How Much Will Medicare Pay For Total Knee Replacement
If its an inpatient surgery, Medicare will cover most of the cost. Youll be responsible for the Part A deductible, as well as additional cost-sharing in the form of coinsurance. If its an outpatient surgery, Medicare will cover 80% of the cost.
Youll be responsible for the Part B deductible and 20% of the cost. Any prescriptions given at the hospital will also be covered under Part B. Any prescriptions that youre prescribed to take at home wont have coverage unless you have a stand-alone Part D plan. Or, if you have an Advantage plan that covered prescriptions.
If you have a Medigap plan, depending on the letter plan you enrolled in, you could have zero out of pocket costs for total knee replacement surgery. If you have a Medicare Advantage plan, youll have to check with the carrier you enrolled with to determine what youll have to pay out of pocket.
Combined Ozone Gas And Viscosupplementation For The Treatment Of Knee Osteoarthritis
Giombini et al compared short-term clinical outcomes between IA injection of HA, oxygen ozone , and the combination of both, in patients affected by OA of the knee. A total of 70 patients with knee OA were randomized to IA injections of HA , or O2O3 or combined 1 per week for 5 consecutive weeks. KOOS questionnaire and VAS, before treatment at the end , and at 2 months after treatment ended were used as outcome measures. Analysis showed a significant effect of the conditions in all parameters of the KOOS score and a significant effect of groups for pain, symptoms, activities of daily living and QOL. The combined group scores were higher compared to the HA and O2O3 groups, especially at follow-up. The authors concluded that the combination of O2O3 and HA treatment led to a significantly better outcome especially at 2-month follow-up compared to HA and O2O3 given separately to patients affected by OA of the knee. This was a relatively small study with a short-term follow-up . These preliminary findings need to be validated by well-designed studies.
Is Coolief Covered By Medicare
Medicare should cover Coolief treatment. Although, we recommend confirming with your doctor and insurance provider. This method of treatment doesnt require any incision, no overnight hospital stay, and pain relief can last up to 12 months.
Most patients report an increase in mobility. In the Coolief clinical study, they found the treatment was longer-lasting and gave greater pain relief than the steroid injections. However, there are risks to all medical procedures discussing your options with your doctor is very important.
You May Like: Is Unitedhealthcare Dual Complete A Medicare Plan
Finding A Specific Code
Some articles contain a large number of codes. If you are looking for a specific code, use your browser’s Find function to quickly locate the code in the article. Sometimes, a large group can make scrolling thru a document unwieldy. You can collapse such groups by clicking on the group header to make navigation easier. However, please note that once a group is collapsed, the browser Find function will not find codes in that group.
Viscosupplementation Therapy For Knee
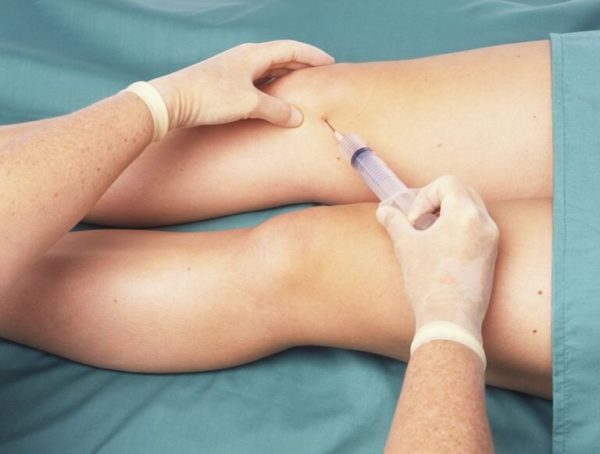
Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT, and the AMA is notrecommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services.The AMA assumes no liability for data contained or not contained herein.
Also Check: A Medicare Supplement Policy Must Not Contain Benefits Which
What Are The Side Effects Of Orthovisc
Although not a complete list, common side effects of Orthovisc include joint pain, joint swelling, swelling of the legs and feet, headache, dizziness, nausea, muscle cramps, and a general bad feeling . Allergic reactions are typically topical reactions to the injection that might include rash, hives, or itching.
Medicare Coverage For Total Knee Replacements And Alternative Treatments
Home / FAQs / Medicare Coverage / Medicare Coverage for Total Knee Replacements and Alternative Tre
Medicare covers total knee replacement surgery if the doctor deems its medically necessary. Medicare will also provide coverage for alternative treatments for knee replacement outside of surgery. The Medicare-covered alternative to knee replacements could include therapy, injections, or Durable Medical Equipment. Medicare may cover other knee replacement alternatives. Here we discuss surgery & alternative treatments for knee replacement surgery thats covered under Medicare.
You May Like: Does Medicare Cover Capsule Endoscopy
How Can A Medicare Supplement Plan Help
While a Medicare Advantage plan may cover most of the costs, you may want to consider a Medicare Supplement plan. Medicare Supplement helps cover costs that Original Medicare doesnt cover. More specifically, a Medigap plan will allow you to see ANY doctor, anywhere in the country that accepts Original Medicare.
For example, if you need gel shots once every six months, you might not meet your deductible in time. A Medigap plan can help pay your deductible, ensuring that Part B covers the injections. This could also save you money on other knee treatments covered by Medicare.
How Does Medicare Cover Knee Injection Treatment
Medicare will cover knee injections once every six months if they are medically necessary. The injections are covered under Medicare Part B and subject to the annual Part B deductible. X-rays are required prior to Medicare approval.
As mentioned above, there are many different injection treatments for the knees. But will Medicare pay for them?
- Does Medicare cover Corticosteroid shots? Yes!
- Does Medicare cover PRP shots? No. Most health insurance plans dont cover PRP shots.
- Does Medicare cover HA shots? Yes!
If you would like to discuss using your Medicare insurance to cover knee injections, call 436-5763 to schedule an appointment with our orthopedic team.
Also Check: When Do Medicare Benefits Start
License For Use Of Current Dental Terminology
End User License Agreement:These materials contain Current Dental Terminology , copyright © 2021 American Dental Association . All rights reserved. CDT is a trademark of the ADA.
The license granted herein is expressly conditioned upon your acceptance of all terms and conditions contained in this agreement. By clicking below on the button labeled “I accept”, you hereby acknowledge that you have read, understood and agreed to all terms and conditions set forth in this agreement.
If you do not agree with all terms and conditions set forth herein, click below on the button labeled “I do not accept” and exit from this computer screen.
If you are acting on behalf of an organization, you represent that you are authorized to act on behalf of such organization and that your acceptance of the terms of this agreement creates a legally enforceable obligation of the organization. As used herein, “you” and “your” refer to you and any organization on behalf of which you are acting.
Viscosupplementation For Muscle Stiffness/spastic Hemiparesis
Mayer presented 2 recent articles that propose novel interventions for treating spastic hemiparesis by changing biological infrastructure. In 18 patients with unilateral spastic arm paralysis due to chronic cerebral injury of greater than 5 years’ duration, Zheng et al transferred the C7 nerve from the non-paralyzed side to the side of the arm that was paralyzed. Over a follow-up period of 12 months, they found greater improvement in function and a reduction of spasticity compared to rehabilitation alone. Using functional magnetic resonance imaging , they also found evidence for physiological connectivity between the ipsilateral cerebral hemisphere and the paralyzed hand. In the 2nd article, Raghavan et al examined the concept of stiffness, a common symptom in patients with spastic hemiparesis, as a physical change in the infras-tructure of muscle. Raghavan’s non-neural hyaluronan hypothesis postulated that an accumulation of hyaluronan within spastic muscles promotes the development of muscle stiffness in patients with an upper motor neuron syndrome . In a case series of 20 patients with spastic hemiparesis, Raghavan et al reported that upper limb intra-muscular injections of hyaluronidase increased passive and active joint movement and reduced muscle stiffness. The author concluded that interventions that change biological infra-structure in UMNS is a paradigm on the horizon that bears watching.
Code Code Description
You May Like: When Is The Medicare Supplement Open Enrollment Period
Combined Use Of Viscosupplementation And Other Intra
These researchers prospectively enrolled 104 patients with knee osteoarthritis and randomized them to receive either a single intra-articular injection of hylan GF-20 , or a single intra-articular injection of hylan GF-20 and 1 ml of triamcinolone hexacetonide . VAS, WOMAC, and Lequesne questionnaires were completed at baseline and at weeks 1, 4, 12, and 24. At week 1 the WOMAC and VAS scores were lower in Group VS + T, compared with Group VS. There was no difference regarding the adverse effects. At weeks 4, 12, and 24 there were no differences in the groups. The authors concluded that the addition of triamcinolone hexacetonide improved 1st-week symptom and functional scores of viscosupplementation, but not beyond. It did not appear to increase the likelihood of adverse effects. They also stated that one can speculate that triamcinolone could positively affect the action in disease progression however, more studies are needed on this matter.
HA/PRP blends have been obtained mixing human PRP and 3 different HA at different concentrations:
What Are Knee Injections And How Do They Help With Pain

A knee injection is a shot that helps relieve joint pain and inflammation. Knee replacement surgery is costly, carries a long recovery time, and comes with the risk of infection or blood clots. On the other hand, injections are very safe, inexpensive, and require little or no time to recover. Your doctor gives you a shot, and thats pretty much it!
Don’t Miss: Does Medicare Cover House Calls
How Effective Are Hyaluronic Acid Injections For Osteoarthritis
Studies show hyaluronic acid injections may work better than painkillers for some people with OA. Other studies have shown they also may work as well as corticosteroid knee injections.
Hyaluronic acid injections seem to work better in some people than others. They may be less effective in older adults and people with severe OA.
Does Medicare Cover Orthovisc Injections
- Does Medicare cover Orthovisc? Discover whether Orthovisc is covered by Medicare and Medicare Advantage Plans and how much Orthovisc costs without insurance.
Knee arthritis is a painful condition that can cause mobility problems. Many people with knee arthritis get relief from an injectable lubricant like Orthovisc. But does Medicare cover Orthovisc? Below, you can find out whether Original Medicare and Medicare Advantage cover Orthovisc.
Also Check: Does Medicare Part B Cover Home Health Care Services
American Hospital Association Disclaimer
The American Hospital Association has not reviewed, and is not responsible for, the completeness or accuracy of any information contained in this material, nor was the AHA or any of its affiliates, involved in the preparation of this material, or the analysis of information provided in the material. The views and/or positions presented in the material do not necessarily represent the views of the AHA. CMS and its products and services are not endorsed by the AHA or any of its affiliates.
Additional Coverage For Knee Treatment And Therapy
While Original Medicare will provide coverage for knee replacement surgery and gel injections, it may not cover other treatments. For example, if you need prescription drugs to manage your pain, youll need to get extra coverage. You could get drug coverage with a Part D or Medicare Advantage Prescription Drug plan .
That said, Original Medicare will cover most knee therapies. Medicare Part A covers inpatient surgeries, while Medicare Part B covers outpatient physical therapy. Part B also covers doctors visits and Durable Medical Equipment .
Call us at to compare Medicare plans that may cover knee gel injections
Don’t Miss: Does Medicare Cover Any Dental Surgery
Brand Selection For Medically Necessary Indications
As defined in Aetna commercial policies, health care services are not medically necessary when they are more costly than alternative services that are at least as likely to produce equivalent therapeutic or diagnostic results. Durolane, Gel-One, Gelsyn-3, GenVisc 850, Hyalgan, Hymovis, Supartz FX, Synojoynt, Synvisc, Synvisc One, Triluron, Trivisc, and Visco-3 viscosupplement products are more costly to Aetna than other viscosupplement products for medically necessary indications. There is a lack of reliable evidence that Durolane, Gel-One, Gelsyn-3, GenVisc 850, Hyalgan, Hymovis, Supartz FX, Synojoynt, Synvisc, Synvisc One, Triluron, Trivisc, and Visco-3 are superior to the lower cost viscosupplement products: Euflexxa, Monovisc, and Orthovisc. Therefore, Aetna considers Durolane, Gel-One, Gelsyn-3, GenVisc 850, Hyalgan, Hymovis, Supartz FX, Synojoynt, Synvisc, Synvisc One, Triluron, Trivisc, and Visco-3 to be medically necessary only for members who have a contraindication, intolerance or ineffective response to the available equivalent alternative viscosupplement products: Euflexxa, Monovisc, and Orthovisc.
Keep Coupons Handy With The Free Singlecare App
Orthovisc is a brand-name injection that reduces knee pain for patients with osteoarthritis, a condition in which cartilage wears away in the joints. The active ingredient in Orthovisc, hyaluronic acid, is a gooey substance produced by the body that works naturally in the body as a lubricant and moisture retainer. Orthovisc is injected directly into the knee by a healthcare provider.
Recommended Reading: How To Request A Replacement Medicare Card
Does Medicare Pay For Knee Gel Injections
Yes, Medicare will cover knee injections that approved by the FDA. This includes hyaluronan injections. Medicare does require that the doctor took x-rays to show osteoarthritis in the knee.
The coverage is good for one injection every 6 months. Hyaluronan is Hyaluronic Acid, its naturally occurring in the body. While this solution may not be best for everyone, it should be something to consider before resorting to a knee-replacement. This treatment is also called Viscosupplementation.
Following Anterior Cruciate Ligament Reconstruction

The day after the procedure, the patients were randomized to receive a single injection of 3 mL HA or 3 ml saline solution after surgical drains were removed. All patients were evaluated at baseline and at 15, 30, 60, and 180 days and 12 months after surgery by use of the following tools: Short Form-36 Health Survey , International Knee Documentation Committee subjective score, VAS for pain, VAS for general health status, and Tegner score. At each follow-up evaluation, the trans-patellar circumference and active and passive ROM of both knees were recorded. No severe adverse events were documented after early viscosupplementation. A significant improvement was documented in both treatment groups. Significant differences were documented in the trans-patellar circumference at 60 days and in active ROM at 30 days post-operatively patients who received HA had better values compared with the placebo group . No statistically relevant intergroup differences were found in the clinical scores. The authors concluded that he findings of this study documented no AEs and had some positive findings in terms of active ROM recovery and trans-patellar circumference reduction. However, the early post-operative application of viscosupplementation did not lead to significant improvement in clinical scores after ACL reconstruction.
You May Like: Does Medicare Come Out Of Your Paycheck
What Are The Risks Of Orthovisc Injections
The most common side effects of Orthovisc injections are pain, aching and swelling around the injection site. Some people also develop a localized skin reaction, such as hives or an itchy rash. Generally, side effects are mild and resolve within a few days. If you develop severe or persistent side effects, you should seek prompt medical attention. You should tell your doctor beforehand if you have an infection or are pregnant or breastfeeding because Orthovisc may not be suitable for you.
Another potential risk of using Orthovisc injections is an allergic reaction. You shouldn’t use Orthovisc if you’re allergic to bird products because it contains hyaluronan harvested from rooster combs.
Does Medicare Cover Knee Gel Injections
If youre living with osteoarthritis in your knees, you know how difficult and painful it can be. Today in the United States, over 50 million people have osteoarthritis and many live with pain, stiffness, loss of flexibility, bone spurs, swelling and tenderness, and a general reduction in their day-to-day quality of life.
Medicare Benefits Solutions
2 people found this article useful
In cases of severe knee osteoarthritis, many physicians may suggest either having knee replacement surgery or treatment with gel injections in the knee. The gel injection treatment is non-invasive and helps by temporarily relieving the pain and restricted mobility that comes with osteoarthritis. While in most cases, people eventually require replacement surgery, getting knee gel injections could be a great option for the relief of your symptoms.
Does Medicare cover knee gel injections?If you have Original Medicare Part B or a Medicare Advantage plan, your benefits include coverage of knee gel injections if you are eligible. To meet the requirements for eligibility, you must meet the following requirements: The injections are for the knees only You show evidence of knee osteoarthritis with X-rays Coverage is acceptable for injections given no more often than every six months Your Medicare-affiliated health care provider must certify that the injections are medically necessary.
Read Also: Is Dexcom G6 Cgm Covered By Medicare
Hyaluronan Acid Therapies For Osteoarthritis Of The Knee
L35427
Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT, and the AMA is notrecommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services.The AMA assumes no liability for data contained or not contained herein.
