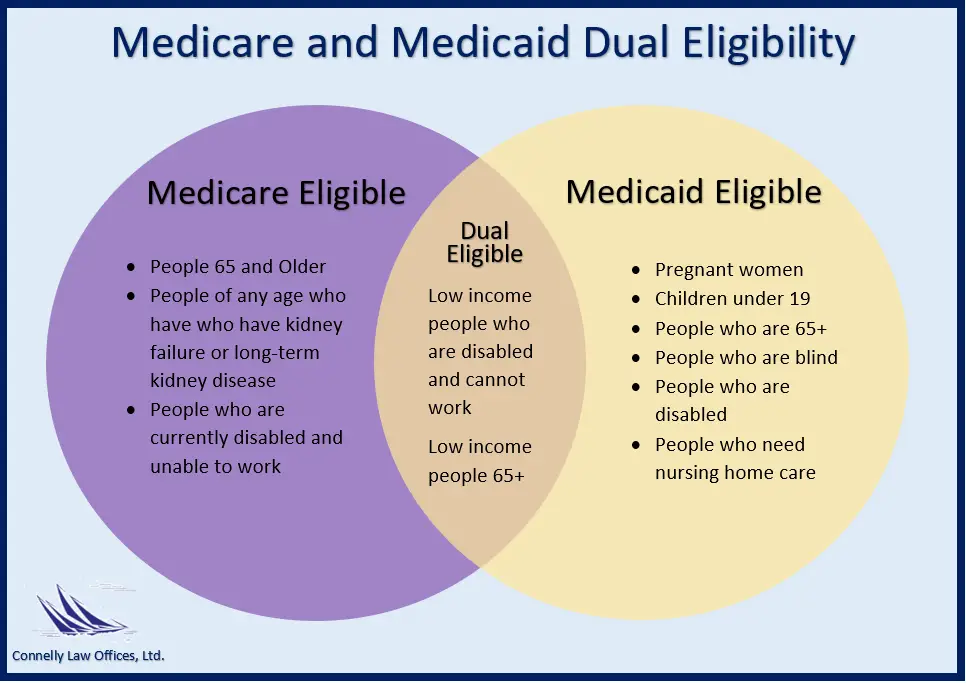
Distinguishing Between Medicare And Medicaid
Applicants qualified for both Medicare and Medicaid programs are referred to as Medicare-Medicaid enrollees having dual eligibility. Since the terms Medicare and Medicaid can be easily confused, it is essential to distinguish between them. While Medicare coverage is a federal health insurance program for seniors and people with disabilities, Medicaid is a state and public medical assistance program for people of all ages who need financial support. Both programs provide several benefits, such as doctor visits and hospitalization, but only Medicaid offers long-term nursing care. Particularly relevant to the subject of this article, Medicaid also covers long-term care and supports in-home and community-based settings, such as ones own home, an adult foster care residence, or an assisted living facility. However, beginning in 2019, Medicare Advantage plans began providing some long-term home and area-based benefits.
The CMS is in charge of both the Medicare and Medicaid programs. CMS collaborates with state agencies to administer the Medicaid program in each state, whereas the Social Security Administration applies for Medicare.
Dsnps Integrate With Medicaid
When you are eligible for both Medicare and Medicaid, you actually receive benefits from both programs. Technically, Medicare remains the primary payer of your benefits, and Medicaid becomes the secondary payer. Medicare pays first, Medicaid then pays some or all of whats left of your responsibility. Medicaid may cover all or part of these costs while youre in Medicare:
-
Part D drug plan premiums
-
Co-payments
-
Deductibles
-
Prescription drug costs
These are all expenses that youll encounter as you use your medical benefits, like when you go to the doctor or have prescriptions filled. Medicaid may pay for other costs, too, like your Part B premium . These kinds of costs are covered as part of the Medicare Savings Programs . There are actually four different programs within the MSP:
-
Qualified Medicare Beneficiary Program
-
Specified Low Income Medicare Beneficiary Program
-
Qualifying Individual Program
-
Qualified Disabled and Working Program
You can qualify for these savings programs based on your detailed eligibility for Medicaid. Generally, the less income and fewer assets you have, the more savings you qualify for. QMB program participants have their Part A and B premiums paid by their state.
How Do I Know If I Should Be Dual Eligible
Beneficiaries can find out if theyre eligible for Medicaid by contacting their Medicaid office. An Internet search for Medicaid offices in a beneficiarys state should provide the number to call but beneficiaries should make sure they are contacting a government office before sharing any personal information.
The Centers for Medicare and Medicaid Services also maintains a list of state agencies that oversee Medicaid. Beneficiaries can see if they already have Medicaid by contacting 1-800-MEDICARE and asking whether they receive Extra Help with their prescription drug costs .
Also Check: How To Apply For Medicare By Phone
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Qualified Medicare Beneficiary Program
This program helps pay for Medicare Part A and Part B premiums, deductibles, coinsurance and copayments.
Eligibility requires:
- Income of no more than $1,094 per month for an individual in 2021, or $1,472 per month for a married couple
- Resources of no more than $7,970 for an individual in 2021, or $11,960 for a married couple
Also Check: Does Medicare Cover Ear Cleaning
What Is The Medicare Savings Program
There are four types of Medicare Savings Programs:
- Qualified Medicare Beneficiary Program
- Specified Low-Income Medicare Beneficiary Program
- Qualifying Individual Program
- Qualified Disabled and Working Individuals Program
If you answer yes to these 3 questions, to see if you qualify for assistance in your state:
If you qualify for the QMB program, SLMB, or QI program, you automatically qualify to get Extra Help paying for Medicare drug coverage.
How To Qualify For Medicaid And Medicare Dual Eligible
If you are one of the thousands of Americans turning 65 soon, you probably understand the need to sign up for Medicare. However, you might be less familiar with Medicaid and what the term Dual Eligible means. There are some very important things you should know about Medicaid and Medicare dual eligible plans.
Read Also: How Much Does Medicare Pay For Ambulance
What If Your Doctor Only Accepts Medicare And Not Medicaid
Doctors are not required to accept Medicaid payment. Why? It requires more paperwork for them, and Medicaid reimbursements can be less than other forms of insurance. What can you do?
- Remember that there are more than 70 million people on Medicaid. Therefore, many doctors are indeed treating people with Medicaid coverage.
- If you already have a doctor you like, explain to him or her that you recently received Medicaid. They may continue to see you as a patient, even if they are not accepting other new patients on Medicaid. After all, you are an established patient of theirs.
- You may have to put a little effort into finding doctors in your area who accept Medicaid payment. Try searching the physician finder websites in your area, ask your Medicaid contact person, and call individual doctors offices.
- If a doctors office says they dont accept Medicaid, ask for a referral to a practice that does accept new Medicaid patients.
How Do I Know If I Qualify For Medicaid And Medicare
Twelve million individuals are currently enrolled in both Medicaid and Medicare.1 These individuals are known as dual eligible beneficiaries because they qualify for both programs. As long as you meet the federal qualifications for Medicare eligibility and the state-specific qualifications for Medicaid eligibility, you will qualify as a dual eligible. To qualify for Medicare, individuals generally need to be 65 or older or have a qualifying disability.
There are several levels of assistance an individual can receive as a dual eligible beneficiary. The term full dual eligible refers to individuals who are enrolled in Medicare and receive full Medicaid benefits. Individuals who receive assistance from Medicaid to pay for Medicare premiums or cost sharing* are known as partial dual eligible.
*Cost sharing is the amount of your health care that you pay out of your own pocket. Typically, this includes deductibles, coinsurance, and copayments.
Read Also: What Is Medicare Chronic Care Management
What Is Medicare Extra Help
Extra Help is a federal program that helps pay for out-of-pocket costs related to Medicare prescription drug coverage. Extra Help is also known as the Medicare Part D Low-Income Subsidy
The assistance that Medicare Extra Help may provide includes:
- Help paying Part D premiums
- Lowered out-of-pocket costs of prescription drugs
- An annual Special Enrollment Period to enroll in a Part D plan or switch to a new one
- Elimination of Part D late enrollment penalties
You automatically qualify for Extra Help if you are enrolled in Medicaid, Supplemental Security Income or a Medicare Savings Program.
You may still qualify for Extra Help if you are not enrolled in any of those programs but still have income and assets below a certain limit.
What Are The State
Benefits for dual eligible beneficiaries candiffer based on your state of residence. Differences by state may include:
- Medicaid offered through Medicaid managed care plans
- fee-for-service Medicaid coverage
- plans that include all Medicare and Medicaid benefits
Income and resource standards are defined by federal law for full Medicaid and the Medicare Savings Programs. At their discretion, states can effectively raise the federally mandated limits.
Youre also considered a dual eligible beneficiary if youre enrolled in Medicare Part A or Part B and receiving cost-sharing through a Medicare savings program .
Below is table summarizing the benefits and eligibility criteria for each of the different MSPs in 2021:
| MSP | ||
|---|---|---|
| Specified Low-Income Medicare Beneficiary program | assists in the payment of Part B premiums | individual monthly income of $1,308 or less, individual resources limit of $7,970 married couple monthly income of $1,762 or less, married couple resources limit of $11,960 |
In addition to the Medicare savings programs, you also may be eligible for some of the following needs-based programs through Medicare:
- PACE : a Medicare-Medicaid joint program that provides medical and social services for people with significant needs who want to continue living at home
- Medicares Extra Help program: can help those with low incomes get the prescription drugs they need at reduced or no cost
Dual eligibility for Medicare and Medicaid means that youre enrolled in Medicare and either:
You May Like: Does Medicare Advantage Cover Chiropractic Care
Qualified Disabled And Working Individual
You may be eligible to purchase Medicare Part A benefits, but unable to afford it because of your low income. In this case, Medicaid will pay your Medicare Part A premium. This is more common with people under the age of 65.
In 2021, the maximum monthly income to qualify is $4,379 for an individual and $5,892 for a couple. The 2021 maximum asset level, however, is set at just $4,000 for an individual and $6,000 for a couple.
Dual Eligible Beneficiaries Under Medicare And Medicaid
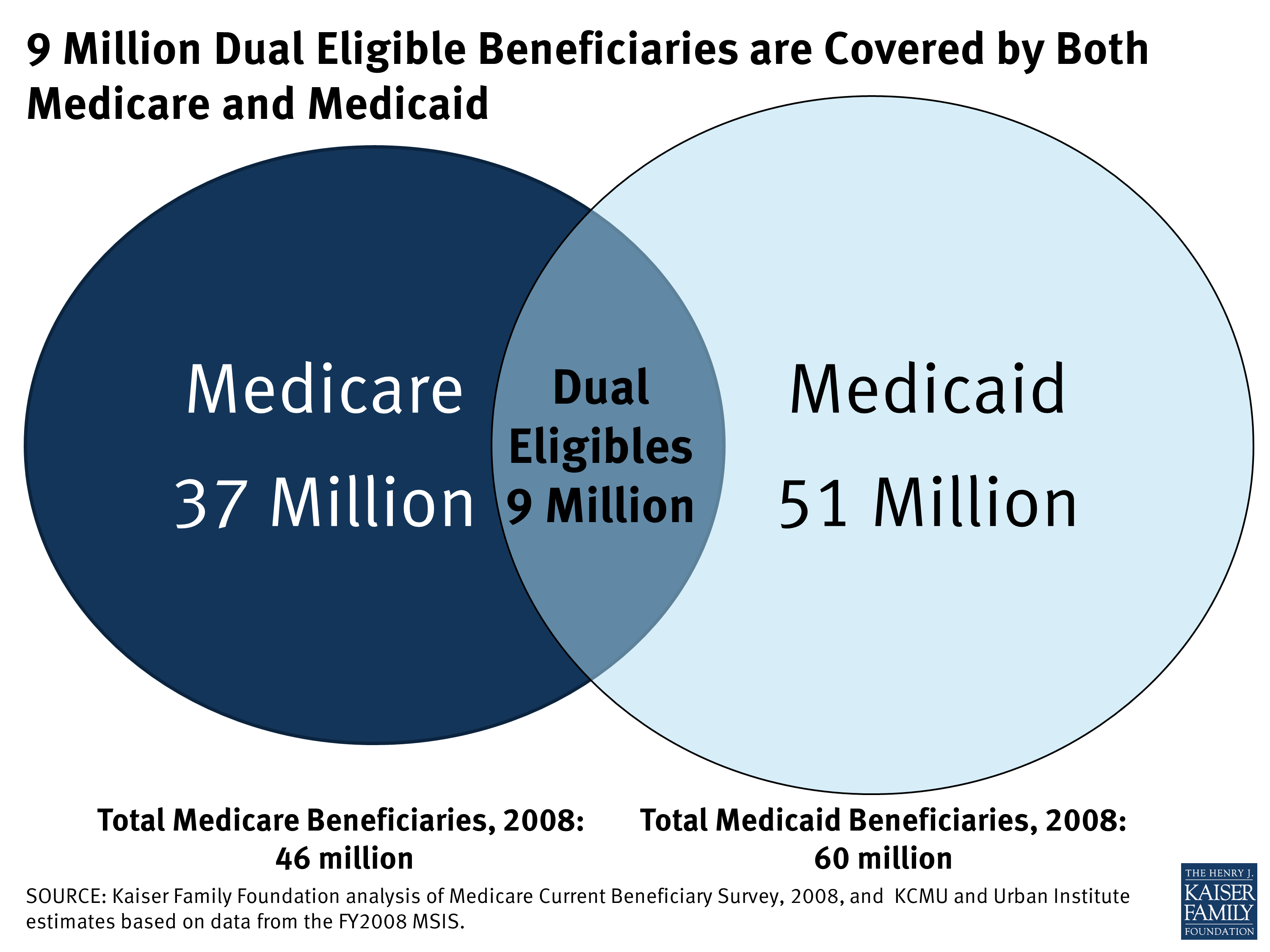
There are an estimated 11.4 million individuals receiving services through bothMedicare and Medicaid. These individuals, or dual eligible beneficiaries, are among some of the most vulnerable members of the patient population, due to a combination of low income and a high incidence of chronic health conditions. However, dual eligible beneficiaries face distinct challenges to receiving the services to which they are entitled.
Don’t Miss: How Soon Can I Sign Up For Medicare
Dual Eligible Special Needs Plans
In some states, dual eligible beneficiaries may have the option of enrolling in a D-SNP, which is different from a traditional SNP or Special Needs Plan. These plans are specially designed to coordinate the care of dual eligible enrollees. Some plans may also be designed to focus on a specific chronic condition, such as chronic heart failure, diabetes, dementia, or End-Stage Renal Disease. These plans often include access to a network of providers who specialize in treating the specified condition. They may also include a prescription drug benefit that is tailored to the condition.
What Medicaid Covers For Medicare Enrollees
Medicare has four basic forms of coverage:
- Part A: Pays for hospitalization costs
- Part B: Pays for physician services, lab and x-ray services, durable medical equipment, and outpatient and other services
- Part C: Medicare Advantage Plan offered by private companies approved by Medicare
- Part D: Assists with the cost of prescription drugs
Medicare enrollees who have limited income and resources may get help paying for their premiums and out-of-pocket medical expenses from Medicaid . Medicaid also covers additional services beyond those provided under Medicare, including nursing facility care beyond the 100-day limit or skilled nursing facility care that Medicare covers, prescription drugs, eyeglasses, and hearing aids. Services covered by both programs are first paid by Medicare with Medicaid filling in the difference up to the state’s payment limit.
Also Check: How To Sell Medicare Advantage Plans
A And B Financial Help
Once you’re dual eligible, youll be able to use your Medicaid to pay some or all of your Original Medicare premiums and health care costs.
But just remember that the type of benefit status you have as a dual eligible will affect how you can use your Medicaid to cover your Medicare.
With some dual-eligible benefit types, you will only be able to use your Medicaid insurance to pay for one part of Medicare .
With other dual-eligible types, you’ll be able to cover the entire cost of enrolling in Medicare. In these cases, Medicaid will pay your Medicare premiums, your deductibles, and your coinsurance amounts.
Key Facts about Dual Eligibles in the U.S.
- In 2020, there were 12.3 million dually eligible beneficiaries enrolled in Medicare and Medicaid.
- Dual eligibles account for around 20% of all Medicare enrollees and 15% of Medicare enrollees.
- In 2019, Wyoming had the lowest number of dual eligibles , and California had the highest .
What Are The Qualifications For Medicaid
Medicaid beneficiaries generally must be residents of the state in which they are receiving Medicaid. They must be either citizens of the United States or certain qualified non-citizens, such as lawful permanent residents. In addition, some eligibility groups are limited by age, or by pregnancy or parenting status.
Also Check: Are Grab Bars Covered By Medicare
What Does Medicare And Medicaid Pay For
Medicaid is known as the payer of last resort. As a result, any health care services that a dual eligible beneficiary receives are paid first by Medicare, and then by Medicaid. For full dual eligible beneficiaries, Medicaid will cover the cost of care of services that Medicare does not cover or only partially covers . Such services may include but are not limited to:
- Nursing home care
- Dental services
- Eye examinations for prescription glasses
The financial assistance provided to partial dual eligible beneficiaries is outlined in the table above.
Can I Get Medicaid If I Have Money In The Bank
Medicaid is the government health insurance program for people with low income and the disabled. There used to be a limit on how much you could have in assets and still qualify for Medicaid. Medicaid does not look at an applicants savings and other financial resources unless the person is 65 or older or disabled.
Recommended Reading: Will Medicare Pay For A Roho Cushion
What Does Medicaid Cover For Adults
Mandatory benefits include services including inpatient and outpatient hospital services, physician services, laboratory and x-ray services, and home health services, among others. Optional benefits include services including prescription drugs, case management, physical therapy, and occupational therapy.
What Is Medicaid And Medicare Dual Eligible
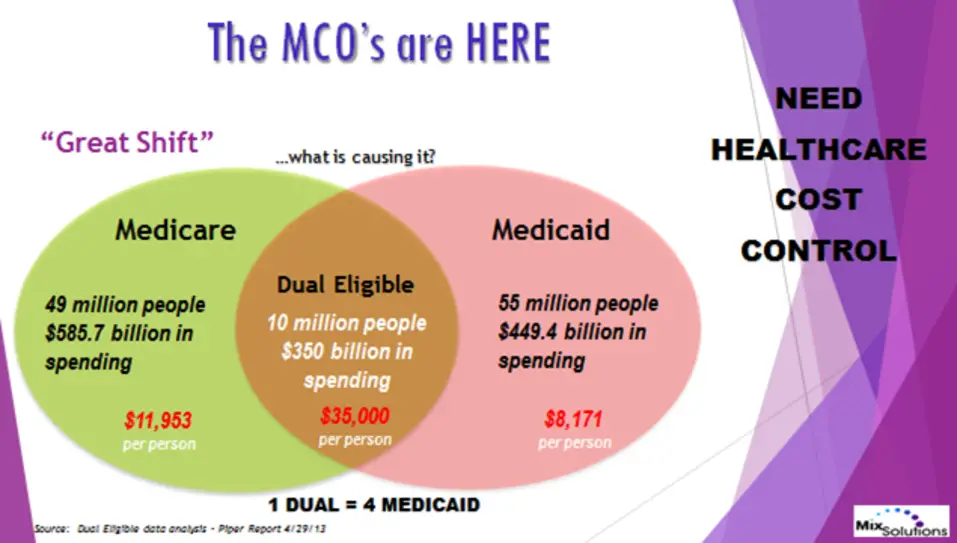
The phrase Dual Eligible simply means you have dual coverage, Medicaid and Medicare Parts A and B. If you have Medicare and Medicaid, you may be able to enroll in a special health plan that offers extra benefits. Each state may have different rules to qualify.
Keep in mind that there are other names for the programs that combine Medicaid and Medicare dual eligible. It is also referred to as Dual Eligible Special Needs Plan . You can have both Medicare Part A and Part B and Medicaid at the same time. Your Medicaid level will determine your qualification for this plan.
Read Also: Are Canes Covered By Medicare
Who Pays First If You Have Dual Eligibility
Since Medicaid is generally the payer of last resort, for dual eligible beneficiaries, Medicare pays covered medical services first.
If you have other coverage, such as employer group health plans or Medicare supplement plans , that coverage will pay first and Medicaid last.
Medicaid may cover healthcare costs that Medicare may not cover, or only partially covers, such as:
What Do I Need To Qualify For Medicare
Medicare coverage is for adults 65 and older and those with certain qualifying medical conditions or disabilities. To qualify, you would need proof of age, proof of income , residency or citizenship documentation, and more. Since Medicare is a government insurance program, anyone aged 65 or older can apply and receive insurance through this program.
Medicare premiums are based on your income and your work history. The eligibility requirements for Medicare Part A are very simple. If you or your spouse worked and paid Social Security taxes for ten or more years, your Medicare Part A premium is free. If not, you will pay a monthly premium for Part AMedicare Part A is hospital coverage for Medicare beneficiaries. It covers inpatient care in hospitals and skilled nursing facilities. It also covers limited home healthcare services and hospice care…..
With Part BMedicare Part B is medical coverage for people with Original Medicare benefits. It covers doctor visits, preventative care, tests, durable medical equipment, and supplies. Medicare Part B pays 80 percent of most medically necessary healthcare…, all Medicare beneficiaries pay a monthly Part B premium, however, if you are a high-income earner you will pay a little more. You can find the current schedule on this Medicare.gov page.
You May Like: Does Medicare Pay For Laser Cataract Surgery
Medicare Part D Extra Assistance Program
Aside from Medicaid, many other programs assist with medical expenses, and government sponsors them. Extra Help, a program that assists Medicare Part D enrollees with their prescription drug costs, can be applied for by a qualified individual.
To be eligible for Extra Help, a persons combined investments, real estate property, and savings must total no more than $29,160 if they are married and live with their spouse, or $14,610 if they are single.
To learn more about Extra Help and how to apply for it, go to the Medicare website.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Don’t Miss: How Soon Before Turning 65 Should You Apply For Medicare
