as the palm, forearm or thigh. However, Diabetes Self Management advises that, you should still check alternate site readings on yourself before trusting them too much.
You May Like: How Is Medicare Irmaa Calculated
Medicare Coverage For Therapeutic Cgm
Medicare Part B covers therapeutic continuous glucose monitors such as the Freestyle Libre 2 and the Dexcom G6 for people with diabetes.
Medicare covers therapeutic continuous glucose monitors as durable medical equipment . You will be responsible for your Medicare Part B deductible and 20 percent of the Medicare-approved cost. Medicare will cover the other 80 percent after you meet your deductible.
A Medigap policy also called Medicare Supplement insurance can cover some of your out-of-pocket costs for the Medicare Part B deductible and coinsurance. Additionally, Medicare Advantage plans are required to cover everything included in Medicare Part A and B coverage but may offer additional benefits.
Both Medigap and Medicare Advantage plans are sold by private insurers. Your plans administrator can verify your policys coverage of therapeutic CGM.
