Does Medicare Cover A Sleep Study For Sleep Apnea
Medicare can offer coverage for sleep studies. However, before treatment, the patient must meet specific criteria.
Medicare Part B can cover a sleep study test if your doctor orders it, if medically necessary to diagnose a condition such as sleep apnea and if sleep is recorded and staged. However, Medicare will not cover a sleep study for chronic insomnia.
Even with coverage, you may be responsible for some of the costs. If you have a Medicare Advantage plan, talk to your plan provider about in-network practitioners, coverage, and costs. Those with a Medigap policy may pay little to nothing out-of-pocket when receiving treatment.
Does Medicare Cover Other Sleep Disorders
Currently, Medicare covers sleep studies if you exhibit symptoms of OSA, but those can also overlap with symptoms of other sleep disorders. If youre diagnosed with narcolepsy or insomnia, your doctor can prescribe you medication. For medication, you will need to be enrolled in a Medicare Part D Drug Plan, which you can be enrolled in on its own or as an additional Plan with your other Medicare Coverage . Under Part D, youll need to meet the current monthly deductible of $415.
Your copay will depend on the drug youre being prescribed. Prescription drugs as listed in a drug formulary categorizing drugs into different tiers. Drugs in Tier 1 are for generics and have lower copayments. Tiers 2 to 5 are brand-name and specialty drugs requiring higher out-of-pocket payments.
Whats Required To Get Coverage For Cpap
Medicare Part B covers CPAP therapy in two stages. Theres a three-month trial period prescribed by your doctor to determine if CPAP works for you. If the trial is successful, theres a rental period of up to 13 months, after which you own the machine. To obtain coverage, you must rent the machine from a Medicare-approved supplier of durable medical equipment.
But even before you begin the trial, you must have a sleep test to determine that you meet the clinical criteria for obstructive sleep apnea. The good news is that if home sleep test equipment is available through a local physicians office or sleep clinic, you need not spend the night in a sleep lab.
You May Like: What Is The Disadvantage Of A Medicare Advantage Plan
Does Medicaid Cover Cpap Treatment
The most effective treatment for sleep apnea is the use of a continuous positive airway pressure, or CPAP, machine. These machines deliver constant and steady air pressure to your airway as you sleep through a hose connected to a mask. In general, Medicaid does cover this sleep apnea treatment.
If youre diagnosed with sleep apnea according to Medicaids criteria, the program will cover an initial 12-week period of CPAP treatment. Medicaids criteria determines how severe your sleep apnea is based on your apnea-hypopnea index . This index measures how often your breathing is interrupted each hour.
If your condition improves during the 12-week period and youve shown compliance with your usage of the CPAP machine, your treatment will continue to be covered in the future. The improvement of symptoms must be confirmed by your doctor or sleep specialist. The compliance requirement basically ensures that youre using the machine enough to gain benefits. Currently, Medicaid requires that you use the machine for at least 4 hours a night, 70% of nights within the trial period.
Keep in mind that Medicaids benefits may not cover all costs, and you may need to pay for accessories such as filters and masks.
Diagnosing Sleep Apnea In Children
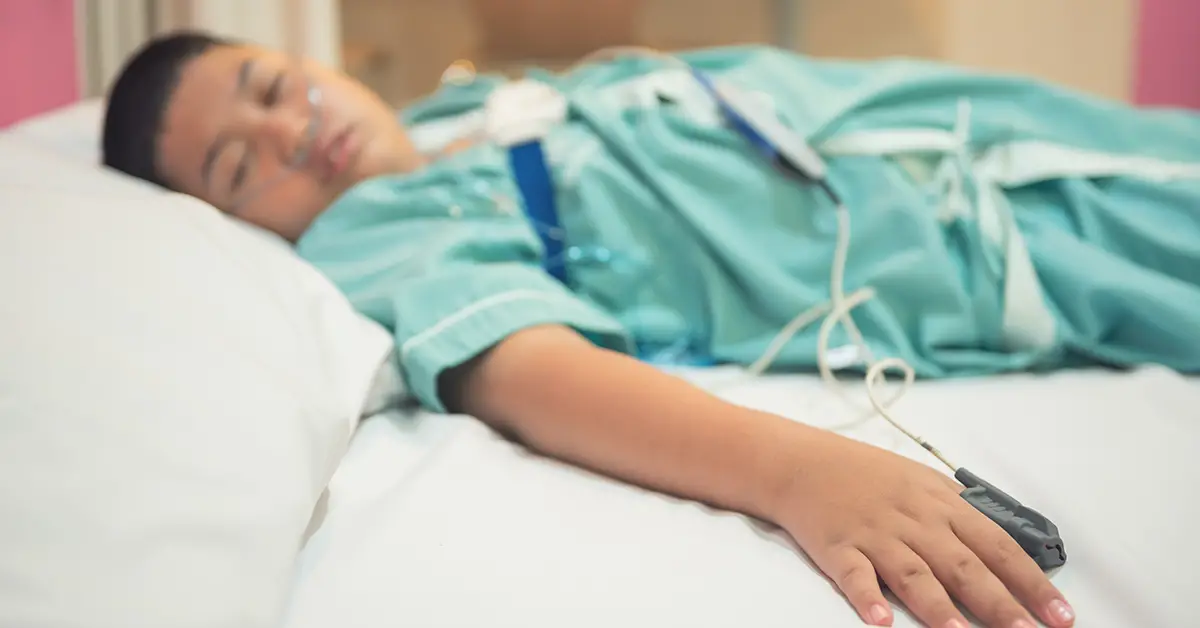
Most doctors follow these guidelines from the American Academy of Pediatrics:footnote 4
- During a routine checkup, your doctor will ask you and your child about snoring. If your child snores, be sure to tell your doctor.
- A complete sleep study typically is needed to find out if your child has sleep apnea and is not just snoring.
- Children who have sleep apnea and other disorders, such as Down syndrome or sickle cell disease, may need to see a specialist.
Don’t Miss: Does Medicare Cover Hearing Aids In Michigan
What Type Of Home Sleep Apnea Test Does Medicare Cover
Medicare will cover two types of home sleep testing devices:
- Type III home sleep test. This is a four-channel device which measures airflow, respiratory effort, heart rate and oxygen saturation.
- Type II home sleep test. This type of home sleep test uses at least seven channels.
Type III devices are the most common. Heres a great article from Sleep Review Magazine about 9 attributes to consider when picking HST devices.
Damaged Or Lost Cpaps
If your CPAP is damaged, lost, or faulty, you will need to contact Medicare regarding eligibility and costs for replacements/repairs. Depending on the situation, Medicare will cover the cost to replace or repair your equipment, and will also cover the cost of renting equipment while the originals are being repaired.
Also Check: Is Medicare Supplement Plan F Going Away
Why Pay For Sleep Studies And Cpaps
For Americans on Medicare, the benefits of CPAP therapy often outweigh the costs of your deductible plus 20% copayment for sleep studies, CPAP equipment, and CPAP replacement parts. As you use your CPAP, youll have a wide range of long-term benefits such as:
- Reduced risk of heart problems like congestive heart failure and coronary artery disease
- Reduced risk of stroke
- Reduced risk for Type 2 Diabetes
- Reduced risk of causing motor vehicle accidents
Youre also likely to experience the following physical benefits:
- Increased daytime alertness
- Reduced or eliminated snoring
Additionally, untreated, severe sleep apnea can cause serious damage to brain tissue over time. For those undergoing CPAP therapy, they will begin to develop a more regular sleeping pattern and ensure that the amount they sleep is quality sleep thereby repairing the damage done to your brain. You shouldnt rule out being able to experience improvements to your well-being in these ways:
- Increased concentration
- Increased emotional stability
- Improved memory
- Better relationships with your partner through improved mood reduction in irritability reduction in depressive symptoms and finally letting your partner get their own quality sleep without being disturbed by snoring.
Does Medicaid Cover Sleep Studies
- If you might have a sleep disorder, your doctor could order a clinical sleep study to learn more. Find out whether Medicaid will cover any costs for a sleep study.
If your doctor believes youâre exhibiting signs of sleep disorders, he may refer you to a polysomnography more widely known as a clinical sleep study. These studies require overnight evaluation to diagnose the severity of your symptoms and how theyâre affecting your sleep continuity, cardiac functions and other factors. This may be in the form of a sleep lab study or a home test. Find out more about whether Medicaid covers sleep studies below.
Recommended Reading: Does Medicare Cover Cpap Masks
Read Also: What Is The Requirement For Medicare
Genioplasty And Genial Tubercle Advancement
Song and associates performed a systematic review and meta-analysis for studies evaluating genioplasty alone, genial tubercle advancement alone, and GTA with hyoid surgery for the treatment of OSA. Three authors searched through November 15, 2015 10 databases were used. A total of 1,207 studies were screened 69 were down-loaded and 13 studies met inclusion criteria. A total of 111 patients were included, with 27 standard genioplasty, 10 modified genioplasty, 24 GTA, and 50 GTA-HS patients. For standard genioplasty, the AHI reduced from a mean ± standard deviation of 18.8 ± 3.8 to 10.8 ± 4.0 events/hour , p = 0.0001. Genioplasty improved lowest oxygen saturation from 82.3 ± 7.3 % to 86.8 ± 5.2 % , p = 0.0032. For modified genioplasty AHI increased by 37.3 %. For GTA, the AHI reduced from an M ± SD of 37.6 ± 24.2 to 20.4 ± 15.1 events/hour , p = 0.0049. Genial tubercle advancement improved LSAT from 83.1 ± 8.3 % to 85.5 ± 6.8 % , p = 0.2789. For GTA-HS, the AHI reduced from an M ± SD of 34.5 ± 22.1 to 15.3 ± 17.6 events/hour , p < 0.0001 GTA-HS improved LSAT from 80.1 ± 16.6 % to 88.3 ± 6.9 % , p = 0.0017. The authors concluded that standard genioplasty, GTA and GTA-HS can improve OSA outcomes such as AHI and LSAT. Moreover, they stated that given the low number of studies, these procedures remain as an area for additional OSA research.
Questions To Ask Your Sleep Surgeon
It is important to have a comprehensive understanding of the role of this treatment in your condition. The first choice for the treatment of obstructive sleep apnea is the use of continuous positive airway pressure . Success with this treatment requires proper mask fitting and optimal device settings.
In some cases, alternatives such as weight loss, bilevel therapy, the use of an oral appliance, or positional therapy can be pursued. In some cases, nothing seems to work.
Once you have exhausted treatment options with your board-certified sleep physician, it may be necessary to consider the role of the Inspire hypoglossal nerve stimulator. Consider some of these questions to ask the surgeon:
- Am I a good candidate for the surgery?
- If you couldnât do this surgery, what would they recommend as treatment instead?
- How often have they done this procedure?
- What is their success rate in resolving sleep apnea ?
- How many patients have complications such as bleeding, infection, or device removal?
- How will I know if the therapy works well for me?
- Do they have support to work through the insurance approval process?
- Will I have testing after the device is placed to determine settings and response to therapy?
- Who will I follow up with once the surgery is complete?
There may be additional considerations based on your specific circumstances.
Read Also: Sheets For A Split King Sleep Number Bed
You May Like: How To Apply For Medicare In Ga
Hypoglossal Nerve Stimulator Services
- 64583
- 64584
Despite AASM advocacy efforts for CMS to finalize the work RVUs for these three codes, consistent with the higher RUC recommendations, the agency finalized work RVUs of 14.00 for CPT code 64582, 14.50 for CPT code 64583 and 12.00 for CPT code 64584. However, CMS is finalizing the RUC-recommended direct practice expense inputs without refinement for all three codes.
Does Medicare Cover Oral Devices For Sleep Apnea
When you have sleep apnea, the need for rapid relief is obvious. Its not simply a question of obtaining a better nights sleep its also about your health. Obstructive sleep apnea, also known as OSA, is associated with increased blood pressure. Its also been linked to a number of other heart issues. That is why finding the correct and efficient treatment for OSA is so crucial.
Paying for medical equipment to treat sleep apnea can get pricey, as with any other medical piece of equipment. Its vital to understand what your insurance will and will not cover so you can plan ahead of time. Lets take a look at sleep apnea, the treatments available for it, and whether Medicare covers some devices.
Recommended Reading: Are Blood Glucose Test Strips Covered By Medicare
What Cpap Devices Will Medicare Cover
Currently, there are no guidelines for the type of CPAP Medicare will cover. CPAPs are incredibly expensive and complicated DME. Modern CPAPs have minimal noise, along with many advanced features. These might include:
- an automatic feature that detects the degree of pressure needed to keep your AHI low
- wireless functions or an SD card that keeps track of use, AHI, and amount of events per hours
- automatic detection on how well your mask is sealed and whether CPAP parts need to be replaced
- a humidifier to prevent dry throat
- automatic detection of when youve taken the mask off (so that it can automatically turn off
- adjustable ramp-up times where the machine sets a default pressure, then increases it once it detects youre asleep this is designed for your comfort
CPAPs can take some time to adjust to. After all, you are trying to sleep with a mask on your face. Remember to be patient and disciplined when starting CPAP therapy. Generally, CPAP users gain the most benefit when theyre able to keep the CPAP on them for at least 4+ hours. If you are able to do that, your device may record that. If you find youre waking up prior to 4 hours, you will need time to adjust to the CPAP and your preferred settings.
Your Cost For A Sleep Study Under Medicare
Sleep studies are considered a diagnostic test and must be ordered by your doctor to qualify for Medicare coverage.
Sleep studies are covered by Medicare Part B. You will owe 20 percent of the Medicare-approved cost of the study, and the Part B deductible applies.
You may owe less if you have supplement insurance, such as Medicaid or a Medigap policy.
If youre enrolled in a Medicare Advantage plan, you may be restricted to sleep centers and clinics within your plans provider network.
You May Like: How To Submit A Medical Claim To Medicare
Is A Sleep Study Worth It
Sleep disorders can lead to health challenges. If you are facing irregular sleep patterns, its important to consult with a doctor regarding next steps.
The CDC has conducted an extensive review of clinical studies on the effectiveness of sleep studies. There is no gold standard like there is for cancer which uses tissue biopsies and other diseases.
But the research shows that sleep studies generally provide an effective diagnosis. According to the CDC, sleep studies will identify a significant proportion of patients with OSA who will respond clinically to CPAP and will exclude a significant proportion of those who will not.
Because of this assessment, Medicare agreed to provide coverage for sleep studies. This has also been the case with various Medicaid programs.
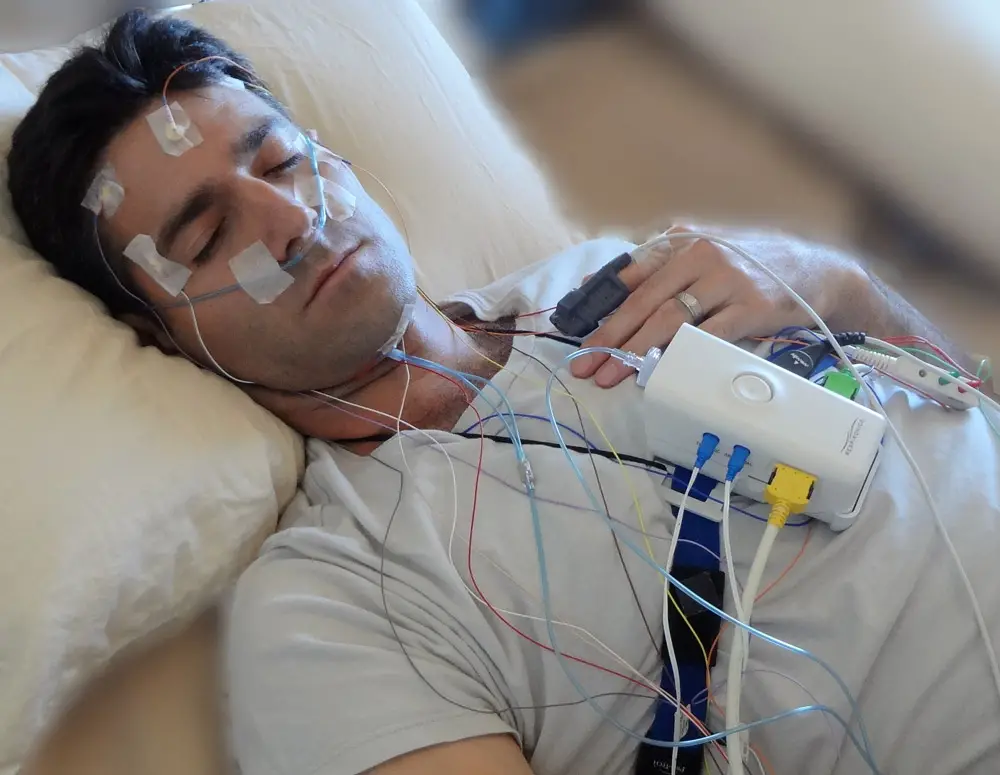
How Is Osa Diagnosed
A normal breathing problem that causes mild symptoms can go undiagnosed for years. Although some people may believe they have sleep apnea, a thorough diagnosis is required in order to receive coverage for any treatments. Patients must participate in a sleep study in order to be diagnosed. The patient spends the night at a sleep laboratory for monitoring during the sleep study. Blood oxygen levels, breathing rate, brain-wave activity, leg movements, and how many partial inhalations are taken each hour are all examined.
If a patients sleep study shows that he or she has sleep apnea, a doctor will either recommend using a CPAP machine or an oral apparatus to help them get some rest. Because a CPAP machine requires users to wear a mask while sleeping and requires them to plug the equipment into an outlet all night, not everyone is successful with it. Thats why people resort to mouthpieces instead. Mouthpieces are intended to provide a similar therapy as a CPAP machine, with the exception of the mask and requirement for an outlet.
Patients wear these custom-made mouthpieces while sleeping. Mouthpieces are used to help the lower jaw move forward and relax the tissues at the back of the throat. This ensures that the base of the tongue does not collapse, preventing airway obstruction. Patients who have mild to severe instances of sleep apnea benefit from mouthpieces.
You May Like: Can You Change Medicare Plans After Open Enrollment
Continuing To Maintain Your Supplies
- This visit has to be Face-to-Face. It cannot be done over the phone. The visit has to have everything listed in the CMS Checklist for Continuation of Suppliesin the Providers report at the time of the visit. CMS will not accept addendums.
- The download of the machine must show compliance of use. CMS states that compliance is > 4 hours per night 70% of the time within a current 30 day period.
- Should you not show compliance, you have to have another study and begin the process over again. See Initial Start to Investigate a Sleep Disorder above.
Medicare Coverage For Sleeping Disorders
Most experts recommend older adults get seven to nine hours of sleep per night however, age-related changes in sleep patterns including trouble falling or staying asleep can make it difficult to catch enough Zs. Lack of sleep can cause many problems, such as excessive daytime sleepiness, falls, overuse of sleep aids, depression, irritability, problems with attention and memory, high blood pressure, diabetes, stroke, and obesity.
If you or a loved one has a sleeping disorder, Medicare may be able to help with a good nights sleep. Learn which tests, items, and services Medicare covers for sleeping disorders.
Don’t Miss: How Many Medicare Plans Are There
Does Medicare Cover In
Yes.
In 2008, the Centers for Medicare and Medicaid Services updated the National Coverage Determination for CPAP to include home sleep apnea testing as a means to qualify patients with obstructive sleep apnea for CPAP therapy .
HST is a type of diagnostic polysomnography which is self-administered by the patient in his/her home. It is used to diagnose sleep apnea by recording several channels of information: respiratory effort, pulse, oxygen saturation, nasal flow and snoring. HST is a cost-effective alternative to in-center sleep testing for many patients if it is highly likely that the patient has moderate to severe sleep apnea, and if the patient has no other significant medical issues such as pulmonary diseases, neuromuscular disease or congestive heart failure. HST cannot be performed on children and cannot diagnose other sleep disorders such as restless leg syndrome, periodic limb movement disorder or narcolepsy. These patients should be tested in a sleep center .
You can read the American Academy of Sleep Medicine clinical guidelines for home sleep testing here.
Get Enrolled In Medicare That Will Help You Pay For A Cpap Machine

From does Medicare cover CPAP machines? to does Medicare pay for walk-in tubs?, we can answer all of your Medicare questions.
We can also help you get some of the costs covered from a Medicare plan thats right for you. Talk with a local Medicare specialist that can help you find the right plan to cover your sleep study, CPAP machine, replacement parts, and more. Costs may vary and plans can even vary state to state.
Learn more about your Medicare options from a local Medicare pro today! Click the button below to get a free Medicare quote.
You May Like: Sleep Number Bed Billings Mt
You May Like: When Can A Disabled Patient Enroll In Medicare Part D
