How To Get Help With Medicare Coverage For Diabetic Shoes
If you have diabetes and need therapeutic shoes, your doctor can help get you started. When you add Medigap coverage, you can be doubly assured your shoes wont break the bank.
Your Medigap plan can help with coinsurance, copays, and your Part B deductible. Our agents can help find the best options for you. Call us today for a quote in minutes! Or, if you prefer, you can complete an online rate form, and a member of our team will reach out to you.
- Was this article helpful ?
What Can I Do If I Have Not Received My Test Strips Allotment But The Pharmacist Says My Claim Has Been Rejected
Your pharmacist can determine the overall annual allotment for test strips by assessing your diabetes therapy in the past six months and the number of strips already reimbursed under the ODB program in your current 365-day period. It is important that you fill your prescriptions at a single pharmacy to facilitate proper tracking of your allotment. Please inform your pharmacist if you have filled test strip prescriptions at more than one pharmacy.
If there is a discrepancy, the pharmacist can contact the ministrys ODB Helpdesk on your behalf for support.
Does Medicare Cover Test Strips
by Christian Worstell | Published January 20, 2022 | Reviewed by John Krahnert
Medicare does cover test strips, glucose meters and other essential tools to help monitor diabetes.
A Medicare Supplement plan can help cover your Medicare costs for test strips and other covered diabetes supplies. These costs can include things like Medicare deductibles, coinsurance, copays and more.
Also Check: Can You File For Medicare Online
Which Medicare Plans Cover Diabetic Supplies
To understand the Medicare coverage of diabetes supplies, it is important to understand how Medicare works. There are four main parts of Medicare:
- Medicare Part A covers in-patient hospital services, so this part does not include diabetic supplies.
- Outpatient medical services, such as doctor examinations and diabetes treatment, are covered under Medicare Part B. Medicare Part B may cover an insulin pump as medical equipment, if you use one.
- Medicare Advantage, also called Medicare Part C, is a private version of Medicare you can enroll in instead of Original Medicare.
- And finally, Medicare Part D is the optional part of Medicare that covers prescription drugs, including insulin and anti-diabetic drugs if they are listed on a plans formulary and you have a prescription from your doctor.
All parts of Medicare can be advantageous to consumers with diabetes. Although Part A does not cover any diabetes supplies, it does cover in-patient hospital services, which could be diabetes-related. That said, Medicare Part B and D are the most beneficial to people with diabetes. Here is a complete breakdown of what each plan covers in relation to diabetes care:
Medicare Part B Covered Diabetes Testing Supplies
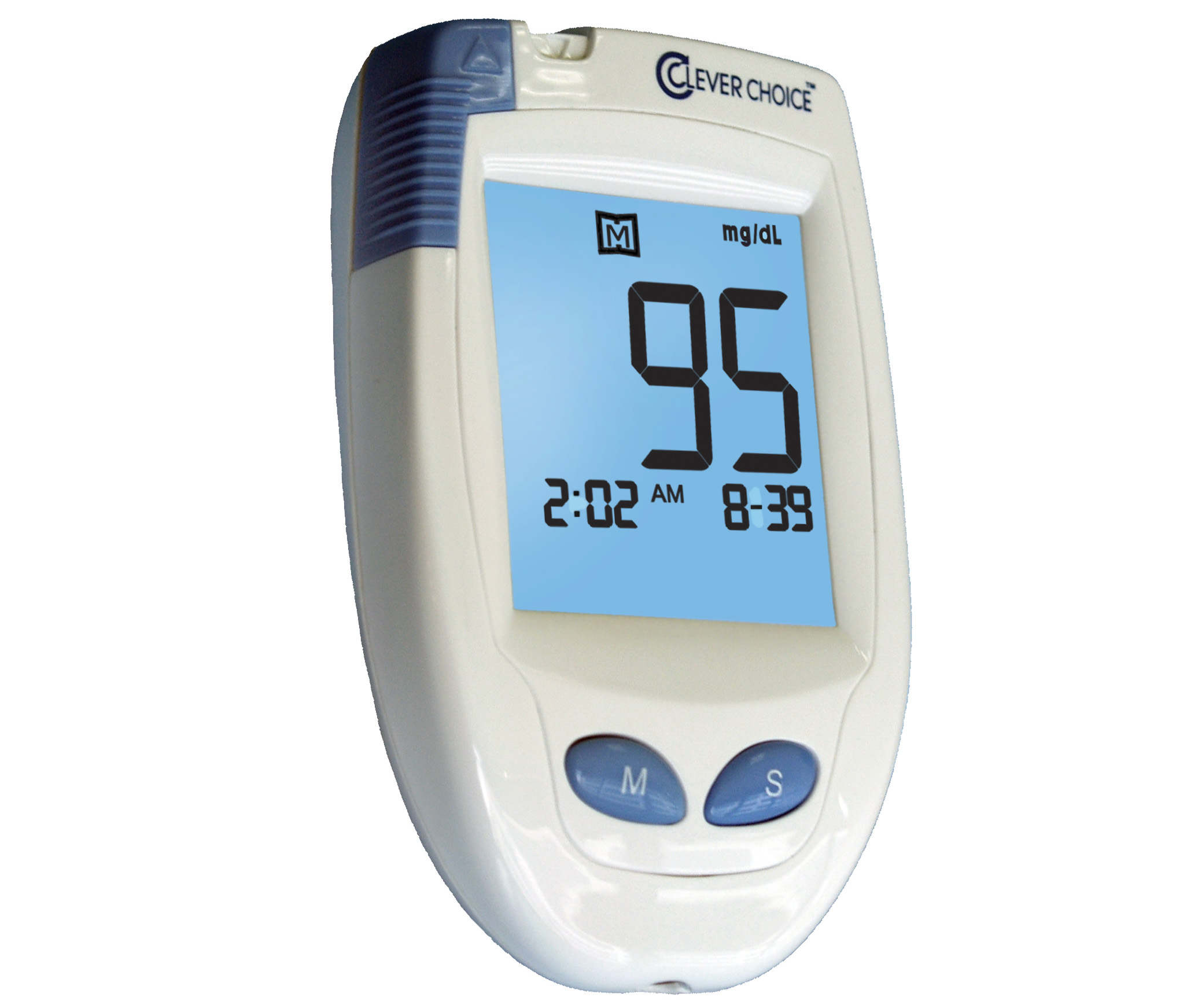
Part B covers a number of blood sugar self-testing supplies and equipment, even if you dont use insulin. These include:
- Blood sugar monitors
- Lancet devices and lancets
- Glucose control solutions
These supplies are considered durable medical equipment, and the actual amount of supplies that are covered varies depending on whether or not you use insulin. For example, if you use insulin, you may be able to get up to 300 test strips and 300 lancets every three months, but if you dont use insulin you may only be able to get up to 100.
If your doctor says its medically necessary, Medicare will cover additional test strips and lancets.
Test strips can be used to help monitor certain substances in the blood. They are small, single-use pieces of paper-like substance that you place one or two drops of blood on, and insert into a testing device. These devices provide results within seconds, and you can address any concerns regarding blood glucose levels.
You May Like: How Old To Be To Get Medicare
What Does Medicare Part B Cover For Diabetic Supplies
Medicare covers supplies related to equipment that measures blood sugar. Covered items include:
- Insulin for insulin pumps
- Sensors for continuous glucose monitors
If you suffer from foot issues related to diabetes, Medicare may cover a pair of shoes and inserts up to once per year. The shoes or inserts must be prescribed and fitted by a qualified physician. Diabetes is commonly the cause of peripheral neuropathy, nerve damage that can make you weak and numb or cause pain. If you have diabetic peripheral neuropathy, you can have a foot exam every six months.
If you use Medicare-approved diabetic supply providers who accept assignment, your out-of-pocket expense should be limited to a 20% coinsurance payment and the Part B deductible. A supplier enrolled in Medicare but not a participating supplier can charge you more than the Medicare-approved rate. Only participating suppliers are required to accept assignment.
For Medigap plan members, the Part B coinsurance is covered anywhere from 50% to 100%, depending on your plan. The 2022 Part B deductible is $233. With enrollment in Medicare Supplement Plan C or Plan F, your Part B deductible is 100% covered.
D Senior Savings Model
Coinsurance also applies every time you fill your prescriptions for insulin or other medications. Copayments depend on your Part D plan and what medications are covered by your plan formulary.
If youre over 65, you can get additional savings by enrolling in the Part D Senior Savings Model. This plan puts a cap on out-of-pocket spending for insulin. You can choose between several covered types of insulin, and your co-payment is capped at $35 for a 1-month supply.
What extra benefits and savings do you qualify for?
You May Like: Does Medicare Come Out Of Social Security
Alternate Site Blood Glucose Monitors
Aetna considers alternate site blood glucose monitors medically necessary DME for the following persons with diabetes, when an alternate site blood glucose monitor is recommended by their physician:
Alternate site blood glucose monitors have no proven value over standard blood glucose monitors for other indications.
How Does Medicare Cover Diabetes
Different parts of Medicare cover different services and supplies. That said, some things arent covered by Medicare, and in many cases, you will pay a portion of the cost, unless you have another insurance plan that covers it.
Medicare coverage for diabetes would usually be obtained by enrolling in Original Medicare or a Medicare Advantage plan .2
You May Like: Does Medicare Cover The Cost Of A Shingles Shot
When It Comes To Diabetes What Does Medicare Advantage Cover
In order to understand Medicare Advantage diabetes coverage, itâs important to first understand what Original Medicare covers for diabetes. The Centers for Medicare & Medicaid Services reports that Original Medicare offers coverage many basic diabetes supplies, including:
- Annual diabetes prevention, screening, and wellness checks
- Blood sugar monitoring equipment such as lancets and blood glucose monitorsâwith limits on which supplies you can use or how often you can buy them
- Durable insulin pumps and the accompanying insulin, under certain conditions
- Diabetes-related foot care for those who have peripheral neuropathy and a loss of protective sensation, including foot exams as well as orthotic diabetes shoes and inserts
Medicare Advantage plans are an alternative to Original Medicare. Advantage plans are supplied by private companies that must follow Medicareâs rules and regulations. While all Advantage plans must offer all of the benefits of Original Medicare, they may come with different rules, costs, rights, protections, and options.
Many Medicare Advantage plans provide benefits you cannot get with Original Medicare. According to the Centers for Medicare and Medicaid Services, some Medicare Advantage plans cover additional diabetes supplies and services, including:
With Medicare Advantage, youâll also have an annual out-of-pocket limit that may help you spend less on health care.
What Do I Have To Pay
Remember that not all covered items are free. For most of your diabetic supplies, coinsurance and copayments still apply. Original Medicare Part B pays for 80% of the supplies and services, and you will pay the remaining 20%. In some cases, your yearly deductible also applies. You will need to reach your yearly deductible before coverage kicks in.
Carefully check your supplies every month and only accept the supplies you ordered. If a supplier sent you any supplies you didnt request, Medicare wont pay for these supplies.
Some services, like nutrition therapy and the diabetes prevention program, are completely free.
Do you have a Medicare Advantage plan? Each plan has different coverage benefits, so ask about your plan to find out what diabetic supplies are free.
Read Also: How To Gain Weight With Diabetes
Also Check: Does Medicare Pay For 100 Days In A Nursing Home
What Is The Childrens Health Insurance Program
CHIP offers free or low-cost Medicaid to children whose parents earn too much for Medicaid but not enough to pay for a private health plan. In some states, CHIP may also cover pregnant women and parents. Learn whether your family members qualify for CHIP through HealthCare.gov or your states Medicaid or CHIP agency.
Learn more about CHIP at www.insurekidsnow.gov or call 18775437669.
How To Save On Diabetic Supplies

For those wanting to save on diabetic supplies, there are a few options that can help cover the costs Medicare does not.
- If you have limited income and resources, look to see if you qualify for Medicaid services, Medicare Savings Programs, or Medicare Extra Help.
- Manufacturer rebates may also be available for specific diabetic supply brands.
- There are also a wide variety of organizations that offer patient assistance programs for diabetic medication and supplies.
- Cutting down on excessive use of diabetic supplies can also help save money. Not everyone needs to test multiple times a day, Hudson says. If I had a patient with well-controlled diabetes on oral medications, I might have them only test their blood sugar once a day or even once every other day.
- If you need help paying for your anti-diabetic drugs or insulin, the SingleCare discount card is a great option.
Also Check: When Do I Receive Medicare
Does Medicare Cover Cgm Equipment And Accessories
Yes, Medicare Part B pays for 80% of the cost of the accessories required to use the device, including the patches. Medicare does cap the number of testing strips and lancets that it will cover. If you use insulin, the general limit is 300 test strips and 300 lancets per three-month period. When a doctor deems that increased testing is medically necessary, Medicare may approve payments for supplies in excess of the established limit.
Also Check: What Is Worse Diabetes 1 Or Diabetes 2
Diabetic Supplies: Therapeutic Shoes And Inserts
Medicare Part B coverage includes therapeutic shoes or inserts for diabetics who have certain conditions ask the doctor who treats your diabetes if you need them. To make sure these supplies are covered by Medicare, please note:
- A qualified doctor must prescribe the shoes or inserts.
- A qualified doctor must provide and fit you for the shoes or inserts.
- Medicare Part B covers one pair of custom-molded shoes or one pair of depth-inlay shoes per calendar year.
- Medicare also covers two additional pairs of inserts each calendar year for custom-molded shoes and three pairs of inserts each calendar year for depth-inlay shoes.
- In certain cases, shoe modifications may be substituted for inserts.
- The supplier must have an order on file signed and dated by the treating doctor if you switch to a different supplier, you may need to have your prescription transferred or get a new prescription from your doctor. Make sure your supplier is enrolled in Medicare.
Read Also: How To Treat Diabetic Sores
Don’t Miss: What Is The Annual Deductible For Medicare Part A
How Does Medicare Pay For Blood Glucose Test Strips
If you have Medicare Part B , youll likely be covered for the costs of test strips.
Medicare covers blood glucose testing strips as a form of durable medical equipment. As such, Medicare will typically pay 80% of the costs of test strips.
However, that means certain costs will still be left up to you. These costs may typically include:
-
20% of Medicares approved costs of test strips
-
Any portion of Medicare Part B deductible that you havent yet paid
Some Medicare Part D prescription drug plans may also cover diabetes supplies, insulin and other medications.
You can compare Part D plans available where you live and enroll in a Medicare prescription drug plan online when you visit MyRxPlans.com.
How Much Does Medicare Pay For Diabetic Supplies
Medicare alone doesnt pay in full for most medical services, including diabetic supplies. Medicare Part B covers about 80% of the costs of a variety of supplies that are used to treat diabetes. Part B will typically cover these services and supplies up to 80%, leaving you responsible for the other 20% as well as any deductibles or copays. In order to help with the expenses, most people have a Medicare Supplement plan or a Medicare Advantage plan.
Its important to note that Medicare Supplement plans rangein coverage, and theyll all pay their portion as long as Medicare pays first. Thecost of your supplies may differ depending on which Medicare Supplement planyou choose.
If you have aMedicare Advantage plan, its your primary coverage instead of Medicare. Forinformation on what your Advantage plan covers, you should contact yourprovider directly.
Also Check: What Age Do You Apply For Medicare
Can You Get Medicare If You Have Diabetes
Yes, you can enroll in Medicare when you have diabetes. In most cases, you can’t be denied coverage because of a preexisting condition, and most diabetics have no extra costs for coverage. The one exception is if you sign up for a Medigap plan after your initial enrollment period, which can sometimes trigger the medical underwriting process.
How Often Do You Need The Test
Your doctor probably will have you take the A1c test as soon as youâre diagnosed with diabetes. Youâll also have the test if your doctor thinks you may get diabetes. The test will set a baseline level so you can see how well youâre controlling your blood sugar.
How often youâll need the test after that depends on several things, like:
- The type of diabetes you have
- Your blood sugar control
- Your treatment plan
Youâll probably get tested once a year if you have prediabetes, which means you have a strong chance of developing diabetes.
You may get tested twice each year if you have type 2 diabetes, you donât use insulin, and your blood sugar level is usually in your target range.
You could get it three or four times each year if you have type 1 diabetes.
You may also need the test more often if your diabetes plan changes or if you start a new medicine.
Itâs not a fasting test. You can take it any time of day, before or after eating.
People with diseases affecting hemoglobin, such as anemia, may get misleading results with this test. Other things that can affect the results of the hemoglobin A1c include supplements, such as vitamins C and E, and high cholesterol levels. Kidney disease and liver disease may also affect the test.
Also Check: How Does Medicare Work If You Have Other Insurance
Best Medicare Plans For Diabetics
The best current Medicare coverage for diabetics will include either a Part D plan or a Medicare Advantage plan that participates in the Insulin Savings Program .
Effective in 2023, all plans will have a maximum $35-per-month copay for insulin, as a result of a new federal law passed in August 2022.
The $35 rate begins right away, even if you haven’t met the plan’s deductible. And the 30-day supply is based on the amount of insulin you need, rather than a standardized amount.
Medicare Covers Some Other Diabetes Supplies And Treatments
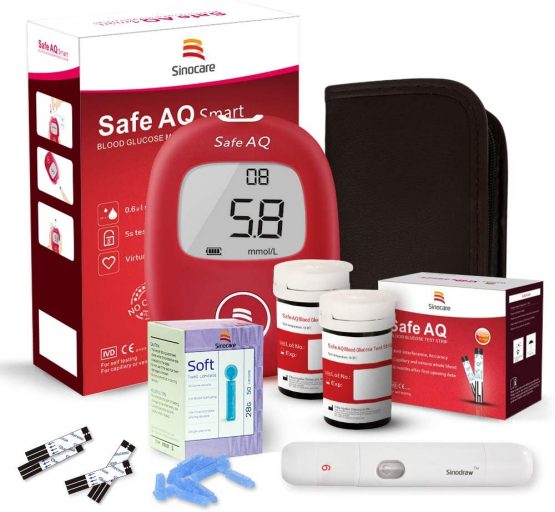
Medicare Part B also helps cover the costs of some other diabetes treatment-related services, which can include:
-
Lancets and lancet devices
-
Blood sugar monitoring and control devices
-
Therapeutic shoes or shoe inserts
It’s important to note that in order for Medicare to cover some diabetes testing supplies, you may need to go through specific durable medical equipment suppliers who are enrolled in Medicare.
Additionally, Medicare Part B covers some diabetes services. These can include:
-
Annual eye exams
-
Medical nutrition therapy services
Read Also: How To Qualify For Oxygen With Medicare
Medicare Diabetes Coverage Screening And Services
After a medical evaluation, your doctor may conclude that you are at risk for diabetes based on your blood pressure or any history of abnormal cholesterol, triglyceride or blood sugar levels. With a high-risk assessment, you may be eligible for two annual glucose lab screenings. Screenings may or may not include a carbohydrate challenge, which is a test of your carbohydrate metabolism, a possible underlying source of fatigue, premature aging, obesity and anxiety.
You may also be eligible for diabetes testing if you are at least 65 years old, overweight, have diabetes in your family history, gave birth to a 9-pound-plus baby or have had gestational diabetes. If two or more of these criteria apply, Medicare covers the screenings.
Diabetes preventive services under Medicare Part B include self-management training and medical nutrition therapy to provide you with self-care strategies. With self-management training, you can learn how to eat nutritiously, keep yourself moving, monitor your blood sugar, manage your medications and reduce your risk.
If you have diabetes, Part B covers annual eye exams to check for diabetic retinopathy, an inflammation of the retina caused by high blood sugar. Check that your eye doctor has the legal right to perform the test in your state.
