How Would I Pay For Care In A Hospice House Residence
This is a matter to be worked out between the hospice and the family. If you believe a prospective hospice patient can only be cared for in a hospice residence, contact the social worker at one of the hospices that have a hospice house . The hospice will require a financial assessment of the familys resources and insurance coverage before admitting the patient to the hospice house. Requests for placement at a hospice house far exceed the number of available beds.
Can I Get Hospice Care In An Assisted Living Residence
Fredrick P. Niemann Esq.
New Jerseys licensure law allows hospice care in any kind of residence. Let the hospice staff know of the living arrangements, and they will work with the staff at the assisted living residence.
If you would like to speak to a NJ hospice attorney, contact Fredrick P. Niemann, Esq. toll-free at 376-5291 or email him at to schedule a consultation about your particular needs. He welcomes your calls and inquiries and youll find him very approachable and easy to talk to.
How Would I Pay For Hospice Care In A Nursing Home
According to the rules of the federal government, one cannot access both the Medicare Hospice Benefit and the Medicare Nursing Home Benefit at the same time. While the previous sentence is technically accurate, patients receiving a Medicaid Hospice Benefit can get their nursing home room and board paid through the Medicaid Hospice Benefit.
Don’t Miss: Does Medicare Plan F Cover Acupuncture
How Long You Can Get Hospice Care
Hospice care is for people with a life expectancy of 6 months or less . If you live longer than 6 months, you can still get hospice care, as long as the hospice medical director or other hospice doctor recertifies that youre terminally ill.
- You can get hospice care for two 90-day benefit periods, followed by an unlimited number of 60-day benefit periods.
- You have the right to change your hospice provider once during each benefit period.
- At the start of the first 90-day benefit period, your hospice doctor and your regular doctor must certify that youre terminally ill . At the start of each benefit period after the first 90-day period, the hospice medical director or other hospice doctor must recertify that youre terminally ill, so you can continue to get hospice care.
How Much Does Medicare Pay For Hospice
- Up to a $5 copayment per prescription for outpatient drugs to relieve pain and manage terminal illness-related symptoms.
- Five percent of the Medicare-approved cost for inpatient respite care.
Did You Know: If a prescription is not covered under the patients Medicare hospice plan, ask a hospice care team member to inquire if the medication is covered under Medicare Part D. If you or your loved one needs a prescription drug plan, visit our list of the best Medicare Part D plans.
Don’t Miss: Why Are There So Many Medicare Commercials
If You’re In A Medicare Advantage Plan Or Other Medicare Health Plan
Once your hospice benefit starts, Original Medicare will cover everything you need related to your terminal illness. Original Medicare will cover these services even if you choose to remain in a Medicare Advantage Plan or other Medicare health plan. If you were in a Medicare Advantage Plan before starting hospice care, you can stay in that plan, as long as you pay your plans premiums. When you get hospice care, your Medicare Advantage Plan can still cover services that aren’t a part of your terminal illness or any conditions related to your terminal illness.
If you stay in your Medicare Advantage Plan, you can choose to get services not related to your terminal illness from either providers in your plans network or other Medicare providers.
If you choose to leave hospice care, your Medicare Advantage Plan won’t start again until the first of the following month.
Differences Between The Medicare Hospice Benefit And Regular Medicare
- Medicare hospice coverage is limited to beneficiaries who are terminally ill.
- Hospice coverage is for pain and symptom management and comfort, not for curative treatment of the underlying terminal illness.
- Hospice coverage is holistic. Not only is medical care covered, but so are social work services, chaplain services, bereavement services and homemaker services.
A Comparison of Medicare Home Health Benefits and Hospice Benefits
| Service | |
| Not Covered | Covered, during periods of medical crisis |
¹ There are additional services that can be provided in the home, but are not included in the home health benefit. Medicare will pay for reasonable and necessary home health visits if all the following requirements are met: 1. Patient needs skilled care 2. Patient is homebound 3. Care is authorized by physician and 4. Home Health agency is Medicare-certified. .² Medicare will pay for hospice care if all the following requirements are met: 1. Prognosis that life expectancy is 6 months or less. 2. Terminal illness is certified by physician 3. Patient elects hospice benefit 4. Care is specified in the hospice plan of care and 5. Hospice program is Medicare-certified. .
Also Check: Is Humana Medicaid Or Medicare
Are You Automatically Enrolled In Medicare When You Turn 65
Yes. If you are receiving Social Security, the Social Security Administration will automatically sign you up at age 65 for parts A and B of Medicare. Social Security will send you sign-up instructions at the beginning of your initial enrollment period, three months before the month of your 65th birthday.
Read Also: Does Medicare Automatically Start At 65
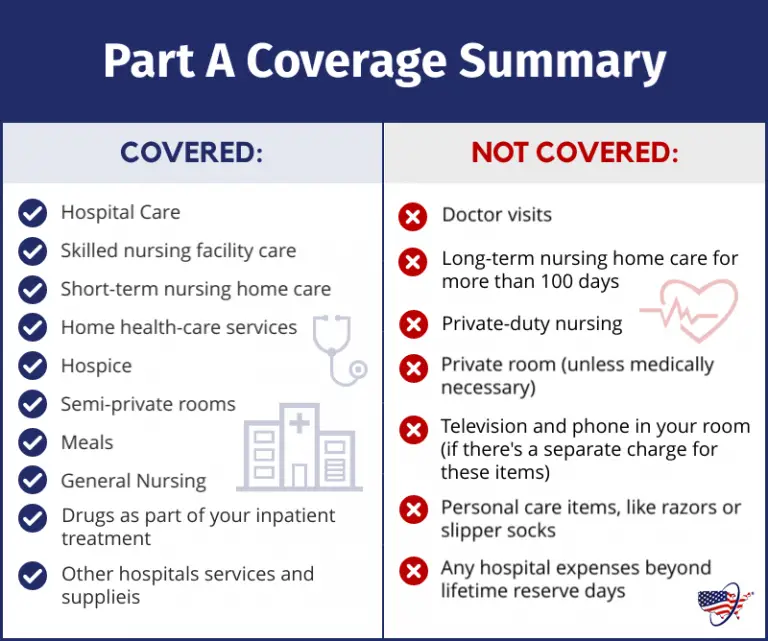
What Hospice Care Is Covered
Hospice care providers care for the whole person, meaning they help address physical, emotional, social and spiritual needs .
The following things related to hospice care are covered, according to Medicare:
-
All items and services needed for pain relief and symptom management.
-
Medical, nursing and social services.
-
Drugs to manage pain.
-
Durable medical equipment for pain relief and managing symptoms.
-
Aide and homemaker services.
-
Other covered services needed to manage pain and additional symptoms, and spiritual and grief counseling for you and family members.
In addition to you and your family members, your hospice care team may include some or all of the following:
|
Doctors |
|
|
Pharmacists |
Volunteers |
Youll also have the option of a hospice nurse and doctor who are on-call 24/7, for the sole purpose of giving your family support.
Recommended Reading: Can You Receive Medicare Without Receiving Social Security Benefits
Are Palliative Care And Hospice The Same
The Difference Between Palliative Care and Hospice Both palliative care and hospice care provide comfort. But palliative care can begin at diagnosis, and at the same time as treatment. Hospice care begins after treatment of the disease is stopped and when it is clear that the person is not going to survive the illness.
How Long Will Medicare Pay For Hospice Care
Hospice care is for patients who have six months or less to live. However, estimating someones life expectancy is not an exact science. Therefore, the Medicare hospice benefit is broken down into two 90-day benefit periods that are followed by an unlimited number of 60-day benefit periods .
A terminally ill patient can continue receiving covered hospice care as long as their hospice physician continues to certify that they have six months or less to live. Some people retain their terminal status yet survive much longer than expected and remain under hospice care for many months or even years.
A patient must be certified as having six months left to live before the services can begin and be recertified at the start of each new benefit period. A face-to-face meeting with a hospice doctor is required prior to the start of their third benefit period to recertify their eligibility. These face-to-face recertification meetings are then required prior to each subsequent 60-day benefit period and must take place no earlier than 30 days before the new benefit period begins.
Due to the ongoing COVID-19 pandemic, keep in mind that the Centers for Medicare and Medicaid Services has temporarily eased some regulations, allowing telehealth services to be used in place of face-to-face encounters where appropriate. This includes hospice recertification visits.
Recommended Reading: What Age Does Medicare Take Effect
Medicare Advantage And Hospice
Medicare covers hospice care under Original Medicare benefits, even for patients who have a Medicare Advantage plan or Medicare Part C.
If you have Medicare Advantage, you will continue to receive the added coverages of your plan, like vision and dental care, even while in hospice care. Medicare Advantage may also cover the cost of prescription drugs that are not covered by Medicare Part A, including medications for conditions that are not related to your terminal illness.
Do Hospice Patients Get Oxygen

Supplemental Oxygen. Supplemental oxygen is frequently prescribed for patients in palliative care to manage their dyspnea at the end of life, even if they are not hypoxemic. In a survey sent to 648 palliative care specialists, > 70% of them responded that they had ordered palliative oxygen if the patient was dyspneic.
Recommended Reading: How Old To Be To Get Medicare
What Is A Hospice Unit
A small but growing number of New Jersey hospitals have a hospice unit. This is a section of the hospital designed to provide a home-like environment in which patients can receive hospice services. Care is provided by the hospice, and hospice staff is present 24 hours per day in these hospice units. Not all hospitals have hospice units.
It is the decision of the hospital which offers a hospice unit whether to admit a patient to the unit. The hospice will consider such factors as severe pain, complicated symptom management, family readiness to accept the patient back home, the absence of a primary caregiver at home, financial resources available to the family, financial resources available to the hospice, and the safety of the patients home environment.
Policies regarding admission, room and board payment, and length of stay in a hospital hospice unit are determined by the individual hospital.
Am I Eligible For Hospice Care
To be eligible for hospice care coverage, you must:
- Be certified as terminally ill. This typically means that you have an estimated lifespan of less than 6 months, although your doctor can extend this if necessary.
- Choose to accept palliative care instead of treatment to cure your condition. Palliative care is focused on providing comfort and support.
- Sign a statement indicating that youve chosen hospice care for your condition instead of other Medicare-covered treatments.
Recommended Reading: Does Medicare Cover Generic Viagra
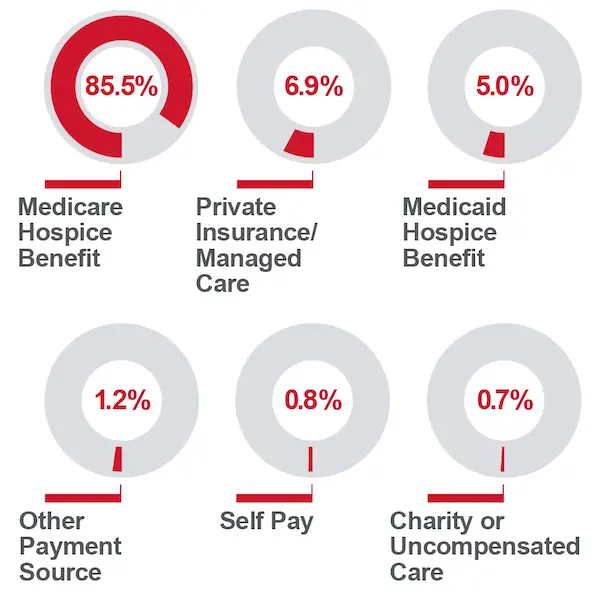
How Do You Pay For Hospice Care
For those not eligible for Medicare or Medicaid, payment for hospice can come from private insurance or an HMO, since these also include a hospice benefit.
Hospices employ financial specialists to help families who do not qualify for federal assistance and do not have insurance find available resources. The payment options for these families include self-pay and charitable organizations.
Facing a terminal illness brings with it many concerns. Paying for end-of-life care shouldnt be one of them.
What Hospice Care Isnt Covered By Medicare
Medicare wont cover hospice care provided by an agency that isnt Medicare certified. You must get hospice care from the Medicare-certified provider you choose, and all care must be included in your individualized plan of care and arranged by the hospice team. You cant get the same type of care from a different hospice unless you change your provider, which you can do once in each benefit period.
Once your hospice benefit starts, Medicare wont pay for:
- Treatment intended to cure your terminal illness or related conditions.For instance, if you want to pursue chemotherapy for your cancer treatment, hospice under Medicare wont generally cover it unless its considered palliative.
- Prescription drugs to cure your illness .
- Room and board. Medicare doesnt cover room and board if you get routine hospice care in a nursing home or a hospice inpatient facility. If your hospice team determines that you need general inpatient or respite care that they arrange, Medicare will cover your stay in the facility. You may have to pay a small copayment for the respite stay.
- Around-the-clock care if you are receiving routine hospice care.
- Care you get in an emergency room or a hospital unless it is arranged by your hospice team or is not related to your terminal illness or related conditions. Medicare doesnt cover ambulance transport either unless your hospice arranges it. If you are enrolled in hospice and have urgent needs, call your hospice, not 911.
Also Check: How To Choose A Medicare Supplement Plan
What Are The Medicare Requirements For Hospice Coverage
- The individual must be 65 years in age or older to qualify for Medicare coverage.
- The individual must be enrolled in Medicare to use the hospice end-of-life benefit.
- A hospice doctor must diagnose and certify the patient as terminal . This diagnosis must be made during a face-to-face encounter.
- The individual must sign a statement choosing palliative care instead of other life-saving benefits.
- The individual must choose a specific hospice care provider to administer all of their care.
Hospice Respite Care For Family Caregivers
The considerable physical and emotional effort involved in caring for a seriously ill loved one, especially someone who is approaching the end of their life, is significant. Short-term inpatient respite care, a hospice service provided by Medicare Part A, is an extremely valuable resource for people who are feeling distressed. This service provides terminally ill individuals the opportunity to continue receiving hospice care while they are receiving hospice services in a Medicare-approved hospice house, skilled nursing facility, or hospital. Their family caregiver may rest and recuperate while this is happening. The respite that an inpatient receives may last up to five days, and they may have to pay a small fee for their room and board while they are in the hospital. It is not unusual for patients and their families to request respite more than once, but the service can only be provided on an infrequent basis.
Also Check: Does Medicare Pay For Medical Alert Bracelets
Who Can Benefit From Palliative Care
Palliative care is a resource for anyone living with a serious illness, such as heart failure, chronic obstructive pulmonary disease, cancer, dementia, Parkinson’s disease, and many others. Palliative care can be helpful at any stage of illness and is best provided soon after a person is diagnosed.
In addition to improving quality of life and helping with symptoms, palliative care can help patients understand their choices for medical treatment. The organized services available through palliative care may be helpful to any older person having a lot of general discomfort and disability very late in life.
How To Find Nursing Homes That Accept Medicare Near Me
Here are a few tips for finding the right nursing home for your needs.
- If you like your doctor, ask if they provide services for any local nursing homes.
- Ask friends, family, and colleagues you trust if they or their family members have had good experiences with a particular nursing home.
- For extra guidance, .
Read Also: What Is Medicare Part C & D
The Basics Of Paying For Long
Custodial care refers to personal care given to individuals to help them with activities of daily living , which include bathing, dressing, and transferring themselves from seated to standing or in and out of bed. Also known as non-medical care, custodial care can be, and frequently is, provided by persons without professional medical training.
Skilled care, on the other hand, requires the provider to have professional medical training and licenses. In a home environment, the distinction between who is providing these types of care is fairly clear. In a hospital environment, it is less evident. Nurses, for example, provide both medical and custodial care at the same time, especially in smaller hospitals.
In the past, the simplest test to determine whether Medicare would or would not pay for care was to consider whether the care being provided was custodial/personal care or medical/skilled care. Up until a recent announcement in regards to Medicare Advantage , Medicare would not cover the custodial care, but would pay for skilled care . That said, original Medicare will still only pay for skilled care , but the rules of long-term care are more relaxed for MA.
How Much Does Hospice Care Cost With Medicare
How much hospice care costs depends on the type of illness and how early patients enter hospice. In 2018, the Society of Actuaries estimated that hospice patients with cancer received Medicare Part A and Part B benefits totaling around $44,030 during the last 6 months of their lives.
That figure includes the cost of inpatient hospital treatments, in addition to at-home hospice care.
The good news is that there are no deductibles for hospice care under Medicare.
Some prescriptions and services may have copays. Prescriptions for pain medications or symptom relief may carry a $5 copay. There may be a 5 percent copay for inpatient respite care if you are admitted to an approved facility, so your caregivers can rest.
Other than those instances, you wont have to pay for your hospice care.
Read Also: Does Medicare Cover The Cost Of An Ambulance
What Medicare Nursing Home Coverage Am I Eligible For If I Need Long
Medicare wont pay your nursing home costs, but you still have your Part A and Part B benefits while youre in a nursing home. For example, Part B covers your doctor visits and medical therapy visits, and if you need hospital care, Part A benefits apply. If you have a Part D Prescription Drug Plan, the medications you take in the nursing home are usually covered. You may have to enroll in a plan that works with your nursing home pharmacy, but the facility should help you choose the right coverage.
If you live in a nursing home, you may be able to enroll in a Medicare Advantage Special Needs Plan, which has benefits designed to best serve residents of a long-term care facility. These plans include Part D prescription drug coverage and may be more affordable than other Medicare plans. You may also qualify for a Special Needs Plan if you are on both Medicare and Medicaid.